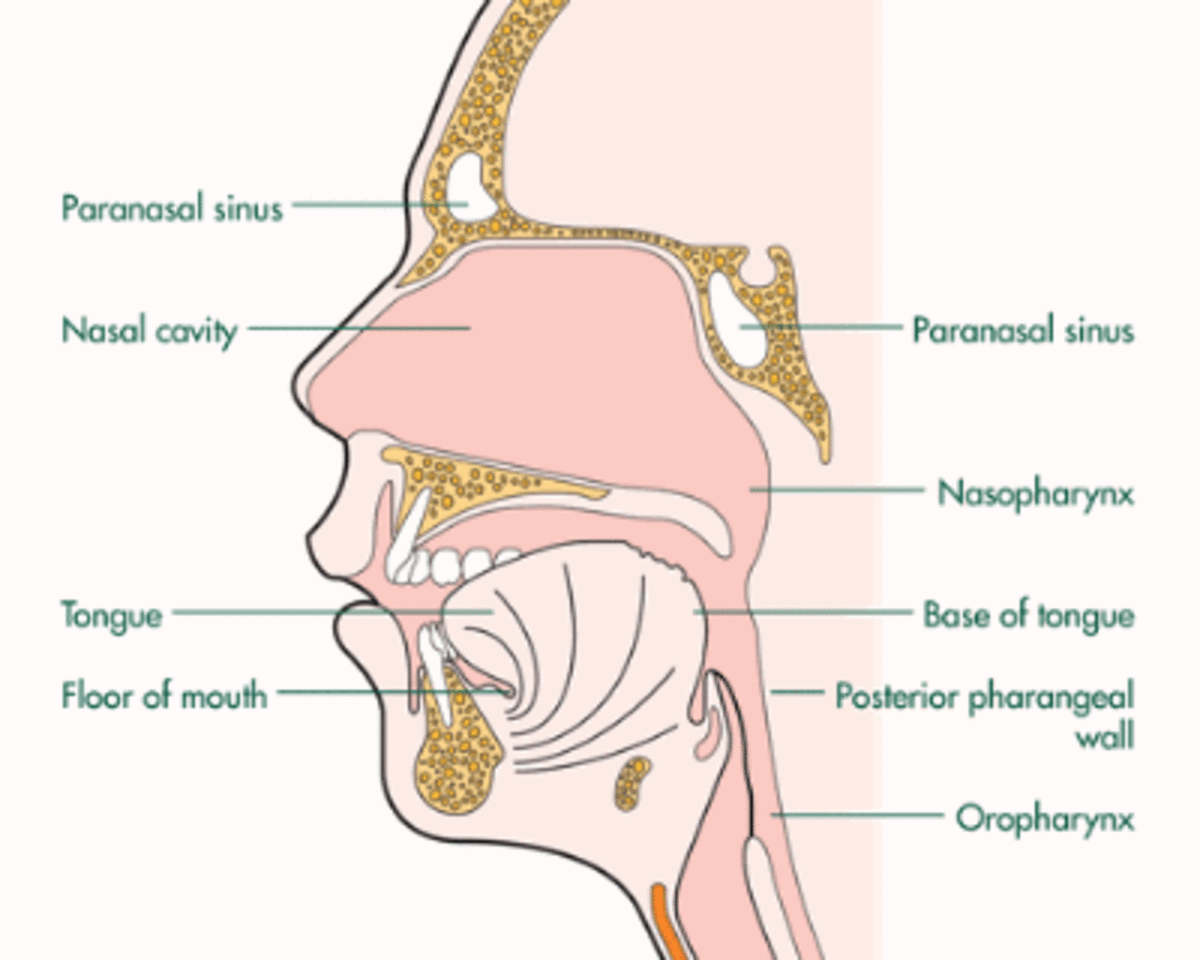
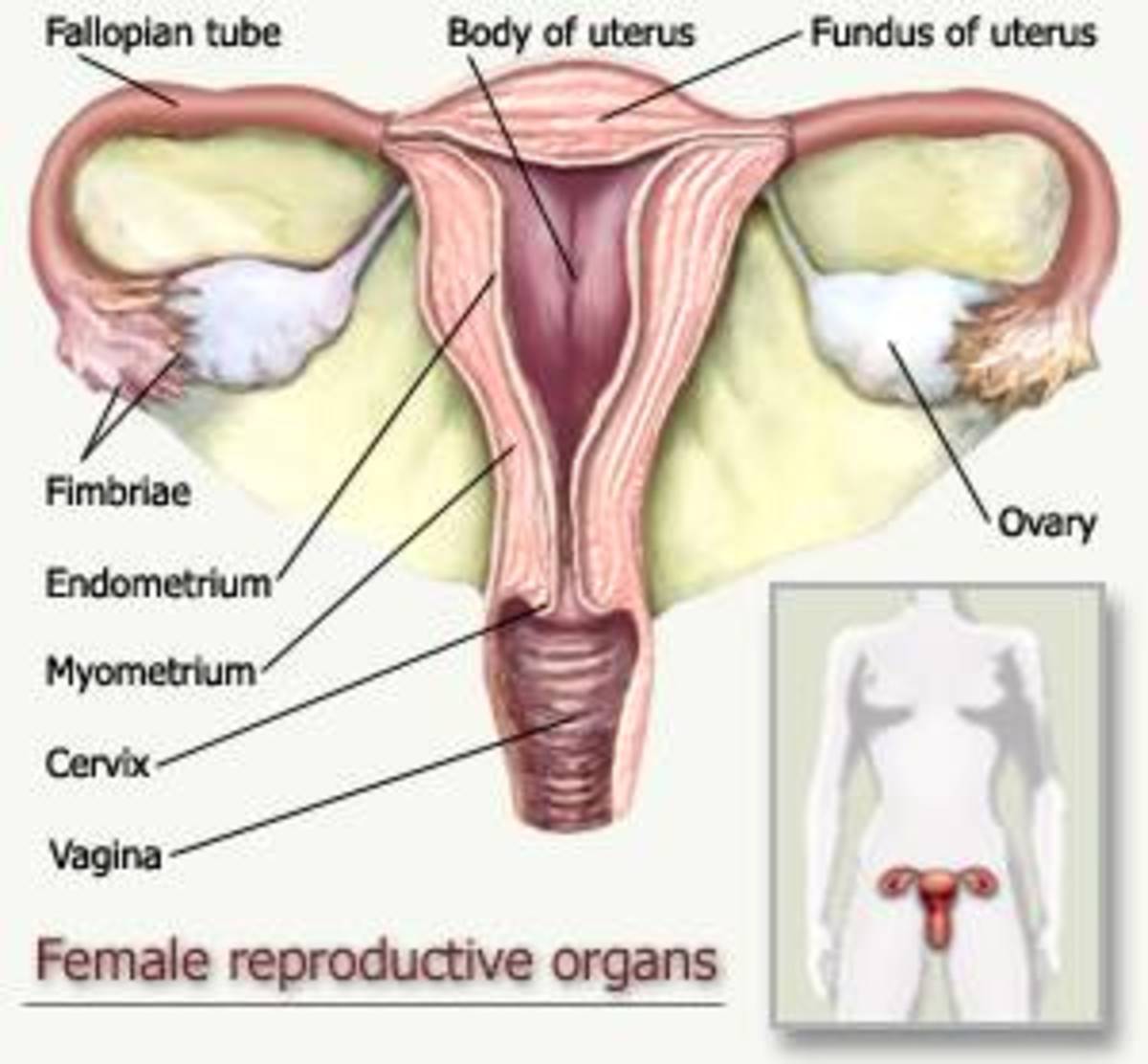
How Heritable Colon Cancer Develops from a Polyp (Benign Tumor)
Polyps in a colon

Antioxidant against free radical damage
A mutation in a gene is inherited and when five to seven mutations more occur in genes of the same polyp, colon cancer is initiated
There are two pathways of heritable predisposition to colon cancer. One is called familial adenomatous polyposis (FAP), an autosomal dominant trait. Another pathway is called hereditary nonpolyposis colon cancer (HNPCC), also an autosomal dominant trait. Autosomal means it is not associated with sex genes like XY of man and XX of woman. So, both man and women can get FAP or HNPCC.
HNPCC is 15 percent associated with defect in DNA repair and with genomic instability. (We will take up HNPCC in more detail in another Hub).
Let us focus on FAP. One percent of all cases of colon cancer is FAP; it occurs in 3 out of 1,000 persons.
Polyps, benign tumors, are found in large intestines. They precede or accompany colon cancer and are considered as first step in colon cancer development. A person with FAP has thousands of polyps. Chances are high that one polyp will develop into adenoma then cancer. Cancer can start with only one polyp.
One inherited mutation plus 5 to 7 more
FAP starts with the mutation of a gene called adenomatosis polyposis coli (APC) during the development of the egg or the "seed" of the father. This process is called meiosis. Such mutation is carried by the 23 chromosomes contributed by the mother or by 23 chromosomes contributed by the father during fertilization. After fertilization, a fetus (with 46 chromosomes) develops that carries one mutated APC. Now we have a sibling composed of mitotic or dividing cells with one mutated APC in each mitotic cell. In the sibling, for one polyp to develop into colon cancer, 5 to 7 mutations more in other genes of a mitotic cell should occur. If it sustained mutations fewer than five, the polyp will develop into a benign tumor or incur intermediate growths. The number and sequence of mutations are important.
Imagine that we are going to see a demonstration of how colon cancer is initiated and how it develops. Let us get inside one enlarged cell, one polyp, accompanied by a guide. Just getting past the cell member of this polyp, our guide begins:
First mutation
"This is the nucleus of this polyp cell. There are 46 chromosomes inside the nucleus and you can number them from #1 to #46. Each chromosome is double helix, like a spiral stairway with one step holder on the left and another step holder on the right. The two joints (left and right) constitute one gene. The joint on the left is an allele; the joint on the right is also an allele. Let us put a tag on the left allele APC, notice that it is in capital letters, meaning dominant. Let us put a tag on the right allele apc, notice that it is in small letters, meaning that it is different but show the same effect in the same person, as polyp/cancer. APC and apc are read the same way but they appear different which shows an inheritance pattern that is called heterozygous dominant. (We will not go further into technical detail). A chromosome is made up of DNA or deoxyribonucleic acid. DNA has a phosphate group, a protein group and a sugar group. A chromosome has a divider across its diameter, not in the middle, that is why it has a long arm indicated as q and a short arm indicated as p"
You ask: what does APC further indicate? The guide eagerly answers:
"Mutation in APC is inherited. This mutation is spontaneous; it occurred during the development of the egg of the mother or in the "seed" of the father. APC has a defect that came from one of the parents of the person who has this polyp. apc is a normal allele. A person who had inherited APC has APC allele in all his cells and apc allele in all his cells. But this single mutation in APC of this polyp, does not make it cancerous. You can see that APC and apc are located corresponding to each other in the long arm of chromosome #5. The mutation of APC is the first mutation. A person with APC can spend a whole lifetime without contracting colon cancer unless...."
Let us walk to another chromosome, #12. Our guide continues her demonstration:
Second mutation
"This is the start of the second step in the development of colon cancer. Look closer into a tagged gene in the short arm of chromosome #12. This gene is called k-ras proto-oncogene, which consists of two copies of alleles. One k-ras allele is mutated that transforms this polyp cell into adenoma, "an intermediate tumor with fingerlike projections," according to Michael Cummings in his book Human Heredity, Principles and Issues published in 2009, pages 293 to 296."
We take note that mutation in one copy of k-ras transforms this polyp into adenoma; the other allele is normal. This is the second mutation that occurs now in the mitotic cells that make up the sibling. We expect to see three more mutations to finally witness the development of a full-blown colon cancer. Let's walk to chromosome #18. Our guide continues explaining:
Third mutation
"This is chromosome #18 of this polyp. Notice that a gene tagged as DCC is located in its long arm. Please take note also that the two alleles of gene DCC are both mutated. This is the third mutation toward the development of colon cancer. It occurs in the mitotic cell of the sibling."
We notice two more tags in long arm of chromosome #18. Our guide looks apologetic or agitated, who proceeds in her demonstration:
Fourth and fifth mutations
"In the long arm of chromosome #18, two more mutated genes are found. Gene DPCA has both copies of its alleles mutated; gene V18-1 has both copies of its alleles mutated. These are the fourth and fifth mutations, respectively. Their mutations add to the accumulating mutations in this polyp cell. These mutations occur in the mitotic cell of the sibling. You may expect to see cancer developed shortly."
We get irritated. We interrupt our guide by asking, half commenting.
"These mutations seem to get on smoothly with nothing to stop them? Is this polyp so helpless?"
Our guide walks us fast to chromosome #17.
"Look into the short arm of chromosome #17. It has p53 gene. This is a suppressor gene, so-called because it is a switch. Switched on, it stops the otherwise uncontrolled growth of this polyp that was turned into adenoma by a mutation of one allele of k-ras gene. Switched off, the same adenoma goes on dividing in the process called mitosis. One adenoma would divide into two adenomas; two adenomas would divide into four polyps, and so forth and so on. These divisions would make for the uncontrolled growth of this formerly one polyp. Each new adenoma contains at least a mutated APC, a normal apc, a k-ras with one mutated allele; a DCC with both alleles mutated; a DC4 with both alleles mutated; a DPCA with both alleles mutated; and a V18-1 with both alleles mutated. Additional mutations occur in each generation and rate of growth increases with each generation.
Switching off the guard
"The last step in the development of colon cancer involves p53 gene. It had been overwhelmed by the accumulated mutations in genes of this polyp. It is also susceptible to factors (sporadic or environmental) that cause its mutation. In this last step, both alleles of p53 gene of a mitotic cell are mutated. Now, it is switched off."
What happens when it is switched off?" you ask anxiously.Our guide answers:
"In the case of inherited predisposition to colon cancer, the mutated p53 genes have nothing to do with the inherited mutated APC. The mutated p53 gene fails to stop the cell cycle of the cell that sustains mutations in apc, k-ras, DCC, DCA, DPCA, and V18-1. A normal p53 gene can stop the cell cycle in two checkpoints in the interphase: one at transition between G1 to S and another at transition between G2 and M or mitosis. Once mitosis has started, colon cancer develops.
Our guide catches her breath and blurts out:
"Let's get out of this polyp lest we get swamped by fast dividing, growing polyps. Mutated cells divide much faster than normal cells."
Now, we are out of the polyp's reach. We are witnessing an increasing number of adenoma stretching the matrix of the polyp that confined it until the matrix breaks down. The first part to give in is its bottom, dissolved by protease or bromelain that come from, for example, pineapple and papaya. This former polyp had developed into adenoma, now to cancer. Thousands of cancerous cells break out and invade the neighboring normal cell. Eventually this normal cell gets infected and more normal cells get infected. The infection spreads. Cancerous cells go to lymph fluid and blood.
In fact, p53 gene is like a switch that when switched on it suppresses the development of other kinds of cancer like breast, lung, and brain cancers.
Causes of mutation
Spontaneous mutation means that mutation had occurred during meiosis or the production of “seed” in the male and egg in the female. This mutation had happened even before fertilization of the egg by the “seed.” Spontaneous mutation consists, among others, deletion of gene, or substitution of amino acids or aberration of chromosomes, like breaks, shortening, thickening and gap.
Sporadic also means environmental that consists of free radicals and X-rays. Free radicals are by-products of normal metabolism in the body, like the production of energy from glucose. Ozone from the atmosphere and electrical gadgets of starters of cars are free radicals. Nitrous oxide from pollution is a free radical. Hydrogen peroxide, derived from oxygen, acts like a free radical. Singlet oxygen, derived from molecular oxygen, is a reactive oxygen species (ROS). Low density lipoprotein, a kind of cholesterol, is turned by free radicals into bad cholesterol and is a ROS. Several ROS are derived from pesticides, herbicides, and fungicides.
Nitrosamine, used to preserve meat, contains free radicals. Tobacco, chewed or smoked, contains free radicals and X-rays that cause mutation in cells. (I have a Hub "Reopening a "Book on Tobacco:" Recasting A Case Study in "Politics of Cancer" by Dr. Samuel S. Epstein, MD").
“Charring food oxidizes it, producing free radical precursors, and this is the reason that charbroiled food are carcinogenic....” (Cranton, E. MD and A. Brecher. Bypassing Bypass. Updated edition. 1984:180).
A carcinogen is a substance that contains free radicals or X-rays that cause mutation in cells resulting in cancer, heart disease, and other diseases.
Free radicals and X-ray can cause the mutations in apc, k-ras, DCC, DCA, DPCA, V18-1 and p53 gene. Free radicals and X-ray can cause mutations in gene apc of a person who did not inherit a mutation in this gene. Conventional medicine ignores free radicals as causes of mutation. This is the main reason why it had not developed an effective means of preventing cancer. However, it has recognized X-ray or radiation as a cause of cancer. I have a Hub "How Free Radicals and X-rays In Cigarette Smoke, Not Tar, Cause Cancer and Heart Disease."
How does a free radical cause mutation? Take molecular oxygen that consists of two atoms of oxygen joined covalently. It has one unpaired, free electron, on each atom. The two unpaired electrons spin around the molecule in the same direction. Each unpaired electron is unstable and is looking for a partner. It gets a partner electron from a molecule, like DNA. DNA is composed of genes. Injury in genes results in mutation. In FAP, free radicals mutate apc, k-ras, DCC, DCA, DPCA, V18-1 and p53 gene. Their mutations result in colon cancer.
How does X-ray cause mutation? X-ray is energy emitted by radioactive material like lead 210 or polonium 210 that are found in tobacco. X-ray excites electrons in inner orbitals of an atom, for example, a phosphorus (P) atom with three orbitals. An orbital is a path of electrons as they spin around the nucleus of the atom. A P atom has two electrons in its innermost orbital, 8 in its middle orbital, and 5 electrons in its outermost. X-rays excite an electron in its innermost orbital and ejects it out of the orbital. This ejection changes the nature of P atom. P is one of the atoms that compose DNA, the hereditary material. A change in P results in mutation. X-rays can eject atoms of other elements composing DNA like nitrogen, carbon and hydrogen. X-rays can cause mutations in genes apc, k-ras, DCC, DC4, DPCA, V18-1, and p53 gene that result in colon cancer.
(This Hub was overly long that is why I made its former second half part into another Hub "Even Without An Inherited Polyp A Person Can Develop Colon Cancer"). This Hub elaborates how to prevent and treat colon cancer