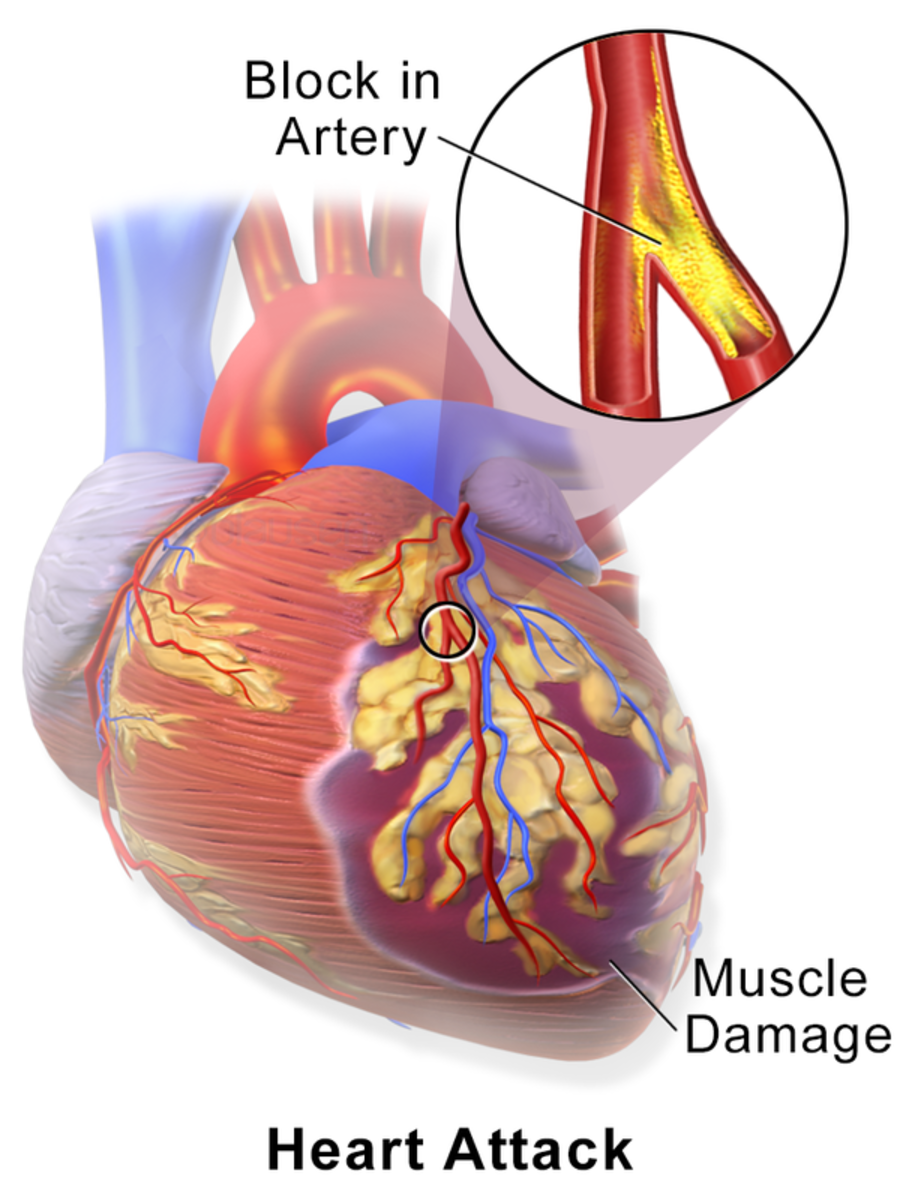
Chronic Valvular Heart Disease: Mitral Stenosis (MS)
Mitral Stenosis

Introduction
In Asia and Africa especially, rheumatic fever is the commonest cause of chronic valvular heart disease. The heart valves are inflamed in the rheumatic process. Approximately 40% of patients with acute rheumatic carditis develop chronic valvular lesions as sequelae. The incidence of rheumatic heart disease (RHD) is approximately 2-3 per 1000 children in school surveys conducted in different parts of Asia. The mitral, aortic, tricuspid and pulmonary valves are affected in the order of frequency. In many cases, valvular lesions are multiple. Very rarely all the four valves may be involved.
Recent evidence suggests that Coxsackie group B which causes carditis may also be involved in the genesis of chronic valvular heart disease. Other causes are syphilis, myxomatous degeneration occurring in Marfan’s syndrome, congenital abnormalities of valves, direct infection by bacteria or other pathogens in infective endocarditis, sclerosis affecting the valves, and connective tissue disorders.
Mitral Stenosis In Diagrams

Clinical Cardiology
Pathology And Pathophysiology
About 60% of patients with mitral stenosis in history are suggestive of antecedent rheumatic fever or other rheumatic manifestations. Others may have subclinical episodes. In the developed countries, MS was found to develop 7-10 years after the episode of rheumatic fever. In india, this interval is shorter. This may be a manifestation of the severe nature of the disease in Indian subjects. It is not uncommon to find full fledged mitral stenosis in children (Juvenile MS).
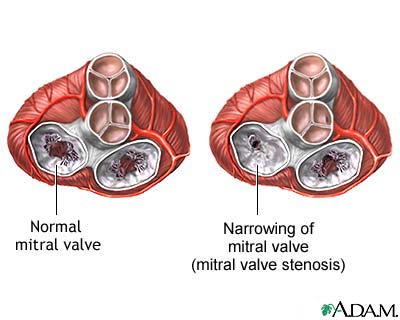
Pathology and pathophysiology: Stenosis results from the involvement of the cusps, commisures and the chordate of the mitral valve apparatus. The cusps become thickened and fibrosed, the commissures fuse and the chordate are thickened. Shortened and fused. These pathological processes cause distortion and narrowing of the mitral valve orifice. In longstanding cases, calcification develops. Normal mitral valve orifice is 4.5 cm2 in area. When it is reduced to 2.5cm2 ausculatatory findings are suggestive of mitral stenosis. Aperture size of 2.5-1.6cm2 is mild mitral stenosis and further reduction to 1.5-1.1cm2 leads to moderate stenosis. Valve area below 1cm2 is called critical stenosis.
In MS obstruction to left atrial blood entering the left ventricle leads to elevation of intra-atrial pressure (up to 25 mmHg). The left atrial pressure is reflected back in the pulmonary veins leading to pulmonary venous hypertension. Subsequently, pulmonary arterial hypertension sets in. The symptom and signs of pulmonary venous hypertension abate when arterial hypertension supervenes. Pulmonary arterial hypertension is the result of the following factors:
- Passive transmission of pulmonary venous pressure to the arteries;
- Reflex spasm of the arterioles in response to the rise in left atrial and pulmonary venous pressure and
- Structural changes in the pulmonary vascular bed.
Chronic pulmonary hypertension leads to right ventricular hypertrophy and eventually right ventricular failure and tricuspid regurgitation.
Mitral Stenosis
Clinical Features
Symptoms: Mild to moderate MS may remain asymptomatic to be picked up on routine examination. Severe MS is always symptomatic. Commonest symptom is exertional dyspnea and its severity depends upon the degree of stenosis. Exertion leads to tachycardia and increased venous return. These may cause sudden rise in left atrial pressure on account of the narrowed mitrial orifice. This in turn causes pulmonary venous engorgement and reduced compliance of the lung which manifests as dyspnea, paroxysmal nocturnal dyspnea and orthopnea. Occasionally this may lead on to acute pulmonary edema. Patients with severe pulmonary arterial hypertension and congestive heart failure may experience fatigue, loss of appetite and occasionally chest pain. Other common symptoms are palpitation, cough and hemoptysis. Hemoptysis is an early symptom in MS. This may result from the following causes:
- Rupture of dilated intrapulmonary bronchial veins due to rise in pulmonary venous pressure;
- Recurrent bronchitis;
- Acute pulmonary edema; and
- Pulmonary infarction
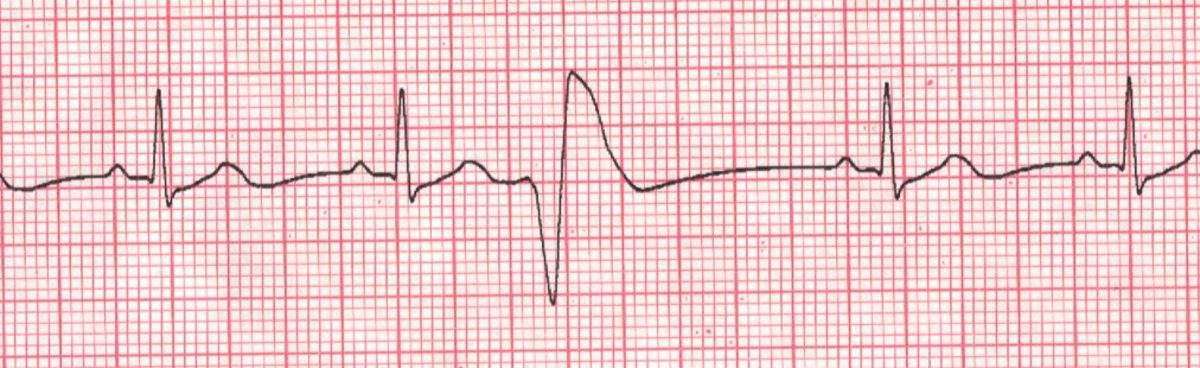
Hemoptysis tends to subside as pulmonary arterial hypertension develops. In longstanding cases of mitral stenosis with gross enlargement of the left atrium, atrial fibrillation develops as a frequent complication. Atrial fibrillation predisposes to the formation of thrombi in the atria and further embolisation. In the younger age groups MS is the commonest cause of atrial fibrillation. Pregnancy aggravates the symptom of MS.
© 2014 Funom Theophilus Makama