- HubPages»
- Health»
- Women's Health»
- Pregnancy
Dealing with Gestational Diabetes
As I am progressing further into my pregnancy, I realize that any time now, I will be administered the oral glucose tolerance test. This is typically done between weeks 24 and 28, and I have heard this is rather unpleasant, as it involves drinking (and keeping down!) a healthy serving of something that tastes like Kool-Aid that didn't have quite enough water added to it.
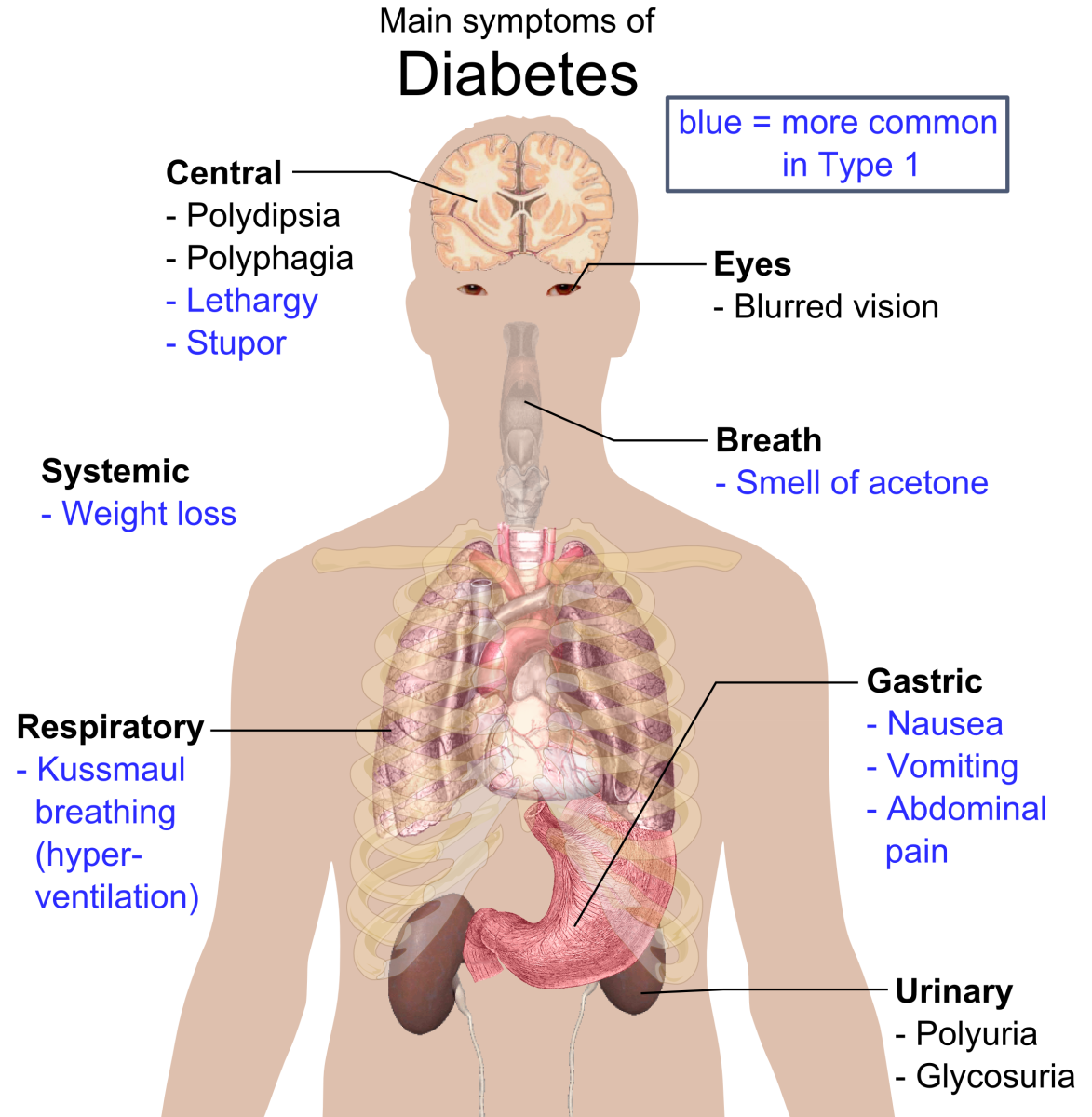
This test will be used to determine if I have gestational diabetes. Like regular diabetes, gestational diabetes means that a patient has hyperglycemia, or high blood sugar. "Gestational" refers to pregnancy, so basically this is diabetes that begins during a woman's pregnancy.
Why is gestational diabetes such a concern?
Gestational diabetes can lead to excess weight gain, not only in the mother but in baby as well. Delivering an abnormally large baby puts the mother at risk for complications during child birth, including the chance of an emergency cesarean section. Unplanned cesareans tend to have more complications than those that were planned ahead of time. Overall, gestational diabetes can also lead to a higher risk of stillbirth.
Dealing with diabetes during pregnancy also leads to an increased chance of the mother developing regular diabetes within 5-10 years after having their child. Having gestational diabetes can also cause the mother to develop hypertension (high blood pressure). High blood pressure can lead to complications such as an early delivery or the life-threatening pre-eclampsia.
It is very important not only to get tested for this condition, but also keeping it under control at all times. You can test your blood sugar levels at home with a glucose meter (a normal reading, without fasting, runs in the low to mid 100's range), cutting down on foods with a lot of sugar and white flour. Although it seems odd to have a pregnant woman on a diet, your doctor may prescribe you do so. It is also important to exercise, just make sure that you do not over exert yourself.