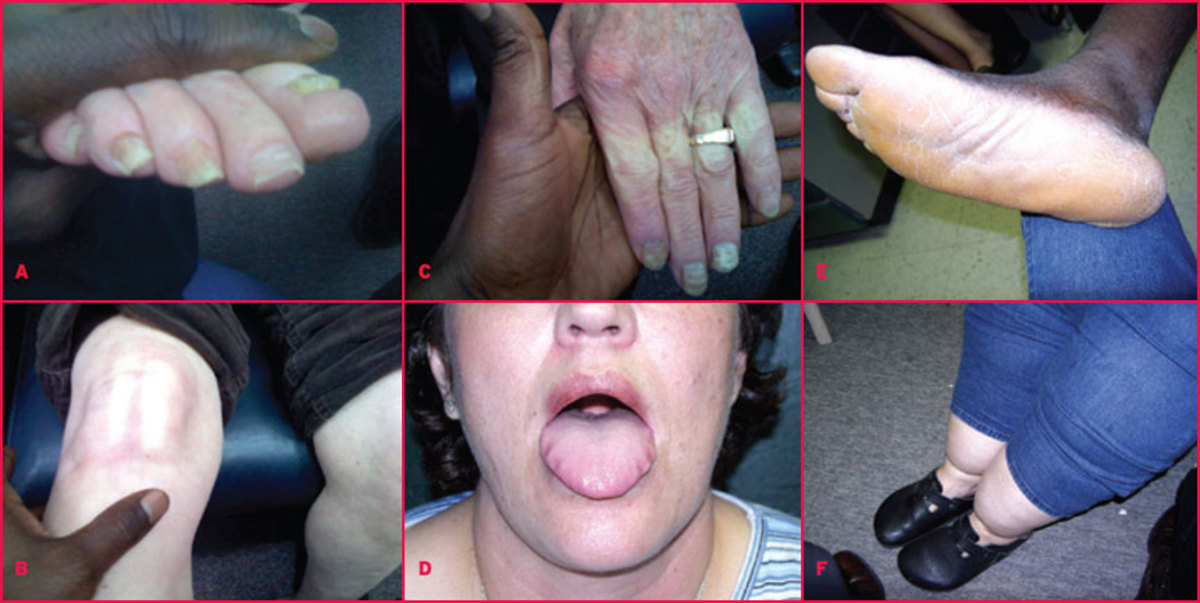
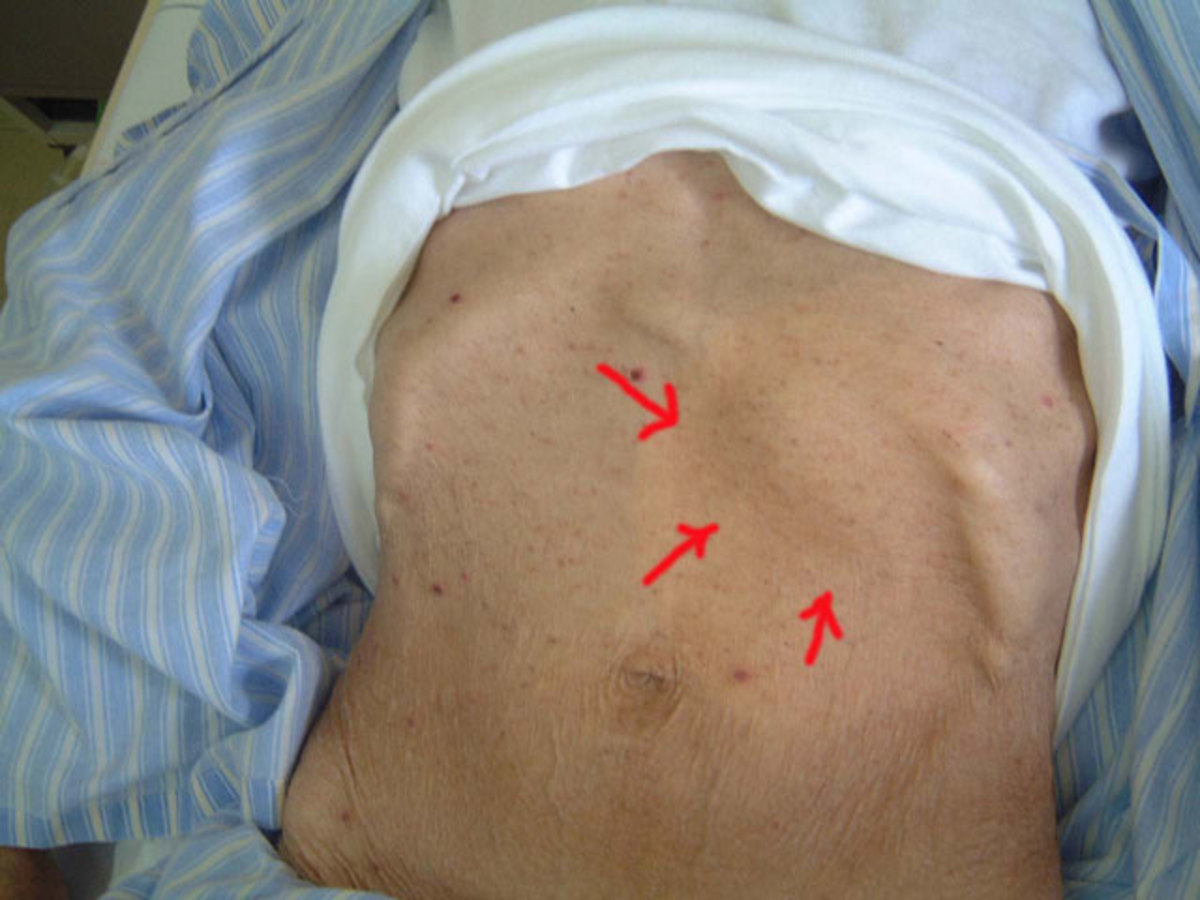
Mycetoma: Pathology, Clinical Manifestations, Treatment And Surgery
Mycetoma Madura Foot
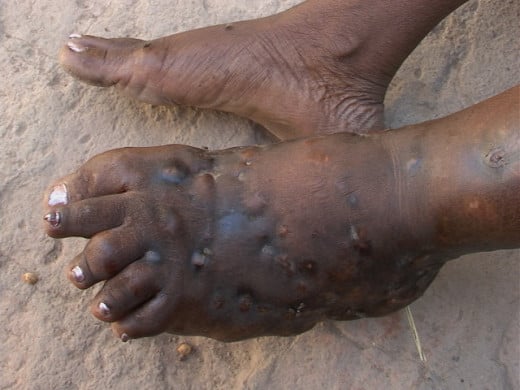
Madura Foot, Maduramucosis
This is a chronic granulomatous inflammation caused by several specieis of fungi or actinomycetes. The lesion starts in the subcutaneous tissues and later on involves deeper structures, including the bones, to form sinuses leading to the eventual destruction of the part. This condition was described in Madurai in 1842 by Gill. This disease is confined to the tropics and is particularly endemic in India, Africa and South America. Most of the cases in India for instance have been reported from the southern regions more. Nocardia are normally present in soil and infection may be exogenous. The organism causing Madura foot is Nocardia madurae. Nocardia resemble Actinomyces morphologically, but are aerobic. In addition to Nocardia, Actinomyces and many fungi can also give rise to mycetomas.
Pathogenesis and pathology: The organisms enter through abrasions on the skin. The lesions are manifest after a long incubation period. A granuloma develops. The organisms are seen to lie in abscesses, surrounded by a zone of chronic inflammatory cells. The organism can be easily identified on microscopic examination. The inflammation spreads along facial planes by contiguity. Nerves and tendons are highly resistant to invasion. Regional lymph nodes are not generally affected.
Lesions In Mycetoma
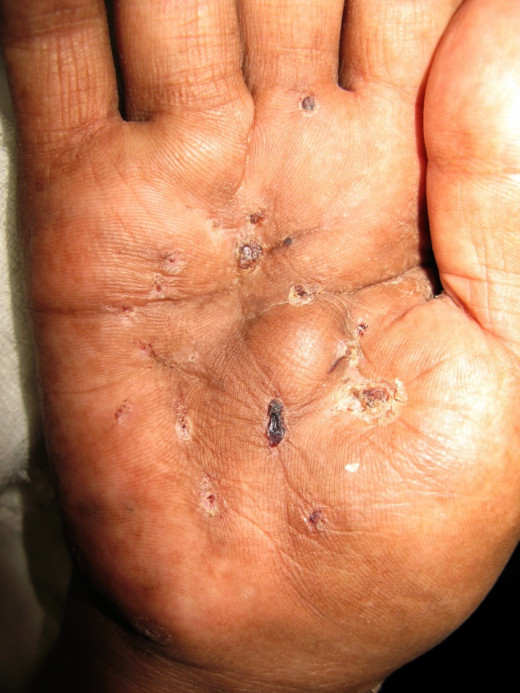
Infectious Diseases
Clinical Manifestations Of Mycetoma
A small painless firm subcutaneous tumour develops in both the nocardial and actinomycotic types. The lesions slowly progress to destroy the part. Sinuses develop which discharge pus containing the organisms. The progress of an actinomycotic granuloma is more rapid than that of a nocardial lesion.
The most common site is the dorsum of the foot, but other regions like the hands, buttocks, back, scalp and orbits may be affected. Systemic symptoms do not occur.
Radiological features: Bone destruction and endosteal or periosteal new bone formation may be demonstrable in localized areas or more diffusely. Progressive painless destructive lesions of the extremities occurring in endemic areas should raise the possibility of mycetoma. The differential diagnosis includes chronic osteomyelitis, tuberculosis, syphilis, elephantiasis and neoplasma. Histology of the lesion and isolation of the organism from the lesion help to establish the diagnosis. Antibodies to the organism can be demonstrated by agar-gel precipitation tests.
Treatment: Drug treatment is effective for actinomycotic lesions, but not so readily for nocardial lesions. Actinomycetomas respond well to prolonged treatment (6 to 12 months) with dapsone (200 mg/day), sulfisoxazole, streptomycin, sulphamethoxypyridazine, cotrimaxazole or nalidixic acid.
Surgery: In addition to drug therapy, surgery may be needed to excise early lesions or to amputate grossly damaged limbs. The lesion may recur after surgery. Mycetomas can be prevented by hygienic habits and regular use of footwear.
© 2014 Funom Theophilus Makama