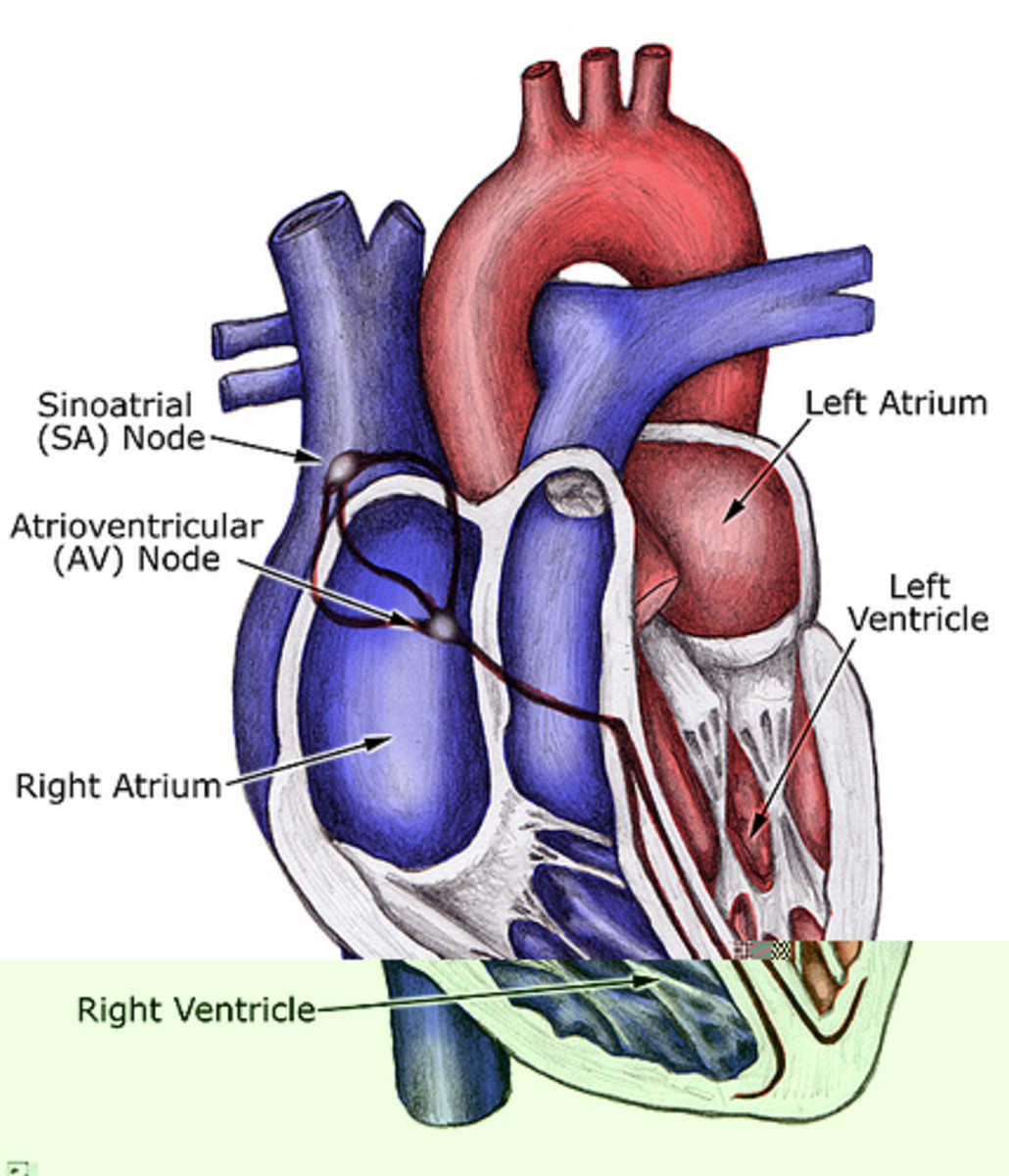
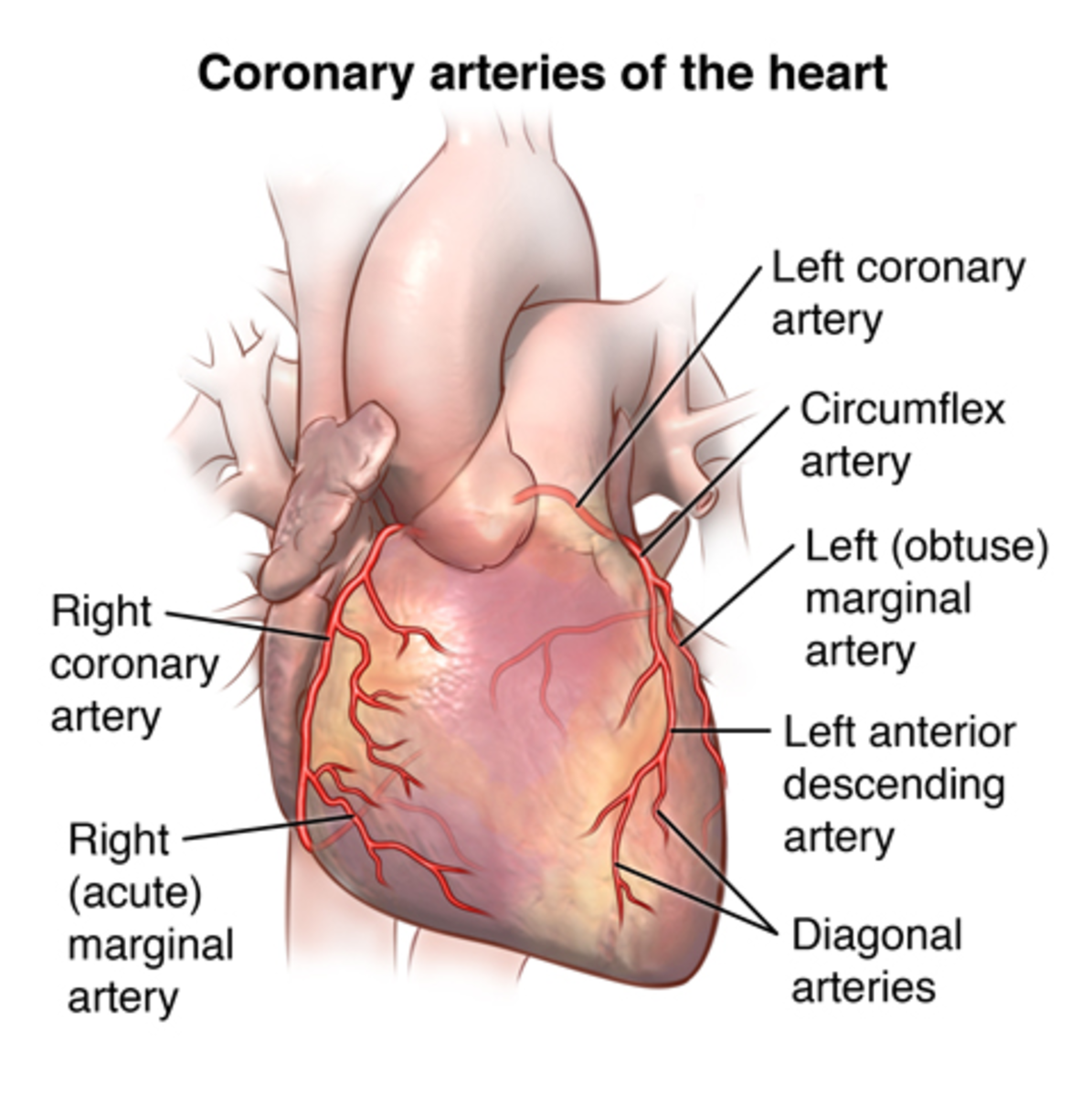
Etiology And Pathology Of Infective Endocarditis
Clinical Presentations
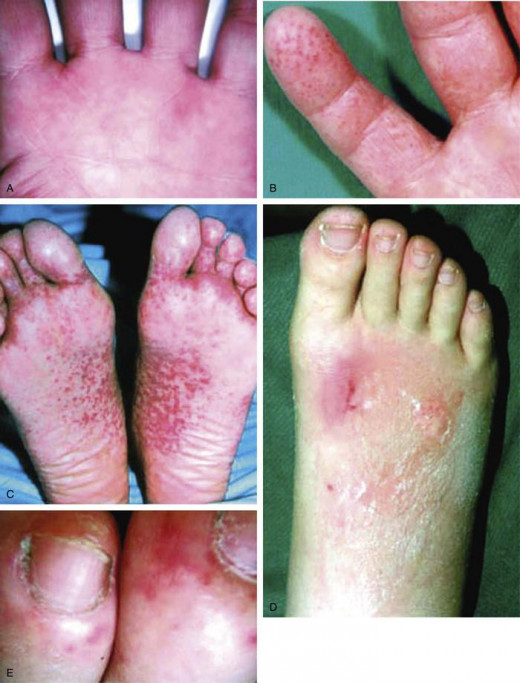
Introduction And Etiology
The heart valves and endocardium may be the seat of direct invasion by microbes. Virulent organisms such as staphylococcus aureus, streptococcus hemolyticus and pneumococci produce acute ulcerative endocarditis during the course of a septicemia and these affect normal valves. Fortunately, this complication is rare. More often infective endocarditis manifests as a subacute illness. In this case, the organisms are of low virulence and the disease supervenes on already damaged tissues.
Etiology
Predisposing factors: Infection is predisposed to by congenital heart disease or rheumatic heart disease. Organisms may colonise on the endocardium, valves or arteries that are already damaged or subjected to hemodynamic abnormalities. Combined valvular lesions are more often the seat of vegetations than pure stenosis or incompetence. Among the congenital lesions, ventricular septal defect, patent ductus arteriosus, pulmonary stenosis, Falot’s tetralogy and coarctation of the aorta may be complicated by infective endocarditis.
This risk is less in the case of second type of atrial septal defect. Open heart surgery and surgical introduction of prosthetic heart valves, grafts and pacemakers are associated with increased risk of bacterial colonization. In immunodeficient individuals and intravenous drug users, even normal valves may become colonized by pathogens.
Microbial flora
Common organisms are streptococcus viridians, streptococcus fecalis and other streptococci. Less common organisms include staphylococci, Pneumococci, H. influenza, gonococci, meningococci, salmonellae, E.Coli, Bacterium antitratium, candida Sp., aspergillus sp., anaerobes and coxiella burneti. Most of these organisms are commensals in the human body, particularly abundant in sites such as the mouth, upper respiratory tract, genitalia and urinary tract; Any infective illness or minor surgical procedures such as dental surgery, tonsillectomy, urinary instrumentation, parturition, abortion or medical termination of pregnancy causes transient bacteremia which conveys the organisms to the abnormal cardiac tissues, where they settle and multiple.
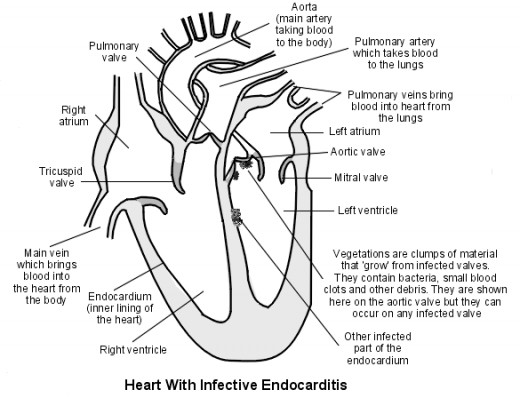
Heart With Infective Endocarditis
Clinical Cardiology
Pathology
On the endocardial surface, the organisms multiply and proliferate. Fibrin is deposited over the organisms and this gives a protective coat against the defences of the host. Further growth of the organism and fibrin deposition result in the formation of friable vegetations which show three layers- the innter layer made up of erythrocytes, leukocytes and platelets; the middle layer containing a heavy growth of the organisms; and an outer layer made up of fibrin. As fibrin gets deposited further, the vegetations grow and they get embolised from time to time.
The vegetations are located differently on the different valves:
- Mitral valve: Atrial surface and line of apposition
- Aortic valve: Ventricular surface and on the right ventricular endocardium where the abnormal jet impinges, and around the defect
- Ventricular and septal defect: On the right ventricular endocardium where the abnormal jet impinges and around the defect.
- Patent ductus arteriosus: Pulmonary artery and the ductus.
The chordate tendinae and papillary muscles may be affected. These may rupture leading to acute valvular incompetence or the udergo fibrosis when they heal. Embolic episodes form an integral clinical feature of infective endocarditis. The embolis may be septic or sterile. Embolism leads to infarction of organs. Sterile emboli reaching the vasa vasorum lead to weakness of the arterial wall and the formation of mycotic aneurysms especially in the intracranial vessels.
Repeated release of organisms into the circulation starts off immunological processes. Large amounts of antibodies are formed which give rise to the formation of immune complexes. Complement activation occurs. As a result, immunological lesions like glomerulonephritis, perisplenitis, and vasculitis develop. Septic emboli also lead to focal glomerulohephritis. Spleen enlarges due to reticuloendothelial hyperplasia and formation of microabscesses.
Untreated cases proceed to death and this is caused by massive embolism of vital organs (brain or heart), cardiac failure or renal failure.
© 2014 Funom Theophilus Makama