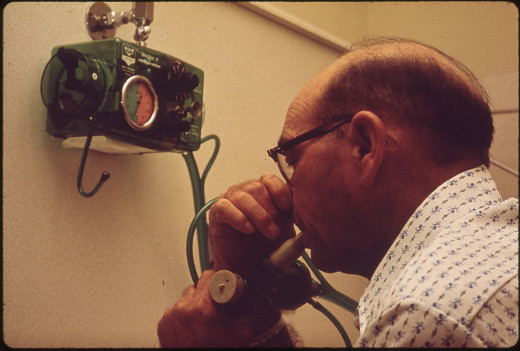
Emphysema: Basics of Diagnosis and Management
Fast Facts about Emphysema and COPD
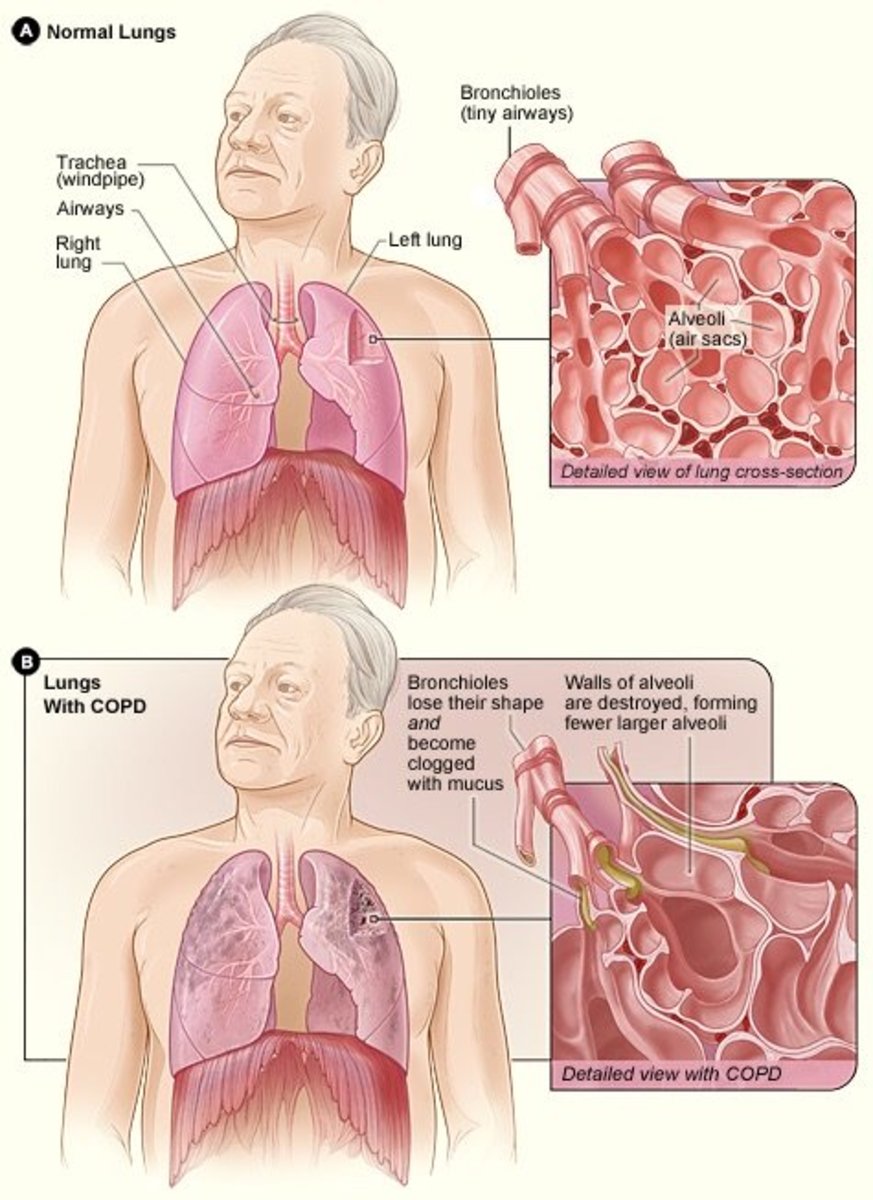
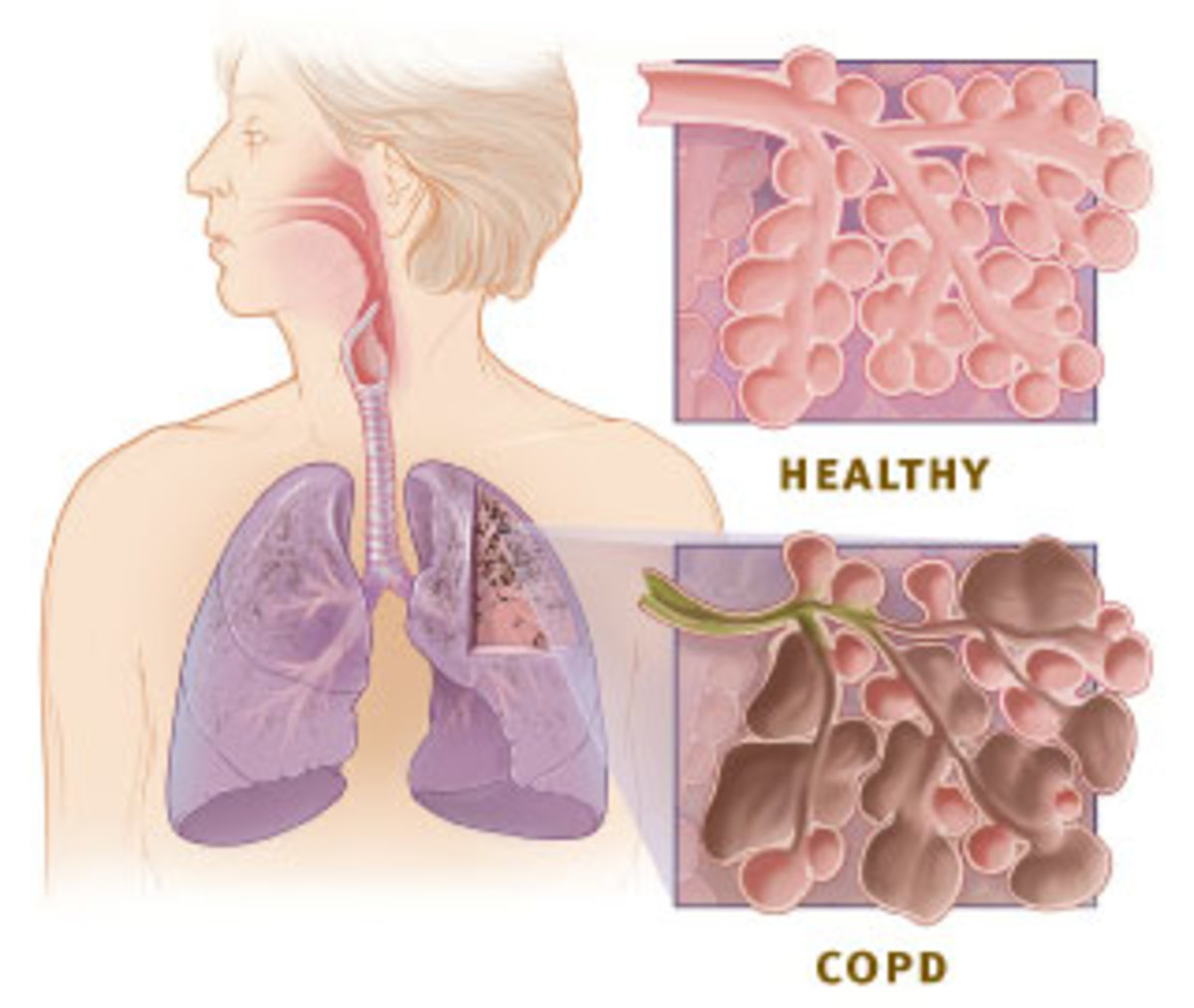
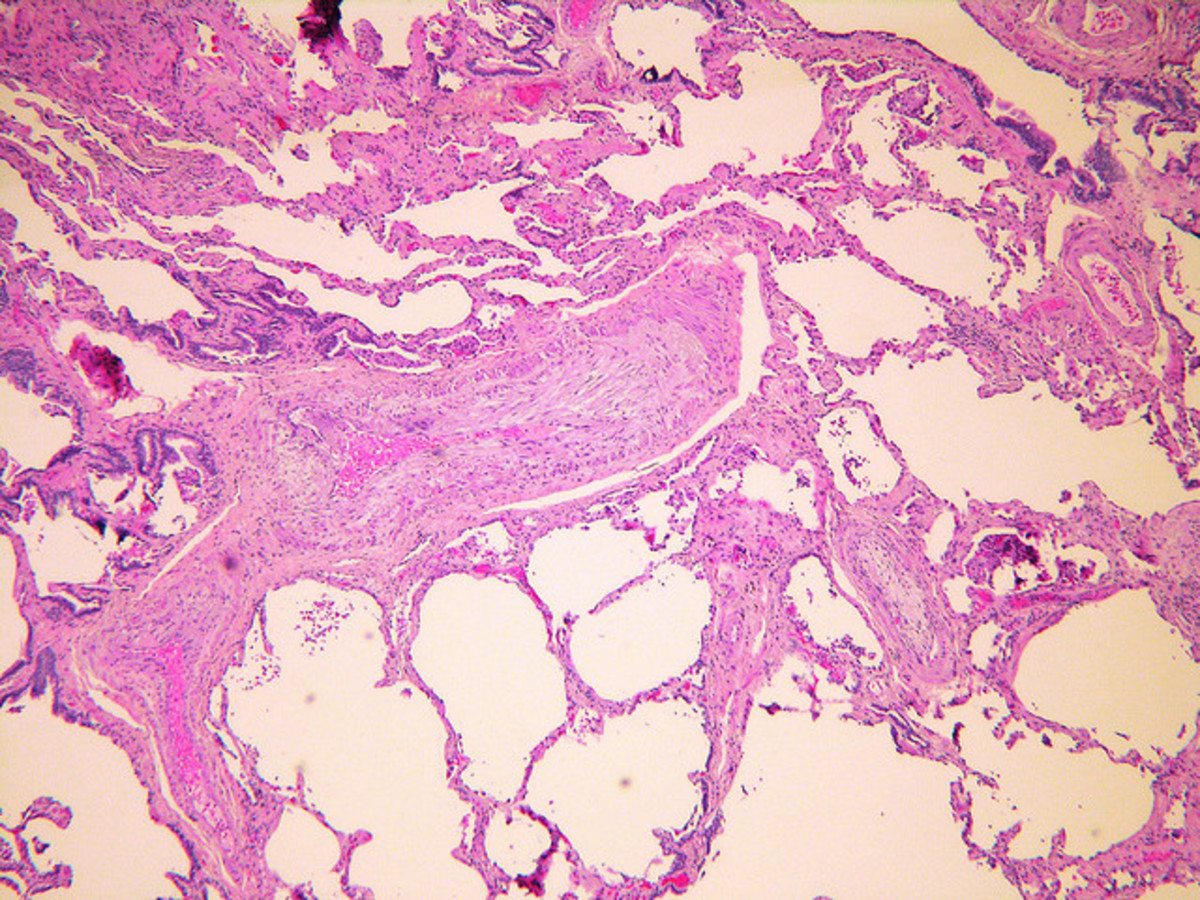
Emphysema is a one type of a Chronic Obstructive Pulmonary Disease (COPD) which is usually seen in many patients across first world to third world countries. It is a progressive disease of the lungs characterized by difficulty of breathing, and inability to cope up with daily activities which usually results from chronic exposure to cigarette smoke and other pollutants. It is further characterized by multiple episodes of exacerbation which causes massive drain in terms of the quality of life of afflicted patients.
COPD is the third leading cause of death in America, claiming the lives of 134,676 Americans in 2010!
— Centers for Disease Control and Prevention, 2013When Will One Start to Consider Emphysema?
Dyspnea as the Most Common Presenting Symptom
The main symptom presented by the patients with emphysema focuses on the initial presentation of dyspnea (commonly known as difficulty of breathing) which gradually worsens over prolonged period of months thru years. This serves as the main focal point for the cases wherein all the possible causes were considered. When presented with cases of difficulty of breathing, different etiologies are considered.
Even the extra-pulmonary and pulmonary causes are also accounted for since these are the most common bases for the pathophysiology of dyspnea. Most patients initially presents with coughing, and this comes hand in hand with the time of the onset of the other symptoms such as shortness of breath, easy fatigability even when just doing light household activities, and even the development of barrel chest.

Other causes of dyspnea that may be accounted for
- Neuromuscular and the Chest Wall Deformity- structural problems in the chest wall itself or how the respiratory muscles contract may cause progressive dyspnea
- Cardiac Disorders- the cardiac causes may cause coughing also, however if there are no overt signs of cardiac pathology, this is made for a less likely diagnosis
Infectious V.S. Non-infectious Pulmonary Causes
Once other common causes are ruled out, the focus of the impression shifts to the pulmonary aspects. When concentrating with these, both infectious and non-infectious etiologies may be considered. In this case, the most important aspect is the onset of symptoms; many infectious diseases are usually acute (starts fast and ends fast) such as bacterial pneumonia or viral infection. As compared to chronic non-infectious cases which may progress in months or years such as COPD. Once it is highly likely that the signs point out to either of the two- COPD may be diagnosed with certainty using different laboratory and diagnostic tests which are outlined below. Nonetheless it is also important to note that it is always possible that there is the presence of both the acute infection which exacerbates the underlying chronic progressive cause. With this, different tests may be employed to complete the initial impression.
Assessment Goals
The main goal of the assessment for COPD is to ascertain the patient’s status in terms of the severity of symptoms, degree of lung affectation, and risks associated with exacerbations and possible presence of comorbidities.
Lung Function Testing
Click thumbnail to view full-size

How is Emphysema diagnosed?
- Spirometry assessment is the gold standard for the assessment of lung function. In this test, the FEV, and the FVC are measured and computed relative to the patient’s demographic data. The predicted value may be measured leading to the classification based on the FEV1/FVC ratio. This is coupled with the use of bronchodilators which may relate to the effect of short-term treatment to the airflow limitation. The reversibility is also accounted for and a ratio of <0.70 is considered as COPD. In this case, even though the patient is already a diagnosed case of emphysema, the test may still be indicated to see the degree of progression of the patient’s decline in lung function. The findings in spirometry and the presence of the signs and symptoms are used to assess for the risk for exacerbations.
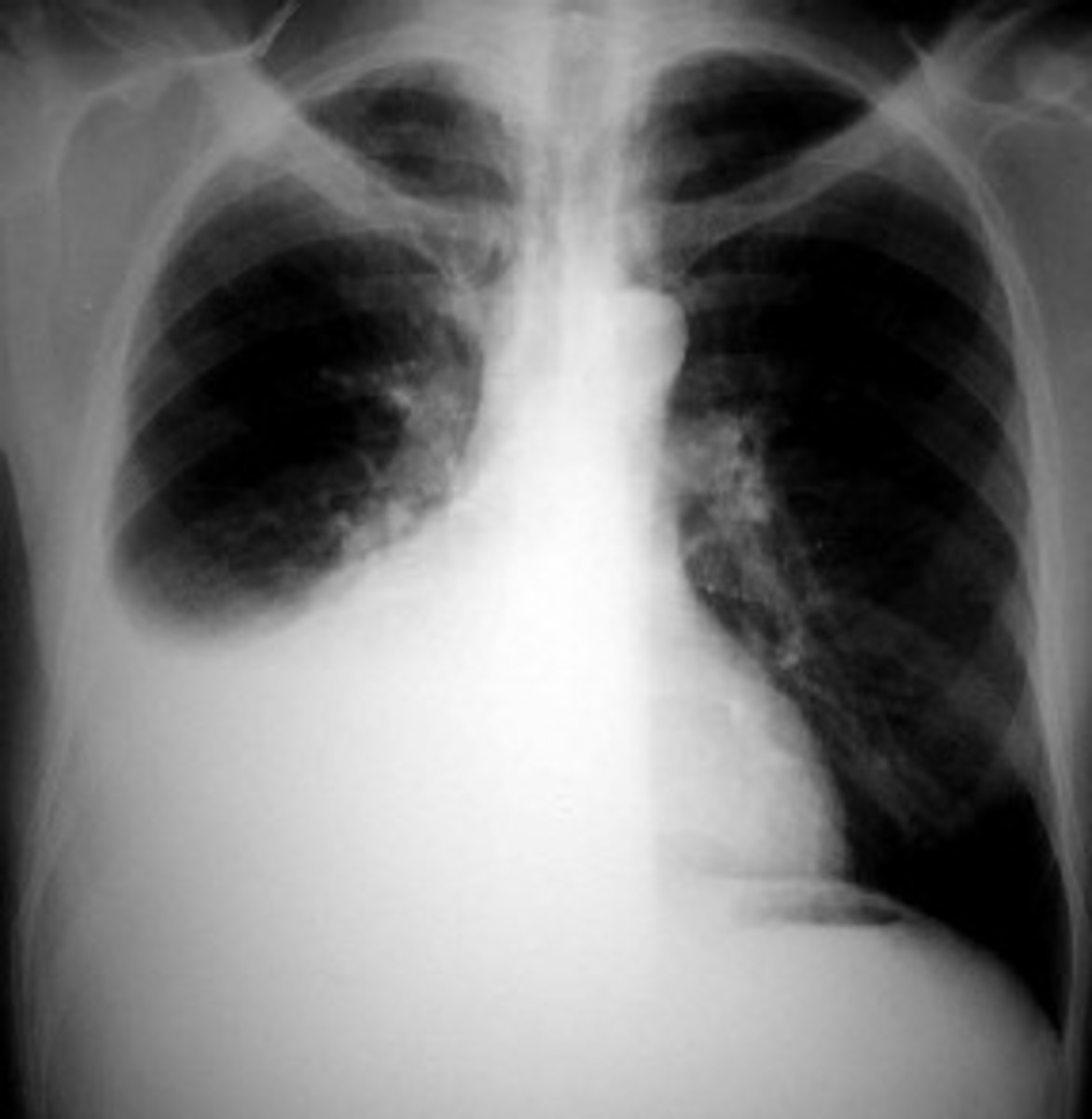
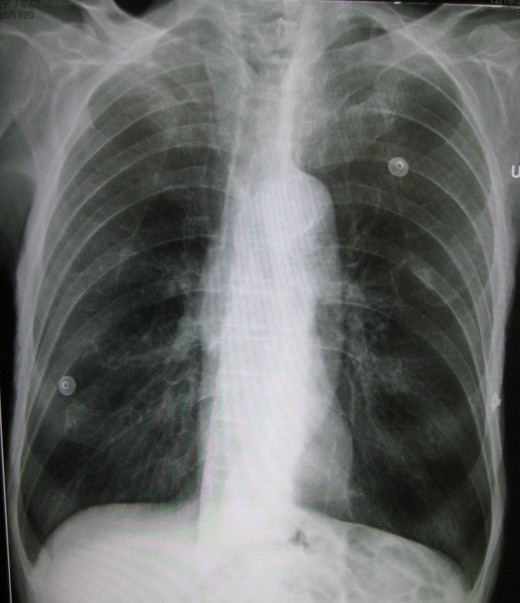
- Chest X-ray may be used to see the not only the changes in lung function in COPD, but also to detect other pathologic abnormalities that may be present. Infectious causes such as Community-Acquired Pneumonia and Tuberculosis can be seen as infiltrates in the lung parenchyma. If the patient is a chronic smoker, the possibility to lung cancer is not far-fetched. Affectation to the heart secondary to pulmonary hypertension may also be noted. All these may be seen through this imaging modality.
- Microbiologic studies for the patient’s sputum may also be considered to completely rule-out infectious etiology. Gram staining and culture may be done to assess the possibility of pneumonia. Sputum AFB may be warranted if the patient is not relieved by an initial therapy for COPD and/or CAP. A possibility of recurrence or worse, reactivation of his previous PTB infection may be possible.
Management Goals
The main goal for management of COPD exacerbation is initially, to manage the current signs and symptoms and reverse the airflow limitation. After this, possible diseases that accompany it are assessed and addressed. Finally, lifestyle modification to prevent another attack is done.
How is Emphysema Managed?
In this section, the different treatmend modalities are explained in order to help patients understand how the disease is being managed.
Initial Management at Home or the Clinic
For the initial management of exacerbation, short acting bronchodilators may be used to open the airways and relieve the patient from dyspnea. Short-acting Beta 2 agonist and anti-cholinergics are used to address the airway hyperresponsiveness. Mucolytics for the hypersecretion are used for some patients. Corticosteroids are used to decrease the immediate relapse, treatment failure and the decrease the length of stay in the hospital. This may be delivered via intravenous route in very acute cases, to via inhalation route for the more responsive ones.
Empirical therapy with the use of the antibiotic Azithromycin for the possibility of pneumonia may be done while microbiologic studies are still being processed. A shift to an appropriate antibiotic once the pathogen is isolated, to discontinuance of this antibiotic may be done later on. Essentially this practice is done by health care providers to ensure that all ground is covered while the other test results are still being processed in the laboratory.
Supportive and Non-pharmacologic measures may be considered also to alleviate the signs and symptoms dependent on the severity of the case of the patient. Supplemental oxygen therapy via low-flow oxygen delivery system may be used to relieve the dyspnea. The patient’s oxygen saturation is also monitored to see the severity of the hypoxemia (or the presence of decreased oxygen in the blood). Elevation of the bed and increase in fluid intake may be able to address the increased bronchial mucus secretion which causes further blockage in the airway of the patients.
Smoking is the primary risk factor for COPD. Approximately 80 percent of COPD deaths are caused by smoking. Female smokers are nearly 13 times as likely to die from COPD as women who have never smoked. Male smokers are nearly 12 times as likely to die from COPD as men who have never smoked.
— US Department of Health and Human Services, 2014What are the essential points that the patient needs to know?
- Health education regarding the decrease in exposure to allergens and airway irritants is warranted
- If the patient is a smoker, smoker cessation is important since studies show that this is the most common modifiable risk factor for this condition
- Long-acting bronchodilators or corticosteroids may be prescribed for home care management
- The step-by-step instructions in the proper use of the inhaler is also necessary
Further Reading and Journals Cited
Global Initiative for Chronic Obstructive Lung Disease. (2014). Global Strategy for the Diagnosis, Management and Prevention of COPD.
Longo, D., Fauci, A., Kasper, D., Hauser, S., Jameson, J., & Loscalzo, J. (2012). Harrison’s Principles of Internal Medicine (18th ed.). New York: McGraw-Hill Medical Publishing Division.
Toller, J. A. K. S. (2002). Acute Exacerbations of Chronic Obstructive Pulmonary Disease. New England Journal of Medicine, 346(13).
© 2015 LM Gutierrez