Type 1 Diabetes: Innovative Treatment, the Bionic Pancreas Brings Hope for Many
Bionic pancreas out performs Insulin Pump

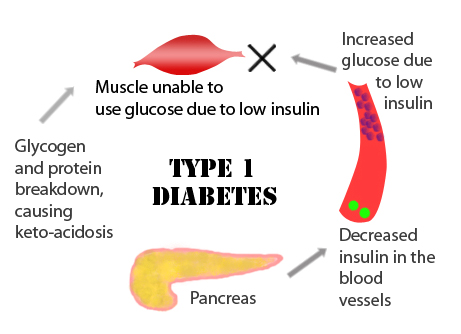
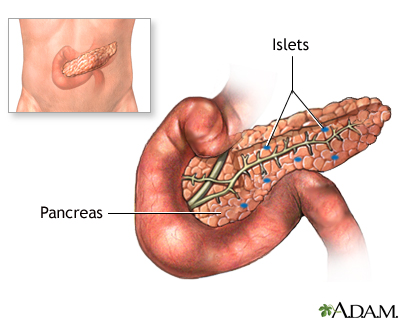
Hope for a cure for type 1 Diabetes

Insulin shot may soon be a thing of the pass
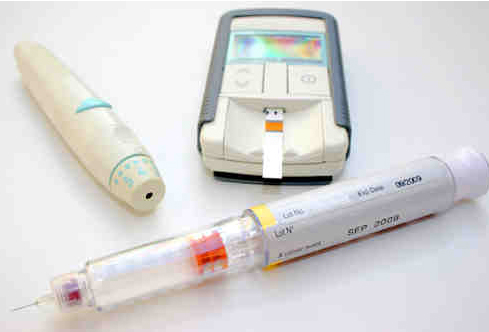
Diabetes
Diabetes is a serious condition that affects both children and adults; its prevalence continues to grow rapidly worldwide.
There are approximately 500,000 children aged under 15 with type 1 diabetes in the world (Patterson et al. 2014).
The need for new innovative treatment for diabetes is also growing, the artificial or ' bionic pancreas' that started its first human studies in 2008 could be the answer to many prayers.
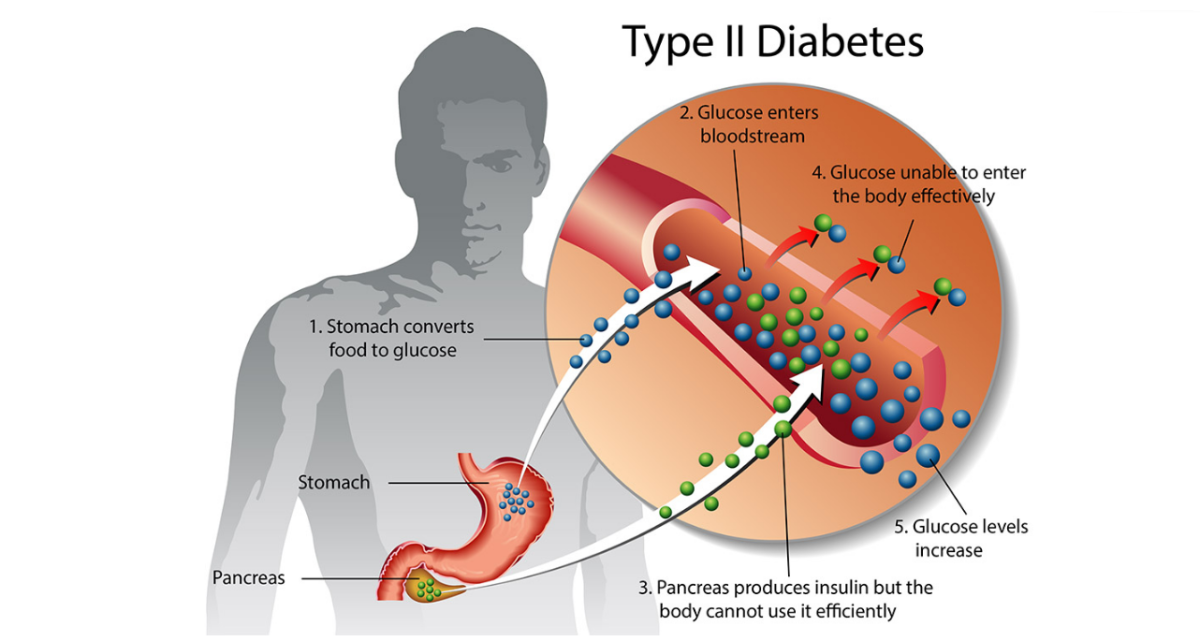
World Health Organisation (WHO) defines diabetes as a chronic condition that occurs either when the pancreas does not produce enough insulin or when the body cannot effectively use the insulin it produces.
Type 1 diabetes can develop at any age but typically occurs in childhood and young adults. Managing the condition can be a real challenge for both the children with diabetes and their parents, particularly when newly diagnosed.
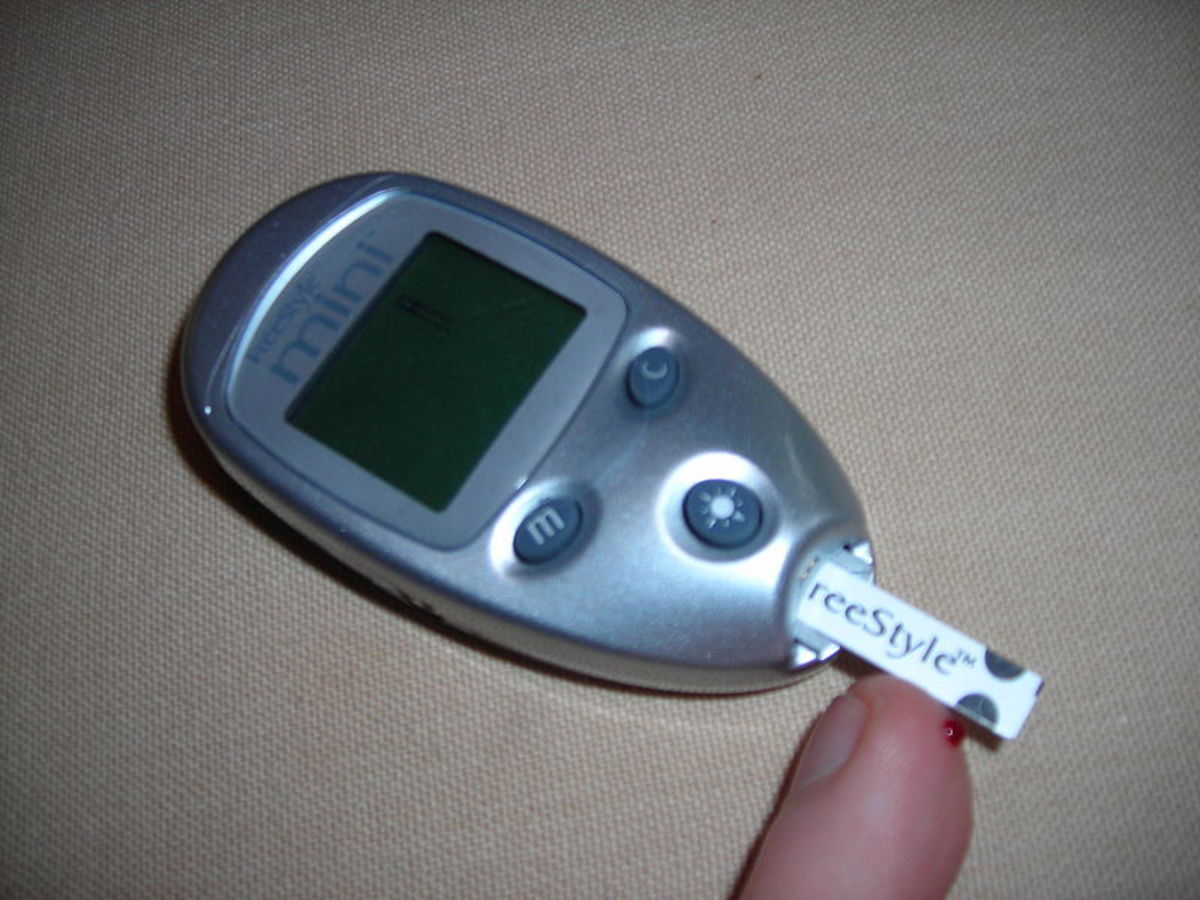
People with type 1 diabetes must very carefully balance their insulin doses either by injection several times per day, or by continuous infusion through an insulin pump. They must also measure their blood glucose (sugar) levels by pricking their fingers several times a day, be aware of what foods they eat, even then, they must still overcome the risk of life-threatening high or low glucose levels.
Cause of Diabetes Mellitus
The precise cause of type 2 diabetes is unknown, risk factors include, genetic inheritance, obesity and a sedentary lifestyle. In a healthy person, the blood glucose level is maintained within a normal range by several complex mechanisms involving the production of Insulin and glucagon by the pancreas.
Diabetes Mellitus often describe as a disease of paradoxes; while the disease typically affects older people, research shows that young and middle-aged individuals are most venerable.
The condition is prevalent in people who are overweight and obese, but emerging statistics suggests that for lean people with diabetes, the outcome can be worse. Uncontrolled, diabetes can lead to life-threatening complications. As the prevalence of diabetes increases, a tremendous burden is placed on health care providers for the future.
While there is no definitive cure for diabetes presently, the race is on for a more efficient way to manage the disease until a cure can be found, hopefully, in the not too distant future.
Complication of Diabetes Mellitus
Uncontrolled diabetes can lead to serious complications in both the short and long term. Short-term complications include:
Hypoglycaemia (low sugar)
Diabetic ketoacidosis (DKA), most common in people with type 1 diabetes, but can also be a complication of type 2 diabetes. DKA occurs where there is a severe lack of insulin and the body is unable to use glucose for energy. Instead, fat is broken down and utilized by the body as a source of fuel. This process results in the production of ketones, a toxic chemical that can build up in the body to cause acidosis, giving rise to the dangerous complication known as ketoacidosis.
Hyperosmolar hyperglycemic state (HHS) occurs predominantly in people with type 2 diabetes in which high blood glucose causes severe dehydration, increase in osmolarity with high risk of complications, coma and death
Long-term complications include damage to small blood vessels by high levels of glucose that can also result in 'furring up' of the arteries (atherosclerosis). When the condition is poorly controlled, many of the organs of the body can be affected such as:
Eyes (diabetic retinopathy) leading to blindness, however, with regular check-ups, most people with diabetes have only minor eye problems.
Cardiovascular diseases (CVD), people with diabetes have a higher risk of developing CVD.
Kidney failure is much more common in people with diabetes
Stroke, diabetes significantly increases the risk of stroke
Neuropathy (Nerve Damage), People with diabetes, are much more likely to be admitted to hospital with foot ulcer than people without diabetes. This is due to poor circulation and reduced feeling in the feet as a result of nerve damage.
People with diabetes often require amputation of toes, feet or legs. According to the American Diabetes Association, more than 60% of non-traumatic lower-limb amputations occur in people with diabetes.
Managing Diabetes
In some cases, type 2 diabetes can be controlled by eating a healthy well-balanced diet and by regular exercises. Some people with type 2 diabetes may need oral medication in conjunction with diet and exercise, preferably a diet that is recommended by a registered dietitian, some people with type 2 diabetes may also require injection of insulin.
Unlike type 2 diabetes, type 1 cannot be controlled or managed by lifestyle changes. A person with type 1 diabetes needs a healthy balance diet, but also frequent injections of insulin. The adjustment to a life that revolves around eating the right foods, testing blood glucose levels and administering insulin can be hard to make and maintained. A father whose child developed type 1 diabetes at 11 months old made it his quest to find a better way to manage the disease. Edward Damiano set a goal to have his invention ready by 2017, the year that his son is due to start college.
The new innovative systems that mimics the function of the Pancreas known as the “bionic pancreas” may well be the answer to many prayers.
The device has out-performed the most traditional means of managing the disease by monitoring glucose levels and manually calculating the dose before administering the required amount of insulin by injection or via an insulin pump.
Cause of Type 1 Diabetes
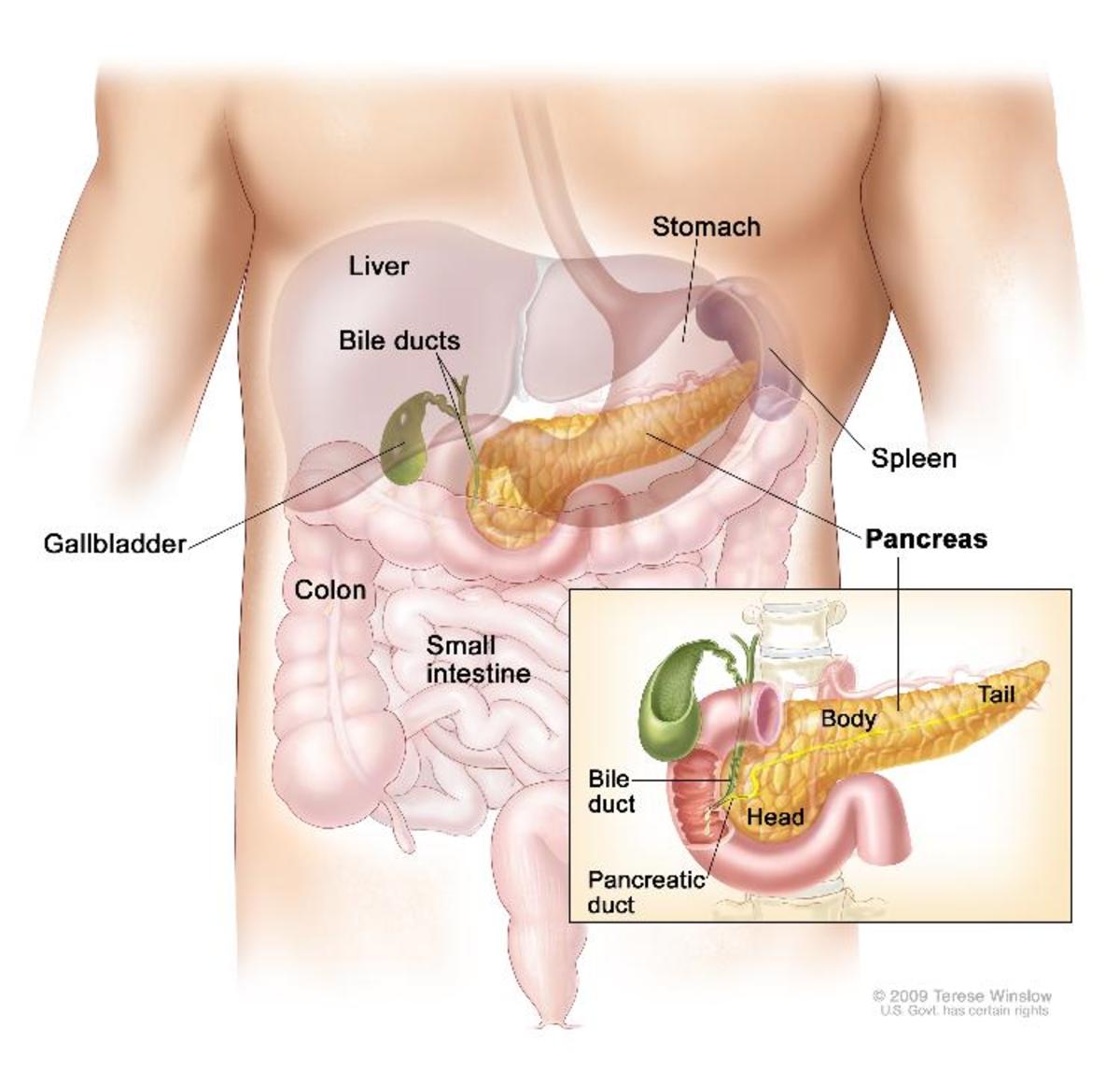
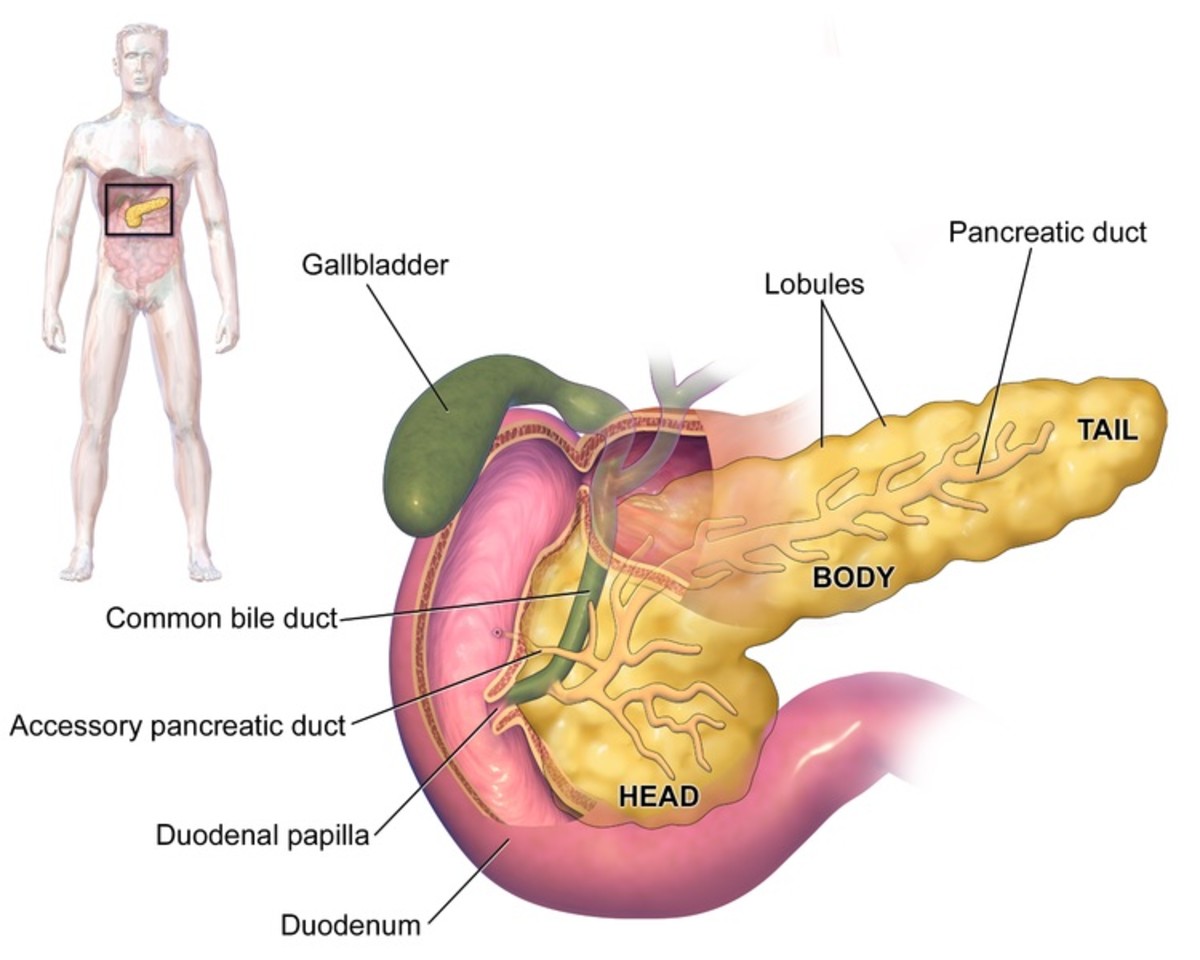
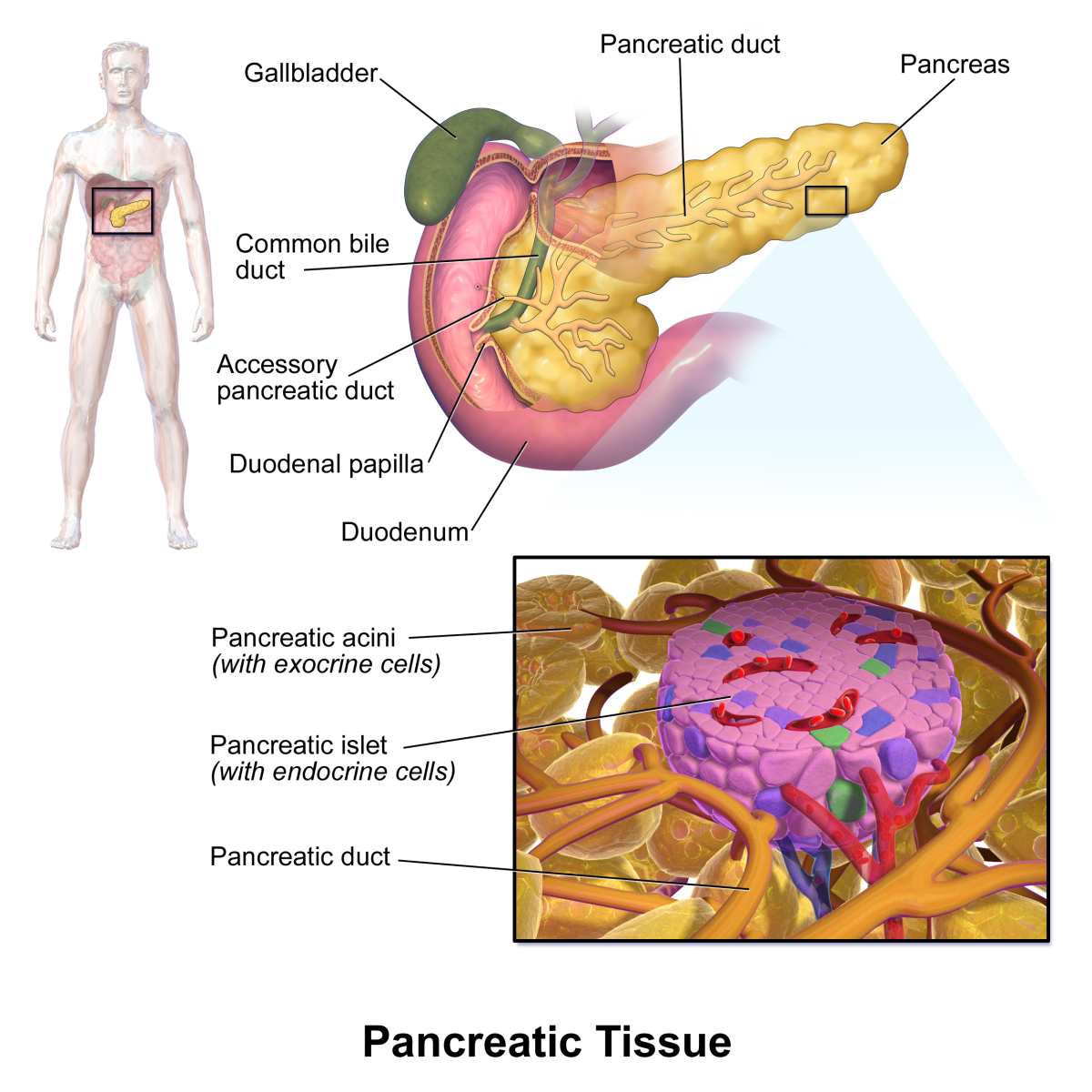
Insulin is a hormone that is produced by specialized cells in the pancreas. Type 1 diabetes, once known as early-onset, juvenile or insulin-dependent diabetes, develops when the pancreas produces insufficient or no insulin.
The exact cause of type 1 diabetes is unknown, risk factors include genetics, in most cases the condition is thought to be an autoimmune disease. This is where the immune system that usually protects the body from foreign invaders such as bacteria and viruses produces antibodies that mistakenly attack and destroy the special beta insulin-producing cells of the pancreas (islets of Langerhans).
The incidence of type 1 diabetes has increased on average, 3% per year between 1960 to 1996 in children under 15 years of age. In the US recent data show that the prevalence of type 1 diabetes increased by 21% in children, between 2001 and 2009 (Dabelea et al. 2014).
Environmental factors may have played a part in the rise of type 1 diabetes in recent times; there appears to be a correlation between the increase of industrial and agricultural chemical production and the rise in type 1 diabetes.
Some studies have suggested that diet may play a role in developing type 1 diabetes. The theory is that Infants who are breastfed and those receiving vitamin D supplements may have a reduced risk of developing type 1 diabetes, while infants with early exposure to cereal proteins and cow's milk, may have an increased risk of developing the disease. More studies into the link between infant nutrition and type 1 diabetes are needed.
One in three adults in England shows evidence of pre-diabetes.The World Health Organisation (WHO) predicts that diabetes will be the 7th leading cause of death by 2030.
Diabetes is predicted to hit 6.25 million people in the UK by 2035, with the increase comes a price tag for the National Health Service (NHS) of £1 million per hour.
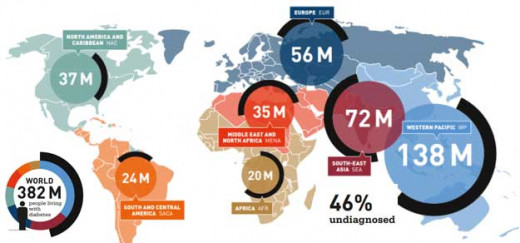
The number of people worldwide with the condition is said to be around 347 million, an estimated 3.4 million people died from the consequences of high fasting blood sugar in 2004, says the WHO.
While a cure for diabetes remains an elusive dream, scientists are trying to find out what triggers the disease, each tentative step hopefully taking us closer to better management of the condition and a possible cure. Innovative treatment like the bionic pancreas and the development of vaccine promises to make managing the condition much easier and safer. New advances in embryonic stem cells may be able to affect dramatically how the condition is treated in the future.
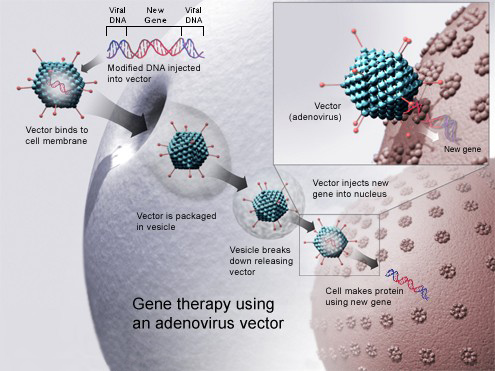
Scientists are using a new technique similar to that used in the cloning of animals to make insulin-producing cells. DNA from a woman's skin cells was placed into donated human eggs. The eggs were then grown in early embryos from which stem cells with the potential to develop into any cell type in the body are grown into insulin-producing cells.
Earlier this year, stem cells were created from a single drop of finger-pricked blood to generate human induced pluripotent stem cells, these are cells that can give rise to all the cell types that make up the body. By genetic reprogramming, matured cells like blood cells can be transformed into properties that are very similar to human embryonic stem cells. The race for a cure is well and truly on, not only for diabetes but many other chronic diseases.
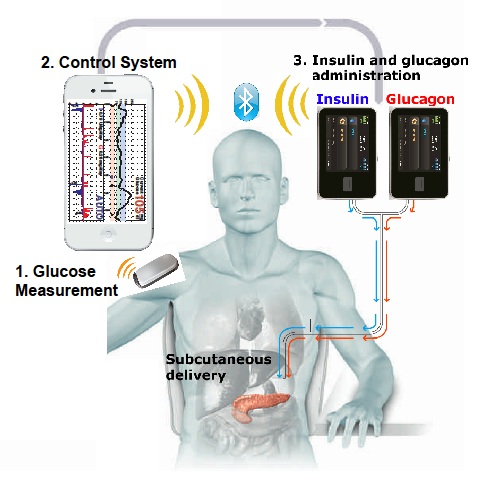
Bionic Pancreas Developed by Ed Damiano Associate Professor, Biomedical Engineering at Boston University and Colleagues

Facts About Diabetes from the American Diabetes Association
- In 2010, 79 million Americans aged 20 and older had pre-diabetes. The statistic for 2012 was 86 million
- Around 1.9 million Americans are diagnosed with diabetes every year
- An estimated 7.0 million American have undiagnosed diabetes.
- 25.6 million 20 years or older or 11.3% of the people in this age group have diabetes
- The death rate of adults with diabetes from heart disease is about 2 to 4 times higher than adults without diabetes.
- Diabetes is the leading cause of new cases of blindness among adults aged between 20- 74 years.
- Diabetes accounts for 44% of all new cases of kidney failure
- Hearing loss is twice as common in adults with diabetes as in those without the condition
- Around 60% to 70% of people with diabetes have mild to severe forms of neuropathy
- Number of Non-traumatic lower limb amputations performed in people with diabetes annually is about 65,700 or 180 per day
- 85.2% of people with type 2 diabetes are obese or overweight
- If present trends continue, 1 in 3 American adults will have diabetes in 2030
- Diabetes kills more Americans each year than AIDS and breast cancer combined
- An individual diagnosed with diabetes at the age of 50 dies six years earlier than someone of the same age without diabetes
- The total costs of diagnosed diabetes in the US in 2012, $245 billion
Treatment for Diabetes, the Bionic Pancreas
Researchers have been attempting to create a device that mimics the function of the pancreas for quite some time, the search for a device that can seamlessly control and stabilize blood glucose levels in people with type 1 diabetes may not be far off.
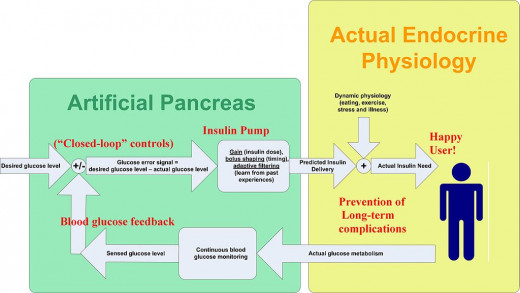
Recent results from two trials funded by the National Institute of Health (NIH), and published in the New England Journal of Medicine, indicated that a prototype for a bionic pancreas developed by a Boston University/Massachusetts General Hospital research team may be on the right track. The intelligent device consists of a smartphone hardwired to a continuous glucose monitor and two small pumps that deliver doses of insulin or glucagon, (an antidote for insulin) every five minutes.
The prototype is controlled by the smartphone through an app built by Edward R Damiano Ph.D. and his team. The wearable bi-hormonal, bionic pancreas improved mean glycemic levels with less frequent hypoglycemic (low glucose levels) episodes, among both adults and adolescents with type 1 diabetes Mellitus
The device was better able to keep blood glucose levels consistent, than patients who managed they own glucose levels. Researchers found that the patients in the study needed 37% fewer intervention for hypoglycemia. In both adult and teen study, participants demonstrated overall improvements in glucose levels using the device, particularly during sleep, a challenging time for someone with diabetes to maintain stable blood glucose levels.
Dr. Edward Damiano, a biomedical engineer whose 11-month-old son was diagnosed with type 1 diabetes in 2000, decided to create a device that would allow his son and millions of others to manage better their condition.
The first-generation device produced by the team of scientist from Boston University was clinically tested in 2009, the second phase in 2010. A series of longer trials got the go ahead starting this month, and will hopefully see the device approved by the US Food and Drug Administration to be ready by 2017 when Damiano's son begins college.
Pre-diabetes
British scientists are confidence that insulin deficiency disease would be wiped out in the next 25 years; I very much hope the prediction will prove to be correct. As the number of adults with diabetes continues to rise, it is estimated that 5 to 10% of adults with pre-diabetes will progress to “full blown” type 2 diabetes in any given years.
Pre-diabetes, also known as borderline diabetes is a condition where blood glucose levels are abnormally high, but less than the threshold for the diagnosis of diabetes. Most people with pre-diabetes will go on to develop type 2 diabetes.
There is an estimated 79 million American with pre-diabetes. The good news is that pre-diabetes can be reversed in many cases. However; it requires some serious lifestyle changes.
Results from research from a large-scale study known as Diabetes Prevention Program shows that for every year after the initial diagnosis of pre-diabetes, there is an 11 % chance of developing type 2 diabetes, with a greater risk of also developing stroke or heart attack when compared to people with normal glucose levels.
Information gathered from the Health Survey for England (HSE) found that there was a significant increase in the proportion of people aged 16 or older with pre-diabetes between 2003 and 2011, an increase from 11.6% in 2003 to 35.3% in 2013.
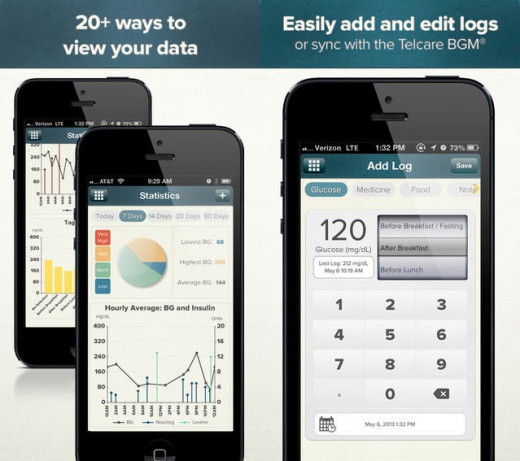
Mobile Apps Help Manage Diabetes
A Sensible Diabetic Diet, Foods with a low Glycaemic Index (GI)

Natural foods to improve health in type 2 diabetes
Diet to provide
| Source
| Action
|
|---|---|---|
Soluble Fibre
| apples, apricots, beets, citrus fruits, berries, carrots, squash and oats
| Help the body to absorb sugar slowly, Soluble fibre help to keep blood sugar levels stable
|
Low Cholesterol
| garlic, onion, vegetables and moderate amounts of sweet fruits
| Help to lower LDL cholesterol (bad cholesterol) and raise HDL (good cholesterol)
|
Antioxidant
| Vitamin C, flavonoids, carotenes
| Help prevent fat from oxidizing to cause damage to the artery walls which can lead to plaque formation and heart disease.
|
Low Sugar
| Basil leaves, ginseng, cactus nopalitos or prickle juice, leaves of bilberry plant, leaves of the fig tree
| Help to reduce glucose levels
|
improved circulation
| Ginkgo
| improve brain function and circulation
|
Be always mindful of using natural medication that lower blood glucose levels, especially when taking insulin or oral medication, contact a herbalist and always consult with your doctor first.
Most people with diabetes are only diagnosed when hospitalized for other conditions
Have you been tested for Diabetes?
Gene Therapy

Most Current Statistics About Diabetes in America

Diabetes Worldwide