Crohn's, the New Leprosy?
They Are Related
Up until now my articles have been based around what happens in a flare up of the disease and how to treat it. I have not ignored what seems to be the actual cause of the disease: Mycobacterium Avium Paratuberculosis (MAP).
In a recent paper by Ellen Pierce, she makes the strongest case yet for both Crohn's and Ulcerative colitis being simply the result of a MAP infection. By using historical data and etiological connections, she has pieced together a reasonable explanation as to how the disease emerged, spread, how it infects, and even why it infects in different ways.
Mycobacterium avium paratuberculosis is an organism related to Leprosy (Mycobacterium Leprae) and tuberculosis (Mycobacterium Tuberculosis), both of which activate the same genes activated in Crohn's disease. In fact, the phenomenon of looking younger than you really are that is often reported with Crohn's is also reported in another disease: “pretty leprosy (Mycobacterium Lepratosis)”;
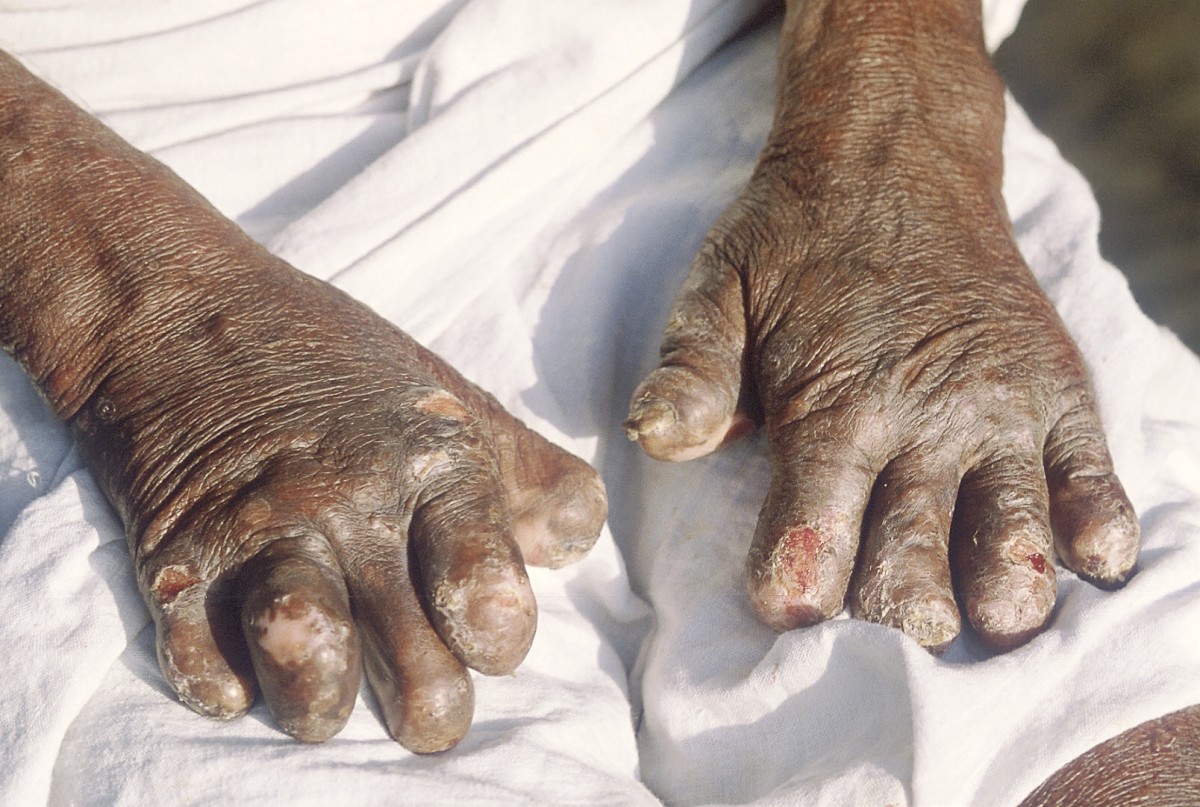
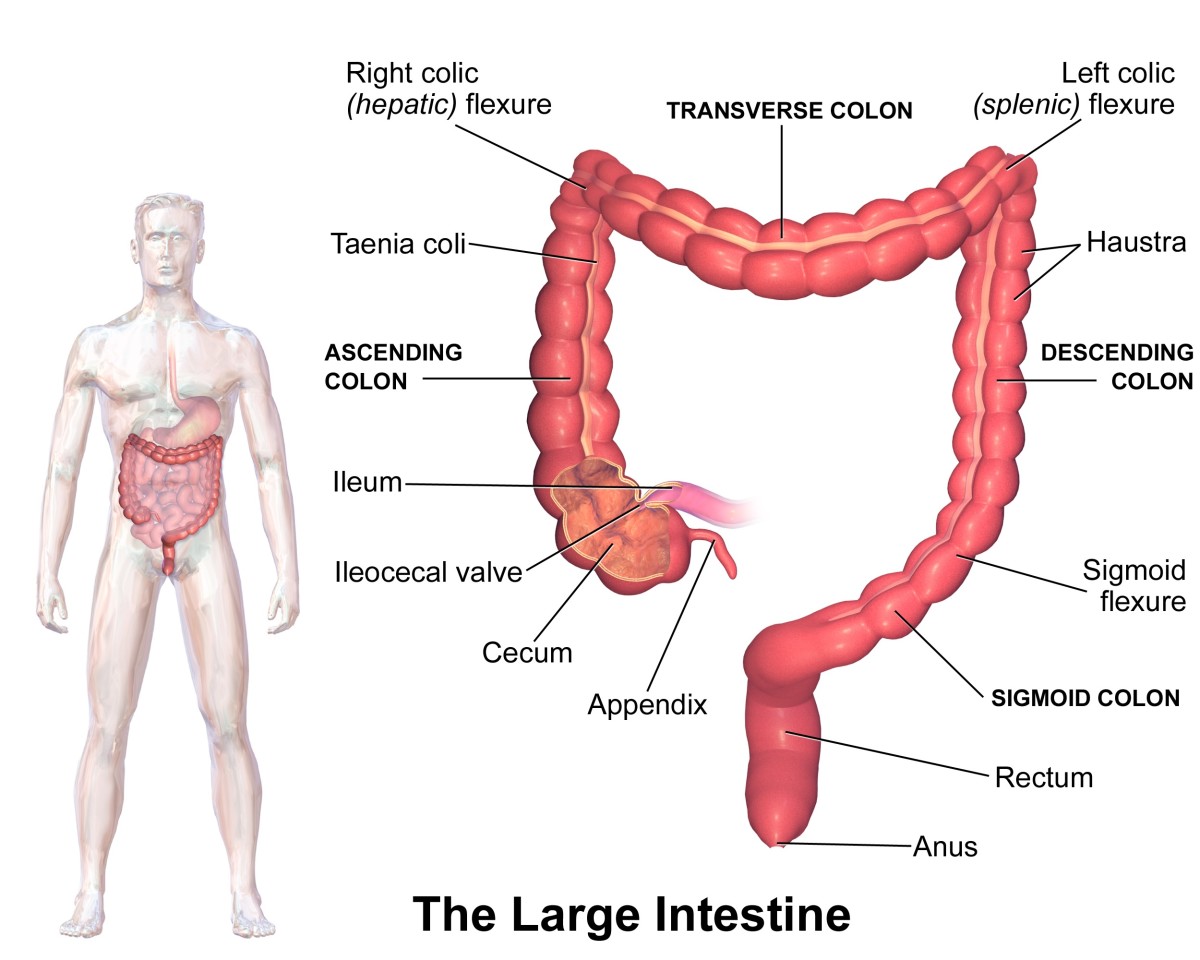
Contrary to folklore, leprosy does not cause fingers and toes to fall off, rather it causes granules to form, much like the “scarring” seen in Crohn's intestines. Furthermore, the withering or “wasting away” often seen in leprosy is usually the result of secondary, opportunistic infections. The MAC (mycobacterium avium complex) has been seen in 60% of the tissues of Crohn's patients (Jeyanathan ,2007).
What is most interesting is that Crohn's and Ulcerative Colitis appeared and spread in the same areas and patterns that Johne's disease had spread 40 to 50 years prior to the emergence of Crohn's. The organism responsible is MAP. While it has not been considered a human pathogen, it can infect herd animals, like cattle, and non human primates. Pierce has shown us that MAT can infect humans via milk and contaminated ground water from farming areas and concentrations of Crohn's seem to cluster in cities and towns with a river that passes through farming country before it reaches populated areas.
One may be tempted to ask the question as to why not everyone in those towns get infected with Crohn's. The answer is very simple: it is a mycobacterium. Just as with other mycobacteria, not everyone is genetically susceptible. It is believed that 95% of the human population is not susceptible to leprosy, so only 5% of the population is actually at risk. In the case of tuberculosis, infections go unnoticed, but only one in ten people will show symptoms, half of those will die if it goes untreated.
One of the problems posed by mycobacterium like MAT is that of their construction. They are neither animal or vegetable, being both a bacteria and a fungus at the same time. Unlike bacteria, mycobacteria have a waxy outer shell instead of a cell membrane. Another problem is that mycobacterium cannot be cultured in the laboratory. They also have very long division times, some up to 2 years!
Another problem is diagnosis. Though studies have isolated MAP in breast milk from Crohn's patients,
linking it to Johne's disease, there is no blood test that has been developed for MAP infections. There could be a study made of the stool of the patient, there is no guarantee that the organism will be present to be identified.
We have come to the point that you may be asking yourself if my previous articles regarding Crohn's
( http://nemobird.hubpages.com/hub/Simply-Crohns-Disease , http://nemobird.hubpages.com/hub/New-Hope-for-Crohns-Patients ) are wrong, the answer is “absolutely not”. In fact, they support the hypothesis posed by Pierce. Mycotoxins in fact, cause elevated levels TNF-a when challenged by other organisms such as Pseudomonas, Candida, and E.Coli. In other words, the immune systems over react in just the fashion that we see in Crohn's.
This is why I have had such success with the Coccoloba intestinal cleanser. The MAP is neither fungus or bacterium, its somewhere in between. Chrysophanol is both antibacterial and anti-fungal in nature. Furthermore, it blocks the production of COX-2 and TNF-a. Historically, other plants bearing chrysophanol have been used to treat tuberculosis and leprosy as well.
We live in a magical era of medicine. We can cure Leprosy and push tuberculosis into remission, so why do we still fall prey to a disease that first affected cattle? The answer is simple: Money. There were few studies done on actually curing MAP infections because after months of treating the animals with antibiotics, there was little chance that these animals would be cleared for meat or dairy production, so it was considered pointless from an economic point of view. Of the few studies conducted, it was found that Azithromycin and Clarithromycin were very effective (both 100%) in vitro,but little data has been done in vivo, especially with humans.
Broad spectrum antibiotics for tuberculosis and leprosy were ineffective. In fact on an anecdotal level, the young lady who inspired me to research Crohn's was treated with Ciprofloxacin at the onset of her disease, which proved ineffective. Against MAP, this is only 55% effective in vitro, and likely less so in vivo.
Even when the mycobacterium is no longer present, an anti-fungal/ anti-bacterial intestinal cleanser such as the Coccoloba cleanser should be beneficial to the patient since the genes to fight the mycobacterium are “turned on” and have been educated to respond to a challenge with high levels of TNF-a, COX-2, IL-1 and IL-6.
I have traveled a long and tiring road of research to come to this destination. I feel confident that this is the end of my journey as far as Crohn's is concerned. To the Crohnie's in the world, God bless you. If you would like the intestinal cleanser which was so instrumental in alleviating symptoms of the hell that is Crohn's, please do not hesitate to contact me.
Sincerely,
Thomas Greenwell