Diabetes Cure: Is There A Cure For Diabetes?
Diabetes Cures... The Good, Bad and the Ugly
If you are one of the millions of Americans who have recently been diagnosed with Type I or Type II diabetes, otherwise known as diabetes mellitus, you may be wondering if a cure currently exists for this potentially deadly disease. If not, is a cure close at hand? What is the current state of medical research into the cause and potential cure? These are a few of the questions that I hope to answer for you. This is by no means an exhaustive or comprehensive look at every possible path that research is currently taking, but it will give you a quick, realistic overview of where science currently stands in the fight against diabetes today.
First, the bad news. No. There is currently no "cure" for diabetes. Although we will cover a number of existing and possibly future treatments here, there is no magic pill or potion that currently exists to cure the disease. The good news is that diabetes is rapidly becoming one of the most heavily researched diseases on the planet today, which greatly improves the odds for eventually finding a potential cure.
Diabetes: Treatment vs. Cure
Although there is a tremendous amount of scientific research being done today on diabetes, the exact cause of the disease is currently unknown. Until the base cause of diabetes becomes known, there is little chance that an actual cure will be developed. There are no credible claims currently being made of any pending one-time treatment to eliminate the disease without the need for surgical transplant, and it is highly unlikely that such a treatment will be developed any time within the next 10-20 years.
The vast majority of research being done on diabetes today is conducted by pharmaceutical companies. Very little research being conducted today by these companies is in search of an actual cure. Most research money is currently being spent on finding new and improved treatments for the disease. The reason for this is twofold. First, our current medical knowledge concerning how the disease works is at such a basic stage that it is unlikely such a research project would produce a genuine cure within a reasonable amount of time. Few businesses, or even individuals, would be willing to begin work on a project that had such a low probability of succeeding in their own lifetimes. It would be financially irresponsible for any pharmaceutical company to embark on such a venture, knowing that it would almost certainly lead to continuing financial losses with no chance for recovering their investment realistically in sight. Such a venture would likely be in direct conflict with the legal duty of corporate officers to work in the best interests of their shareholders, who could hold such officers both financially and criminally liable for their actions. This is not only the nature of corporations, it's also the law.
The second reason is simple economics. Pharmaceutical companies stand to make very little money from curing any type of disease. This is especially true of any disease that would be as difficult to find a cure for as diabetes. Drug companies generally make profits by developing and marketing treatments, rather than cures. Treatments do not cure disease. They merely treat the symptoms and/or slow down the disease's progression. Generally speaking, the more serious the disease, the more desperate patients are for any type of treatment that may improve the condition. Chronic, debilitating illnesses, such as diabetes, are extremely lucrative markets to develop treatments for, since there is not only a high demand among patients but because these treatments are generally needed for a patient's entire lifespan. Demand from such a "captive audience" provides a strong incentive for researchers to create drugs and devices that will extend the lifespan of their customers as long as possible without actually curing the underlying problem. Unfortunately, this is one trade-off of living in a supply and demand economy. If and when a cure for diabetes is to be found, it will most likely be the product of government-funded research or private studies.
Diabetes Treatment: Current Options
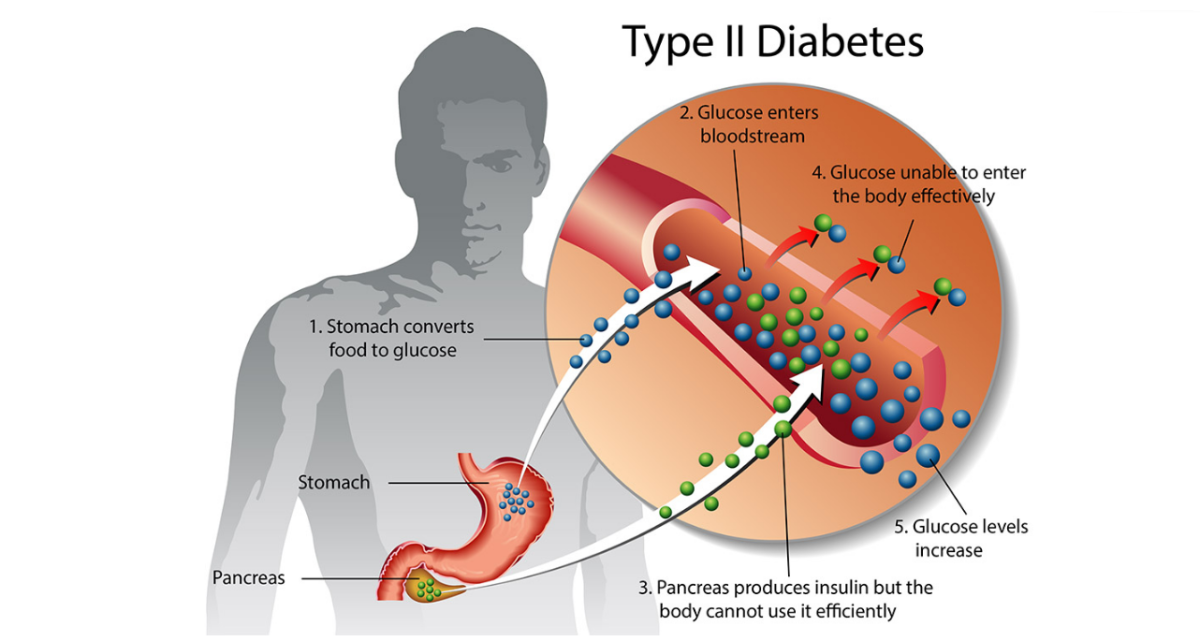
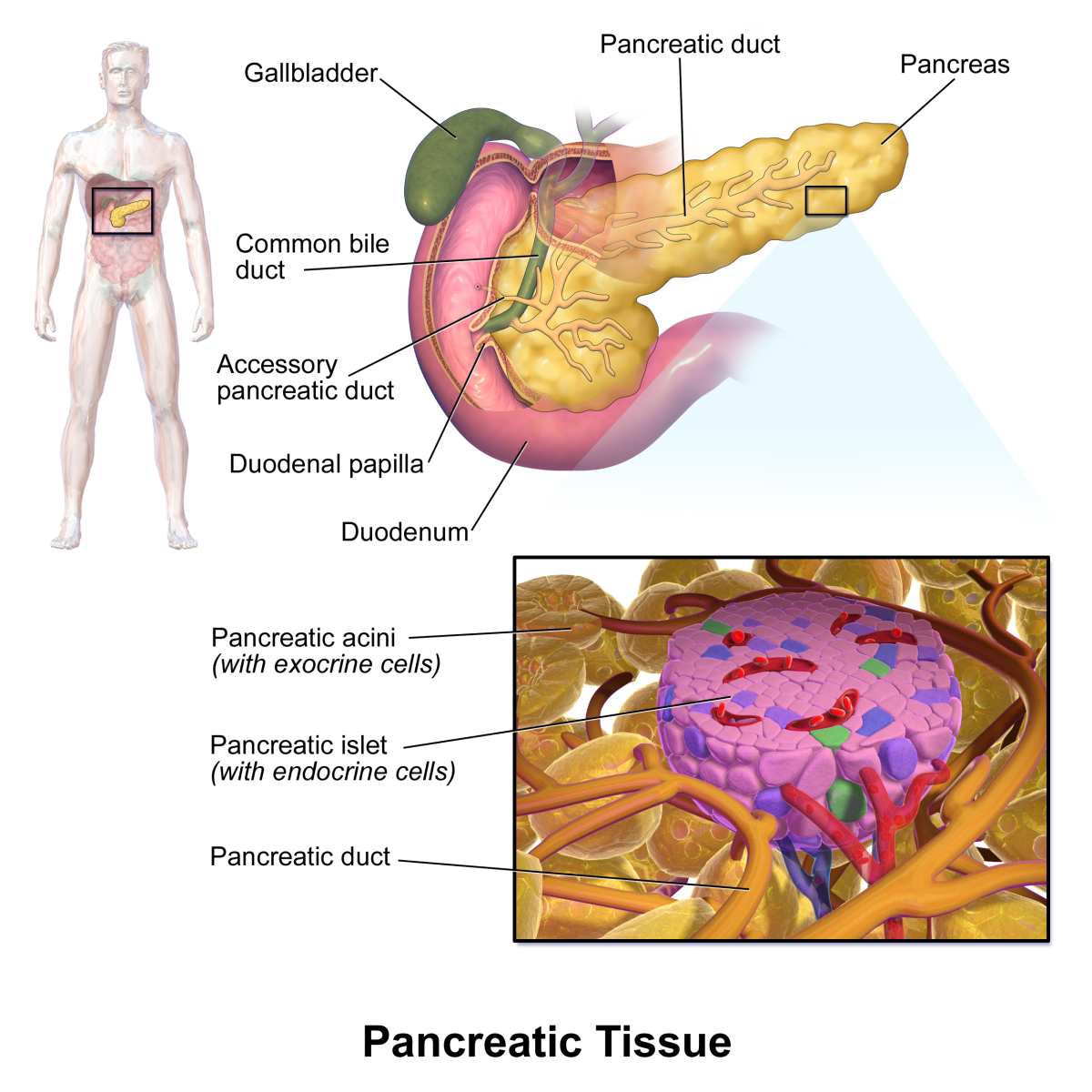
The vast majority of diabetics today are treated with either prescription medications in the form of pills, or injections of proprietary formulas that contain synthetic versions of insulin. Insulin is a hormone that is naturally produced by one's own pancreas and needed to regulate blood glucose levels in the bloodstream. Pills are most often prescribed to Type II diabetics, who are less severely affected than Type I diabetics. Type I is often referred to as insulin dependent diabetes, since patients are unable to survive without regular injections of prescription insulin formulas. Type II diabetes can often be treated with pills that simply amplify the effectiveness of insulin naturally produced by the pancreas. Type I diabetics have a pancreas that produces little to no insulin naturally. Injections of synthetic insulin replace the insulin normally made by one's own body. Type I diabetics generally must take injections of synthetic insulin for the rest of their lives. Injections of proprietary, synthetic insulin are NOT a cure for diabetes, and they come with a long list of potentially deadly side-effects.
Videos On Natural Diabetes Treatments
Natural Remedies For Diabetes
Although it is not currently known what causes diabetes, it is generally well-accepted theory that poor diet, lack of exercise and obesity dramatically increase one's chances of developing the disease. While there are obvious genetic factors at work, one can greatly reduce their chances of developing diabetes by eating a healthy diet, getting regular aerobic exercise and keeping one's weight at a healthy level.
The association between diabetes and food intake has launched a number of "diabetes diets", some of which claim to actually reverse diabetes itself. Although it is presently technically impossible to reverse (or cure) diabetes, stringent attention to diet alone has been known to stabilize the blood glucose levels of some diabetics to the point where a patient no longer requires any type of prescription medication or insulin injections to obtain effective blood glucose control. Although a number of patients have shown very promising results on such diets, to date, there have been no widely-accepted, peer-reviewed studies proving that diet modifications alone can "reverse" diabetes or permanently achieve blood glucose level stability.
Unfortunately, there seems to be no current consensus in the medical community on what type of diet is best for diabetics. In fact, two of the most popular diabetes diets are at exact opposite ends of the spectrum. For example, Dr. Richard K. Bernstein, a leading expert in the treatment of diabetes research and inventor of the modern blood glucose monitor, stresses the need for a high-protein, moderate fat diet. According to his theory, carbohydrates, especially simple carbohydrates, are to be avoided in order to maintain optimum blood glucose levels. Dr. Bernstein's books are some of the best selling in the diabetes industry, and he cites numerous success stories in his practice.
On the other side of the aisle is the "raw food" movement. Sometimes called "live food" or "living foods", this diet stresses an all-vegan diet, devoid of any type of meat, dairy, eggs or other animal products. This relatively new phenomenon has been famously depicted in the documentary film Simply Raw: Reversing Diabetes In 30 Days. It has been embraced by such authors as Gabriel Cousins, M.D., Dr. Gary Null, Dr. Joel Fuhrman and Dr. Neal Barnard. The documentary, in particular, shows rather dramatic results in normalizing the blood glucose levels of six individuals who are put on a strict vegan diet for a period of 30 days. These included both Type I and Type II diabetics. All were able to obtain vastly improved or even normal blood glucose levels while simultaneously quitting all (or nearly all) of their diabetes medications, including insulin. However, it is unclear from the documentary whether the effect of this diet is permanent or simply temporary. The static nature of documentary films does not tend to provide a long-term "big picture".
The final type of popular diabetes diet is the one most widely accepted in today's medical community as well as the one recommended by the American Diabetes Association. Unlike other diets though, this one does not make any promises about being able to stop taking diabetes medications in order to stabilize blood sugar levels. It is simply a standard low-glycemic diet. It stresses a diet of foods that are low on an indexed scale. The scale's numbers are frequently different, based upon what source you obtain them from, but the general idea is that foods which raise one's blood sugar levels the fastest are high on the scale (avoid) and foods that do not spike one's blood glucose levels are low on the scale ("good" foods).
Although this may be the most widely accepted diabetes diet in use today, it doesn't work for everyone. Different individuals seem to react differently to certain foods. This makes basing one's diet on numbers found in a book (especially when most books differ considerably in their index figures) a shaky proposition, at best. The diet works excellent in a purely theoretical sense. It has very mixed results outside of the laboratory though. Unfortunately, most who recommend this diet fail to mention the dangers of assuming that everyone responds to foods the same way, and that there is currently no standard in the scientific community for obtaining values for any particular version of the glycemic index. Several books have been published with greatly varying glycemic index figures, all of which are based upon controlled studies using a very limited number of test subjects. No single, defacto study has emerged as a benchmark thus far.
It can take literally years to determine how one's own blood glucose levels react to every single type of food. This is what is genuinely needed in order to determine what is a proper low glycemic diet for each individual though. The difficulty in properly obtaining data to customize a low-glycemic diet is most likely the reason that simpler, alternative diabetes diets have become so popular among diabetics (if not the medical community) in recent years. They are simple to follow and give almost immediate results. They will either work, or they won't. Why these diets work for some, and not others though, is currently unclear.
Medical Implants, Insulin Pumps, Automated Insulin Injections
One of the latest trends in the treatment of diabetes is the increasing use of medically implanted insulin pumps. The number of younger Americans who suffer with Type I, or juvenile diabetes, using these devices has skyrocketed in recent years. What makes these devices so popular with diabetes patients is the end of painful and exhaustive blood glucose monitoring and insulin injections. The job of insulin pumps is to automatically monitor blood glucose levels and inject precise amounts of insulin through a tube or syringe implanted into the body and connected to an external electronic device. One's blood sugar levels dictate the amount of insulin to be injected by the unit. The patient needs only make sure that the external unit is supplied with adequate "refills" of insulin.
At least, that's how it is supposed to work. In reality, many patients have found these devices to be inaccurate in their readings and can actually keep their blood glucose levels lower through traditional blood glucose monitoring and insulin injections. These units are currently in their infancy as a form of treatment, are extremely expensive (units start at around US$6,000) and often sound much better in theory than they operate in practice. Results vary greatly from patient to patient.
Regardless of how well these units may work, they are by no means whatsoever a cure for diabetes, just a high-tech form of treatment. The devices do not address the problem of insulin resistance at all and their long-term affects on diabetes patients (especially children) will take many years to become fully understood. While it may make the disease less inconvenient for some diabetes patients, they are at best an intermediary technology that will most likely become irrelevant in the next 10-15 years.
Yet Another recent development in diabetes treatment is a proprietary medical device called an "OmniPod". Although it closely resembles an insulin pump in many ways, the company stresses in it's literature that it is NOT, in fact, an insulin pump. The main difference between this device and an actual insulin pump is the fact that it uses a device called a "pod", which is what actually releases insulin into your bloodstream. The pods affix to your body via a "sticky" backing that will adhere to one's skin for approximately 3 days, after which a new pod must be placed on the body. The pod has a small needle integrated into it that actually releases the insulin, which you manually sill with a syringe (see photos to the right). The release of insulin is completely controlled by an external (unattached) electronic device that determines how much insulin should be released through the use of an integrated blood glucose monitor and test strips, which must be checked manually, just as with any other type of blood glucose monitor and test strip.
This is more a convenience device than anything else. It is probably less cumbersome and painful than a standard insulin pump, but may not be as full-featured. That stands to reason, since insulin pumps cost upwards of $6,000 and the OmniPod "starter pack" retails for approximately $700. Unfortunately, the starter pack is much, much cheaper than the ongoing cost of using the device.
First, you need to buy the actual insulin, with syringes to inject them into the pods. Second, you will need to purchase enough test strips to check your blood glucose levels regularly. Since it uses an integrated Freestyle brand meter, the test strips needed are generally more expensive than that of a number of other brands. Third, you need to buy a regular supply of pods, which must be replaced every 3 days. If our math is correct, this means that you will need to purchase approximately 10 pods each and every month. We checked around online for how much these pods can be purchased for via mail order, and the best deal we found was $396. The RETAIL price of 10 pods (a month's supply) is $619.45.
As far as we can tell, the ONLY feature this device has that you can not accomplish yourself manually using a blood glucose monitor, test strips, syringe or pen-type insulin injector and a small chart showing what amount you should be injecting yourself with for any given blood glucose level, is that the OmniPod automatically calculates the right amount and injects the insulin for you automatically. Instead of injecting yourself with a needle on a regular basis, you basically have a needle inserted into you continuously that must be replaced every 3 days. Like insulin pumps, this is definitely no "cure" for diabetes, or anything remotely resembling it. If you have a GREAT insurance plan, it may be a more convenient form of insulin treatment than regular injections, but it's use beyond that seems fairly limited.
Natural Diabetes Treatment Books
A Diabetes Cure In Supplements?
There have been a number of claims made in recent years as to the benefit of supplementing one's diet with a variety of vitamins, minerals, spices, tea leaves, extracts and other substances in order to improve blood glucose regulation. Among the most popular supplements in use today are cinnamon and chronium picolinate.
A very limited number of proper studies have been done on supplements commonly marketed as being "proven" to help regulate blood glucose levels in diabetics. Studies on cinnamon, in particular, have been largely inconclusive. Many of the studies produced conflicting results and no consensus seems to exist as to a standard dosage, species of cinnamon used, means of cinnamon bark extraction, purity or even the basic conditions under which the studies are conducted. The most commonly cited study "proving" that cinnamon is beneficial to diabetics was conducted in Pakistan, and has come under increasing scrutiny in recent years due to the inability of scientists to reproduce the same results in similar conditions. The American Diabetes Association has issued a "warning" to consumers not to rely upon cinnamon in particular to help treat diabetes.
There are currently no supplements being marketed today which are conclusively proven to help regulate blood glucose levels in diabetics. There are definitely no natural "cures" for diabetes in the form of a pill, tea or supplement, and many of the studies cited in literature for these supplements are highly suspect. The most attractive lure of these supplements is that they are made from ingredients that are generally very inexpensive and easy to find at any local supermarket. It is still possible that these supplements may one day be proven by science to be beneficial in the treatment of diabetes though, and since none of these supplements have proven to be harmful in any way, they may be worth investigating by individuals as to whether they are helpful as supplements to their own diets.
Transplant Technology May Cure Diabetes
Perhaps the most promising medical development to date for finding a cure to diabetes is a surgical procedure developed by Dr. Camillo Ricordi at the Diabetes Research Institute at the University of Miami Miller School of Medicine.
Dr. Ricordi made headlines in December 2009 when it was reported that his transplant procedure had been successfully used by Walter Reed Army Medical Hospital in Washington, D.C. and the University of Miami to cure a wounded soldier of diabetes.
In this instance, an American soldier had been wounded in battle, resulting in the near total destruction of his pancreas. Without a pancreas, the soldier would have become permanently diabetic and required daily insulin injections for the rest of his life. A handful of cells from the soldier's destroyed pancreas were used to generate healthy islet cells that were surgically attached to his liver.
Though the soldier still, technically, has no pancreas, his body is producing insulin and he is today free from diabetes.
This particular procedure, known as an islet allograft, has been performed successfully in excess of 700 times since 1990, when it was first developed. Due to the fact that the transplant procedure uses cells from one's own body, the chances of rejection (which is the most common problem with any type of transplant) are minimal. It is currently a complicated and expensive procedure that is reserved for Type I diabetics with few other options available to them. The procedure is growing in popularity though and may one day be a common surgery used to permanently cure patients of diabetes. Of all the research into cures and treatments for diabetes, this one seems to hold the most immediate hope for a real cure.
Diabetes Cures: In Conclusion
When it comes to diabetes, an ounce of prevention is genuinely worth far more than a pound of cure.
However, there have been a number of promising developments in recent years, giving diabetes patients a growing number of options to choose from. Although transplant surgery is currently the best cure we have for the disease, such procedures are not frequently available as an option to most diabetes patients.
Unfortunately, the main barrier to developing a cure for diabetes is the same as with most diseases. Money. Much more money is being pumped into developing more effective treatments for diabetes by pharmaceutical companies than is being spent on trying to find a cure. Until the paradigm between profit motive and doing what is best for those who suffer from disease is solved, it is highly unlikely that any type of medication will be invented that cures diabetes without the need for procedures such as surgical transplants.
Updates
Due to new policies implemented by HubPages, I have had to remove all informational links that were available here previously. This is despite the fact that all URLs on the page linked to government websites, universities, physicians or non-profit organizations. Hubpages would not specify which (if any) link on this page was "bad", so it was impossible to determine what it was they wanted corrected. Thus, all of them had to be removed. There will be no further updates to this page as a result.