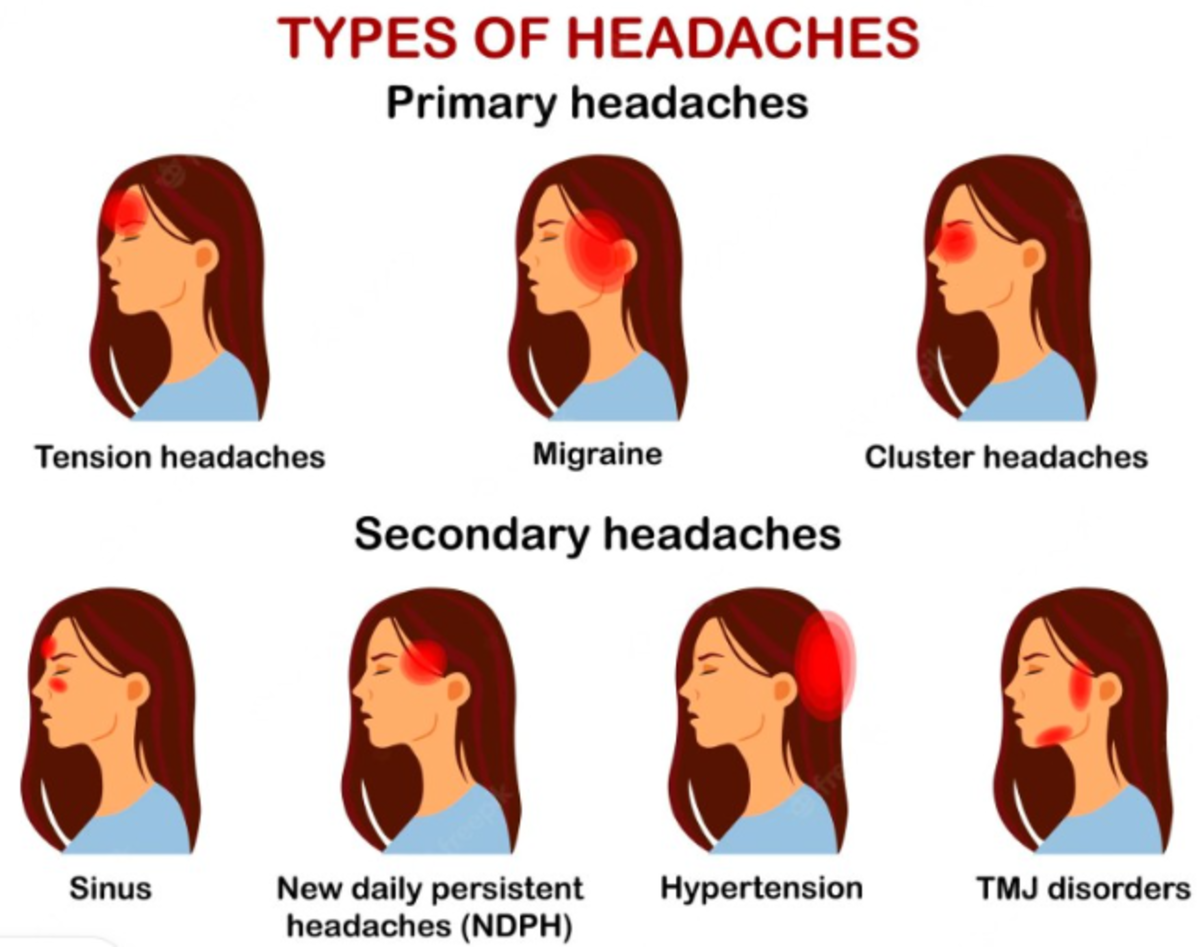
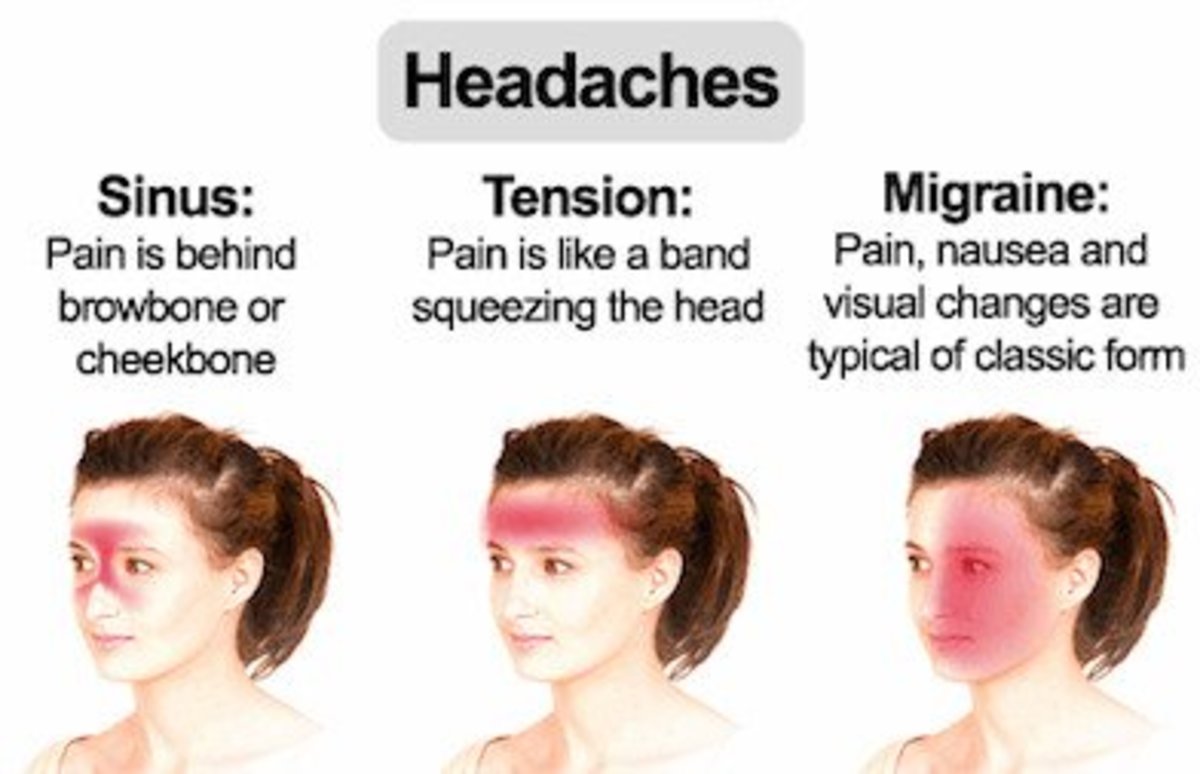
How to Identify and Treat a Migraine Headache

Migraine headaches are typically hereditary and may be identified using some very basic criteria.
For instance, if you have a headache that last for more than a few hours, experience throbbing pain in one side of your head that is intense enough to cause nausea or vomiting and experience sensitivity to light and sound, you probably have a migraine headache.
Migraines are a disorder that is caused by vascular and neurological changes inside the brain. The pain centers inside the brain become hypersensitive to various stimuli that cause pain. This hypersensitive state starts with a stimulation in the nerve cells that control inflammation of blood vessels in the brain. That's the cause of the intense throbbing sensation.
I have experienced migraine for more than 50 years and for me, there is nothing worse than migraine pain. They always begin with some sort of visual disturbance. I notice a blind spot in the center of my vision and what appears to be window blinds being opened and closed very quickly.
These lights appear in my peripheral vision, usually to the upper left. Visual distortions appear in about 15-20% of migraine sufferers.
Knowing the triggering mechanisms of a migraine headache can help you manage your behavior and avoid the onset of these sometimes debilitating headaches.
.

Managing Your Migraine Triggers
Of all the various different types of headaches - tension headache, stress headache, cluster headache, etc. - the migraine can be the most painful and debilitating.
As a sufferer of migraine headaches myself, I have learned a few things about how to know the difference between any other types of headaches and a migraine.
The main thing I have learned for me is what specific triggers start the process of a migraine that eventually end with the onset of an intense headache.
.
Migraine Trigger #1: Alcohol
Some migraine suffers have reported that they experience headache pain after just one or two drinks of alcohol. Most people that suffer this type of migraine trigger can isolate the type of alcohol that actually triggers the headache. For example, you may discover that vodka is the only type of alcohol that triggers your migraine.
This is easily managed by avoiding that specific type of alcoholic beverage.
.

Migraine Trigger #2: Blood Sugar Fluctuations
Some folks discover that missing a meal or eating too much of the wrong type of food can bring on the intense pain of a migraine headache. Missing meals can wreak havoc on your blood sugar levels.
Sometimes, this fluctuation in blood sugar may start with a small headache and cascade into a much larger headache - eventually leading to a migraine.
To avoid this trigger, don't go more than 3 hours without food and always include some high protein foods to help regulate healthy blood sugar levels.
.

Migraine Trigger #3: Sleep Deprivation
Recent research on rats has indicated that sleep deprivation may cause changes in proteins related to migraine headaches.
Getting the right amount of sleep and restful sleep is critical. If you're having problems with insomnia or if you are having problems falling asleep, you may want to take a look at this article, "Can't Sleep? 5 Ways You Can Learn How to Fall Asleep Fast" or "Insomnia: How to Fall Asleep."

Migraine Trigger #4: Caffeine Intake
discovered this one through my own experience with drinking large amounts of coffee when I had a stressful job in a big corporation many years ago. I was drinking about 10-12 cups a day and didn't realize how much effect it was having on me until I started developing migraine headaches just about every weekend.
The caffeine withdrawal was causing it's own headache which, in turn, stimulated those migraine areas in my brain. First the caffeine withdrawal headache would start and then escalate to a migraine soon after. This was easily managed by just limiting my caffeine intake to under 200-250 mg each day - about one 8 oz cup of coffee.
.
Other Migraine Triggers
There are any number of things that can cause the onset of a migraine headache. I discovered that physical stress over an extended period would almost always result in an excruciating migraine headache. One experience in particular comes to mind. I had been playing golf for about 6 hours one August day in Texas. Temperatures soared above 105°F and I was playing most of the day in direct sunlight.

Migraine Headache: The Medical Explanation
The stress on my body was soon apparent as I experienced the most debilitating migraine of my life. I experienced the visual blind spot and flashing light aura, my head began to throb in intense pain, nausea and vomiting soon set in. I made it to a hotel room and slept for about 12 hours. I have to tell you, I have learned from that day to carefully identify and avoid any of my specific migraine triggers.
Another thing I have learned about my own migraine headaches is to treat the pain as soon as symptoms occur. I discovered that if I allow the first minimal pain to remain untreated, this minor pain will increase gradually resulting in the full-blown pain typical of a migraine headache.
The specific migraine triggers in people are as varied as the number of people who experience them. Everything from chocolate. champagne, emotional stress, dropping estrogen levels - you name it. The key to managing a migraine headache is getting to know your own triggers.
If you are uncertain what type of headache you are experiencing, it's always best to seek the help of a doctor or medical professional to help determine what type of headache you are experiencing. If you already know suffer from migraines, you should start identifying specific behaviors, activities, foods, etc. that may trigger your migraine headache. Once you have done this, you will be able to manage the things that lead to your headache and avoid or control them.
________________________________________________________________
The information in this article is provided as an information resource only. This information should not used for treatment or diagnosis of any medical conditions. As a first step, always consult your physician or healthcare professional before making any decision or assessment regarding any possible medical condition.