Diagnosing Anthrax Through X-ray Pictures: Different Radiographic Representations Of Anthrax
Doctors With X-rays
Introduction
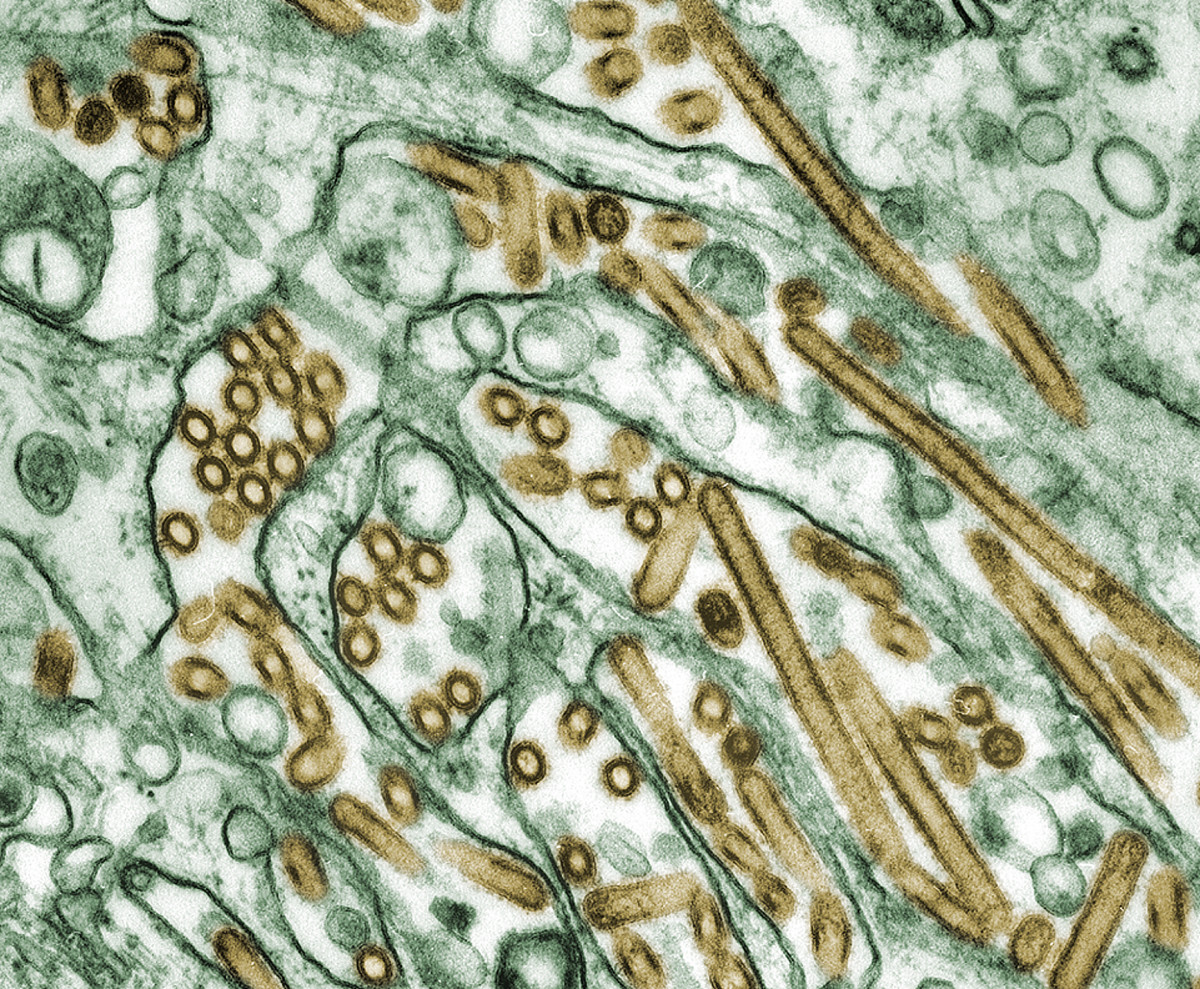
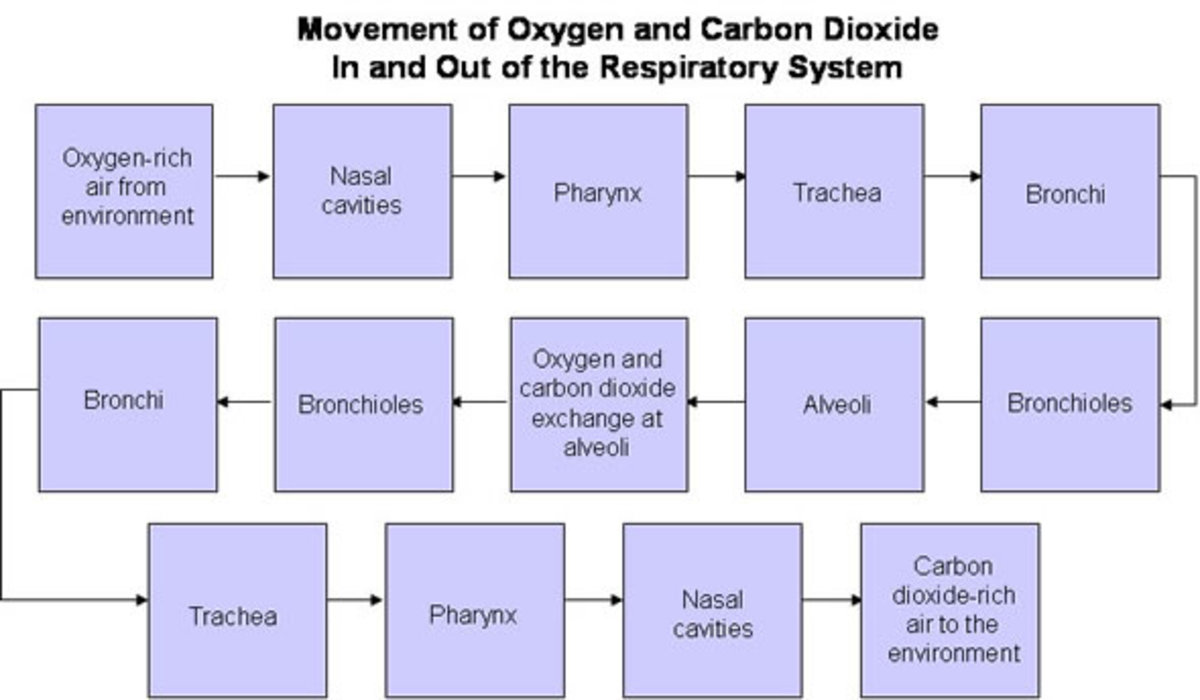
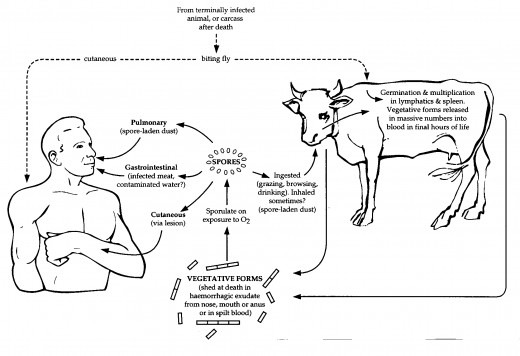
This Hub is centered on showing just the X-ray diagnostics of Anthrax as there are a million articles on Anthrax already. Anthrax is caused by the Bacteria, Bacillus Anthracis. Anthrax manifests as a multi-organ disorder. What this means is, it does not just affect the respiratory system but other systems and organs. Most notable of such are the digestive system and skin.
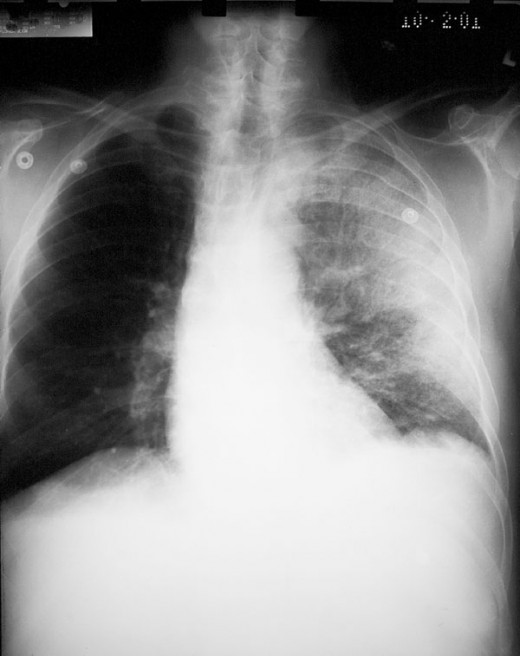
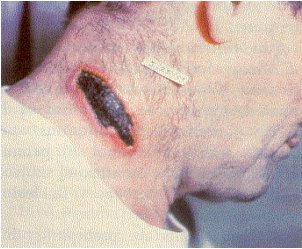
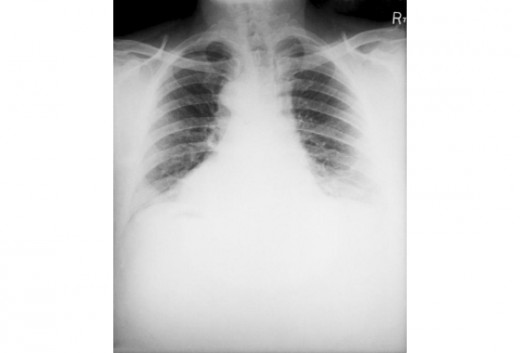
So, in this hub, photos showing its pulmonary effect and cutaneous effect would be displayed.
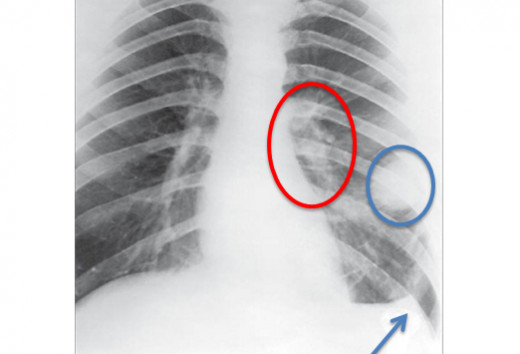
Anthrax On X-ray
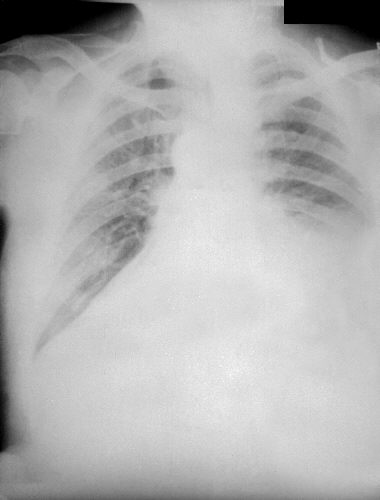
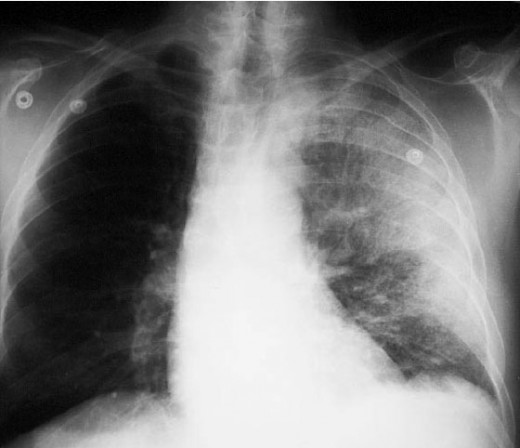
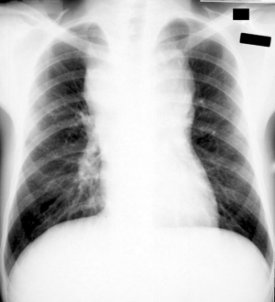
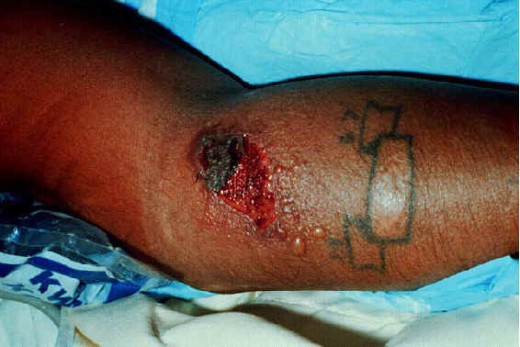
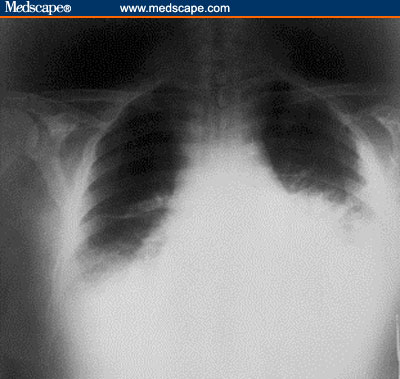
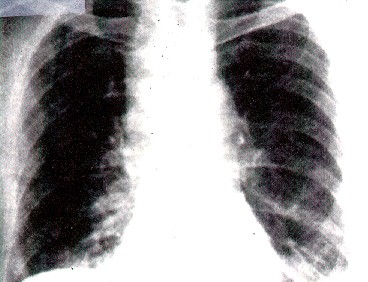
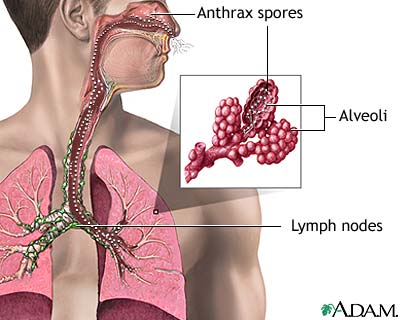
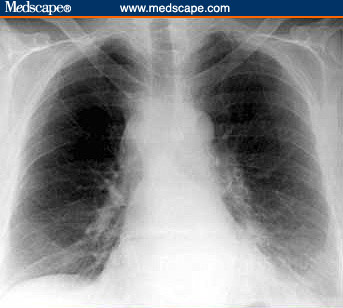
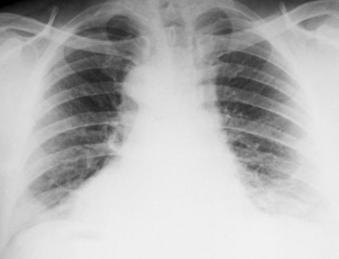
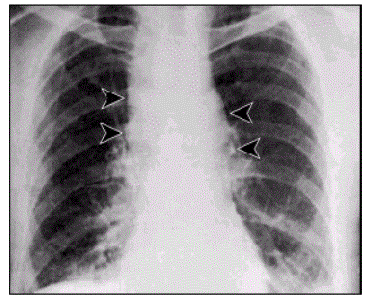
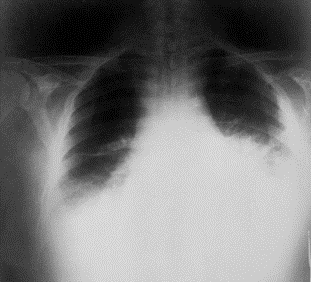
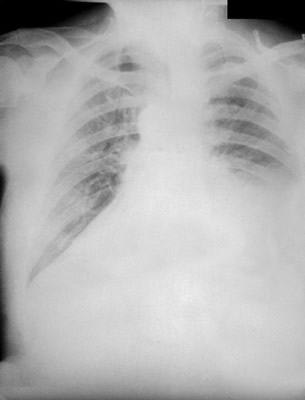
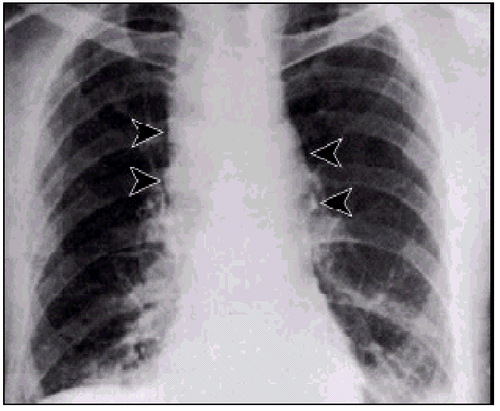
References
1. All X-ray photos here are from DFM E-Group, in the photo and X-ray section.
2. Notes and explanations: Wikipedia, Essentials of Clinical Medicine by Kumar and Clark's, Medicinenet and Mayor's Clinic.
© 2014 Funom Theophilus Makama