ESBL in Urine
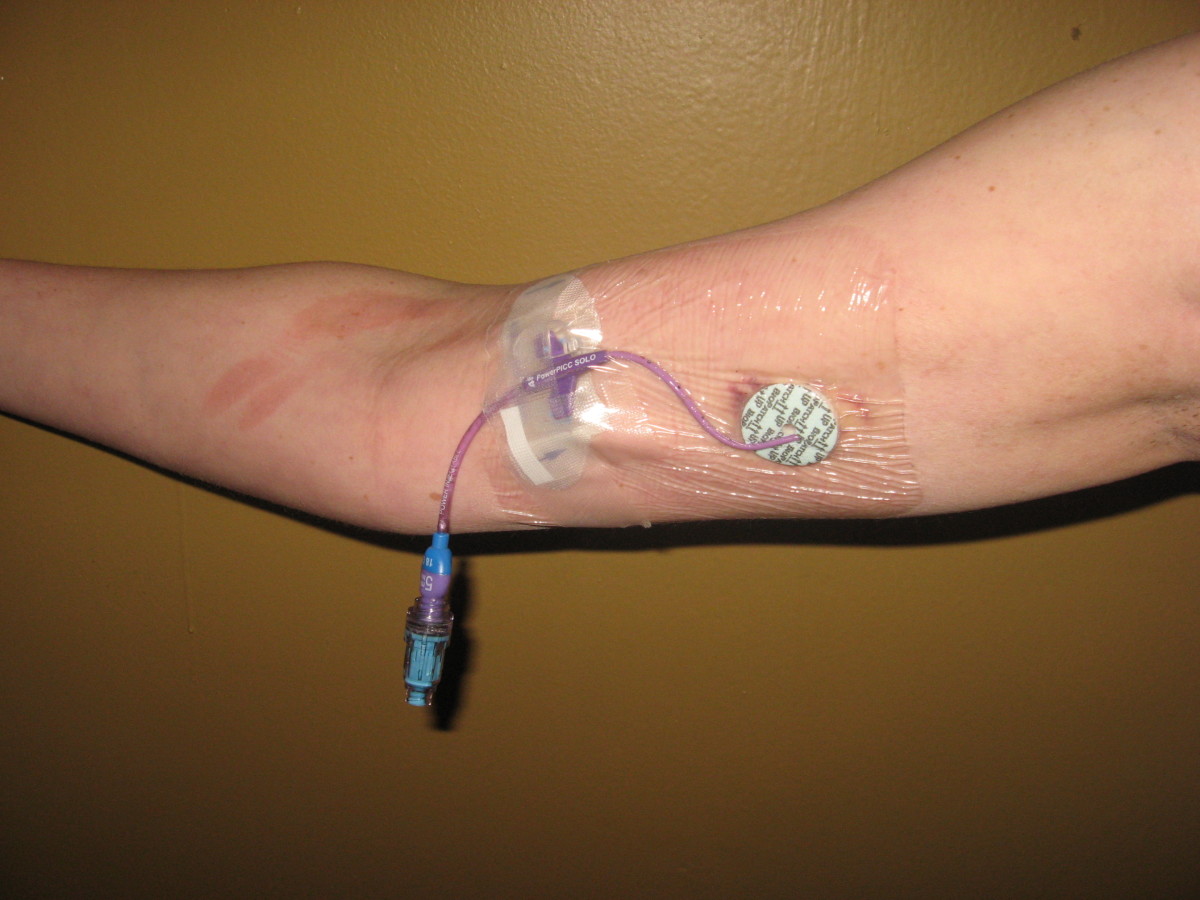
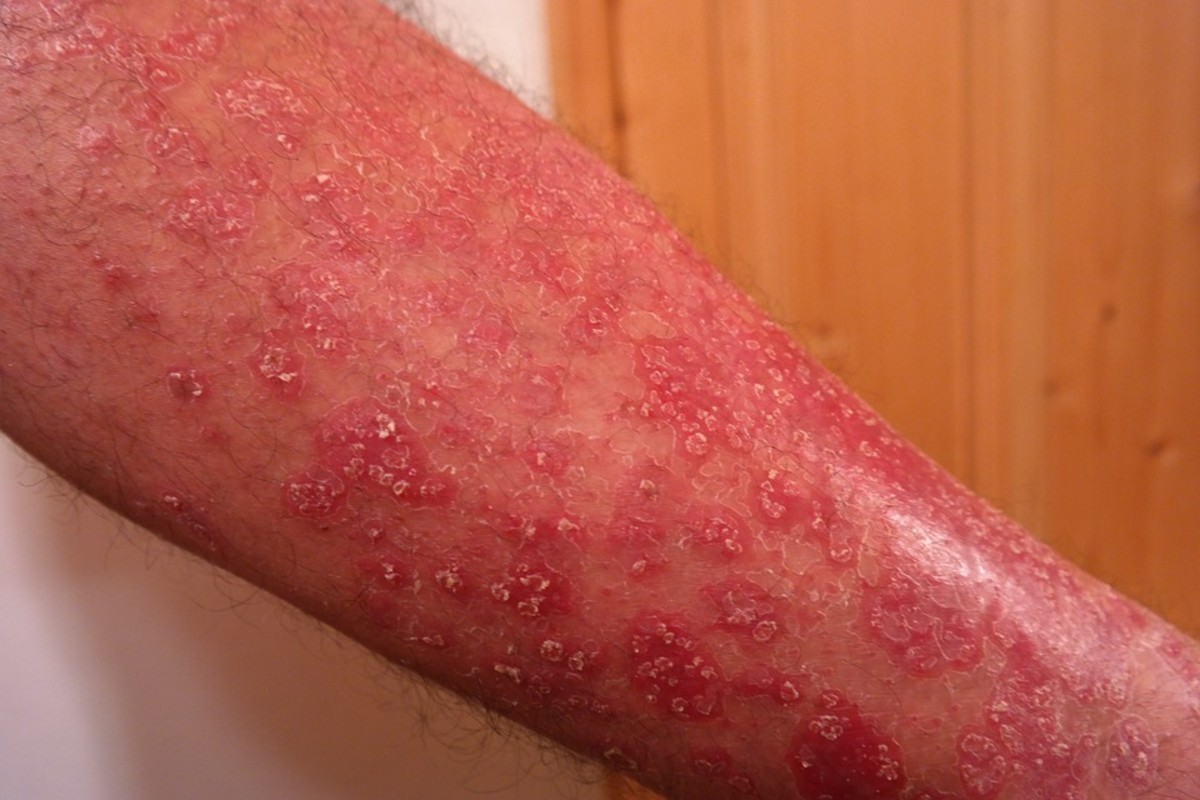
ESBL is an abbreviation for ‘Extended-Spectrum Beta Lactamase’. It is a type of bacteria that is resistant to the effects of antibiotics and causes varied infections that are primarily acquired in hospitals. Hence the detection of ESBL in urine is considered a dangerous condition.
ESBL bacteria are dissimilar from other kinds of superbugs. This is due to the fact that ESBL does not denote one particular type of bacteria. For instance, MRSA specifically refers to the strains of S. aureus that are resistant to methicillin. ESBL on the other hand, represents a specific enzyme that destroys the effects of antibiotics and which can be produced by bacteria.
The History of ESBL
Penicillin antibiotics were known to be the first antibiotics, known to be effective against a variety of diseases. In order to counter the effects of penicillin, varied types of bacteria started creating beta lactamase. It is an enzyme that protects the bacteria against attack by penicillin-based antibiotics.
Researchers then discovered other types of antibiotics which were able to kill and destroy the pathogens which could create the beta lactamase enzyme. ESBL or extended-spectrum beta lactamase is a modification acquired by bacteria to meet the challenge of the newer antibiotics. The ESBL enzyme can overcome the effects of both penicillin-type antibiotics as well as cephalosporin antibiotics.
Why is ESBL in urine a threatening condition?
ESBL bacteria are no different from other kinds of bacteria. The only reason they are clubbed in a different category is because of their immunity to varied antibiotics. Other than this fact, ESBL bacteria are the same and cause the similar effects as most other species of bacteria. These cause analogous diseases which are no more severe or milder than the diseases resulting from infections by non-ESBL bacteria of the same kind.
The resistance of ESBL bacteria to certain antibiotics can make treatment a lot more difficult and complex. It may result in hospitalization for longer duration, elevated healthcare costs, and higher death rates.
The ESBL enzyme detected in urine or blood can be produced by several bacterial species, including gram negative as well as gram positive bacteria. Klebsiella and E.coli are the most prevalent species of ESBL bacteria. Both these types of bacteria can be found in blood infections and surgical area infections. These are also the most common cause of UTIs or urinary tract infections, which can be diagnosed by the presence of ESBL in urine.
Diagnosis and treatment of ESBL in urine
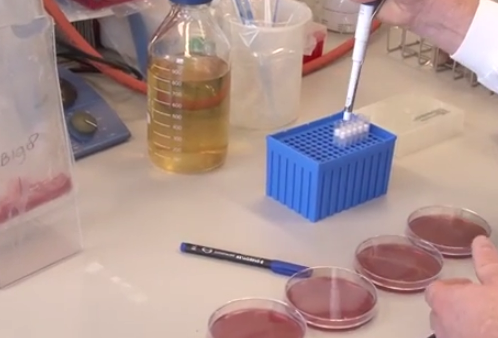
The diagnosis of ESBL bacteria involves collection of urine or feces sample and culture testing it in a laboratory. Doctors can also take a swab of a wound or the rectum.
It may also be noted that as ESBL bacteria are primarily hospital-acquired, patients may be tested for ESBL on or before hospital admission. People, who are diagnosed with ESBL in urine, or in other samples, are then placed in isolation so as to prevent its spread.
The diagnosis and treatment of ESBL pathogens can be quite complicated. As per the CDC, certain types of ESBL microorganisms cannot be identified through the typical laboratory procedures as they can result in false-positive diagnosis.
After the successful and correct diagnosis of ESBL in urine, the pathogens need to be checked for sensitivity to antibiotics. Varied strains of ESBL can be resistant to different antibiotics. Hence, each ESBL sample is checked in a laboratory for its vulnerability to specific antibiotics. This process is referred to as a ‘sensitivity test’. This test allows doctors to start treatment of ESBL in urine with the right antibiotics. It is however important to note that antibiotics that destroy ESBL bacteria in a lab may not produce the same results in a human body since it is more intricate as opposed to a Petri dish.
Prevention of ESBL in urine
As treatment of ESBL in urine is complex, the best option is to prevent its spread. The lack of any transmission route from a patient to a healthy person or others will eventually result in elimination of that particular ESBL bacterial strain.
ESBL bacteria are transmitted via contact, mostly through contaminated hands of healthcare providers. It can also transfer directly from a patient to another, or to or by visitors. Fortunately, it is quite easy to prevent the transmission of this pathogen. Studies have shown that washing your hands with an antimicrobial soap can eliminate the bacteria by 98 to 100 percent.
Individuals affected by ESBL infections may be given a private room. The patient may or may not be placed in isolation. Doctors, nurses, and other healthcare workers have to wear gloves and wash their hands after handling such patients. They can also wear plastic gowns to guard their own apparels. Medical equipment like thermometers, stethoscopes, etc; are either disposable or kept exclusive for ESBL-affected individuals to prevent the migration of bacteria.