Facts and Information About IUGR (Intrauterine growth restriction), including our diagnosis
The Definition
IUGR is defined as the poor growth of a baby while in the womb during pregnancy. More specifically, it means the developing baby weights less than 90% of other babies at the same gestational age. Another part of the definition and diagnosis is a fetal weight that is below the 10th percentile for gestational age. Essentially, the fetus is much smaller than a normal baby of the same gestation age.
Causes and Risk Factors
1. Lack of oxygen and nutrients - The baby's growth can be restricted due to reduced blood flow, therefore she is receiving less oxygen and nutrients through her umbilical cord. Causes of the restriction can be due to:
- Pre-elampsia
- Problems with the formation of the placenta
- Carrying multiple babies in the pregnancy
- Mother lives in an area of high altitude
2. Mother's Health - There are some risks of developing IUGR if the mother's health is jeaopardized due to any of the following:
- Poor nutrition
- Smoking
- Blood clotting disorders
- Drug or alcohol abuse
- High blood pressure
- Heart disease
- Diabetes
- Mother's weight is less than 100 lbs
All of the factors will be considered by your doctor before a diagnosis is confirmed.
For more support, check out these titles:
Diagnosis
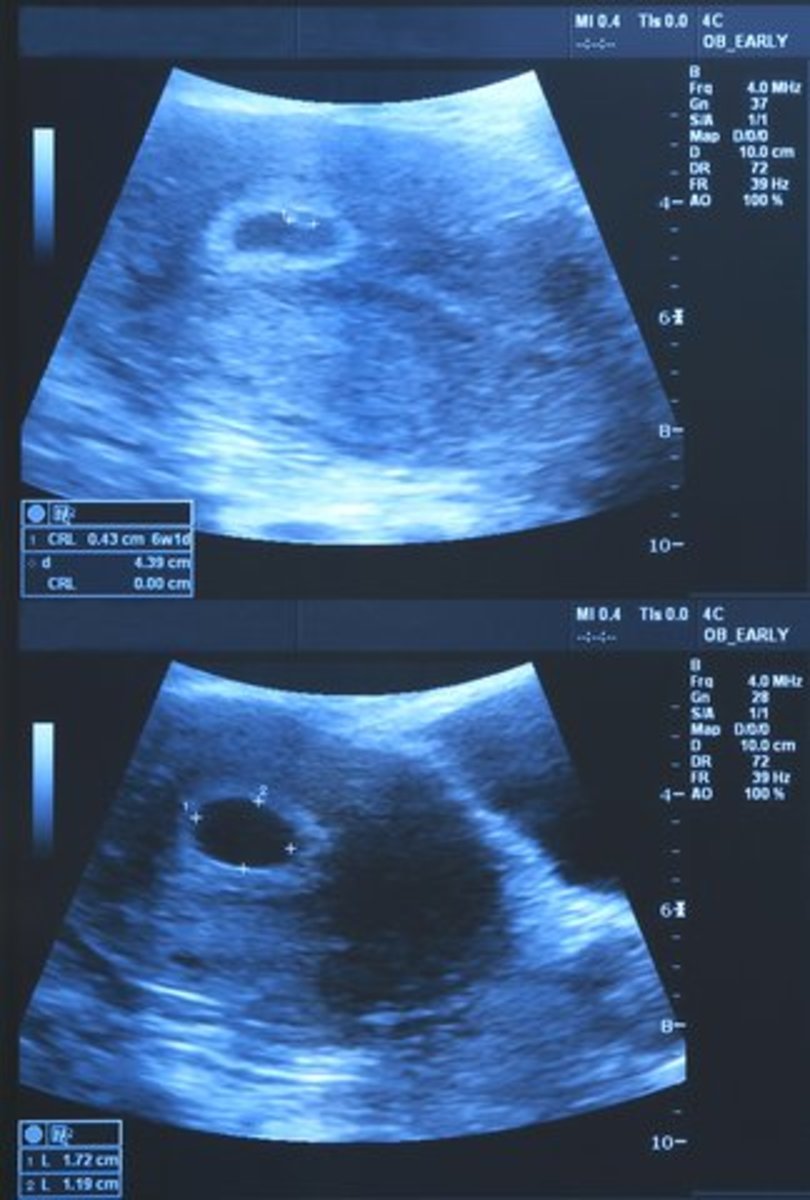
Gestational age must be confirmed before diagnosing IUGR. The mother should know when her last menstrual cycle was or when she thinks conception may have occured. The doctor needs the most accurate date in order to calculate the fetus' gestational age. IUGR can be diagnosed through a series of measurements taken during an ultrasound. The amniotic fluid levels will be measured, along with actual size and weight measurements of the baby. A doppler ultrasound can show the blood flow in the cord and in the baby.
IUGR must be closely monitored; the baby faces a greater risk of dying in the womb if left untreated. If IUGR is confirmed, the mother will face these options:
- If gestational age is less than 34 weeks - the mother will be monitored with ultrasounds to check the baby's growth as well as the blood flow. Babies are viable outside of the womb as early as 23 weeks, but they will face extreme risk of developmental disabilities and illness. The goal will be to keep the mother pregnant for as long as the infant health is stable.
- If gestational is greater than 34 weeks, the baby may be delivered early so treatment and support can be delivered outside of the mother.
Prognosis
Once diagnosed and a treatment plan is put in place, the best outcome would be the mother carrying the baby to at least 34 weeks to avoid major complications. However, the most likely outcome is the baby will need to be delivered early and be treated in a special care nursery or NICU. A perinatal doctor and an OB/GYN doctor will make the decision if and when to deliver an IUGR baby.
The severity of the restricted growth and the gestational age when the baby is delivered will determine what complications the baby may have in development in the short and long term scenarios.
Our IUGR Experience
Our baby was diagnosed with IUGR when I was 20 weeks pregnant. Her growth measurements were in the 5th percentile. The amniotic fluid levels were also very low. A doppler ultrasound confirmed there was a problem with the blood flow in the umbilical cord. I was diagnosed with PIH (pregnancy induced hypertension). After being placed on bedrest, a perinatologist was able to confirm that the umbilical cord was not attached to the placenta, but to the membrane that surrounds the baby. This abnormality is extremely rare and was the cause of my PIH and her IUGR. She was delivered by emergency c-section at 29 weeks and spent 3 months in the NICU. She was 2 lb 3 oz at birth and today she is close to 10 lbs. She is an absolute miracle.