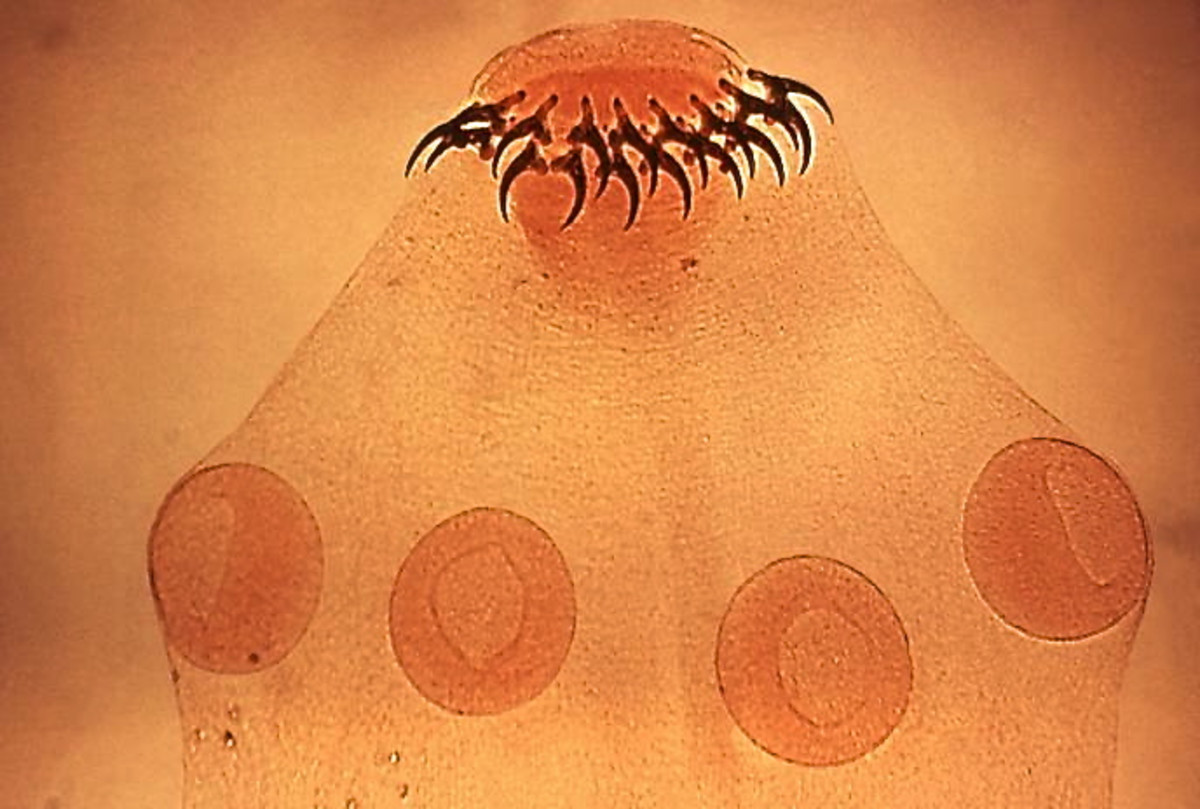
Filariasis As A Tissue Nematode: Clinical Significance Of Its Diagnosis, Treatment And Prevention
Taking Care Of A Patient With Filariasis
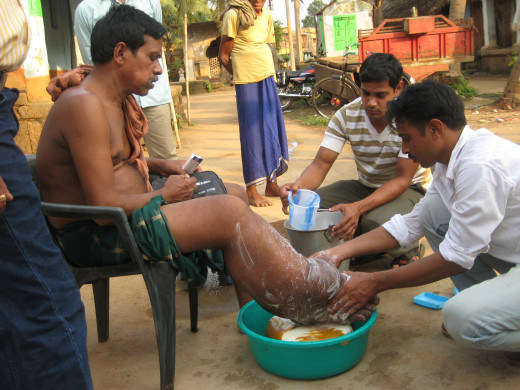
Diagnosis Of Filariasis
The diagnosis is evident if recurrent febrile episodes associated with lymphangitis occur in an endemic area or if there is history of residence in an endemic area. At this stage, microfilaria are demonstrable in the night blood film. For this 20 cmm of blood from the finger tip is collected between 8p.m and midnight, made into a thick smear and stained with Leishman or Geimsa stain. This helps in identification of the species. Motile microfilaria are generally seen in fresh films and this is helpful in rapid diagnosis. Concentration methods and techniques to filter the microfilaria through Millipore filters are available to enable easy detection even in early cases.
Provocative test: A dose of 100 mg of diethyl carbamazine taken orally, 50 minutes before collecting the blood sample increases the positivity rate to 90% and nocturnally periodic microfilaria can be demonstrated even during day time.
A moderate rise in eosinophils (up to 20%) is usually present, though this is not invariable. Chylous urine and hydrocele fluid may show microfilaria. In the chronic stage, microfilaria are usually absent in peripheral blood. Cytoscopy and retrograde pyelography help in establishing the site of communication between lymph varix and the urinary tract.
Immunodiagnostic tests are available for detection of filariasis but none is sufficiently sensitive and specific to be reliable. Lymphangiograms reveal the extent of lymphatic obstruction and may be of use preoperatively. Histological examination of lymph nodes or swellings may reveal the adult worms.
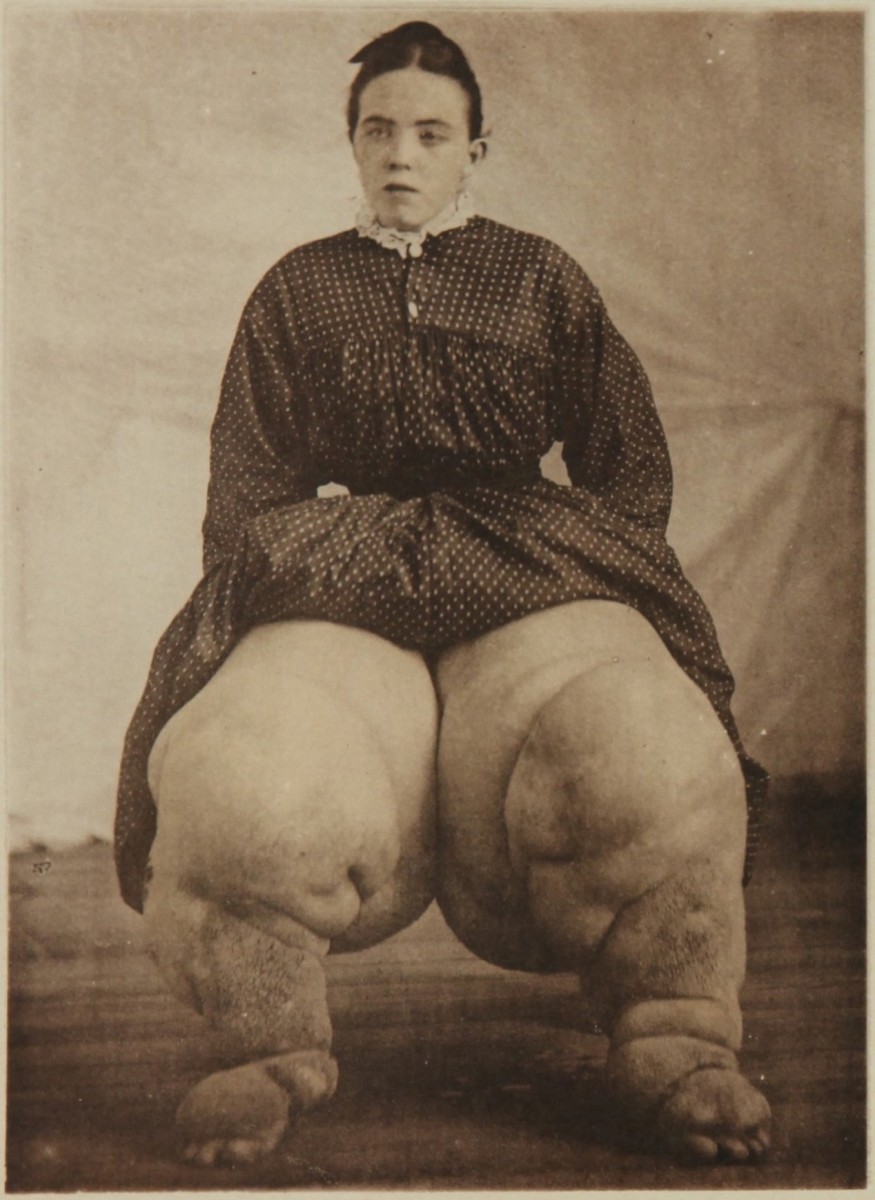
Filarial lymphadenopathy has to be differentiated from other causes of lymph node enlargement. Elephantiasis may rarely occur in other conditions like lymphogranuloma venereum and lymphatic obstruction by malignant tissue. In certain sandy areas, especially Ethiopia and Kenya, elephantiasis may occur due to damage to the lymphatics by chemicals absorbed through skin abrasions.
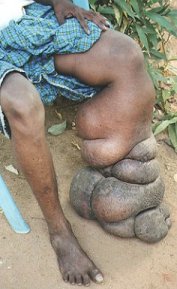
How To Treat And Prevent Elephantiasis
Infectious Diseases
Treatment And Prevention Of Filariasis
Treatment: The drug of choice is diethyl carbamazine (DEC) which rapidly destroys the microbilaria and reduces their number. When given in repeated courses, the drug eliminates microfilaria permanently suggesting that the adults may also be killed or sterilized. Some cases of W. bancrofti may be resistant to treatment. By reducing the infectivity of the affected subjects this drug also helps in reducing the transmission. The drug is given 4 to 6 mg/Kg daily in 3 divided doses for 3 weeks. Three to four courses given at intervals of 3 months are required to bring about lasting relief and prevent relapse. The outcome of treatment depends on the stage at which the treatment is started and the compliance with treatment. In the majority, recurrences are abolished or significantly reduced. In early cases, if the edema is still soft, it subsides considerably. If it is nonpitting, the reduction in size may not be appreciable. Elevation of the limb at bed time and supportive bandage during working hours help in clearing edema rapidly and preventing relapse.
Chyluria may be relieved by prolonged drug treatment. Advanced obstructive lesions such as elephantiasis and hydrocele do not benefit by drug treatment. Diethyl carbamazine (DEC) is safe and relatively nontoxic. Side effects include allergic manifestations and sudden exacerbation of fever and local manifestations of filariasis developing during the early phase of therapy. These are probably due to sudden destruction of numerous microfilaria with liberation of their products. Even if allergic reactions occur, the drug should be continued under cover of antihistamines. Some patients may discontinue treatment unless they are informed of these complications in advance.
Symptomatic treatment consists of the use of analgesics and anti-inflammatory drugs. Antibiotics such as penicillin or tetracucline are indicated if secondary infection is present. Obstructive lesions, such as hydrocele and elephantiasis require surgical management after a course of medical treatment.
Prevention: Mass treatment with low doses of DEC either alone or administered with common salt over prolonged periods bring down the microfilarial counts. Daily administering of 100 mg diethyl carbamazine for 5 days every month brings down the transmission rate in the community and prevents exacerbations in many cases. Full mosquito control measures have to be instituted on a long-term basis. Personal protection against mosquitos can be achieved by the use of mosquito nets and insect repellants.
© 2014 Funom Theophilus Makama