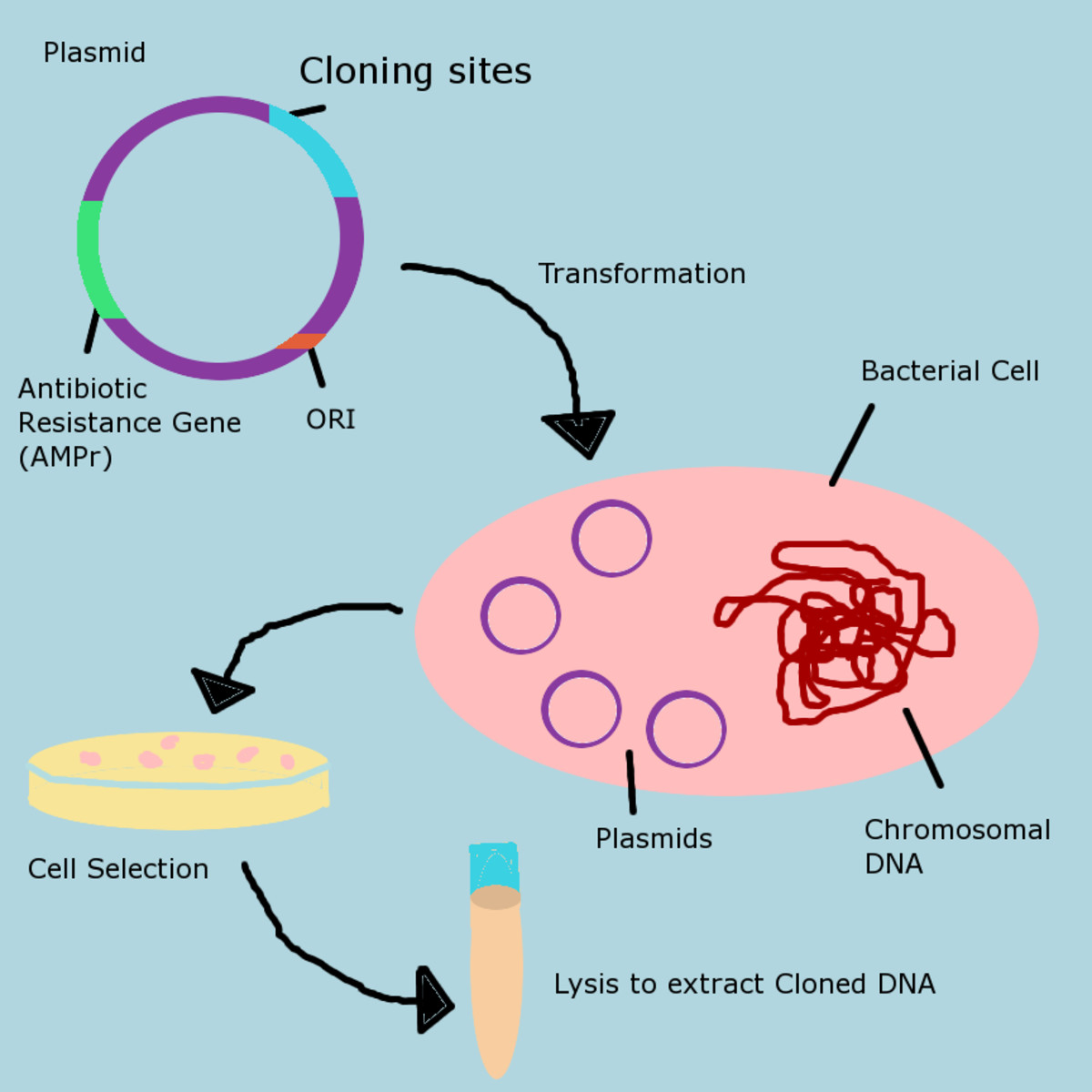
The Flu virus: a sneaky opponent.
You vs. the Flu
In one corner we have you. Sure you are tough. Your first line of defense includes skin, hair, mucous membranes, not to mention some mechanisms to deter, such as sneezing, coughing, crying. Your immune system is ready to recognize and kick out anything foreign. But in the opposite corner of the ring there is the influenza virus. Capable of so much shady trickery without even knowing what it is doing. The flu virus can sneak right into your bodies' cells, and get your cells to do the work to make its genome. Yes, you read that right. It tricks you into the doing the work for it. Your cells, unknowingly, make tons of copies of the viral genome while neglecting its own work. The influenza factory (your cell taken over) is soon ready to ship out virus particles all over your upper respiratory tract to infect more host cells.
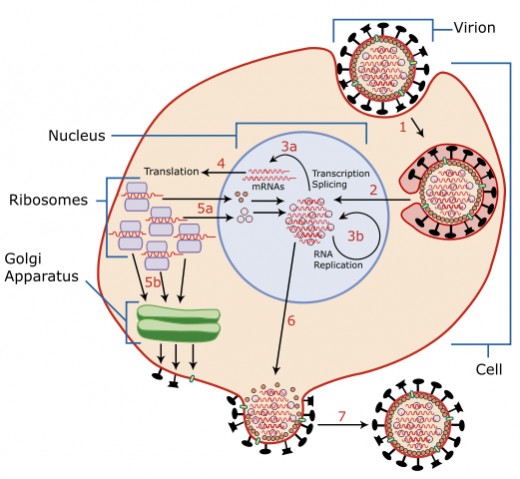
Virology and immunology are two sides of the same coin where virology is what the virus does to the host and the immunology is what the host does to fight back. It is hard for me not to geek out when thinking about virology and immunology. I am so impressed by how viruses gain access to the host I sometimes forget that when this happens people get sick. But equally fascinating is the way the human body fights back which is what immunology is all about. These two fields are equally fascinating but this article is focused on the villain- the flu virus and its virology.
Influenza is a tricky virus.
Why?
1. It is an RNA virus
2. It has a segmented viral genome
Influenza virus is a negative-sense, single strand RNA virus belonging to the Orthomyxovirus family. Viruses can either be RNA or DNA viruses. RNA viruses can be either positive-sense or negative-sense where, to put it simply, positive sense match the host and negative sense do not. What matches, or doesn't, is the messenger RNA which is the template for proteins during transcription. Since negative-sense RNA viruses don't match the host they need to bring their own equipment to replicate, specifically in its genome it needs to contain blueprints for RNA polymerase, an enzyme that makes a copy of the influenza RNA to match host messenger RNA (mRNA). The virus mRNA needs to match in order to trick your cell's machinery into transcribing it into viral proteins. But here's the thing the RNA polymerase messes up a lot, and unlike its counterpart- DNA polymerase- it doesn't have a proofreading mechanism to fix its mistakes. The RNA polymerase cranks out many different erroneous versions of the viral RNA, it is estimated that one mutation can present itself every time the genome is replicated.
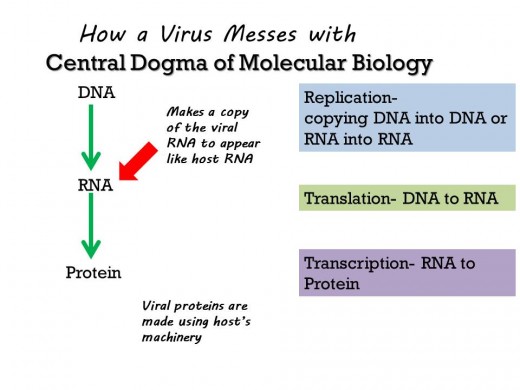
Think of the influenza virus as an opponent in a match. First the virus needs to enter the playing field, the human body, but in order to attack it needs to get to the actual opponent, the bodies' cells. The virus needs many tools and tricks to evade the human bodies' non-specific barrier protection. And even more tricks to attack the actual opponent, the cell. When the RNA polymerase makes errors-mutations- in the code most of the time these changes don't affect the virus at all. Other times these changes have a negative outcome, preventing the virus from invading the body or attacking the cell but sometimes out of sheer probability (I'd say luck but remember it is a virus, not a living thing) an accidental mutation ends up being good for the virus and bad for the host. A mutated version of the viral RNA might give an advantage during the path to invading the host, a change better than the original viral RNA had to begin with.
Another reason why mutation is bad news for the host, it allows the virus to use a different technique to harm the host. It opens up new ways to attack the host cell by unintentionally reconfiguring its genome for optimal virulence. Since this different strategy is new the established antiviral medicines may be rendered useless against it. This is the thing that has always fascinated me about virology. Even if it boils down to you being in bed for three days with a sore throat, aches all over, and those annoying chills the way in which the virus has gained access to your cells, taken control, and makes its own genome is pretty fascinating stuff. Crazy to think how much of what allows a virus to be successful is just sheer luck, in the form of mutation.
This mutation or change is gradual and subtle. It is referred to as Antigenic Drift. For the most part these small changes within the viral genome don't affect how our immune system responds to the virus. However over an extended period of time, these little changes can ultimately make the virus undetectable to us.
Another key factor allowing influenza to be a successful opponent is the organization of the viral genome- for influenza the genome is segmented. This means the RNA is divided into separate sections and then all of these sections are contained together within a single virus particle. This segmented genome allows for genetic reassortment. Now keep this genetic reassortment idea in mind as it is key for why the flu virus is so good at being bad. But let's first get into what proteins the genome holds the instructions for because this is yet another interesting aspect of this virus.
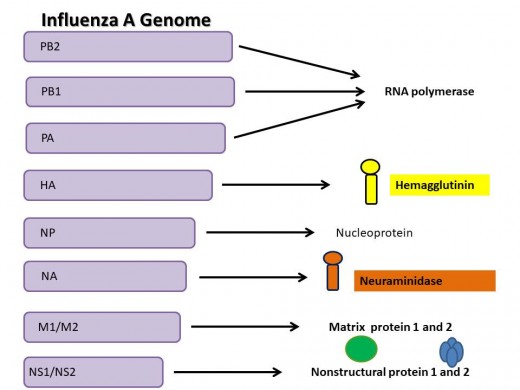
Influenza‘s genome is made up of eight genes. Four genes make up the components necessary for transcription- PA, PB1, and PB2-which work along with the nucleoprotein made by the NP gene. The PA, PB1 and PB2 make the RNA polymerase, the enzyme previously mentioned as necessary to the virus to make copies of itself in the correct orientation to mimic your cell's mRNA.
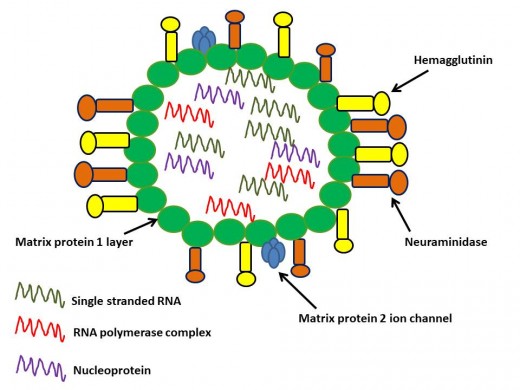
The M gene makes up two matrix proteins, M1 and M2, and the NS gene codes for two non-structural proteins. These genes are both able to make two different products due to a shift in the reading frame. The M1 protein forms a heterogenous shell, many M1 proteins lined up together, giving strength to the virus wall. Lastly, The HA gene codes for the surface protein haemagglutinin (or hemagglutinin), while the NA gene codes for a second surface protein neuraminidase. Hemagglutinin is necessary for breaking into the host cell and neuraminidase is needed for getting the newly made virus particles back out of the host cell. The naming of Influenza A is based on which type of Hemagglutinin and Neuraminidase are found in the virus. H1N1, H1N5- a bit more on this later.
Let's take a minute and think about how diabolical the influenza virus is. It carries out all its symptoms, the fever, the chills, muscle aches, running nose, headache, and sore throat all from nine proteins. Nine proteins. That is it. Impressive right? Impressive from a virology standpoint. From the infected host's standpoint not so great.
We are going to delve into the hemagglutinin and neuraminidase viral proteins a bit more. Hemagglutinin has 18 subtypes, different versions of the protein, while neuraminidase has 11 known subtypes. H1, H2, and H3 and N1 and N2 are the most common subtypes to infect humans. While other subtypes predominantly infect animal species. The species specificity boils down to these surface proteins- they are the key to entering the host cells and later getting the virus particles out of the host cell. In order to get in, hemagglutinin must identify and bind to a particular sugar reside, sialic acid, on the host cell’s receptor. In theory the lack of this particular sugar residue on a given species’ receptor is the reason why only certain subtypes of the Influenza A are able to infect that particular species.
Different subtypes of the flu virus have different affinities for the type of sialic acid, that is how the sialic acid is linked to the sugar in the chain. For example Avian flu prefers an alpha (2,3) linkage while the human strains prefer the alpha (2,6) linkage. Pigs have both types of sialic acids. Also of note is the type of sialic acid residue the hemagglutinin prefers to binds to is expressed differently throughout the body. For humans it is mostly found in the epithelial cells of the upper respiratory tract.
The characteristics of Influenza discussed above, namely the high mutation rate and the segmented genome, allow for inter-species infectivity. When two subtypes of the virus have the opportunity to intermingle, gene reassortment of the virus’ genes can occur and this creates a genetically novel flu strain.
Genetic reassortment is an established phenomenon but how the influenza strains are able to achieve it is still in the theoretical stage. Some researchers feel a third host allows for it. This theory was looked into in an article in the Journal of Virology in 1999 by Zhou et al. The paper details this idea of two strains of virus, one human and one avian, infecting a third host simultaneously and rearranging to form new genetic variations of the virus. The host in recent years is pig, which is known to be infected by both human and avian strains of the flu. Other experts feel that this concept is overthinking it and the various strains can intermingle and reassort in a primary host. Humans for example.
Regardless of what allows genetic reassortment to happen, it is a big deal and incredibly relevant to our battle against Influenza. Our immune system has no experience fighting these new versions of flu and these strains are not represented in any flu vaccines for initial outbreaks. In simple terms the vaccine does not protect against these novel strains. This type of sudden, major change is called Antigenic Shift. Antigenic shift is the culprit behind Influenza outbreaks that have caught us off guard throughout history.
Flu Pandemics
Year
| Strain
| Origin
| Estimated # of Deaths
|
|---|---|---|---|
1889-1890
| H2N2 or H3N8
| Spain
| 1 million
|
1918
| H1N1
| Spain
| 50-100 million
|
1957-58
| H2N2
| Asia
| 1-1.5 million
|
1967-68
| H3N2
| Hong Kong
| 1 million
|
2009
| H1N1
| Mexico
| 2500-6000
|
The Russian Flu or Red Flu was named for the supposed place of origin, although it was later attributed to starting in China. It is not included in the table as it was an epidemic affecting children and did not reach pandemic status.
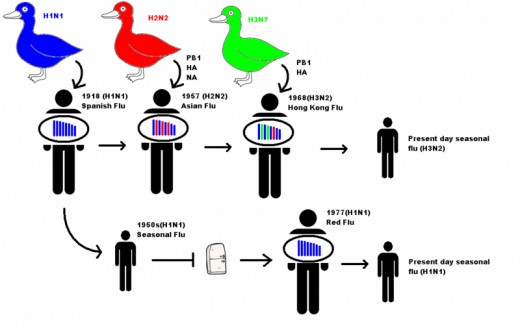
The major takeaway from the above diagram is these reassorted, novel strains go on to cause pandemics. Pandemics are global epidemics. Epidemics are classified as fast spreading disease outbreaks where the number of infected and or the spread of the infection exceeds normal expectations. While an endemic is an infection that is contained within a population or geographic where it originated.
The three major types are Influenza A, B, and C. This nomenclature goes in order of severity of infection. A is the type that almost all outbreaks are caused by, B causes a milder infection than A, and C doesn’t really cause much infection at all. Influenza A causes 95% of all flu infections. The remaining 5% is largely Influenza B. Influenza B has not caused any pandemics because it can only infect two different species, us and seals. While Influenza A can infect humans, pigs, birds and other animal species such as whales and horses. There is also an Influenza type D, which infects only cattle.
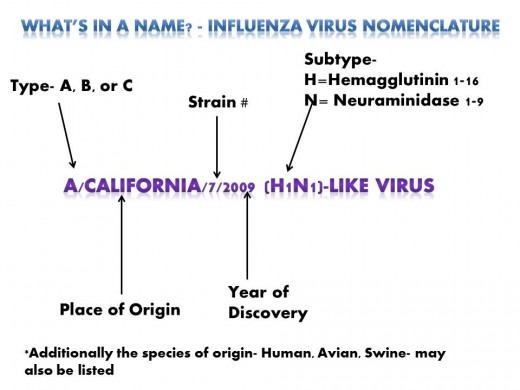
Since the 2009 flu outbreak, most people are familiar with the phrase H1N1. This additional naming of the flu virus is the subtype and it is only used for type A. As mentioned above, H refers to the hemagglutinin protein and N refers to neuraminidase protein.
Let's finish up our discussion with some basics. For the most part this article focused on Influenza A, as it is the numero uno opponent of humans. But there are additional types of Influenza.
In summary, the flu virus has a lot of tricks up its proverbial sleeve to attack your body. It is an always changing opponent. To protect yourself during flu season - take all the help you can get whether it be traditional western medicine- vaccines and antivirals- or alternative therapies- Echinacea, Elderberry, and Vitamin C- coupled with hand hygiene, low stress, and plenty of sleep.
Sources
http://www.virology.ws/ Influenza 101 by Vincent Racaniello. Wonderful resource with all the basics of influenze virology.
Centers for Disease Control. https://www.cdc.gov/flu/index.htm
Zhou et al. Genetic reassortment of avian, swine, and human influenza A viruses in American pigs. Journal of Virology. 1999.Oct;73(10):8851-6.