Filariasis: Health Implications, Morphology And Lifecycle And Epidemiology
How Can Filariasis Be Diagnosed?

A Clinical Overview Of Filariasis
Infection by nematodes belonging to the super family filarioidae constitute filariasis. Wuchereria bancroffi, Brugia malayi, Loa loa, Onchocerca volvulus, Dipetalonema perstans, Dipetalonema streptocerca and Mansonella oozardi parasitize man. Wuchereria bancrofti and Brugia malayi, which cause lymphatic filariasis, are widespread in India and South East Asian countries. Though W. bancrofti and B. malayi differ in morphology, epidemiology and transmission, the clinical features and pathological lesions are broadly similar and, therefore, they are described together.
Morphology and lifecycle: The adults of W. bancrofti are 4 to 10 cm long, whereas those of B. malayi are only 3 to 5 cm. The males are smaller than females. The adults are seen in the lymphatic vessels and lymph nodes and their lifespan ranges probably from 7 to 15 years. Periodically, the female worm discharges numerous embryos (microfilaria are seen most numerous in the peripheral blood at night, but in other geographical areas like the Pacific islands they circulate during day. This periodicity of the microfiliaria is probably nature’s adaptation to enable transmission and it coincides with the biting habits of the vector mosquitos and the sleep rhythem of the subject. When they are not present in peripheral blood, the microfilaria remain in sites as the lungs, liver and spleen. Some strains of W. bancrofti are nonperiodic and the microfilaria occur both during day and night in peripheral blood. The microfilaria are sheathed, vary in length from 200 to 300 microns, and are actively motile. Man is the only known definitive host for W. bancrofti, but animals like monkeys and wild carnivores also harbour B. malayi.
Further development occurs when the microfilaria are ingested by the appropriate mosquito vectors. For W. bancrofti, many species of Culex and some species of Anopheles mosquitos act as vectors. Brugia malayi is transmitted by mansonia and anopheles mosquitos, the former is more important. The adult worms do not multiple in the host, nor do the larvae multiple in mosquitos, so that the extent and severity of infection ultimately depend on the number of bites by the vector. In the mosquito, the microfilaria exsheath, reach the wing muscles, become shorter and thicker, moult twice and develop further. Depending on the temperature and humidity of the environment and species of the mosquitoes, they become ineffective in 10 to 14 days. The infective larvae which measure 1.4 to 2 mm X 18 to 23 mm migrate to the proboscis-sheath to be deposited at the bite wound when the mosquito bites. The larvae enter the skin at puncture sites and reach the lymphatics to grow, mature and mate. Microfilaria appear in circulation, 6 to 12 months after entry of the larva. The severity of infection is determined by the number of adult worms harboured by the host. The microfilaria remain viable for 2 to 3 months after which they die and are removed by the microphages of the liver and the lungs.
Physical Presentation Of Lymphatic Filariasis
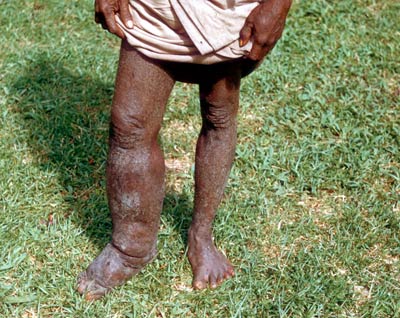
Infectious Diseases
Epidemiology Of Filariasis
A modest estimate is that at least 250 million people throughout the world are infected with W. bancrofti or B. malayi. Infection by W. bancrofti is endemic between latitudes 410 north and 300 south involving most parts of India, Burma, Africa, South East Asia, West Indies, Central America, the Pacific Islands and Eastern coastal plains of South America. Infection due to B. malayi is restricted in its distribution. It occurs widely in south-east Asian countries and there are many pockets in India. It is now becoming clear that several areas hitherto unsuspected, coastal, midland and even mountainous are endemic for bancrofti filariasis. In India, B. malayi is confined to rural pockets in Kerala and Andhra Pradesh along the coastal and backwater regions.
© 2014 Funom Theophilus Makama






