Epidemic Typhus (Louse-Borne Typhus): Pathology, Clinical Manifestations, Diagnosis, Treatment And Prevention
General Symptoms Of Epidemic Typhus
A General Overview On Epidemic Typhus
Epidemic typhus is a severe febrile disease caused by Rickettsia prowazekii. Man is the only known host for this parasite. As age advances the disease assumes more serious proportions. Several epidemics have occurred during famine, war and other natural calamities, when people had to be kept in camps under unhygienic conditions.
Rickettsia prowazakii is transmitted by the body louse (Pediculus humanus corporis) and rarely the head louse (Pediculus humanus capitis) from man to man. The lice are infected by the blood meal. An infected louse passes the organisms in feces for the rest of its life (4 weeks). When the patient scratches, the lice are crushed and their body contents are smeared on to the bite wound through which organisms enter the host. Inhalation of the dried lice feces is another possible mode of entry. Lice leave dead bodies to sek new hosts and in this process they spread infection. Persons who suffer from typhus acquire lifelong immunity. In some cases, relapse occurs after a long latent period and this is referred to as Brill- Zinsser’s disease. Occasionally, epidemics have followed such sporadic cases.
Pathology: Pathologically, the lesions are characterized by angitis seen in the small blood vessels of various organs including the skin, heart, skeletal musucles and brain. The blood vessels are thrombosed or they may rupture. Rickettsiae are seen in the proliferated endothelial cells. Various tissues show infiltration by round cells, macrophages, and sometimes lymphocytes and plasma cells. The vascular changes lead to patchy gangrene of the skin, sloughing of the skeletal muscles and myocarditis.
Epidemic Typhus In Burundi
Infectious Diseases
Clinical Manifestations And Treatment Of Epidemic Typhus
Clinical Manifestations
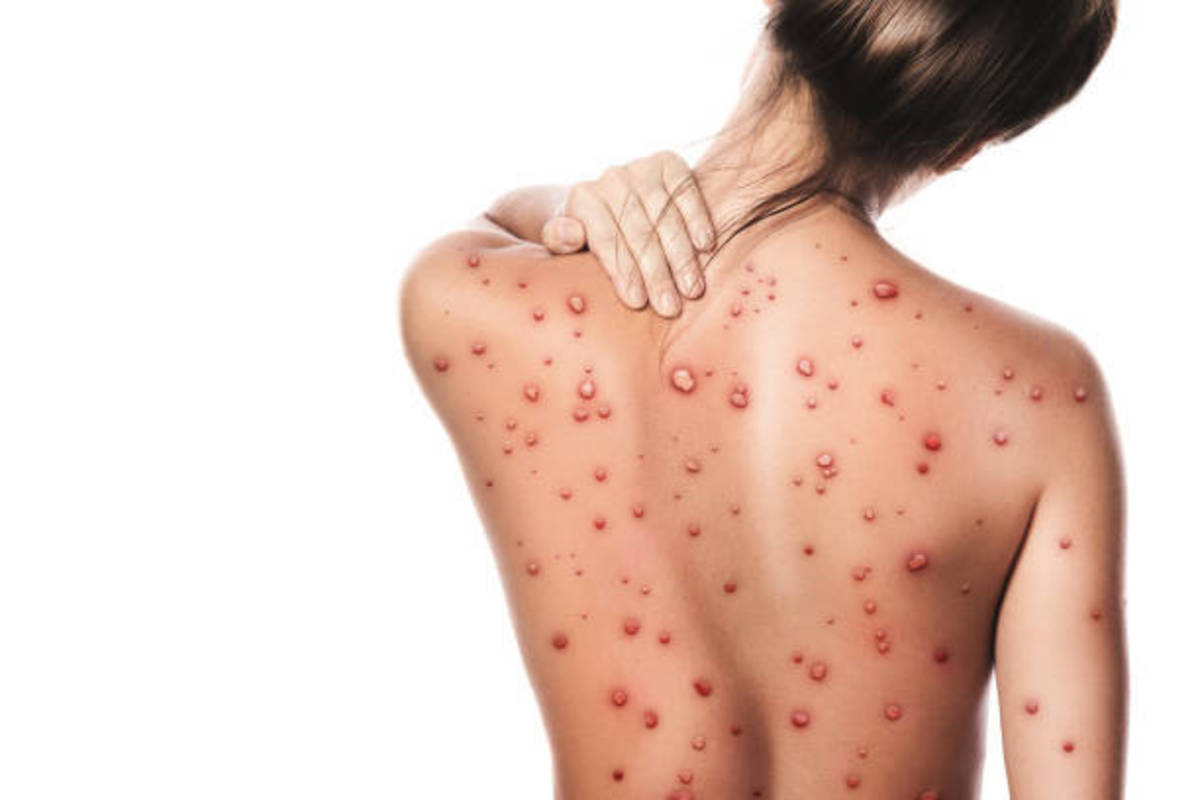
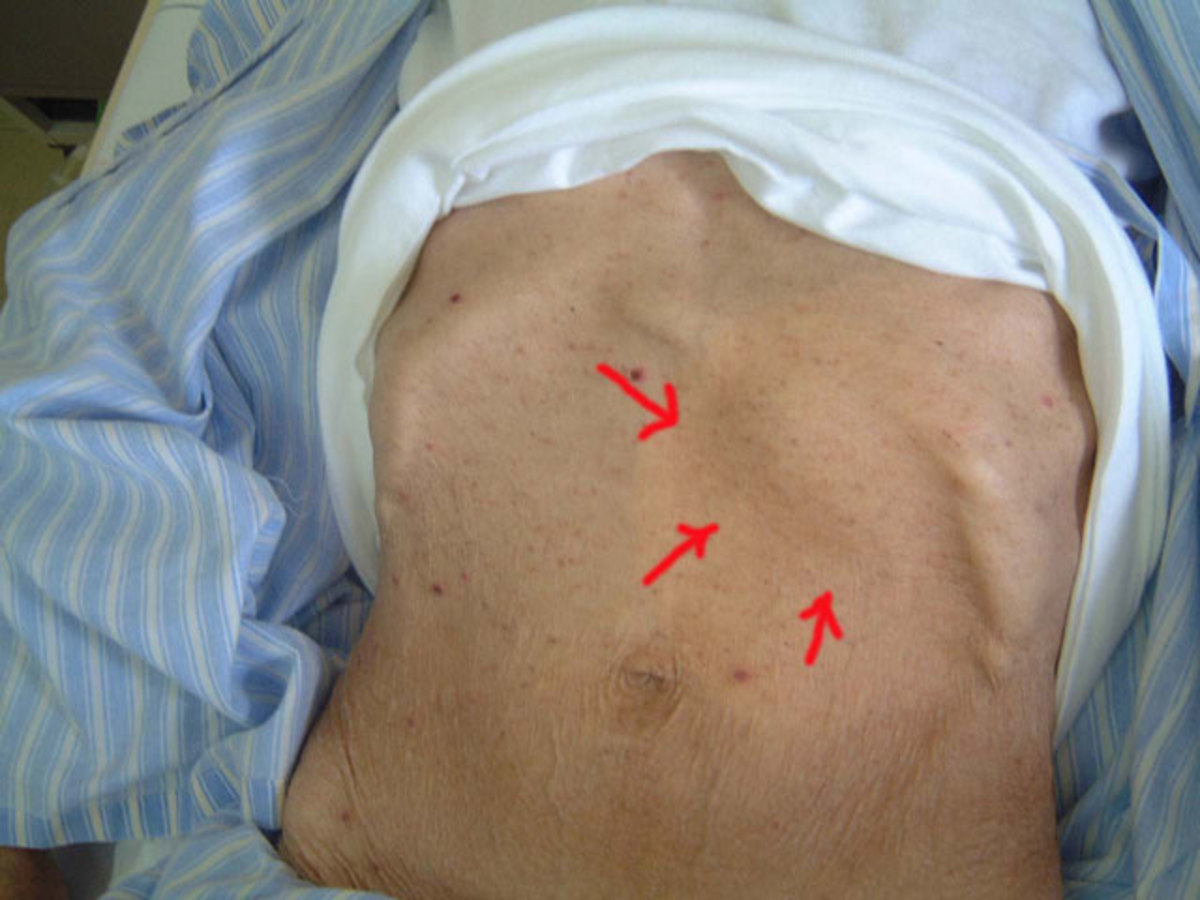
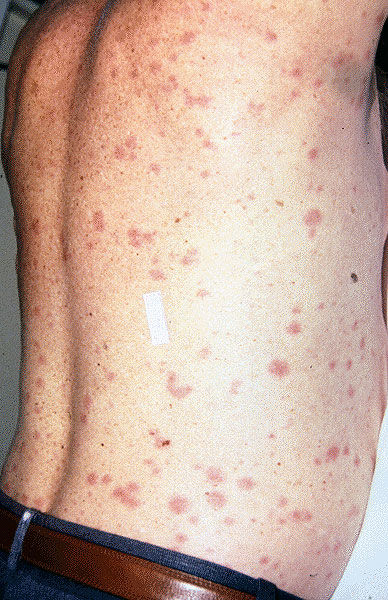
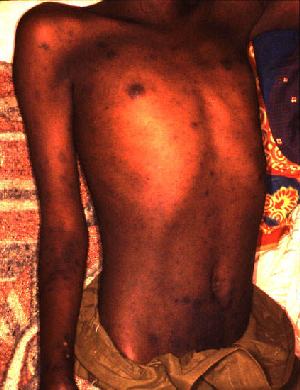
Average incubation period is 7 days (5 to 21 days). Fever is sudden in onset with malaise and myalgia. Temperature rises to 39 to 400C and remains continuous. The face is flushed, conjunctiva is injected and there is severe sore throat. A macular skin rash appears on the fifth day. It is particularly seen in the axilla, abdomen, chest, back and extremities. The rash starts to fade by about the tenth day. Involvement of the central nervous system leads to headache, stupor, coma and urinary incontinence. Bleeding from the mucous membranes gives rise to hematemesis, epistaxis, melena and hematuria. Respiratory involvement leads to bronchitis, bronchopneumonia, lung abscess or gangrene of the lung. Myocardial involvement is manifested by tachycardia, hypotension and cardiac failure. In uncomplicated cases, the temperature comes down by the twelfth to fourteenth day by lysis.
Complications include patchy gangrene of the skin over the extremities, parotitis, cardiac failure, and renal failure. Death may occur in the latter part of the second week due to complications. Though the disease used to be associated with high mortality during the epidemics, early diagnosis and specific therapy have considerably lowered the mortality rate.
Diagnosis: The disease has to be diagnosed by the clinical features. Epidemic typhus has to be differentiated from typhoid, malaria, tuberculosis, pneumonia, relapsing fever and other rickettsial diseases. Laboratory diagnosis is by the Weil- Felix reaction and other specific tests including isolation of the organisms. The organisms can be isolated from blood collected during the early phase of the illness.
Treatment
Chloramphenicol and tetracyclines are specific and highly effective, when given in a dose of 2 to 4 kg daily. They have to be continued for a week after the temperature reaches normal to avoid relapse.
Prevention: On admission to the wards, the clothes of the patient should be disinfected by heat or 10% DDT or 1% Lindane powder. Personal prophylaxis may be achieved by vaccination. Vaccines containing either killed rickettsiae (Cox vaccine) or live avirulent strains are available.
© 2014 Funom Theophilus Makama