Dangerous Eye Complication of Juvenile Arthritis: Uveitis

A few Thanksgivings ago, my great-niece, who suffers from juvenile arthritis and has a history of eye complications known as uveitis, woke with eye pain. While her mom stayed home with the rest of the family her father and uncle wisely drove her to the emergency room where her ophthalmologist was going to meet them because they knew that a delay in treatment could lead to blindness for my niece.
All parents whose children have been diagnosed with juvenile arthritis need to be aware that eye pain or reduced vision requires prompt treatment. Although there are many disorders that are associated with uveitis, this article will stay focused on the association between juvenile arthritis and uveitis.
Touching Video About JRA & Uveitis
Facts About Juvenile Arthritis
Almost 300,000 children under the age of 18 have been diagnosed with juvenile arthritis in the United States and many more children from around the world also suffer from juvenile arthritis. It is a chronic disease and the symptoms are generally felt in the child's joints as pain, swelling and stiffness. The most commonly affected joints are the child's knees, hands and feet. The symptoms may worsen in times of flare-up, may remain steady or may sometimes go away during times of remission.
Facts About Uveitis
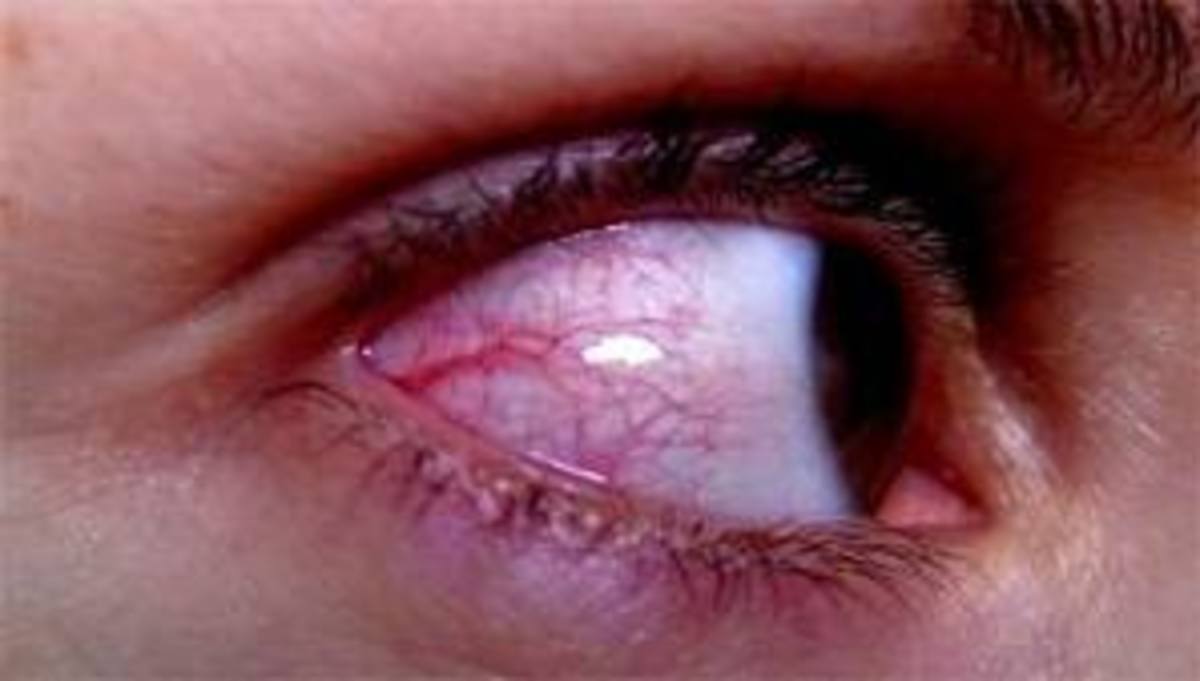
Children who have juvenile arthritis are at risk for developing uveitis. Uveitis is the inflammation of the middle layer of the eye. The middle layer consists of the iris (colored portion of the eye) and the lens of the eye (back part of the uvea). If uveitis isn't diagnosed and treated early, the child is at risk for glaucoma, cataracts and permanent visual damage that can lead to blindness in one or both eyes. However, diagnosis can be difficult because the child may not experience symptoms until the eye is already damaged. Once symptoms do occur the onset may be rapid and include: blurred vision, dark floating spots, eye pain and sensitivity to light and redness of the eye(s). Uveitis is most treatable when detected early which is why frequent eye screenings in children who have juvenile arthritis can be critical to saving their sight.
If the inflammation occurs in the iris, the condition is referred to as iritis.
New Study Reveals Unexpected Findings About Uveitis in Children With Juvenile Arthritis
A recent study led by Dr. Saurenmann was done by a team of international researchers and published in the June 2010 issue of Arthritis and Rheumatism. Dr. Saurenmann and her cohorts found that 13% of the 1081 children in the study eventually developed uveitis.
Dr. Saurenmann's study may lead to changes in the most current pediatric guidelines because the findings of her international research team suggest that kids diagnosed with juvenile arthritis before age 5 should get eye exams every three months until 7 years after their diagnoses, which is more frequent than the current recommendations. Some other significant findings of this study that differ from what has been previously believed are:
- The specific kind of arthritis that a child has (called a subtype) doesn't seem to correlate with the child's risk of getting uveitis (although there were a few exceptions).
- Girls seem to be more at risk of developing uveitis than boys especially when the girl was younger than two when first diagnosed with juvenile arthritis.
- Age at diagnosis of juvenile arthritis is correlated with increased risk of uveitis, especially for girls.
What Parents Need to Know About Juvenile Arthritis and Eye Exams
In an article that appeared in Arthritis Today, which is published by the Arthritis Foundation, the chief of pediatric rheumatology at Johns Hopkins Children's Center, Dr. Edward Sills, stated that he was familiar with the Saurenmann study and feels it detected important points that practitioners need to be aware of. But he cautioned that kids who do not fall into the Saurenmannn high risk groups should still be having their eyes screened. Dr. Sills' advice to parents of all children diagnosed with rheumatoid arthritis is to have their children's eyes examined by an ophthalmologist at least twice a year and even more frequently if their child is in the higher risk groups identified by the Saurenmann study. This is vital because early diagnosis of uveitis can allow effective treatment which can help maintain normal vision and minimize the risk of complications from uveitis possibly preventing blindness.
Treatment and Prognosis for Uveitis
Treatment and prognosis (future outcome) will vary depending on which part of the uvea is affected. If it is the iris the condition is called iritis and treatment consists of dark glasses, eye drops to dilate the pupils to relieve pain, and steroid eye drops to alleviate inflammation. With proper treatment for iritis, the condition will usually clear up within days or weeks, but may recur in the future.
If the back part of the uvea is affected, powerful anti-inflammatory medicines called corticosteroids and the use of antibiotics may be required. This is a more serious eye condition and the inflammation may last from months to years with the potential for permanent vision damage despite treatment. Possible complications may include cataracts, fluid within the retina with or without retinal detachment, glaucoma and vision loss.