- HubPages»
- Health»
- Women's Health»
- Pregnancy
Pregnancy induced hypertension and Pre-Eclampsia
Signs of Pre-Eclampsia
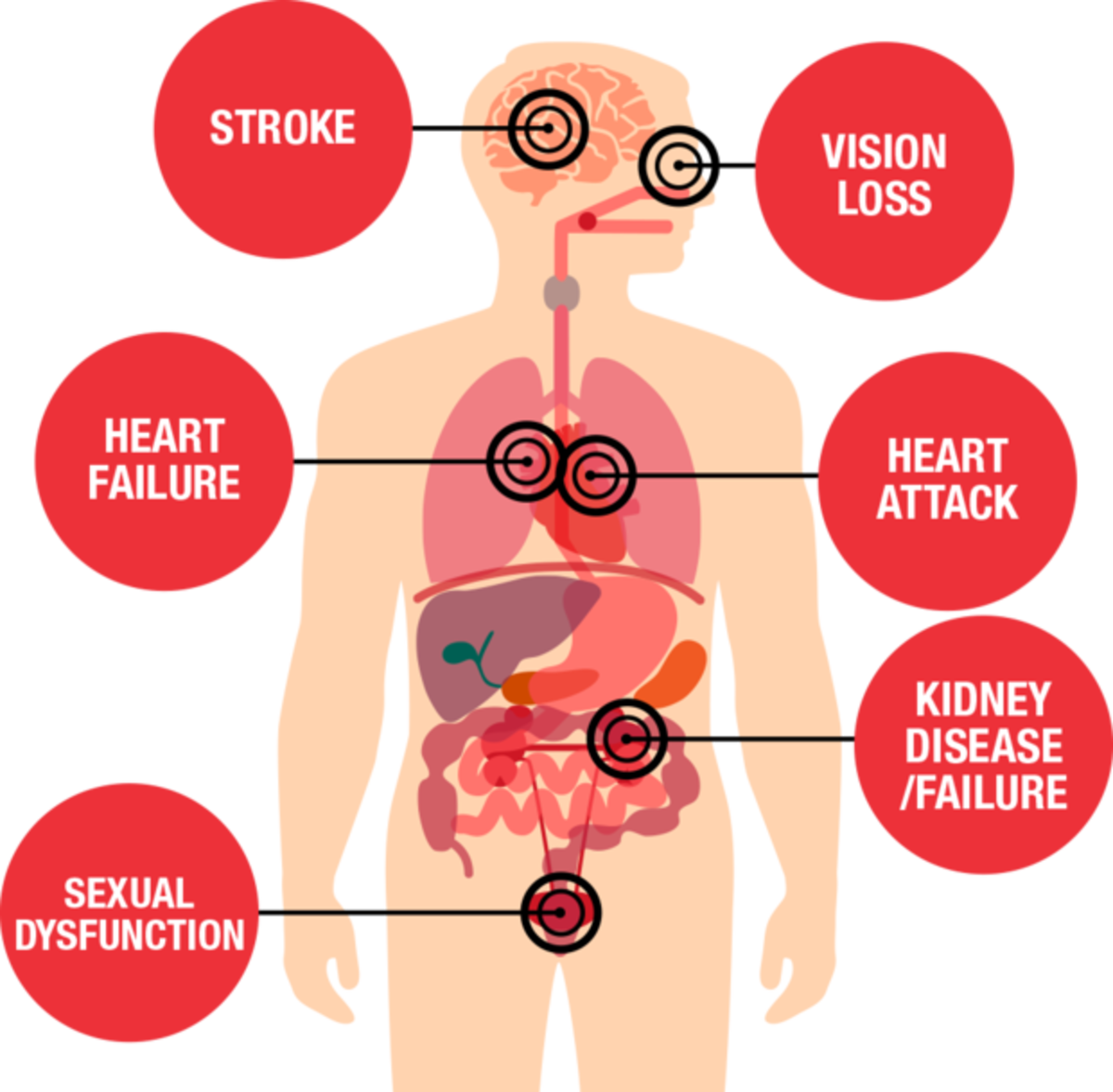
In pregnancy, blood pressure is monitored every time you visit your midwife, any rise in your blood pressure can be one of the first signs of a condition called Pre-Eclampsia. This is also known as pregnancy induced hypertension (PIH) or Pre-Eclamptic Toxaemia (PET).
- Some of the symptoms of pre-eclampsia are
- Raised Blood pressure
- Dizziness or fainting
- Protein in your urine
- Not Urinating enough
- Oedema (Swelling) of your Legs, hands, face or feet
- Pain just below your ribs
- problems with your vision such as seeing flashing lights or blurred vision
- Persistent Bad Headaches
- Vomiting
- Confusion
- Seizures
These symptoms can manifest themselves as one or a combination of a few of these symptoms and the only way to confirm a suspected pre eclampsia is to be taken care of in a hospital under a consultant Obstetrician where they can perform a series of blood tests to confirm this.
However it has been known with just a few women to have severe Pre-Eclampsia without any of these symptoms at all.
What causes Pre Eclampsia?
Its not very clear what really causes Pre Eclampsia but it is thought to be some kind of injury to your blood vessels or disruption to the hormones that maintain the blood vessels, this triggers off a chain of physiological changes in the woman's body that can have a serious effect on the mother and her baby.
If Blood pressure goes up too high to a dangerous level then this can trigger off an Eclamptic fit, called Eclampsia. It is life threatening if left untreated.
How can my baby be affected?
Pre eclampsia can be very serious for your baby
- A raised blood pressure can restrict the flow of blood through the vessels of the placenta, therefore depleting the nutrients to the baby. This in turn causes baby to be growth restricted and small. A baby with growth restriction can have problems maintaining it's temperature and have problems feeding.
- High Blood pressure can also lead to the depletion of the placental vessels and they begin to separate from the wall of the uterus causing severe bleeding and abdominal pain. This is called a placental abruption, the excessive bleeding can cause death of the mother and baby.
Who is at risk of Developing pre eclampsia?
You are at risk of developing this condition if:
- This is your first pregnancy
- If you Smoke
- Have a raised BMI (Body mass Index) of 30 or more
- If Pre Eclampsia runs in the family ie: your mother and or your sisters had it with their pregnancies
- Your a teenager or over 40 years of age.
- You already have high blood pressure before you became pregnant
- You are having a twin pregnancy or mutiple pregnancy.
Research has shown that taking a low dose aspirin every day for women with these risk factors has a preventative effect towards developing pre eclampsia, speak to your midwife of obstetrician before taking any medication in your pregnancy.
What treatments are there to stop Pre eclampsia?
There are medication that can be given to women who develop pre eclampsia in pregnancy to help lower blood pressure.
If the medications do not work or the maximum doses are given then the best way to stop pre eclampsia is to deliver your baby. Most blood pressure problems develop in late pregnancy, but if you are delivering a premature baby then there are drugs that can be given to you to help the babys lungs mature quicker. There is also the risk of your baby being cared for on the neonatal unit as they are at risk of developing complications especially if they are growth restricted or premature.
- Phases of Labour Explained - Latent and first stage of Labour.
What are the stages of labour and how do you know when you are in Labour? How can you cope with the early stages of labour - read this article and find out! - Second and Third stages of labour explained
What ids the second stage of labour? What does it feel like? How is the placenta delivered and when? Read this useful article and find out. - Pethidine in Labour
Using pethidine in labour is down to personal choices and also how you wish to manage your labour and delivery, but don't rule it out of your plans as some women can cope perfectly well without further drugs and there are situations when pethidine in - Infections transmitted during Pregnancy
Infections in pregnancy can affect the Mother and the unborn baby in different ways. Here are just a few of the common infections that are prevalent in the UK and which ones we routinely test.