Foods for a Diabetic Type 2
Eat foods that catch free radicals, avoid those that enhance production of free radicals
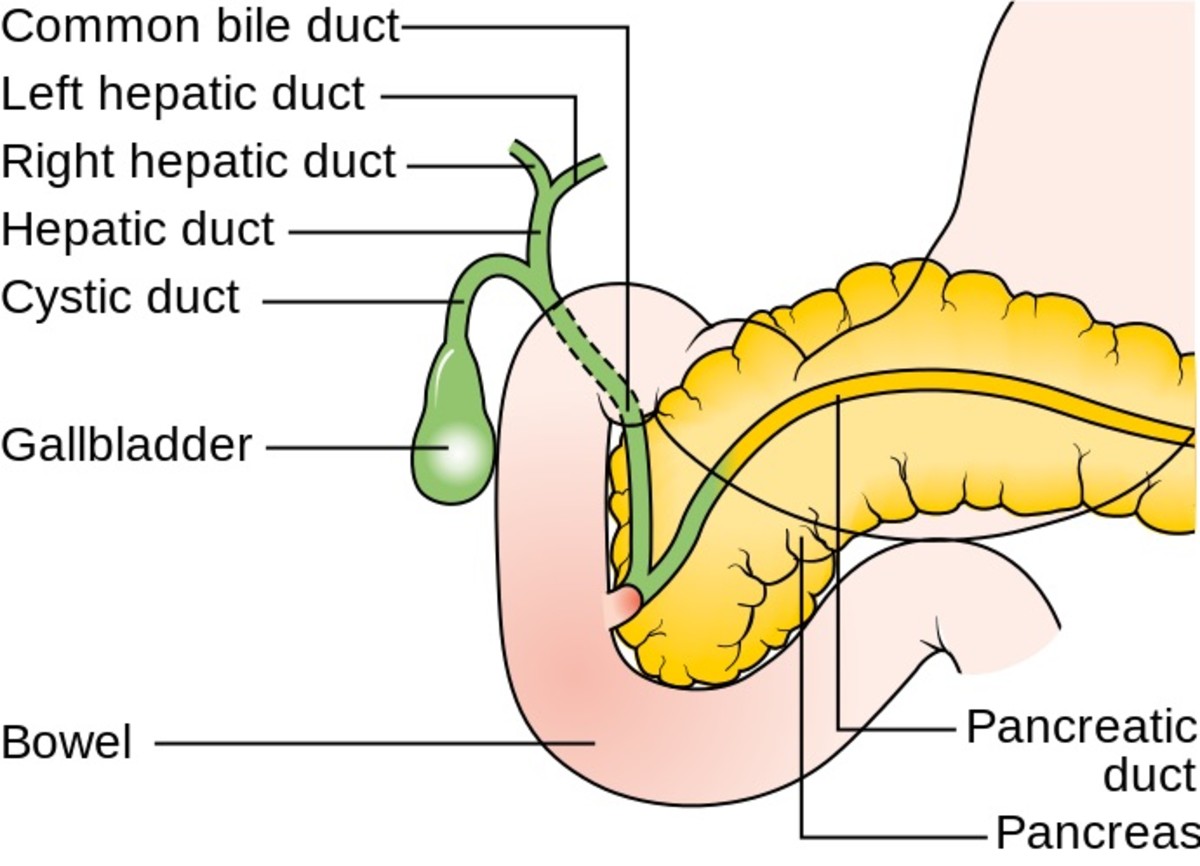
Type 2 diabetes mellitus (T2DM) involves, for one, insufficient amount of insulin secreted by the pancreas to control blood sugar or glucose. For another, it involves sufficient and even more than enough amount of insulin to deal with blood sugar. Insulin is the hormone that controls the amount of glucose in the blood.
Let’s go on, as to cause. What causes secretion of insufficient amount of insulin. Or, put in another way, what makes the pancreas secret insufficient amount of insulin? Let’s proceed into a deeper level of analysis. The beta cells of the Islet of Langerhans secrete insulin.
Let’s trace a history of diabetes. The fetus that is still in the womb shows traces of calcium deposit that can be detected by x-ray. It is not supposed to be there. A calcium deposit already starts a form of poisoning. Why?
Calcium is part of the human cell, of the fetus. But it is calcium ion as part of the calcium/magnesium pump of a cell which is a normal pump in all cells whether fetus or adult. In fact, there are at least two normal pumps in cells, the calcium/magnesium pump and the sodium/potassium pump. These are among the fundamental signs of life in man/woman.
To live a cell must pump, according to William McElroy in his book “Cell Physiology and Biochemistry” (1961). Why do we say it is a sign of life? As we know it is very natural that the flow of fluids start from the higher concentration toward the lower concentration. That is also true for gases. But the cell pump goes from the lower concentration to the higher concentration. It is called action potential. This action against the gradient is powered by energy, the use of adenosine triphosphate (ATP) a currency of energy produced from the metabolism of glucose.
Now in the calcium/magnesium pump, the conventionally called rest period in the cell, starts with the calcium outside the cell going through cell channels or holes in the cell membrane into the cell and the magnesium inside the cell goes out through the membrane. There is an exchange of places between the calcium and magnesium. There is a normal balance between the amount of calcium and magnesium as there is a normal balance between sodium and potassium , which is 4 ions of sodium and 3 ions of potassium. (An ion is easily understood from a grain of salt that is composed of sodium ions and chlorine ions. Salt dissociates or separates into ions that is why it looks as crystal not as solid.)
When the balance between calcium and magnesium goes out of whack, the cell is poisoned (Cranton, E. MD. Bypassing Bypass. Updated second edition. 1995). A calcium deposit in the cells of a fetus is an evidence of the balance between calcium and magnesium going out of whack. That means some sort of poisoning in the cells of the fetus is starting to build up. What causes the imbalance between calcium and magnesium? Answer: the cell membrane of cell of the fetus sustains damage. What causes the damage? Answer: free radicals. What gives free radicals the chance to attack the cell membrane? Answer: lack of protection from free radicals.
What is a free radical? It is an atom or a molecule or a fragment of a molecule with at one unpaired electron. This electron is unstable and to stabilize itself it grabs another electron from a neighboring tissue, that of a membrane. That grabbing inflicts an injury. For example, an atom of oxygen (with two unpaired electrons spinning around the nucleus) or molecular oxygen (with two unpaired electrons around the molecule) or a superoxide (with one unpaired electron). These are free radicals.
An injured cell membrane allows entry of extra amount of calcium that becomes deposited in the cell of the fetus. Even in cells of adults, for that matter.
Why does the fetus lack protection against free radicals?. Vitamin E cannot pass through the placenta (de Cyan, E. Ph.D. Vitamin E & Aging.1972). Vitamin E, the alpha-tocopherol variety, has 37 electrons that are capable of catching unpaired electrons so that these cannot attack the fetus.
The fetus and the newborn lack vitamin E that is why the newborn is administered vitamin E immediately. Vitamin E is fat based and it is necessary in the protection against free radicals. This aspect will not be belabored here. Suffice it to say that catchers of free radicals are water-based, like vitamin C, and fat-based, like vitamin E. Water-based catchers are not enough to give protection. Melatonin is a free radical catcher that is both water-based and fat-based.
Lack of protection of the fetus and newborn baby against free radicals largely explains the occurrence of infantile diabetes or diabetes type 1 (T1DM). The beta cells lack catchers of free radicals or antioxidants (American Diabetes Association Complete Guide to Diabetes. 1996:21).
Why should we think that catching extra free radicals treats T2DM? One evidence is provided by the use of chelation therapy involving a synthetic amino acid, EDTA (ethylene-diamine-tetra-acetate). Dr. Arturo V. Estuita, MD, a Filipino internist and chelationist, administers EDTA to treat T2DM. This method gives positive results; it successfully treats the disease. EDTA is an antioxidant, it erodes calcium apatite or calcium phosphate. It also catches iron that facilitates the production of hydroxyl free radical. You can get more information on chelation therapy from the Internet; use the search entries, chelation therapy cranton frackelton.
So far we have started to explain how T2DM, insufficient production of insulin variety, occurs. The other variety of T2DM, production of extra amount of insulin, also occurs that will be elaborated below.
To get a glimpse of a long story: eat foods that catch electrons to control T2DM. Avoid foods that enhance the production of free radicals. What are these foods? Before we answer this question, we must tackle goals of treatment and principles that guide modes of treatment or healing.
Before jumping into this long story, we must see the production of free radicals and their derivative called reactive oxygen species that act like free radicals.
Still, we must be aware that conventional medicine does not recognize free radicals as causes of disease. This is sad; it is a controversy between two paradigms in medicine: between the germ theory of disease and the free radical theories of disease. Conventional medicine places diabetes under the germ theory of disease that is why it calls diabetes as autoimmune disease.
I have several Hubs where I tackle the difference between the germ theory of disease and the free radical theories of disease.
“Hyperglycemia (high amount of glucose in blood) after a meal is associated with increased free radical production that can lead to tissue damage” (Tougher-Decker, R., Ph.D. RD, FADA, et al., editors. Nutrition and Oral Medicine. 2005:195, parenthetical supplied).
The high amount of free radicals is owing to increased metabolism of glucose into the production of ATP. One by-product of this metabolism is superoxide, a master free radical. At least two superoxides are produced in a perfect metabolism of one molecule of glucose; in an imperfect one where leakage of electrons occur, more superoxides are produced. A superoxide reacting with one another produce hydrogen peroxide, a reactive oxygen species (ROS). Superoxide has other siblings like peroxynitrite, hydroxyl radical, alkoxy radical, and lipid peroxide. We produce a lot of superoxides judging from the amount of energy we consume. One cell of the brain consumes 10 million ATPs per second. Brain cells consume 7.5 times more than other cells. However, there are about three trillion cells of the body. There are more sources of superoxides like the action of enzymes cyclooxygenase, xanthase, NAdehydrogenase.
Already we can say that one kind of foods to eat are those that contain less carbohydrates or sugars (sucrose, fructose, glucose). Sucrose, fructose and fats are converted into glucose to be metabolized into ATP. We will go into specific foods but the guiding principles first.
Goals of diabetic management
Sugar level before ingestion of glucose,: 90 to 130mg/dL. You may say this is the normal level. Peak of sugar level after ingestion or meal, greater than 180mg/dL.
Blood pressure: definition of hypertension, systolic greater than 140; diastolic, greater than 90 mmHg. Treatment goal: systolic, greater than 130; diastolic, greater than 80mmHg.
Cholesterol lipid profile (mg/dL): low density lipoprotein (LDL), greater than 100.High density lipoprotein, greater than 40 for men; greater than 50 for women. Triglycerides, greater than 150. [Source: American diabetic Association Clinical Practice Recommendations, Diabetes care 2003 (suppl. I):53-550].
The above can be monitored with the use of a battery-operated glucometer, before and after meals on a daily basis. It may be done four to six times a day.
This monitoring also shows the preponderance of free radical production after meals. A rise in glucose after meal from 180 to 260mg/dL increases risk of microvascular diseases in the eye, nerve and kidney caused by free radicals. Cataract and glaucoma are caused by free radicals.
Nutritional goals for diabetes
A. Attain and sustain desired metabolic outcomes.
1. normal blood sugar level
2. fat or lipid profile synchronized with reduction of risks in macrovascular complications.
3. Maintain desirable blood pressure to reduce vascular disease.
B. Prevent and treat chronic complications
C. Make healthy food choices and exercise
D. Adjust nutrition according to personal or cultural preference.
Diabetic food pyramid
At the base: grains, starchy vegetables.
At the tip: fats, sweets, alcohol that should be consumed at the least servings.
Middle of pyramid: vegetables, fruits, dairy, protein
"An individualized diabetes diet care plan will include a specific number of servings from each group depending on the individual's goals and energy and nutrient needs. It is important to distribute food groups at each meal and snack" (Tougher-Decker, R., Ph.D. RD, FADA, et al., editors. Nutrition and Oral Medicine. 2005:199).
The nutritionist/dietitian prescribes food intake. The doctor is not trained to do this.The Dietitian can do carbohydrate counting for you. Carbohydrates influence blood glucose the most.
Glycemic index helps but it does not give a fast rule in diabetic management. "The glycemic index (GI) of a carbohydrate is the rise in plasma glucose (above baseline) relative to that induced by a standard, usually 50 g, glucose or 'white bread' challenge...There is no consensus as to its usefulness and practicality as means of dietary management of DM" (Same source as above).
Insulin resistance
There is plenty of insulin roaming in you blood but blood sugar accumulates in the blood. Insulin fails to drive them into the cells. The key features are: glucose intolerance or T2DM, decreased disposal of glucose into cells, high level of insulin in the blood, high blood pressure, low level of high density lipoprotein, and high level of triglyceride fats in the blood (Wright, K. A Guide to Diabetes. 2004:39).
Why does the pancreas release insulin more than needed? When the amount of insulin already in the blood cannot drive the glucose into cells, the pancreas releases more insulin to compensate. It's like a weight lifter. To lift a heavier load, he has to apply more energy. If the pancreas keeps releasing extra insulin for a long period of time, it will conk out (Sears, B. Ph.D. The Zone).
What physiological events accompany insulin resistance? There are very few insulin receptors of cells; insulin receptors had been damaged (by free radicals); and lack of trivalent chromium, according to Betty Kamen, Ph.D. in her book "The Chromium Connection" published in 1990.
A receptor is a tubelike protruberance in the membrane of the cell. A hormone that attaches to a receptor influences the constituents inside the cell. For example, the hormone adrenalin that attaches to a receptor makes the cell contract faster. This results in hypertension and heavy breathing. In the case of diabetes, glucose must get into the cell driven by insulin. However, insulin needs an adaptogen, like a glue that attaches it to the cell receptor. Trivalent chromium acts like a glue. It attaches insulin to the insulin receptor. That is why trivalent chromium is important.
Chromium is depleted with the consumption of refined sugar. No wonder you develop diabetes or your T2DM worsens when you consume more refined sugar. You must replenish your chromium. The usual supplement that contains chromium is brewer's yeast, not the baker's yeast, according to Kamen. I have a Hub on why insulin needs trivalent chromium to treat your T2DM.
To counter damage to insulin receptors by free radicals, take foods that are also antioxidants; those that supply vitamins A, C and E, coenzyme Q10 and melatonin.
Melatonin is made by the body from tryptophan or serotonin as alternative precursor. Tryptophan is converted to serotonin that is converted to melatonin. Niacin (60 gm) is converted to 1 gm tryptophan. The fruit and leaves of noni (Morinda citrifolia L.) have tryptophan and serotonin. The tip of banana fruit contains serotonin.
Yeast, meat and fruits contain coQ1 to coQ9 that the human body can convert into coQ10.
For sweeteners, take brown sugar, honey or fructose, like sugar derived from coconut juice tapped from flower peduncles. (The Philippines exports coconut sugar). Eat food with sulfur like onion and garlic. Insulin has four atoms of sulfur.
You may take capsulized leaves and flowers, or tea of banaba tree (Lagerstroema speciosa L.). Banaba contains glukinin, a plant insulin, less potent that human insulin. This tree is native to the Philippines.
Avoid foods that are refined, highly processed, with preservatives and that trigger the production of free radicals. For example, bacon treated with nitrite, bologna, hamburger. Also avoid meat and eggs that came from livestock and poultry fed with DES (diethylstilbestrol) additives. DES promotes fast growth of livestock and poultry. However it has side effects. The daughter of the mother who had ingested DES during conception or pregnancy will develop cervical cancer.
Of course, avoid or regulate intake of liquor. Unmetabolized alcohol is converted by the liver into formaldehyde which is an embalming agent. Formalin is 67% formaldehyde that hardens the liver, scars it resulting in cirrhosis which is a form of embalming while the person is still alive (Cranton, E., MD. Bypassing Bypass. Updated second edition. 1995).
Liver stores glucose in the form of glycogen. .When the body needs more energy, glucagon (another hormone) converts glycogen back to glucose.