"Eye, Eye, Sir!" Treating Epiretinal Membrane in the Eye
Although complex, the eye is tougher than many realize
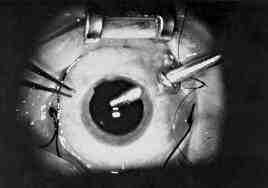

Modern Eye Surgery need not be Intimidating
Many hubbers research articles in answer to a friend, or family member’s, personal condition or interest.
Such is the case for the article today. The writer is no ophthalmologist, or any other “ist,” except perhaps pessimist.
Eye surgery, though, is no stranger to me, as have had a cataract removed - rather unpleasantly, as it happens, as the old lens “stuck,” becoming difficult to extract - forcing words between the Indian surgeon’s compressed lips I could only hope were not Punjabi for “Oh, darn it, nurse, pass the glass eyes will ya?”
But the cataract surgery 8 years ago was finally successful and I really still wear glasses from habit more than need.
My friend told me she, too, needed a cataract operation in the near future. “But,” she went on, “First I need another kind of operation to remove a membrane.”
I mulled that over and realized I had no idea what she was suffering with, so I identified the condition, “Epiretinal Membrane,” and began to research the disease for today’s article.
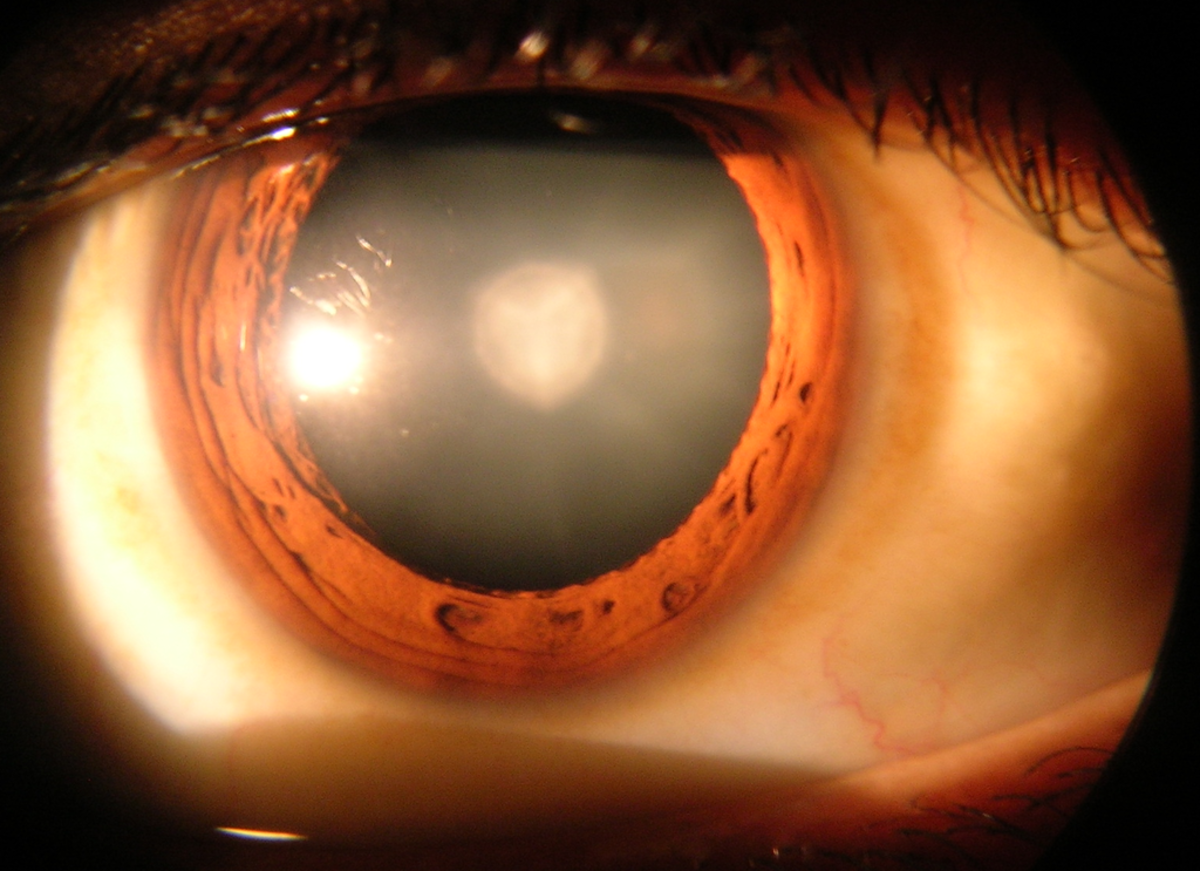
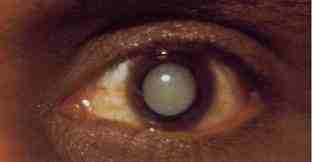
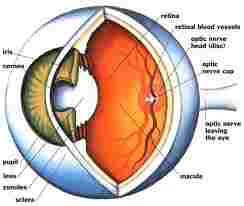
The condition, also know as “Macula Pucker,” affects the most sensitive part of the retina - the Macula - as a layer, or membrane, of scar tissue covers the macula and then contracts, causing this part of the retina to have a crumpled effect - rather the same effect you would get from crumpling some old photographic film.
As you can imagine, this can affect the vision in some bizarre ways, such as showing straight lines as being crooked or bent, and images to be blurry in the center - where the scar tissue develops in the retina. As in an ageing television, colors and brightness of normal vision may be diminished.
This condition is usually confined to one eye and does not mean the macular itself is degenerating. It can be caused by inflammation in that eye, or, as might be the case with my friend, an earlier, now controlled, diabetic condition - also a common cause of cataracts. Further, it might be a result of other eye surgery, and I have found this operation - to remove the scar tissue - often goes hand-in-hand with - or is succeeded by - an operation to remove a cataract.
Another irritating effect of this condition is that the function of normal binocular vision might be impaired, the affected eye causing the suffering to squint, or even close one eye in an attempt to see clearly.
The condition reaches a point where it becomes stable and these is little danger of blindness. But it also rarely clears up by itself and an operation is indicated to restore good vision.
Many people have been disappointed after this operation, saying there was little improvement, but they can be assured that most improve continuously for up to a year or even longer. (I found a similar situation with my cataract operation, but it only took weeks to improve).
A word of caution. As in all surgery, there may be after effects and the results are not always guaranteed.
Statistics show that:-
* About 1 in 50 patients are made worse by the operation.
* In a few patients, the condition may recur.
* A further operation will be needed.
* In only 1 in 100 patients, the retina may detach, potentially causing blindness in one eye. This will call for another operation to re-attach the retina.
* In a very few patients, serious infection may develop, even leading to glaucoma (dangerously raised pressure). This thought to be as low as 1 in 300 patients.
As you can see, these unlucky people are very much in the minority and this operation, as well as that for cataracts, is a matter of routine in specialist eye hospitals or clinics.
In Britain, both cataract operations and those for epirentinal membrane removal are covered by the NHS, although waiting times may be several months.
As was mentioned previously, cataracts may occur in conjunction with - or as a result of - this surgery. Eye specialists routinely offer both procedures at the same time.
(Remember, we are talking about one eye, and diabetics, or others who often have two cataracts present, will need to return to have the other eye treated…this is so doctors can observe one eye working well, before they put the other at the slight risk of surgery).
Surgeons may need to insert a bubble of gas in the eye to support the retina during the procedure; this may entail the patient lying face-down for a while - and not being able to fly for some weeks afterwards!
Apart from this, these operations are out-patient procedure done under local anesthetic (painless but unpleasant!). There is a short period beforehand as special drops are inserted in the eye. Afterwards, a cup of tea and a sit down and you can go home and see all the wrinkles on your mate anew!
The recovering eye will be covered at night for a week or so to prevent you scratching in your sleep.
You will return in a couple of weeks to have the fine stitching removed and your operation checked.
This humble article is dedicated to my friend, H., who, after she has her eye operation, I hope will still look upon me favorably, now she clearly sees what the ravages of time has wrought on her friend, Diogenes!
And to all out there who may be facing this type of eye surgery, always a daunting prospect, yet usually mere routine in today’s fine eye hospitals…