Cry for Breath: A Case of Pneumonia in the Newborn
When one sees a newborn child for the first-time, only a very few souls are about to resist the urge to quickly jump on it. The most instinctive reaction is to hug and snuggle the poor bastard until he/she struggles to be released from the loving arms of their close relatives, friends, and family members. In the process, the unwary adults are exposing the neonate with significant risks to develop all forms of infection. Many consider newborns as small fragile human beings who are very vulnerable to their environment. True enough, they can be considered as small adults who are nearly a little bit too unready to face the world they have been just put into. Among the most notorious culprits targeting the newborn’s developing (and incapable) immune system are the infections in which adults, usually carelessly, expose them into. Atop the list of this infections is the Neonatal Pneumonia.
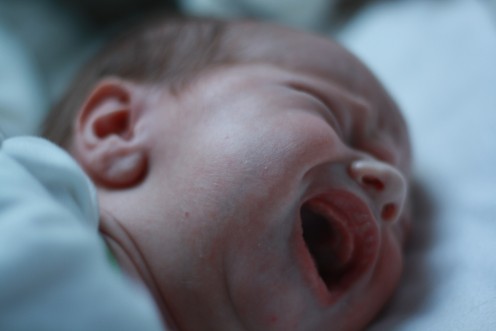
The Cry Baby
Here is a case of Baby R., a five day old male neonate who initially presented for consultation for excessive crying.The parents reported that the infant has been crying incessantly over a span of 12-18 hours with only a few short breaks just after they were sent home from the birthing clinic. He is the third child of the of his parents; the couple expressed that they were quite contented that the delivery and birthing process went well. They were not first-time parents and were capable to identifying common causes of infant cry, but even after their usual troubleshooting the patient was still continuously showing signs of crying. It was noted that certainly, something was wrong with the child since he acted strangely just recently and was well during their stay the hospital.
Upon examination, it was seen that the patient had a small elevation in body temperature and, a normal heart rate, and a slightly elevated respiratory rate. He was able to breastfeed well, with good sucking. There was slight pale discoloration around the lips; the chest was also slightly showing signs of in-drawing. Aside from this, the rest of the physical examination was unremarkable.
Disambiguation and Delineation of the Presentation
First things first, the terms neonates, infants, and newborns should be given delineation. Medically speaking, neonates are those who are less than a month of age, while infants are those less than a year of age: hence, neonates are considered as a subset of infants, but with special needs of their own. Newborns is a colloquial term which encompass vague identification for children ranging at these ages.
The initial presentation of the patient was excessive crying early less than 48 hours after birth. Aside from a preliminary period of apnea (period without breathing) during the time of birthing, the patient’s manifestations were unremarkable. The mother reported that the patient had good sucking and was able to breastfeed adequately. There was no jaundice (yellowish discoloration of the skin), meconium stain (passage of infant’s first stool to the amniotic fluid), or respiratory distress upon birth.
Crying is a common denominator for a variety of illnesses, ruling out apparent causes of hunger, sleepiness, tiredness is the first step in identifying the cause of crying. For febrile infants without a focus of infection, the management should be based on guidelines of sepsis work up. ‘Guidelines for sepsis work-up’ pertains to a set of protocol usually followed by a pediatric department to manage cases that are suspected for sepsis. In general, sepsis is defined as an infection which has spread to the bloodstream. Hence, it is very severe since the pathogen can cross anatomic borders and cause system-wide infections. Sepsis treatment is usually the initial choice for ambiguous causes of disease for the simple reason of being thorough is better than being sorry.
The Death Toll
Every year nearly 41% of all under-five child deaths are among newborn infants, babies in their first 28 days of life or the neonatal period. Three quarters of all newborn deaths occur in the first week of life.
- Partnership for Maternal, Newborn & Child Health, 2011
Head to head: Pneumonia and Sepsis
As in this case, since the patient has no identifiable symptoms aside form crying, and slight variations in respiration and temperature—the sepsis protocol may be considered. Based from the onset of symptoms and the possible severity of the differential diagnoses, neonatal pneumonia and neonatal sepsis are the main problems that may be addressed initially.
Neonatal pneumonia is the primary diagnosis because the patient presents with tachypnea (increased breathing rate) which may signify a respiratory problem. Unlike infants and children, neonates do not always present with fever, and the lung sounds typical of pneumonia may not be present until the later course of the disease. The usual predisposing factors for early onset pneumonia such as premature rupture of membranes, infant prematurity, or meconium aspiration are not present in this case. However, it is notable that the patient was apneic (not breathing) during the first three minutes and the midwife opted to resuscitate the patient through mouth to nose resuscitation. This may be an entry point of possible pathogen.
Pneumonia, is basically an infection of the respiratory tract; in which may be divided into the upper and lower parts. In children and in adults, common colds, and cough are considered upper respiratory tract infections (URTI) while those affecting the lungs and its airways such as bronchitis, and lobar pneumonia are labelled as respiratory tract infections (LRTI). Usually, the pathogens are isolated where they initially infects, however in neonates, the immune system is still underdeveloped and the structures are too close together hence infections usually enter the lower tract with an increased capacity to wreak havoc.
Neonatal sepsis may be considered also, but it does not manifest with the usual signs and symptoms such as weakness of crying, reduced sucking, loose limbs, hypothermia/ cold to touch, vomiting or abdominal distension, umbilical sepsis, and chest indrawing.
Pneumonia is the leading infectious cause of death in children worldwide, accounting for 15% of all deaths of children under 5 years old. The disease killed an estimated 935, 000 children under the age of five in 2013!
— World Health Organization, 2013Diagnostic Tests to Confirm the Diagnosis
In support of the clinical signs and symptoms several laboratory diagnostic tools may be employed in identifying bacterial infections in neonates. A chest radiograph may be requested to identify possible infiltrates, however this is non-specific in some cases because it is dependent on severity of the pneumonia and the immune response which is not yet fully developed during the first few days as in this case. Second, blood culture may be requested to identify a possible pathogen in the blood and to rule out sepsis. It is important to facilitate the proper antibiotic treatment if empirical therapy of antibiotics will not help the patient.
Even though the pathogen is not isolated, complete blood count which show elevated WBC counts and/or serum markers with elevated CRP and ESR may identify an ongoing infection. The white cell count differentials may help point out the non-specific class of infectious agent as well.
How are patients with pneumonia treated?
Empirical treatment should be initiated for the patient. That is, initial dosages of broad-spectrum antibiotics may be given even though the organism is not yet isolated. This may then be shifted to another more specific type once the pathogen is already ascertained. This method ensures that the patient may already have a head start for the protection of spread of the bacteria.
The management is dependent on the severity and age. For all febrile neonates, as seen in this case, all patients should be hospitalized and should be started with empirical antibiotic therapy as early as possible. In one protocol, an initial management of ampicillin, cefotxime, or gentamycin should be initiated to cover for the usual pathogens such as Group B streptococcus, and E. coli. In hospital management with intravenous antibiotics with supportive therapy is highly warranted in suspected cases of neonatal pneumonia and/or sepsis since it is the leading cause of mortality in this age group.
Supportive therapy may be given if the patient manifests with dehydration during cases of febrile episode and poor feeding. Isotonic intravenous therapy or D5IMB solution may help sustain the patient during the acute phase of the illness.

The Preemptive strike was successful!
After a few rounds of antibiotic therapy, the patient has responded and has shown significant reduction in morbidity. His infection may have been caught at an early stage. The pneumonia has not progressed to affect the whole respiratory tract or progressed to sepsis. He was discharged from the hospital within a week.
Other Useful Articles
- Meningitis in Infants- Another case describing meningitis, a common disease in this age group. The review features an infant initially presenting with non-specific symptoms. This article provides insight on how to diagnose the disease with emphasis on characterizing seizures.
References
- Arumugam, J., Sivandam, S., & Vijayalakshmi, A. M. (2012). The evaluation and management of an incessantly crying infant. Sri Lanka Journal of Child Health, 41(4), 192–198.
- Bang, A. T., Bang, R. a., Reddy, M. H., Baitule, S. B., Deshmukh, M. D., Paul, V. K., & de C. Marshal, T. F. (2005). Simple Clinical Criteria to Identify Sepsis or Pneumonia in Neonates in the Community Needing Treatment or Referral. The Pediatric Infectious Disease Journal, 24(4), 335–341. doi:10.1097/01.inf.0000157094.43609.17
- Duke, T. (2005). Neonatal pneumonia in developing countries. Archives of Disease in Childhood. Fetal and Neonatal Edition, 90(3), F211–9. doi:10.1136/adc.2003.048108
- Freedman, S. B., Al-Harthy, N., & Thull-Freedman, J. (2009). The crying infant: diagnostic testing and frequency of serious underlying disease. Pediatrics, 123(3), 841–8. doi:10.1542/peds.2008-0113
- Rappaport, D. I. (2009). Community-Acquired Pneumonia in Children. Hospital Physician, (October).
- Zaidi, A. K. M., Ganatra, H. a, Syed, S., Cousens, S., Lee, A. C. C., Black, R., … Lawn, J. E. (2011). Effect of case management on neonatal mortality due to sepsis and pneumonia. BMC Public Health, 11 Suppl 3(Suppl 3), S13. doi:10.1186/1471-2458-11-S3-S13
© 2015 LM Gutierrez