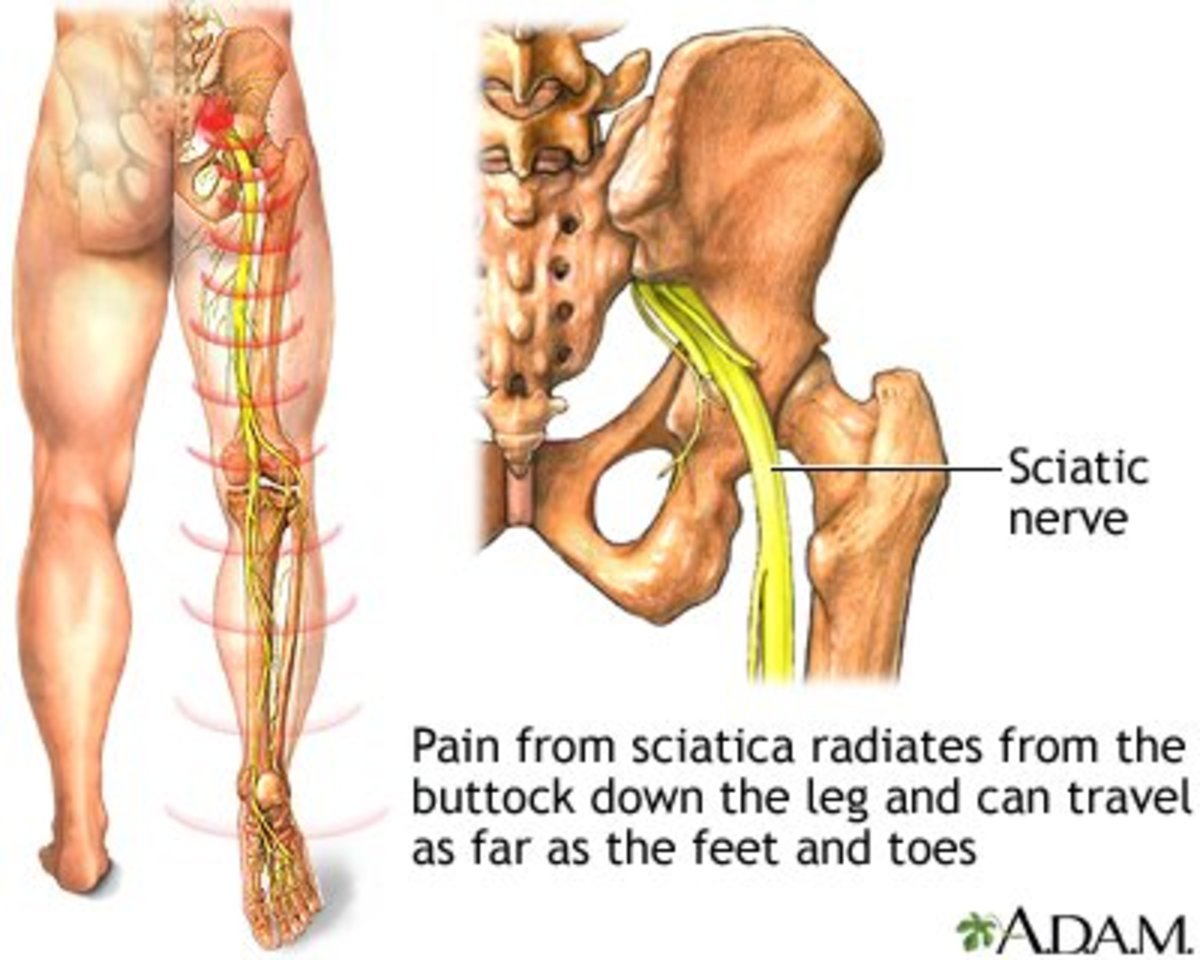
Chronic Fatigue Syndrome-Causes and Treatments


Simple drug approaches are unlikely to repair complex functional disruption of multiple organ systems.
- Chronic Fatigue Syndrome is a clinically defined condition primarily characterized by profound, disabling fatigue that has been present for six or more consecutive months that is not alleviated by rest and associated with 4 of the following symptoms:
- -Impaired memory or concentration
- -Sore throat
- -Adenopathy
- -Myalgias
- -Arthralgias
- -New headaches
- -Unrefreshing sleep
- -Post-exertion malaise
- A variety of non-specific symptoms also are apparent and include fever, headaches, myalgias, sleep disturbances, neurocognitive symptoms and depression
- Has multi-factorial causes and antecedents
- Many people also frequently experience these symptoms; nausea, drenching night sweats, intolerance of alcohol and pharmaceuticals and dizziness as well as environmental sensitivities
- Can affect any age and ethnicity; majority of cases affect Caucasian women between ages of 25 to 45.
- The average CFS patient has been ill for four or more years and is significantly disabled i.e. unable to work or perform tasks of daily living
- Epidemiologists point out that the prognosis is improved if the onset is acute or associated with an epidemic compared to one of gradual onset and sporadic outbreaks
- Several risk factors are associated with CFS and they are as follows:
- -Virus, Stress, Toxin, Allergic reaction or other transient traumatic condition may chronically activate the immune system
- In many cases, the immune system which usually gears down after an infection has been eliminated, remains activated after the initiating infection has passed
- Other theories have suggested disturbances in the endocrine system or point to the possibility that a single causative agent (still unidentified) causes CFS
- Difficult to differentiate CFS from many other conditions [1; page 151]
- There is no known specific treatment for CFS [1; page 154]. Conventional treatments revolve around the proposed etiological models (the immunological and the central nervous system model)
- Given the complexities of the various pathophysiologies likely to coexist in CFS,
The approach to assessing the functional processes that contribute to CFS.
- The inciting and sustaining etiology for CFS remains unknown [1]
- Management strategies (both allopathic and alternative) for CFS have usually targeted symptom relief
- Allopathic methods include antidepressants, antivirals, CNS stimulants, immune modulators, hormone therapy and various pain medications
- Alternative treatments use herbs and nutrients targeted at adaptogenic regulation of the immune system as well as acupuncture and massage for pain reduction and improving lymphatic drainage [1]
- Although abnormalities are often observed in many clinical tests from CFS patients, there is at present no single diagnostic test that establishes the presence of CFS. Thus many CFS sufferers are often ignored and labelled as malingerers, hypochondriacs and hysterical
- Most current treatment approached focus on symptoms alone
- Functional processes that contribute to CFS:
- -the capacity of a person’s detoxification system could also be a factor in determining that person’s risk for developing CFS and/or subsequent ability to recover from CFS
- -80% of CFS patients had significant abnormalities in detoxification pathways
- -An abnormal, increased intestinal permeability has also been observed in about 40-50% of CFS patients suggesting that this ‘leaky gut syndrome’ can contribute to the toxic burden of the liver
- -The CFS hypothesis suggests that nutritional support interventions directed at improving gastrointestinal function and detoxification capacity as components of a CFS treatment protocol [1]
- The empirical therapies for CFS include:
- *Magnesium (Oral or Parenteral)
- *Vitamin B12 supplements
- *Amino acid supplements
- *Antioxidants (such as Co-Q10, N-acetylcysteine and glutathione)
- *Address the combined impaired hepatic detoxification and leaky gut syndrome (Configured nutrition using “medical foods” may be the most important element in a multi-dimensional approach of complementary medicine)
Medical History and Potential Causes Underlying CFS [1; page 157]
Although there is no single physical finding or laboratory test deemed sufficient in diagnosis of CFS, two hallmarks of the disease are :
-poor tolerance to previously well-tolerated exercise
-positive Romberg/tandem stance finding
(Both these characteristics are associated with mitochondrial oxidative phosphorylation disorders)
Underlying Causes of CFS
Symptoms and (habits that trigger it)
Nutritional Imbalances or insufficiencies
-Physical Weakness
-Musculoskeletal pain
-Sleep disorders
-Cognitive dysfunction
-Premenstrual syndrome
-Dry skin
-Excessive thirst
-Hair loss
-Moodiness
-Irritability
-Restless legs syndrome
-Constipation
-Heart palpitations
Immunological imbalances and inflammation
*History of fevers and chills
*Sweats
*Recurring respiratory infections
*Environmental/food sensitivities
Elevated intestinal permeability
(history of non-steroidal anti-inflammatory drugs, nicotine, caffeine or alcohol)
Exposure to Parasites,
Impaired Digestion and/or absorption or intestinal Candida overgrowth
-History of foreign travel
-History of Irritable Bowel Syndrome or other intestinal disorders like excessive gas, bloating, distension, diarrhoea and constipation
Impaired detoxification
*History of chronic flu-like symptoms
*Exercise intolerance
*Increases sensitivity to the environment (MCS)
*Brain fog
*Fatigue
Two biochemical tests that need to be carried out in external and specialist laboratories prior to prescribing an adjunctive nutritional support program for CFS.[1; page 159-160]
Laboratory Assessments pointing to CFS (Please see 2 starred biochemical tests)
(1) Nutritional Imbalances
- RBC mineral imbalances (especially RBC Magnesium) which are often within normal limits but are often depressed
- *Rbc EFA imbalances
- Abnormal amino acid and urinary organic acid analysis
- Abnormal methyl malonic and homocysteine values
(2) Immune/Inflammatory Imbalances
- Up-regulated CD4/CD8
- Decreased NK cell activity
- Abnormal 2’-5’ RNase
- *IgG/IgE reactivity to specific foods are frequently found
Critically examine the results of these two tests indicating the range of values that are acceptable before nutritional intervention is required, e.g. a low incidence of abnormalities in detox pathways indicates a low incidence of CFS.
RBC EFA results and ranges [2; page 160-161]
The Major EFA markers:
SATURATED FATS (normal range: 19.3%-39.4%)
- Marker: Palmitic Acid
- Significance: One of the most common saturated fatty acids found in plants and animals. Main sources include butter, cheese, milk and meat. Dietary intake of palmitic acid increases the risk of developing cardiovascular disease. Elevated consumption is associated with increase in LDL cholesterol and may increase risk of diabetes
MONOUNSATURATED FATS-Omega 6 (Total Omega 6 range: 12.1%-29.2%)
Marker
Significance
Linoleic acid (LA); range:5-12.4%
-The parent or precursor for the omega 6 PUFAs
-Excess is common in the Western diets and may lead to increased metabolism od AA to proinflammatory eicosanoids
-Deficiency may lead to low levels of GLA
-Found in safflower, sunflower and sesame oils
Gamma-linoleic acid(GLA); range: 0-0.1%
-The precursor to DGLA required for Series 1 eicosanoids which have inflammatory-modulating properties
-Found in breast milk, borage oil and evening primrose oil
Arachidonic Acid; range: 6.2-13.7%
-A substrate used for the pro-inflammatory eicosanoids
-High levels are common in inflammatory conditions and contribute to increased risk of cardiovascular disease
-Found in meat, animal fats and peanuts
MONOUNSATURATED FATS-Omega 3
Marker
Significance
Alpa-linoleic acid (ALA); range:0.1-0.2%
-The parent fatty acid for the omega 3 PUFAs
-Dietary deficiency may lead to increased levels of Omega 6 PUFAs relative to Omega 3 PUFAs, resulting in increased metabolism of AA to proinflammatory eicosanoids
-Found in flax, pumpkin, hemp, walnut and soybean
Eicosapentanoic acid (EPA); range: 0.1-1.2%
-Low levels may indicate increased inflammation and higher risk of cardiovascular disease and stroke
-Found in fish oils
Docosahexanoic acid; range: 2.5-7.5%
-In conjunction with EPAs, low levels may increase risk of cardiovascular disease and stroke
-Found in fish oils
REFERENCES
1) Health Schools Australia Course Notes; Adjunctive Nutritional Support for Chronic Fatigue Syndrome 2012; pages 148-164.
2) Practitioner Manual-A guide to laboratory testing. ARL Pathology