Clinical Significance Of Vascular And Platelet Disorders
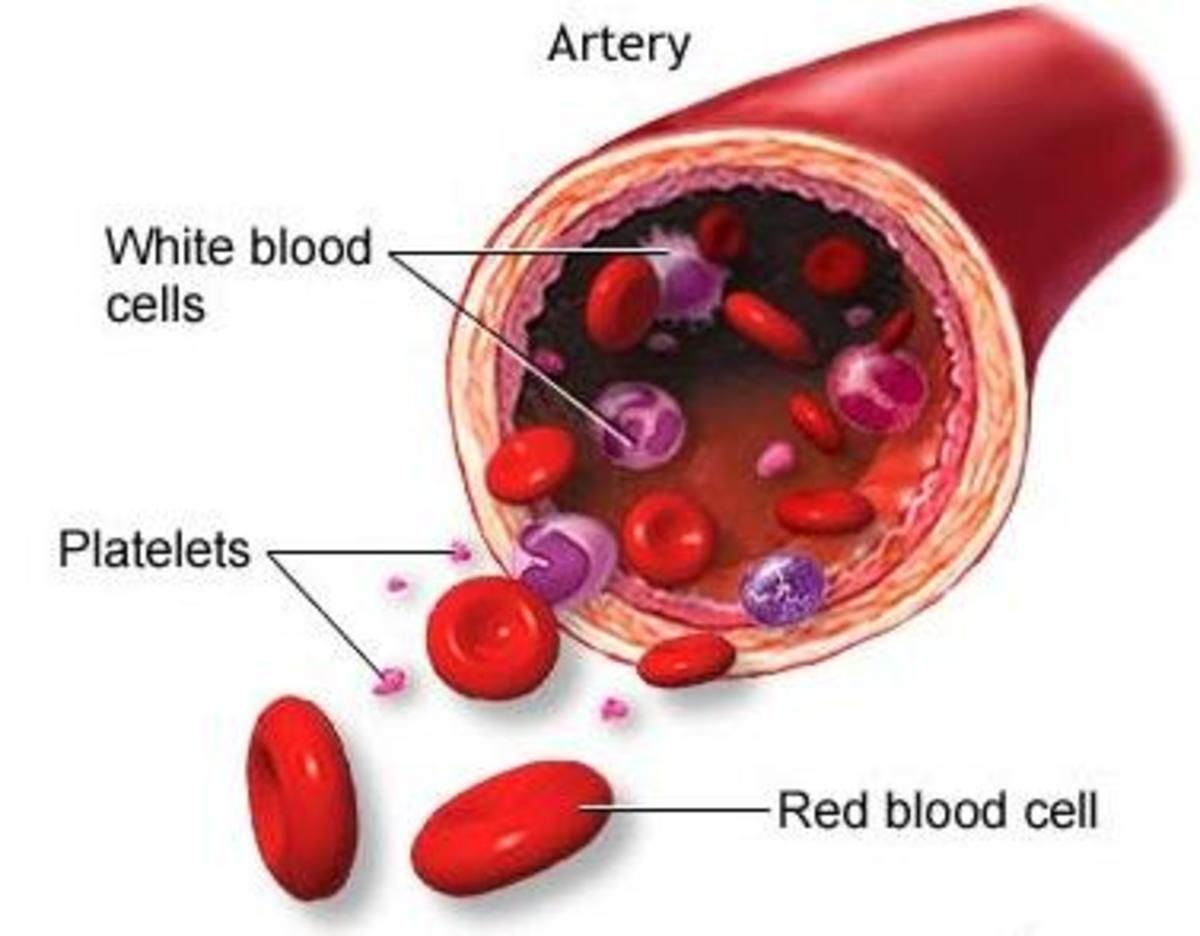
Vascular And Platelet Disorders
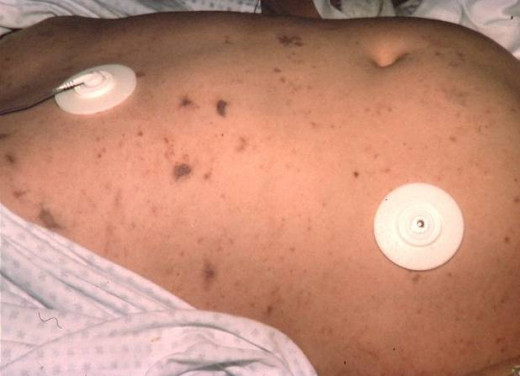
A General Overview
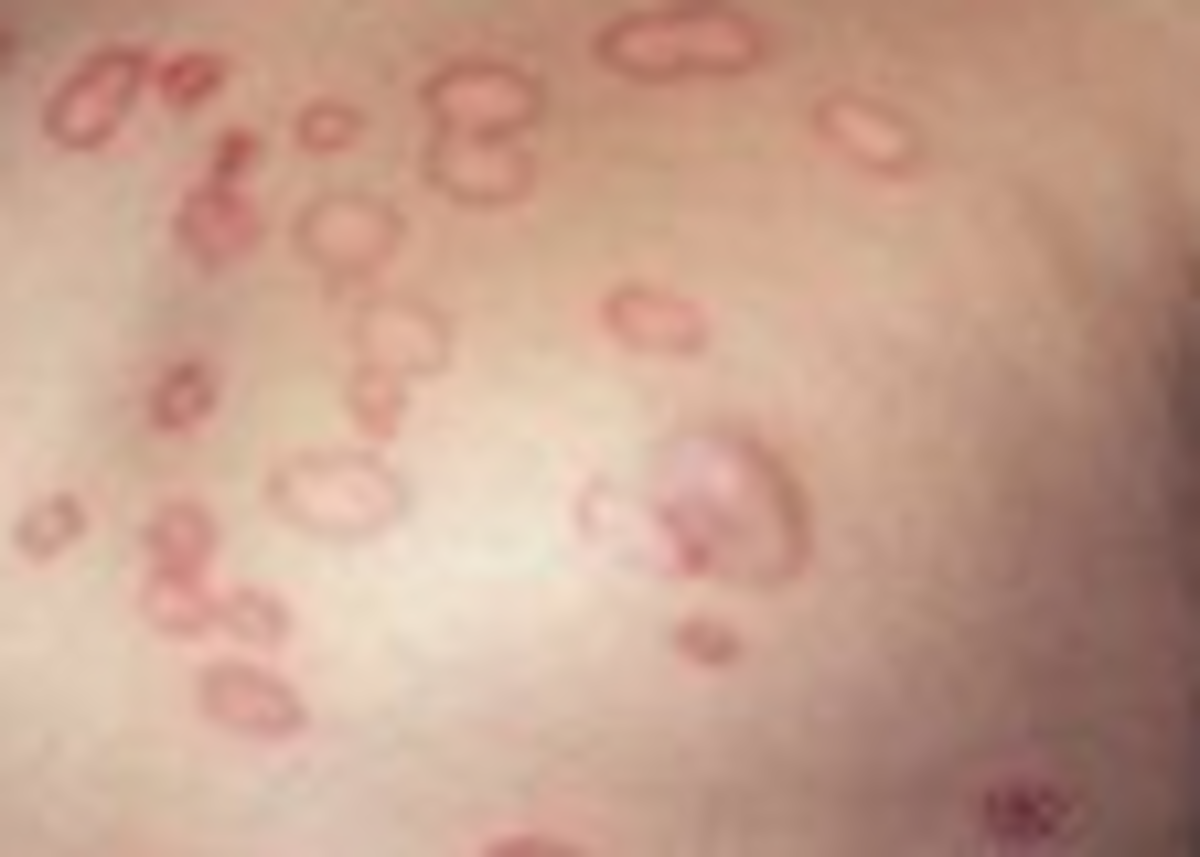
The term purpuric disorder is applied to a hemorrhagic state characterized by bleeding into the skin in the form of dot like purpura, ecchymosis or deep hemorrhages and often associated with bleeding from the mucous membranes of the mouth, nose, gastrointestinal tract, uterus and urinary tract. Purpuras are caused by primary disorders of blood vessels or thrombocytopenia or thrombocytopathy. Purpura has to be distinguished from macular rashes. The former does not blanch on the pressure whereas the latter does.
When the platelet count falls below 100,000/cmm (1010/liter), it is designated as thrombocytopenia. Even at this level, mild bleeding tendency may start, but bleeding becomes pronounced when the platelet count falls below 50,000/cmm. Severe bleeding occurs when the platelets fall below 20,000/cmm. The severity of the bleeding does not always correlate with the degree of thrombocytopenia. Bleeding may be spontaneous or may follow minor trauma. Purpuric bleeding usually stops within 24 hours either spontaneously or on local compression.
Clinical Features Of Thrombocytopenia
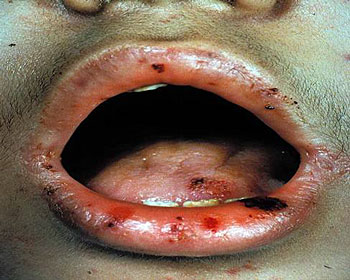
Causes of thrombocytopenia
Thrombocytopenia may result from either diminished production or increased destruction of platelets. In some, both may operate. It may also occur in disseminated intravascular coagulation and massive transfusion of stored blood. The various causes of thrombocytopenia are as follows:
- Diminished production of platelets
- Aplastic anemia, selective hypoplasia of megakaryocytes or inhibition of platelet production by antibodies
- Dyshemopoietic states, e.g. megaloblastic anemia, leukemia, lymphoma, myelofibrosis, disseminated carcinoma and multiple myeloma.
- Heavy alcoholism, (ethanol leads to inhibition of megakaryocytes).
- Increased destruction of platelets
- Idiopathic (immune) thrombocytopenic purpura
- Chronic or acute secondary immune thrombocytopenia following viral infections, systemic lupus erythematosus, lymphomas and chronic lymphatic leukemia.
- Drugs like sedormid, quinine, quinidine, paraminosalicylic acid, sulphonamides, rifampicin, stibophen, digoxin, streptomycin, alpha methyl dopa, heroin, carbimazole, chloramphenicol, tetracycline, mesantoin, troxidone and phenylbutazone.
- Sequestration of platelets eg, giant hermangioma, arterio-venous fistulae, disseminated intravascular hemolysis.
- Dilutional thrombocytopenia, eg, transfusion of massive quantities of stored blood poor in platelets.
Finally, platelet disorders are the result of thrombocytopenia or disorders of platelet function, e.g. those occurring with aspirin treatment and uraemia. Congenital abnormalities of platelet number (e.g. Fanconi’s anemia, Wiskott-Aldrich syndrome) or function (e.g Bernard-Soulier syndrome) are all extremely rare. Increased destruction or decreased production can be differentiated by bone marrow examination, which will show respectively increased or decreased numbers of megakaryocytes (platelet precursors).
Idiopathic Thrombocytopenic Purpura
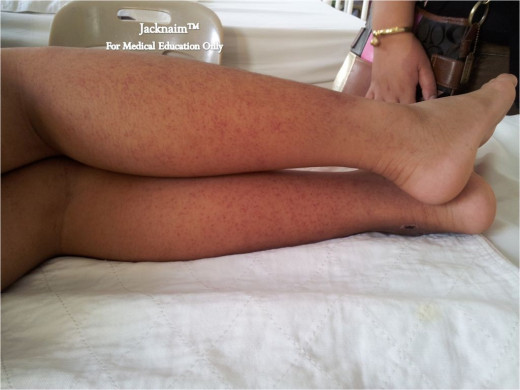
Clinical Manifestations Of Idiopathic Thrombocytopenic Purpura (ITP)
Also called auto-immune thrombocytopenic purpura, or immune thrombocytopenic purpura, this is one of the commonest hemorrhagic disorders seen in clinical practice in places like Ukraine, India, Egypt and America. In the vast majority of cases, antibodies develop which help in destroying the platelets and these antibodies are demonstrable by suitable tests. Though, the exact antigenic stimulus for production of the antibodies is not clear, it is seen that they are directed against many of the components of the platelets. The antibody-coated platelets are sequestrated in the spleen, liver, bone marrow and other reticuloendothelial organs, and selectively destroyed by macrophages. The antibodies are produced in the spleen and bone marrow.
They are IgG in 70%, IgM is 5% and IgG and IgM in 20% of cases. In the circulation, they are attached to the platelets. Lifespan of the platelets is reduced and the reduction is inversely related to the amount of platelet associated IgG. There is compensatory increase in platelet production brought about by increase in the number of megakaryocytes to 3-5 times the normal, but platelet destruction exceeds the renegeration and ultimately the platelet count falls. The antibody has also action in inhibiting the production and release of platelets from megakaryocytes. In the bone marrow, many megakaryocytes are seen to possess hyaline cytoplasma and entire margins, indicating absence of platelet production.
ITP In A Pediatric patient
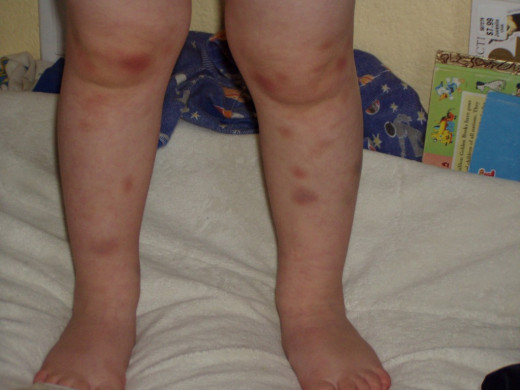
Clinical features
Idiopathic thrombocytopenic purpura (ITP) may occur at any age, but younger subjects are affected more. The disease may present as the acute and the chronic varieties. In chronic ITP, duration of the disease exceeds three months. Acute ITP is more common in children whereas the chronic variety is more common in young women. Both sexes are equally affected below the age of12 years, but after that age, females are affected about four times more frequently than males.
In at least a few cases of ITP in children, purpura may be preceded by an upper respiratory infection or other specific diseases like measles or mumps. The acute form is characterized by rapid onset of bleeding from the gums, purpura, echymosis and bleeding into deeper tissues. Majority of these patients seek medical help within 1-2 weeks of onset. In the chronic form the onset is insidious and the course is prolonged over several weeks or months, sometimes even years, before they seek medical help. Periods of exacerbations and remissions occur. In women one of the common presentations is menorrhagia and intermenstrual bleeding. The monorrhagia tends to be severe and in some cases blood loss may be considerable to necessitate blood transfusion. Due to this complication, ITP tends to be more severe in women than in men.
© 2014 Funom Theophilus Makama