My Da Vinci Hysterectomy Experience
Ovarian Cyst
Like many women who either opt for, or are encouraged by medical professionals to have, surgical removal of part, or all, of their internal reproductive organs to relieve a variety of symptoms and issues, I had a history leading up to that point. As a teenager my menstrual cycles were nothing odd. They were not painful or extremely long or even very heavy. They just were. I say this because I have known many women whose personal problems with their reproductive system started the moment they began menstruating. But this just wasn't the case for me.
In fact, there were no real problems with that facet of my life until after giving birth to three children. By this time I was around 25 years old when the odd began happening. My first symptoms began with severe bloating and the absence of a period for two months. My gut had bloated so severely I could no longer button my pants. Several pregnancy tests came back negative, and so I just ignored it thinking maybe I was just overly stressed, or eating too much junk food. I ignored it until I woke up in extreme pain one night and ended up in the emergency room. There I was told I was pregnant, had a urinary tract infection, and had a very large ovarian cyst on the left ovary that would have to be removed surgically right away due to risk of bursting. I was told they might be able to do the surgery without losing the baby. Within a couple of days I was admitted for surgery.
The surgery to remove the cyst was supposed to be done via laparoscopic incisions, meaning only small cuts on the abdomen were to be made so that tools could be inserted to cut and remove the offending cyst. The benefits of a laparoscopic surgery are reduced chance of infection, less bleeding, speedier recovery time, and overall better outcome. Unfortunately, once inside to actually see the cyst that had only been observed via ultrasound, it became apparent that it could not be removed through a one inch incision. The cyst was quite large and was filled with approximately one liter of fluid. When I awoke after the surgery I was quite surprised to find an incision running across the top of my pubic bone being held shut by staples. My recovery time jumped from just a couple of weeks to almost two months. I miscarried the baby about a week later, at around 12 weeks gestation.
The Author, age 38

Hysterectomy Facts
The following facts are found online at womenshealth.gov, a service of the U.S. Department of Health and Human Services Hysterectomy Fact Sheet, last updated December 15, 2009.
- Hysterectomy is the second most occurring surgery performed in women in the United States, topped only by Cesarean section
- Reasons for hysterectomy include a variety of problems, including but not limited to, endometriosis, prolapsed uterus, chronic pain, fibroids, cancer, and abnormal chronic bleeding
- Recovery time for abdominal hysterectomy is typically 4 to 6 weeks and vaginal or laproscopic is typically 3 to 4 weeks. Da Vinci robotic hysterectomy recovery time is not listed, but has been listed as a 6 day recovery on other sources.
How do you feel about a robot assisted surgery?
Would you opt for a robotic surgery?
My belly incision
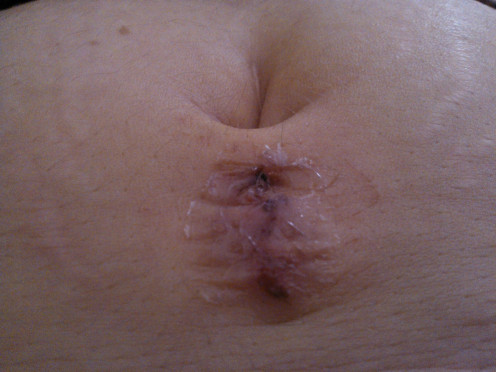
Endometriosis
After the surgical removal of one very large ovarian cyst and subsequent miscarriage it was a few years before more symptoms were noticed. In fact, the fourth and final baby was born before more symptoms were noticed. But once they started, they never stopped.
The problems began with heavier menstrual cycles and the passage of large clots of blood. Cycles would begin with intense pain and the passage of dark blood indicating it was actually old blood that had not passed previously when it was supposed to. Then came pain with intercourse. Then pain with walking, or simply standing upright for too long. There was constantly pain on the left side, the same side where the large cyst had been found years earlier. A visit to an OB/GYN resulted in a preliminary diagnosis of endometriosis. It cannot truly be diagnosed without surgery to confirm.
Treatment for endometriosis might include using birth control pills or hormones to manage the amount of menstrual cycles a woman experiences and reduce the further development of endometriosis. It can be removed during surgery by cutting or burning any identified tissue. My doctor suggested laproscopic surgery to do just that after trying a variety of pills and shots to control it. Via some very small incisions in my abdomen he was able to confirm the diagnosis of endometriosis and remove some of it, but not all. I was virtually pain free for a while. It was great. But it didn't last.
All my normal symptoms returned, plus new ones. It hurt to urinate, it hurt to walk for too long or stand for too long. Sex hurt with certain positions or depths, or for no apparent reason at all. Premenstrual pain became so severe that I got used to giving up a whole day because I knew I would be curled up in bed. I worried that my pain would hit me at work and I wouldn't be able to work around it. I was in a lot of pain, but I just figured I would have to put up with it because I had endometriosis and the laparascopic hadn't taken care of it before. I was resigned to the pain.
Another cyst...
Flash forward several years and a long time of grinning and bearing the pain of endometriosis. During an ultrasound performed for something not related to endometriosis, doctors found another ovarian cyst. I was referred to talk with a surgical gynecologist for recommendations. I was given a long list of possible treatments to include all of the ones I'd already tried in the past to control endometriosis. Hormone shots, birth control pills, laparascopic surgery to remove the cyst as well as newly formed endometriosis, or do nothing. But this time a new suggestion was made. Because I was happily married for an extended period of time, had all the children I was going to have, and was continuing to experience a variety of issues, the doctor suggested hysterectomy. I was shocked! I thought hysterectomy was for old ladies, not for me. I listened to his suggestion and his reasoning, and agreed to see a specialist doing Da Vinci Robot assisted hysterectomies.
I met with the surgeon who said I was the perfect patient for such a surgery. I considered the idea of not ever having another menstrual cycle, or endometriosis pain, or ovarian cyst. It sounded wonderful. The fact is that endometriosis may return, even after hysterectomy, and that it feeds off of estrogen, which I need, but the odds are greatly reduced that I'll have anymore issues with it after the hysterectomy.
Sign me up!
Robotic Surgery Demonstration
Surgery day
Just a few weeks after the consult with my surgeon it was time. My husband and I arrived at the hospital at 5:15am for a 7am surgery start time. My surgeon did not have me do a bowel prep the day prior, but some do. I was grateful mine did not as enemas and laxatives are no fun.
Upon arrival I had three wristbands placed on me after confirming my identity. We were taken to the back and shown to my room. I changed into a paper gown and put all my clothes in a bag which was placed under my bed. There were a lot of questions and people coming by to talk to me. Since I had a history of getting nauseated I was given lots of anti-nausea medication to include a patch behind the ear. When it was time to go into the surgical suite, the anesthesiologist injected something into my IV that made me relaxed and a little dizzy. I was wheeled into the room where the robot was. It was quite impressive. The last thing I remember was asking if that was the robot and the staff telling me I would have to move over to another bed.
When I woke up I was back in the recovery room. I had expected to be in a lot of pain, but honestly, I just felt tired. They had placed a catheter during surgery and told me I would have to leave it in place when I went home and then remove it the next morning. My four incisions were very small, maybe an inch at most, and were covered by a type of surgical super glue. I was asked if I wanted to go home that day, or the next day. I wanted to get home as soon as possible so I could rest on my own couch with my own tv and my own family. I was able to stand up, get dressed, and leave the hospital.
On the way home I nodded in and out, but I was aware of the drive. We stopped at the pharmacy on the way home and picked up my prescriptions for pain and nausea medications. Once at home I took up residence on the couch and took a nap. Following my doctor's orders, I made sure to get up and walk around periodically as it would help with recovery. By the next day I was up and walking around. I went to the store and walked slowly, then went home and rested some more. I spent the first two nights sleeping on the couch because it was more comfortable sleeping in an upright position. After the first couple of days, it seems as if nothing has happened and I can't wait to go back to work. It's only been 4 days.
Update 4 Weeks Post-Op
4 weeks after the surgery I have to remind myself that I actually had surgery! It's truly amazing! I returned to work after 2 weeks at home, have returned to low impact exercise, and have no pain at all. I begin to question if the surgeon really removed my uterus, ovaries, cervix, and fallopian tubes, but then I remember that I do have an estrogen patch on my belly and 4 very small incision scars.
Since the surgery not only have I not had the previous pain from endometriosis, but my rheumatoid arthritis has also seemed to improve. I don't know if there is a link between the two, although both are considered inflammatory diseases. Personally, I believe there is a link between the estrogen and inflammation in my case, but I'm not a doctor. Before my surgery, there was a noticeable spike in arthritis pain corresponding to menstrual cycles. Now that I have no menstrual cycle, I have noticed a spike in arthritis pain. Perhaps it's just a coincidence, perhaps not.
I have been to the doctor for 2 follow-up appointments since the surgery. The first was at 1 week post-op where I was informed that I also had something called adenomyosis. This involves infiltration of endometrial tissue into the uterus where it doesn't belong. It is often undiagnosed in women until some kind of surgical procedure, or removal and dissection of the uterus. Adenomyosis causes heavy or prolonged menstrual bleeding, pain during intercourse, and painful periods which get worse with time. No one ever mentioned to me that I might have this despite years of issues, but it makes a lot of sense in hindsight.
The second post-op appointment was at 3 weeks. During this visit the doctor performed an internal exam to make sure the stitches at the top of my vagina were healing. There was no pain during this exam and the doctor said I was healing perfectly and could resume sex after 6 weeks of healing. That means I've got another 2 weeks to go before sexual intercourse as of this update.
While I understand some are against hysterectomy and see it as an over performed, unnecessary surgery, it has already improved my life and I highly recommend the Da Vinci procedure for anyone who has tried everything else to reduce their pain and suffering. Everyone heals differently and mine may be an unusual experience, although I have talked with other women who report the same positive healing process.