Diabetic Retinopathy: Identifying, Preventing and Treatment
What is Diabetic Retinopathy?
If you or a loved one is living with diabetes, you are probably most concerned about complications related to the disease including potential loss of limbs and loss of vision. Diabetic retinopathy is an eye disease that is often diagnosed in patients with uncontrolled high blood sugar and/or other difficulties in managing their diabetes. Blurred vision is common and, if left untreated, blindness ultimately may occur. Surgery may even be necessitated to remove an eye significantly damaged by retinopathy.
Proper management of diabetes requires consultation and regular appointments with a variety of specialists, sometimes called a "diabetes team." This includes your internal medicine doctor or pediatrician, an endocrinologist, nutritionist and an opthamologist (total eye care doctor).
I have had diabetes since 2003. Even though I have never worn corrective lenses, I see my opthamologist each year so that he can monitor my eyes for early signs of diabetic retinopathy. As discussed in this hub, by the time symptoms of the disease are detected by the patient, significant damage may have already occurred.
Prevention and early, continuous monitoring are key.
Please note that the information in this hub is not a substitute for professional medical advice. Be sure to see your doctor with any questions or concerns!
Statistics and Facts About Diabetic Retinopathy
- Diabetic retinopathy is a leading cause of blindness in the United States
- It is a progressive disease, which often develops over 10 years or longer
- Between 40-45% of Americans diagnosed with diabetes have some stage of diabetic retinopathy
- An estimated 80% of Type 2 diabetics develop the disease
- Smoking, high blood pressure and high cholesterol may make diabetic retinopathy worse
- Early stages of the disease are usually undetected by the patient because they do not experience any changes in vision or pain
- 90% of the cases of diabetic retinopathy could be caught before complications develop simply with annual comprehensive dilated eye exams
- Even if you develop proliferative retinopathy, the risk of blindness can be virtually eliminated with timely treatment
Why are Diabetics Prone to Retinopathy?
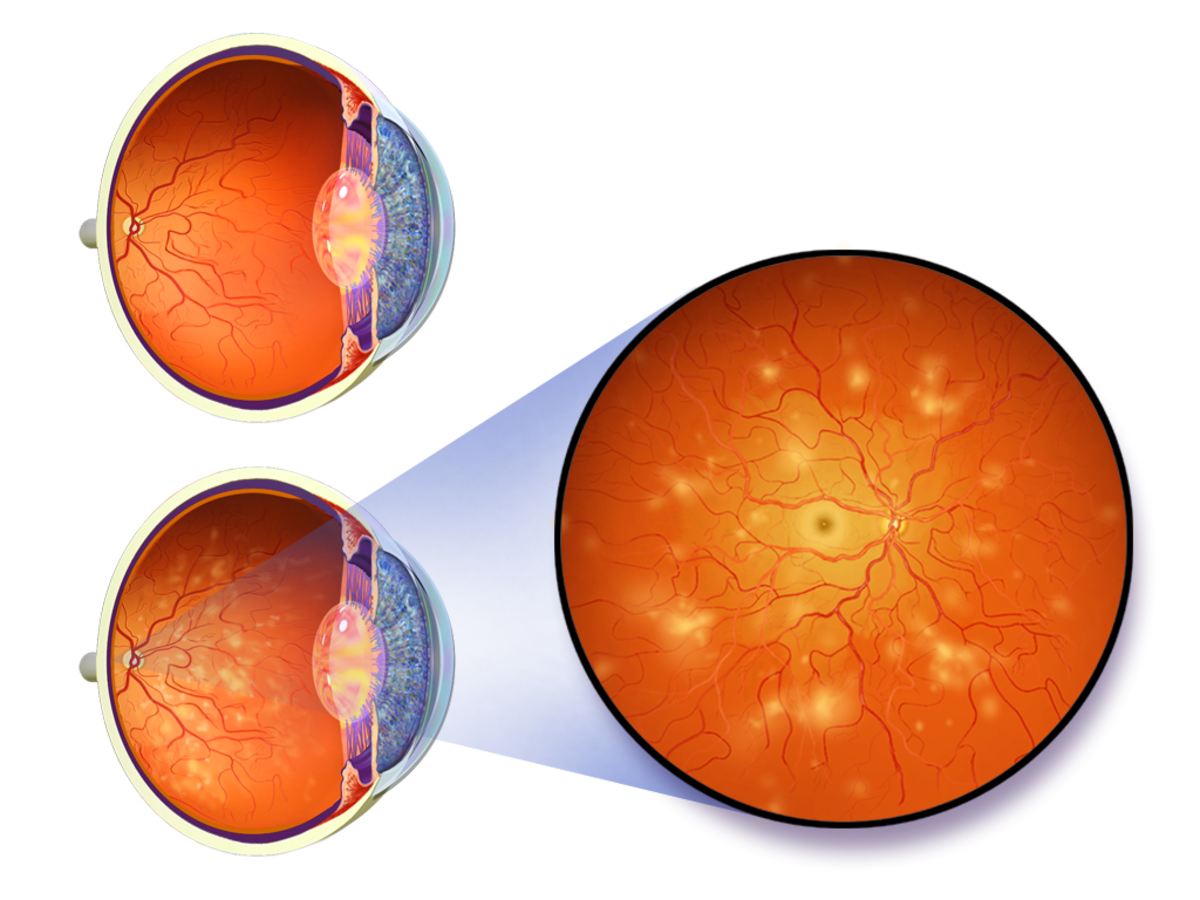
There are a number of different causes of retinopathy, from radiation exposure to prematurity in infants. It can result from damage to the retina, which is the innermost part of the eye and communicates light and images via the optic nerve to the brain. Without a properly functioning retina, eyesight is impaired, and blindness may even occur.
Diabetic retinopathy, like other forms of the disease, can be diagnosed by an opthamologic eye exam. People with diabetes often have blood sugar levels outside of a normal, healthy range. Frequent high blood glucose causes dehydration as the body works to "flush out" the excess, unused sugar. The blood itself changes its viscosity, becoming thicker, and resulting in both slower healing of abrasions/skin lesions and damage to blood vessels in diabetics.
Among the smallest vessels in the human body are those in the eyes. Damage to retinal vessels from high blood sugar can cause inflammation, swelling and leaking fluid. Some diabetics also suffer from high blood pressure, which also contributes to progression of the disease. With fluid in the center of your eye, significantly blurred vision results. The tiny blood vessels become progressively blocked, if blood sugar levels remain at unhealthy levels, further damaging the retina via starvation.
At its most advanced stage, diabetics may experience growth of new, abnormal blood vessels on the retina, called proliferative retinopathy. The blood vessels do not nourish the eye, but rather are prone to rupture and bleeding. Scar tissue may develop, as well. At the extreme, the optic nerve may be damaged, preventing images from the retina to be transmitted to the brain for sight. Oftentimes, it is too late to save functional vision at this late stage.
A Doctor Explains How Diabetes Affects the Eyes
What Will You "See" in the Stages of Diabetic Retinopathy?
Keep in mind that early stages of retinopathy may be present without any impact to vision and thus, undetectable without regular full, dilated eye examinations by an opthamologist.
When diabetic retinopathy progresses to the point that blood vessels in the eye break, the patient will experience vision affected by dark spots, known as "floaters" because the blood is blocking light from reaching the retina for proper vision.
As the blood vessels heal, scar tissue may form, pulling the retina itself from its proper position in the eye. This process may distort vision, or even lead to more significant vision loss if areas of the retina become detached.
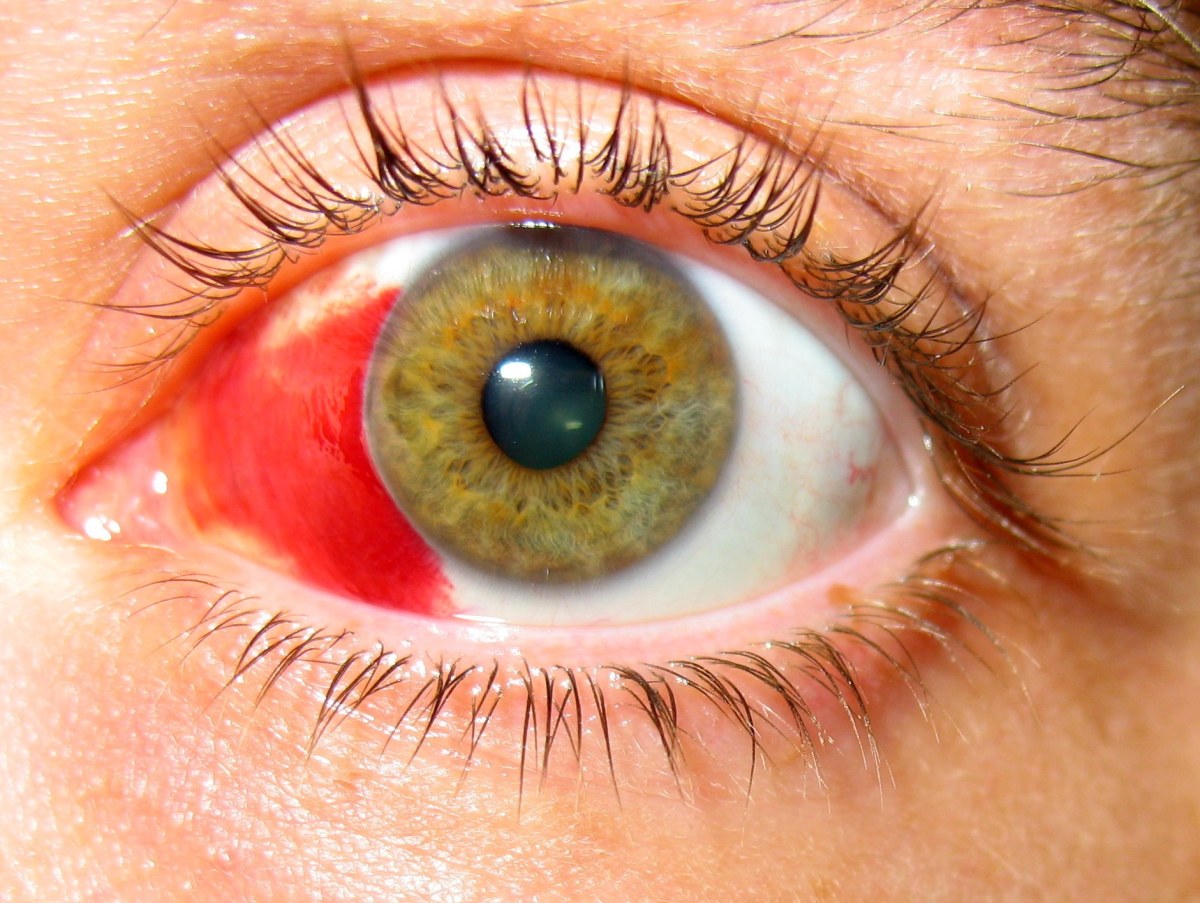
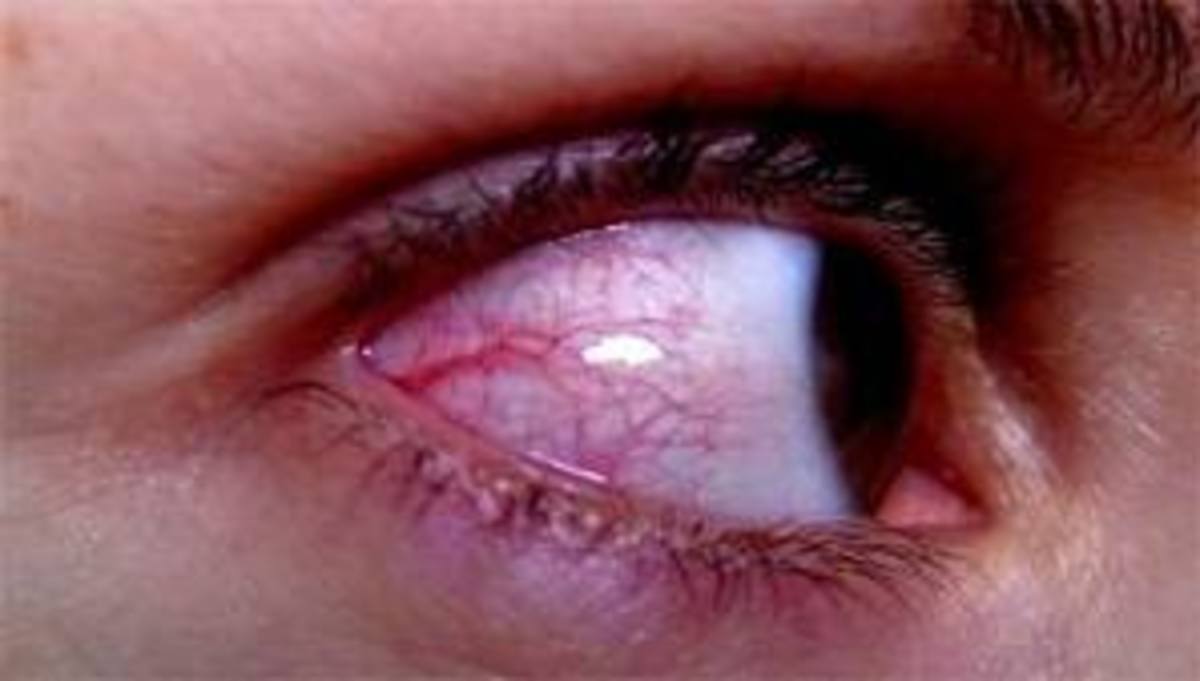
Some diabetics experience retinopathy so advanced that new blood vessels can even occur in the iris, and visible to anyone looking at the patient's face. They may block fluid from flowing out of the eye, causing pressure to build up and damaging the optic nerve, which sends signals from the retina to the brain where images are processed as sight.

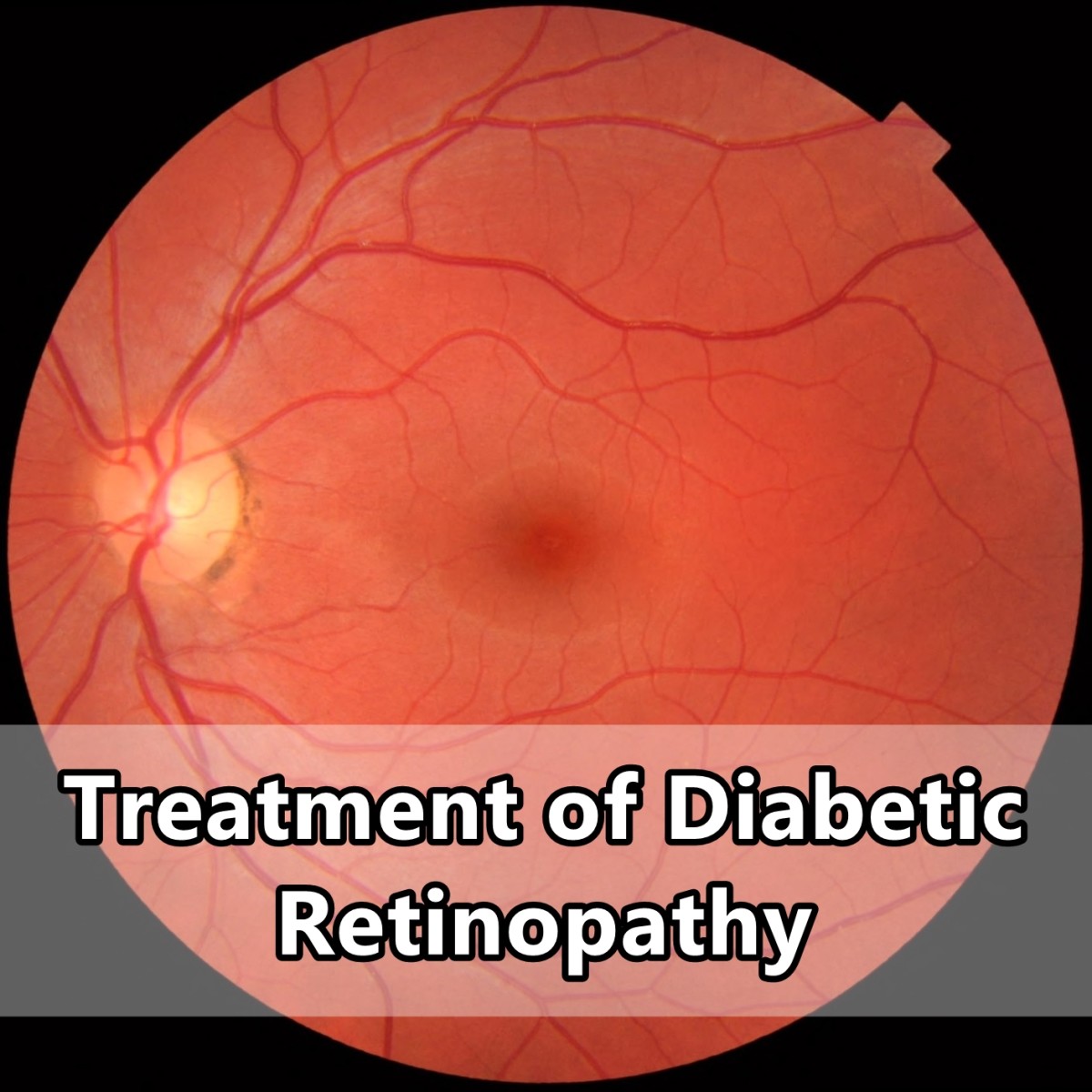
Diabetic Retinopathy: Treatment and Prevention
Do You or a Loved One Have Diabetic Retinopathy?
Can Diabetic Retinopathy be Treated or Reversed?
The good news is that, in most cases, diabetic retinopathy can be treated/controlled, especially if caught early. To avoid developing the disease, tight blood sugar control is necessary. It goes without saying that a motivated patient who follows a good diet, tests blood glucose regularly, exercises and schedules required doctor visits is less likely to develop diabetic retinopathy or any other diabetes complications.
Good blood sugar levels will slow the progression of the disease, as well, even if you have been lax in your diabetes care in the past. Talk to your opthamologist and endocrinologist for guidance specific to your medical condition.
By the time vision has been affected, or lost to some degree, reversal of diabetic retinopathy is more challenging. A variety of surgeries may be considered, including laser surgery, if your opthamologist suggests such measures.
Once again, the two things that are largely within any patient's control when it comes to this disease are: (1) ensuring that they receive annual comprehensive eye exams and (2) managing blood glucose levels with the help of medical professionals!
This content is accurate and true to the best of the author’s knowledge and does not substitute for diagnosis, prognosis, treatment, prescription, and/or dietary advice from a licensed health professional. Drugs, supplements, and natural remedies may have dangerous side effects. If pregnant or nursing, consult with a qualified provider on an individual basis. Seek immediate help if you are experiencing a medical emergency.
© 2013 Stephanie Marshall