Diagnostic Features And A Careful Management Plan Of Chronic Renal Failure Patients
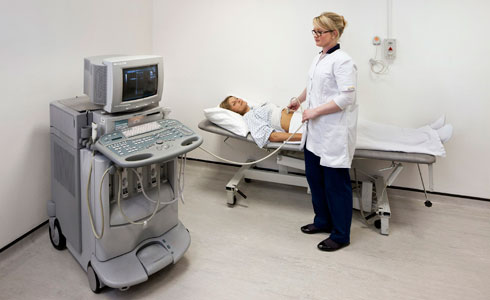
Ultrasonography Of Kidneys
A General Overview
Diagnostic features include biochemical analysis of blood (which is the main), urine analysis, radiology and ultrasonography.
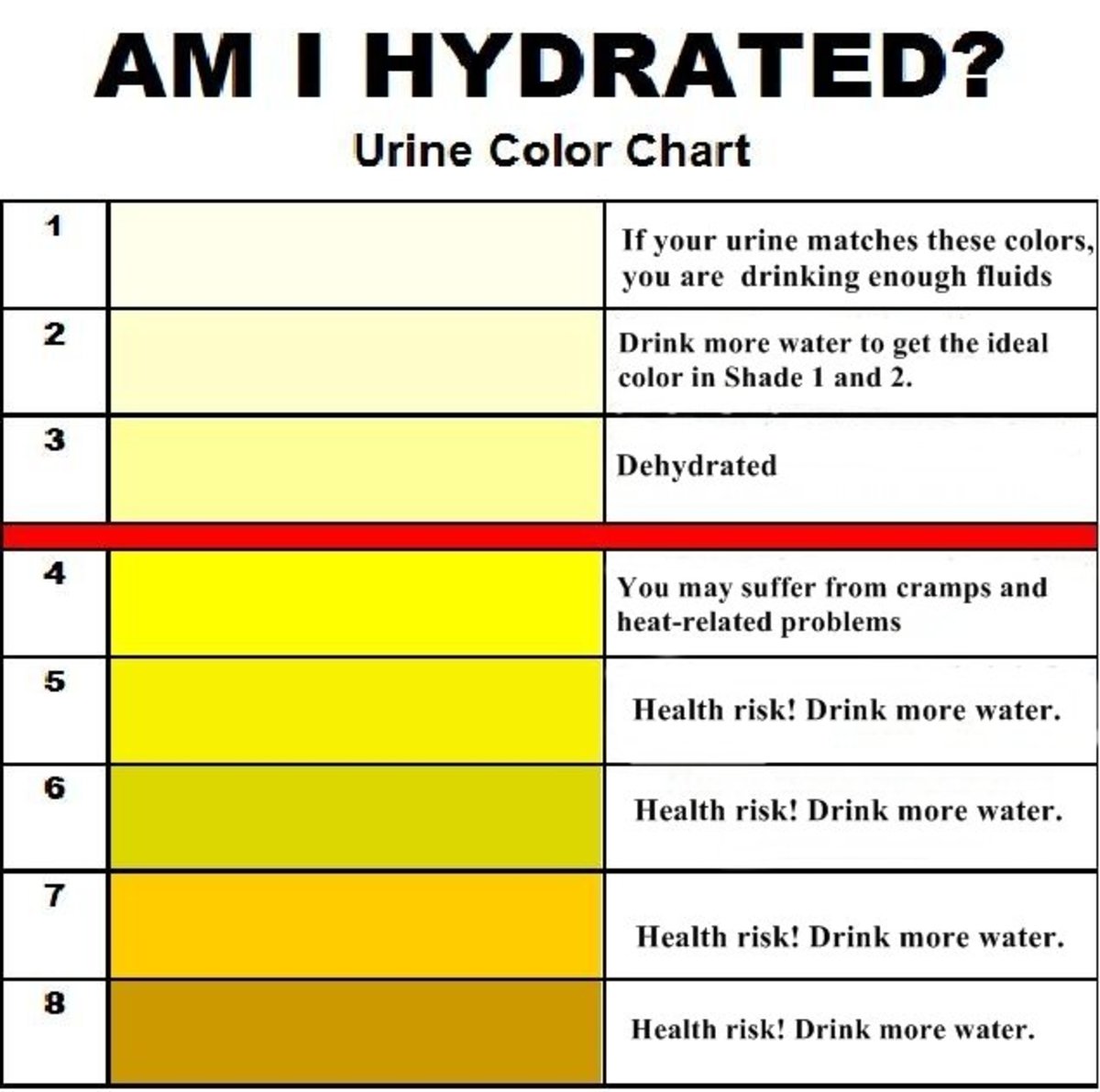
Urine Analysis: Volume is high (2-3 times in 24 hours). Mild proteinuria may be evident. The most remarkable feature is the fixed specific gravity around 1010 (isosthenuria) and an osmolality of 300 mOsm/Kg water. The presence of broad casts in urine confirms the chronic nature of the illness. The estimation of urinary loss of sodium helps in identifying salt-losing states. Blood urea, serum creatinine, serum uric acid and inorganic phosphates are elevated. Calcium and bicarbonate levels are reduced.
Radiology: Plain X-ray of the abdomen may help in revealing the small size of the kidneys.
Ultrasonography: This is another elegant method used in assessing the renal size. If the kidney size is normal, a renal biopsy may help in arriving at the precise histological diagnosis. Function of individual kidneys can be studied by split renal function tests.
The level of serum creatinine correlates with the degree of renal functional impairment as assessed by creatinine clearance. Serial estimations of serum creatinine values therefore, are of great help in assessing the progress of the disease.
Management Of Patients With Chronic Kidney Failure
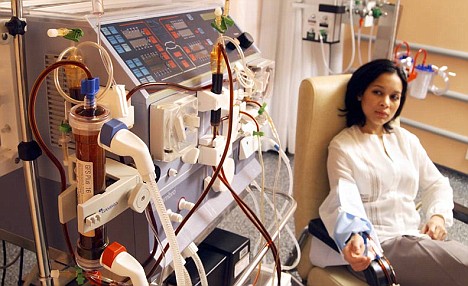
A Dialysis Patient
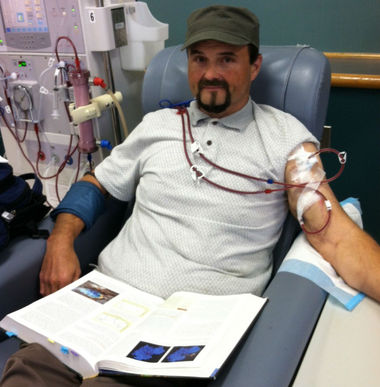
Nephrology
Management
Treatment of chronic renal failure is influenced by several factors and also the stage at which the paitient is first seen. The reversible complicating factors have to be identified and treated. These include salt and water depletion or overload, dietary indiscretion, infections, use of nephrotoxic agents, cardiac failure, urinary obstruction, hypercalcemia, and intercurrent diseases.
Attempts should be made to maintain the mileu interior as near-normal as possible.
- Water intake: It is guided by the ability of the kidney to excrete water. It is advisable to have an output of 2-5 to 3.0 liters per day by appropriate increase in water intake if the patient can tolerate it.
- Sodium: Salt has to be restricted if edema, congestive cardiac failure and hypertension are present, and salt should be supplemented, if postural hypotension, polyuria and dehydration are present.
- Potassium: Intake of potassium has to be restricted, if there is oliguria or hyperkalemia.
- Bicarbonate: If the serum bicarbonate level is less than 15 mEq/liter or if acidotic breathing is present, bicarbonate should be supplemented.
- Diet: Adequate calories have to be provided by a diet containing carbohydrates and fats. It is important to adjust the intake of proteins according to the renal reserve. Approximately 40 g/day can be given in moderate renal insufficiency. In uremia protein intake should be restricted to 20g/day or less.
- Anemia: When the hemoglobin level is below 8g/dl or PCV is below 20%, packed erythrocyte transfusion may be required. All contributory factors such as nutritional inadequacy and blood loss should be attended to.
- Hypertension: Two types of hypertension can be identified. (1) Fluid overload hypertension, often associated with edema and tendency for sodium retention responds best to salt restriction and diurectics. (2) In the other form in which there is no edema, the rennin-angiotension system may play the major role and this type may respond better to beta-adrenergic blocking drugs like propanolol or metoprolol. Specific angiotensin-converting enzyme-inhibitors like captopril are indicated if results are not satisfactory with beta-adrenergic blocking drugs.
- Renal bone disease: this occurs as a result of defective converstion of vitamin D to its active form. Large disease of Vitamin D (100,000 units/week) or new synthetic preparations similar in action to 1,25-dihydroxycholecalciferrol, such as l-alpha hydroxyvitamin D3 (0.5- 1ug) help to improve the symptoms and biochemical abnormalities. Supplementation of calcium lactate 4-6 g a day orally helps in reducing hypocalcemia.
- Hyperphosphatemia: This is controlled by advising diet low in phosphorus. Orally administered aluminium hydroxide binds dietary phsophage in the gut and prevents its absorption.
- End-Stage renal failure: When the renal failure is advanced and conservative management is unlikely to sustain useful life, regular repeated dialysis therapy or renal transplantation should be considered, depending on the available facilities.
When renal function is below 15% the full fledged uremic syndrome develops. In this all systems are affected and clinical features are referable to all organs. General symptoms include fatigue, lethargy, anorexia, nausea, loss of weight, headache, confusion and mental disturbances. Frequently, the precipitating factors tip the patient into coma. The urine volume may be high in the uncomplicated case with nocturnal polyuria. Urine volume is reduced when oliguric renal failure or cardiac failure develops. Susceptibility to infection is high.
© 2014 Funom Theophilus Makama