How to Cope with Cancer: High Blood Calcium Levels
Coping with cancer is never easy for the patients and their families alike. Having been one of them I know that well. Truth is, cancer definitely affects your daily life and the quality of day-to-day living. There are a lot of issues that need to be handled, including pain, and new health conditions that have to be managed. Keeping your blood calcium levels as close as normal is essential, for many reasons than one, and here is why:
Importance of Calcium in Our Body
Calcium is a mineral and key player in bone health that must constantly be consumed to be able to keep the blood calcium within normal levels and build bones. Although 99% of calcium is stored in bone tissues, the remaining 1% that circulates in the body fluids, like blood, or inside the cells, is equally important. Other than helping build bones and teeth and allowing muscles work properly, it is also responsible for blood clotting and for ensuring the normal brain and central nervous system function.
As previously mentioned, calcium is absorbed in our bodies via the food we eat and then stored in the bones. The amounts of calcium released in bloodstream are very carefully controlled by our bodies. Our system is alert; so, if blood calcium levels drop in dangerous low levels, the bones release amounts of calcium to meet normal bloodstream calcium levels as much as possible. Supplementary, the body absorbs more calcium from food intake and the kidneys, which act like refining machines, get rid of calcium in less amounts that normal, through urine. Of course it is a vice versa function when calcium levels get too high.
Hypercalceamia
Having either too high or too low blood calcium levels is dangerous. Too much calcium in the blood leads to a condition called hypercalcaemia. “Hyper” is a Greek prefix meaning “too much”. It is estimated that 10% of people with cancer develop hypercalceamia, most usually in the advanced levels, although there are cases when hypercalceamia is developed in earlier ones. It happens because cancer makes calcium that is stored in bones leak out and enter the bloodstream, which in turns increases the calcium levels. The same applies to people that have bone metastasis. Kidneys may also be affected since they might not be able to get rid of excessive amounts of calcium. Other than the aforementioned, being sick and dehydrated might also affect the blood calcium levels.
Hypecalceamia is a serious condition that must be treated; otherwise, the patient might feel more and more drowsy as days go by, sleep most of their time, which may lead into passing into a comma state and eventually die. Hypercalceamia is usually most common among people with multiple myeloma, kidney cancer, prostate cancer, breast cancer, head and neck cancers and squamous cell lung cancer. It is estimated that about 10% to 30% of cancer patients have hypercalceamia and unfortunately, its prognosis is rather poor, due to its similarity with disseminated disease.
It is also proven that chemotherapy in breast and lung cancer patients also affects blood calcium levels; in cases with cancer-hypercalceamia, chemotherapy is found to drop blood calcium levels.
Pathophysiology, Signs and Symptoms of Hypercalceamia
Symptomatology
The problem with hyperclceamia is that you might not have any symptomatology. Feeling rather weak or not well are enough to bring you to the doctor’s office to get you tested, since the severity of hypercaleamia is not equivalent to increasing blood calcium levels. Meaning, there are patients with picky calcium blood levels and experience severe symptoms and vice versa. What makes it difficult for doctors to pick up with hypercaleamia is the fact that symptoms of hypercaleamia are very much the same with symptoms in the advanced cancer levels.
So, it is advised to see your doctor is you experience fatigue, weakness and/or lethargy, loss of interest or reduced concentration, constipation, anorexia, or mild confusion. If you fail to treat hypercalceamia in its early stages, you may progress into feeling very thirsty, sick, drowsy, agitated, experience muscle spasms, pain and weakness in the bones, tremors, heart beat out of the regular and difficulty in speaking and thinking clearly, have seizures and hallucinations, be unable to coordinate muscle movement; thus not be able to move and walk properly, before you enter the final fatal stage (if you leave hypercalceamia untreated).
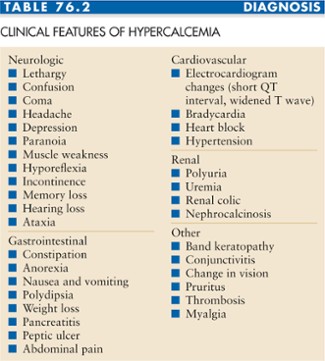

How to Treat Hypercalceamia
Of course, lowering blood calcium levels is the main target, alongside trying to relief from the aforementioned symptoms.
The most commonly used and effective treatments for hypercalceamia are:
1. Bisphosphonates
Bisphosphonates are drugs that have proven to be effective when trying to treat hypercalceamia. You can take them either as tablets or through a drip into your vein; however, it is highly likely that you would need vein-fluids coming in your system. Apart from reducing blood calcium levels, bisphosphonates help relieve from bone metastasis and partially prevent bones that are damaged to break. However, it is advised you run blood tests regularly, as bisphosphonates could reduce your blood calcium levels too low and cause hypocalcaemia. At this point, you should notice any symptoms that indicate any change in your sensations, such as tongue-burning and lip-burning feeling or tingling.
As soon as hypercalceamia is diagnosed, patients are given bisphosphonates intravenously for their proven effectiveness on decreasing bone breakdown. Other possible benefits deriving from bisphosphonates is that they could diminish bone pain and hold back this condition from turning into other types of cancer, like breast cancer, lung cancer and multiple myeloma.
2. Calcitonin
Apart from Bisphosphonates, calcitonin can also help prevent damaged bone breakage. It is an injected drug and can be supplemented with other hypercalceamia-symptoms relief drugs.
However, it is not very widely used due to its short-lived effects that last only up to 3 days. Also, it is not recommended to have repeated doses of calcitonin as the body develops tolerance to all the lower-calcium-levels attempts and has no real effect.
3. Denosumab
Denosumab is a monoclonal antibody. Monoclonal antibodies attach to proteins found on cell surface and work according to the protein they have attached to. Each monoclonal antibiotic recognizes one protein only and attaches to it. A variety of monoclonal antibodies are available for cancer treatment and there are also some still in clinical trial phase. According to the bodies that make decisions as to which cancer treatment should be available, denosumab is suggested for secondary bone cancer treatment, while there is no solid evidence that suggests denosumab could be used for cancers that have been spread to the bones and have initiated from the prostate gland.
4. Fluids/Hydration
Drinking much fluid is suggested, as it helps flush out all extra calcium circulating in your bloodstream. Mainly, cancer-related hypercalceamia is treated with either intravenously either with normal saline or bisphosphonates, and the amount of fluid is specified by the patient’s cardiovascular status.

Get tested
As previously mentioned hypercalceamia is usually asymptomatic and is confused with other disease, which is why you should go to your doctor as soon as you experience any of the aforementioned symptoms. Your physician will run a full test on you that will definitely include a routine blood test to determine your blood calcium levels and your parathyroid hormone levels. If you have high blood calcium levels or suppressed parathyroid hormone levels your doctor might ask for a chest X-ray, MRI (Magnetic Resonance Imaging), CT (Computerized tomography) and/or Mammogram to determine whether you have cancer or other lung disease and malignancies.
Note
Cancer-related hypercalceamia is not affected by increasing or lowering the calcium in your diet.
TIps:
Make sure you get lots of fluids (up to 3-7 liters per day), exercise regularly, control vomiting and nausea and make sure you address to your doctor before you change your medication in any way.
May God be with You.
Sincerely,
Litsa Boudouri
Main Sources Used- Special Thanks to:
1. National Cancer Institute
2. Canadian Family Physician Journal, September 2013, 59(9)
3. Cancer Research UK organization
© 2013 litsabd