Everything You Wanted to Know About Knee Arthroscopy
Introduction
In the past decades, arthroscopic surgery has contributed greatly to the advancement of orthopaedic repair of knee-related problems. During a typical arthroscopy, a small tube-shaped camera (called arthroscope) is inserted into the joint and allows the surgeon and his team to see inside it without making a large surgical incision. The knee joint was the first in which the arthroscopic method was used both for diagnostic purposes and for performing surgical repair.
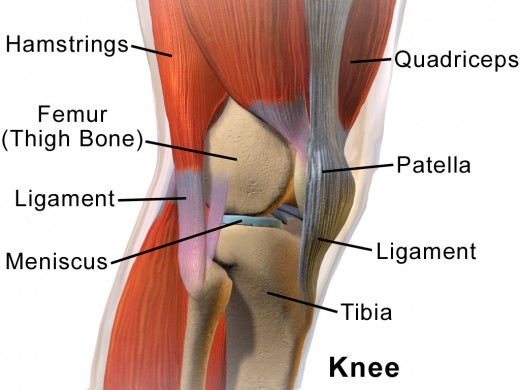
Knee Anatomy
The knee joint is made of three main parts. The femur, the tibia and the patella (kneecap). The patella flows on the front surface of the knee during flexion and extension movements.
The knee joint is surrounded by a sealed pouch called the joint capsule. This pocket is formed by the knee tendons, the connective tissue and the synovial membrane. During an arthroscopy, the synovial capsule is filled and expanded with sterile saline. After this, the surgeon can use the arthroscope to view all the parts that make up the knee, e.g. the articular surfaces of the femur, tibia and patella, the two menisci, and the anterior and posterior cruciate ligaments.
On each side of the knee is a meniscus. The medial meniscus on the inside of the knee joint and the external meniscus on the outer side. The menisci are also known as "semi-lunar" cartilages, due to their half-moon, crescent shape. Their main role is to protect the articular cartilage on the femur and tibia. As for the articular cartilage, it is a smooth, rubbery tissue that covers the end of the bones that comprise the joint and prevents injuries caused by friction.
Ligaments are persistent collagen fibers which bind the bones together.
The anterior cruciate ligament lies in the center of the knee joint, passing through a slot in the back of the thigh bone and connects in front of the tibia bone. It’s prime role is to simply connect and stabilize the joint by limiting the movement of the tibia forward, in relation to the thigh. If there is excessive forward movement, the anterior cruciate ligament (ACLD) may rupture. ACL may also rupture during sudden pivotal movements.
The posterior cruciate ligament is at the center of the joint, just behind the anterior cruciate ligament and connects the medial femoral condyle with the back of the leg. The posterior cruciate ligament controls posterior movement of the tibia relative to the femur. If the tibia moves too far back, the posterior cruciate ligament might rupture.
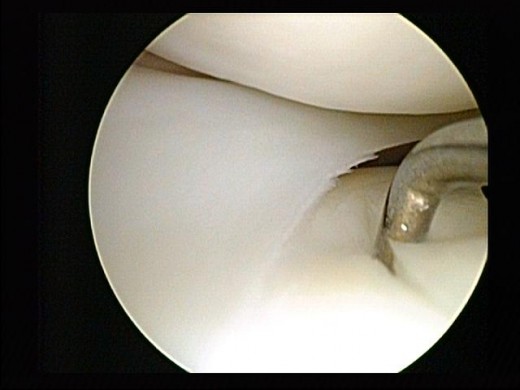
What are the objectives of the surgeon during an arthroscopy?
In 1970, when arthroscopy became first available it was performed purely for diagnostic purposes. Today, an arthroscopy can be used to treat a wide range of diseases of the knee. Some of the main applications of knee arthroscopy include:
- Meniscectomy and meniscal suturing
- Repairing damage to articular cartilage
- Chondroplasty cartilage transplantation
- ACL recontrusction
- Patellar realignment
During surgery, the surgeon aims to eliminate or reduce the problem the patient suffers from. By using the arthroscope, the doctor is able to see (on a monitor) a live, enlarged image of the inner joint while performing the operation through very small incisions. This results in less tissue injury hence rapid return. Having said that, the results of surgery depend on the type and amount of damage, the age of the patient, the effort made by the patient during rehab and so many other factors.
Advantages
Since arthroscopy is minimally invasive compared to traditional surgery, it has numerous advantages,including:
• Muscles and tendons don’t have to be incised
• Less bleeding during surgery
• Less scarring
• Smaller incisions
• Faster recovery and return to daily activities
What do you need to know as a patient before arthroscopic surgery?
The patient and the doctor first have a discussion on the surgery, why it is needed and whether there are alternative options or not. Ideally, the patient must have a good understanding of what will happen during the surgery and address any questions or concerns he might have.
Once the decision for surgery is made, the patient should follow certain steps. Initially the doctor will ask the patient to make a series of tests to ensure that he is able to undergo surgery. Often these tests are made on the day before surgery, or even in the same day for emergency cases.
The patient might also be asked to visit a physiotherapist to learn the rehabilitation program required after (and sometimes before) surgery. The physiotherapist might also check pain levels (before surgery), the ability of the patient to carry out its daily activities and to control movement, strength and flexibility of each knee.
The physiotherapist besides the recovery program, should show the patient how to walk with crutches, and explain all the basic strengthening exercises that should be done during rehab.
The patient is typically admitted the day before, or the morning of the day he will have surgery. You will be asked not to eat and drink anything for 12-24 hours before the time surgery is scheduled.
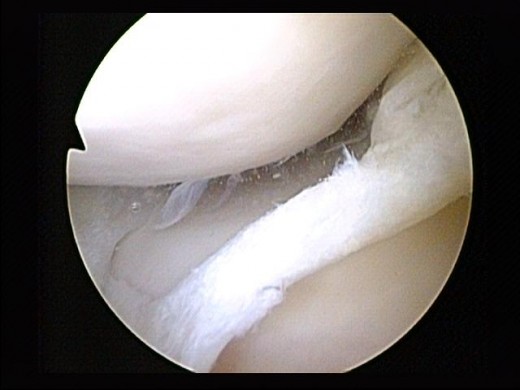
What happens during surgery?
Before surgery, the patient will receive some type of anesthesia which may be general or epidural anesthesia. For simple cases, local anesthesia might be sufficient. Before the surgery, special brackets are adjusted to the operating table, so that the doctor can move the foot and bend the knee safely. The operating table will be surrounded by the equipment necessary to perform the surgery.
The surgeon begins the operation by making two or three small incisions in the knee through which the arthroscope and several small surgical instruments will be inserted. Then a plastic or metal tube will be placed inside the joint, to provide sterile saline in order to inflate the knee joint.
The arthroscope is a small tube of optical fibers, which is used by the surgeon to see and work within the joint. It has a diameter of approximately 0.5 cm and a length of eighteen centimeters. The camera displays the image that captures inside the knee and sends it in a display the surgeon watches during surgery. The surgeon can move the arthroscope to any point within the joint.
The development of arthroscopic surgery led to the use of new, more sophisticated tools to perform arthroscopic surgery. Many procedures that were previously made through large incisions, are now performed using this minimally invasive technique, like the removal or repair of a ruptured meniscus or a torn acl.
Once the surgery is complete, the incisions made during arthroscopy are closed with sutures and you will be bandaged from thigh to foot. Wrapping the leg with an elastic bandage reduces swelling and helps prevent clot formation in the area. Finally you will be taken to the recovery room.
What can go wrong? (Complications)
Like all surgical procedures, there is a small risk of complications during arthroscopy. Below are some of the most typical (but very rare) problems that may occur:
• Complications from anesthesia
• Thrombophlebitis
• Infection
• Slow recovery
Arthroscopies in general have an extremely low complication rate of approximately 0.01%, compared to conventional surgical methods that have a risk of about 1%.
What to expect after surgery?
Due to its minimally invasive nature, arthroscopy does not require hospitalization and you might even return the same day at home. In more complex procedures that require larger incisions (e.g. ACLI reconstruction) or interventions that modify the bone, a patient may need hospitalization to help him him deal better and more effectively with the pain and other problems that might arise. In both cases, the patient can usually begin his rehab right after he wakes up from surgery.
After surgery, you should follow the instructions given by your surgeon to the letter. You will probably have to walk with crutches and keep the operated leg non-weight bearing for as long as specified by your surgeon. It may also be necessary to apply ice to the knee and to place your foot raised to a support when lying or sitting. A CPM machine may be given to you. This device will help you to regain your ROM and is believed to enhance the results of surgery. Other aids may also be recommended, like a calf-pump device which will help you retain muscle mass and increase circulation and flexibility.
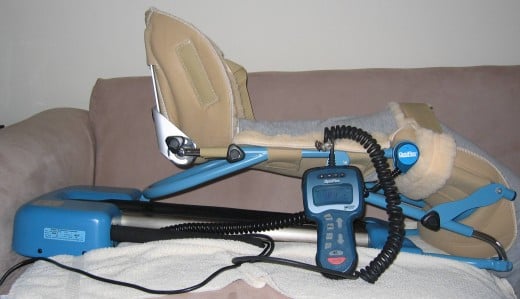
Rehabilitation
Rehabilitation is dependant on the type of surgery performed and the initial condition that led you to surgery. After a simple diagnostic surgery, rehab might not be required. Just a few a few exercises during the first week usually suffice.
Generally, the more difficult the procedure is the more tedious and prolonged will the physiotherapy program be. In the early sessions, the goal is to reduce pain and swelling after surgery. The physiotherapist will also show the patient how to progress with weight bearing.
Today, arthroscopy is often used to perform fairly complex corrective reconstruction while using very small incisions. It should be emphasized that because the incisions are small, this does not mean that the same is true for the interior of the joint itself. If the patient has undergone a major reconstructive surgery, the time it will take to fully recover will be several months and in some cases years.
The goal of the physiotherapist is to keep the pain under control, improve range of motion and help strengthen the leg while simultaneously teaching the patient what to do and not to do to protect the work done inside the joint by the surgeon.
Over time, and as the knee improves you will be making less and less frequent visits to the physiotherapist until the day comes that you are 100% cleared from physio.