How Stress Affects the Immune System
We've all heard of the "mind-body connection" and that "stress makes you sick." But, are they the stress hormones themselves that make us sick, or do our unhealthy habits during stressful situations make us more prone to illness?
This article examines three of the hundreds of discoveries made over recent decades that mainstream the medical understanding of the psycho-neuro-immunology connection.
Immunosuppression Model
Most of us understand the basic relationship between stress, immunity, and disease. This model (Miller and others 2002), describes how stress suppresses the immune system, leaving us vulnerable to disease and infection. But, have you wondered what actually accounts for this reaction?
Three hypotheses are discussed in brief here:
- Direct Effect Hypothesis
- Indirect Effect Hypothesis
- Allostatic Load Hypothesis (referring to the duration of stress)
These three hypotheses are now seen as complimentary and are commonly accepted in the psychological and medical communities today.
Direct Effect Hypothesis
The Direct Effect Hypothesis asserts that stress affects the nervous, endocrine, and immune systems, the effects of which can directly lead to disease.
This hypothesis states that, at the cellular level, stress hormones (which produce immunosuppression) and lymphocytes have epinephrine and norepinephrine receptors for corticosteriod (stress) hormones. Stress activates these systems, directly affecting the nervous, endocrine, and immune systems, leading to disease.
Indirect Effect Hypothesis
This hypothesis contends that stress leads us to employ maladaptive behaviors (such as smoking, over-eating or eating poorly, consuming alcohol or drugs, sleeping less, exercising less, etc.), which behaviors then lead to slower healing times and lowered white blood cell activity.
For example, drinking alcohol and/or taking drugs can lead to irregular sleep patterns. The deep sleep needed for secretion of growth hormones that facilitate wound healing by activating macrophages to kill bacteria are not produced, thereby delaying healing.

Allostatic Load (The Effects of Long-Term Stress)
B.S. McEwen describes allostatis as the duration of stress and the cumulative, long-term effects of the body's physiological response to stress, especially stressors that are unpredictable, uncontrollable, longer in duration, and difficult to cope with.
The effects of a heavy allostatic load seem to be a form of accelerated aging, and include:
- Decreased immunity
- Elevated epinephrine levels
- Increased abdominal fat
- Decreased hippocampus size (reduces thinking and memory)
- Overproduction of proinflammatory molecules produced by immune cells that communicate with our neurons
The ability to recover from a stressful experience has a lot to do with the total burden that stressor has on us.
Modern Illnesses from Modern-day Stress
Research has shown reduced immune functioning following major life events such as divorce, death of a loved one, unemployment, also during military training, academic exam times, and job-related stress.
Those of us who overreact to stress or don't know how to handle stress properly are significantly more prone to illness and disease.
To learn more about effectively coping with stress, see: How to Cope with Stressful Situations and How to Deal with Physiologic Stress.
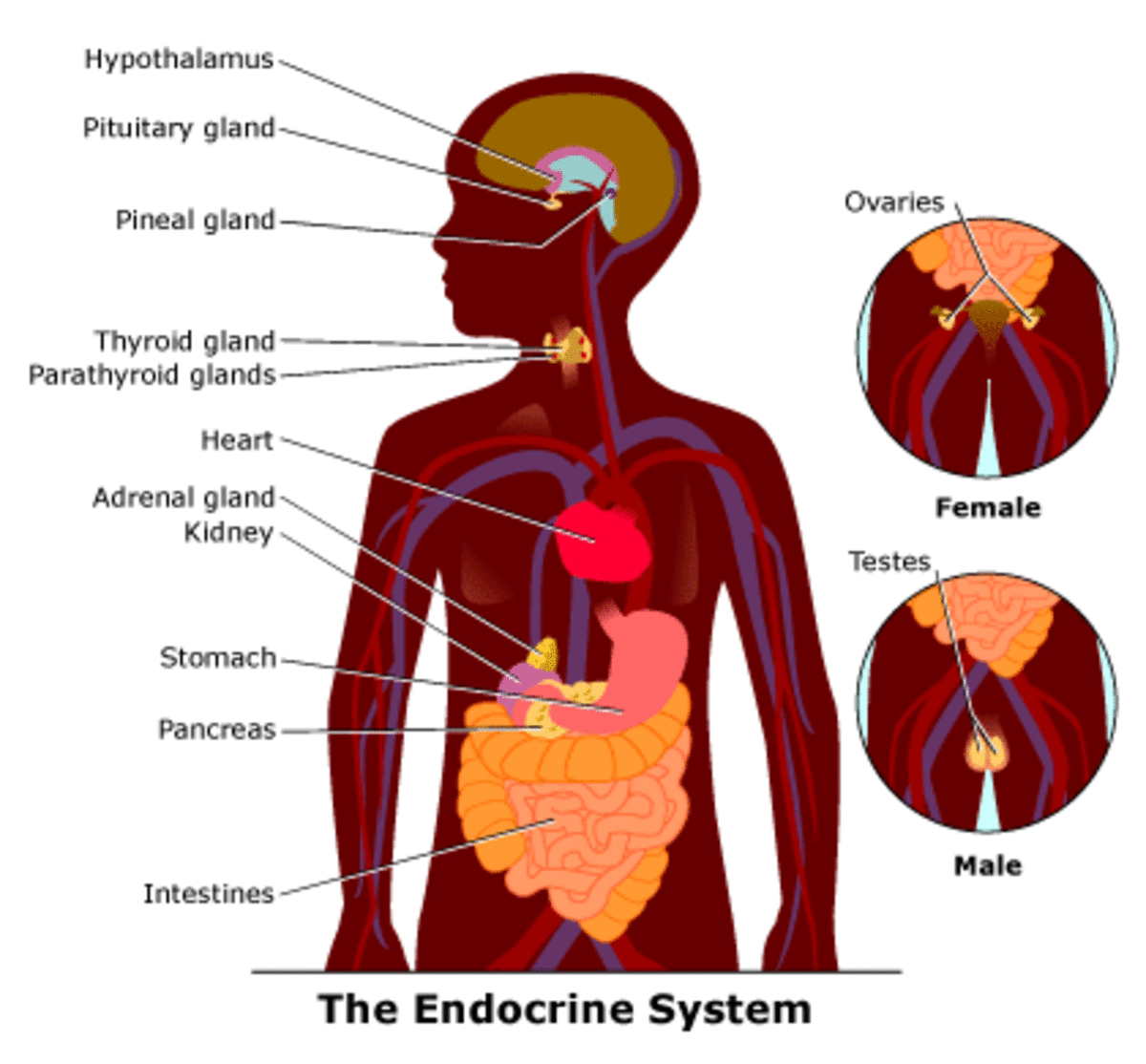
Brain/Endocrine System
In essence, the immune system doesn't work alone. It is part of a coordinated system involving both the brain and the hormone-secreting endocrine system. The brain regulates the production of stress hormones, which in turn influence the body's immune defenses, directly and indirectly.