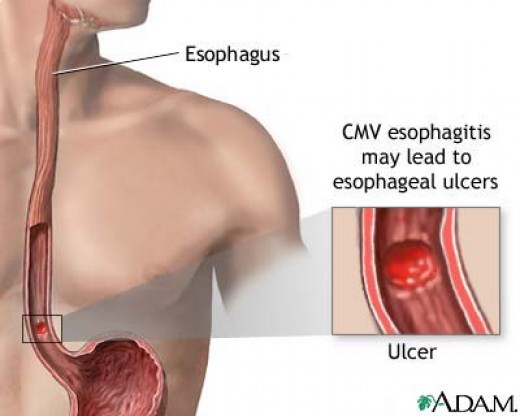
Oesophagitis: The Story Of Gujarati Konkani From Mumbai, India
Clinical Manifestations Of Esophagitis

Viral Oesophagitis
Gujarati Konkani's story
Gujarati Konkani is 38 years old from Eastern India. He has been a Diabetic patient for 4 years now and very obese with a BMI of about 33. Even with his condition, he still smokes and as well loves the traditional Indian recipe: Charpati with spicy sauce which most a times consist of lots of Garlic and Onions.
After a wedding where he ate lots of spicy recipes, he came back home with sharp pain behind his breastbone, which was gone after some hours. The following day, the sharp pain returned immediately after lunch. In the same day, he started experiencing painful swallowing during dinner with the feeling of stucked swallowed food in the Oesophagus. He refused to see a doctor not until the following day when the symptoms intensified and were accompanied with heartburn with reflexive grasp. In the Hospital, Barium X-ray was done and Endoscopy, together with additional laboratory results; leading to the Doctor's diagnosis: Infectious Oesophagitis.What the heck is this? Would Gujarati die?
Patho-morphologic Classifications of Oesophagitis
Oesophagitis could result to a thick exudate. An exudate is any fluid which filters from the circulatory system into lesions or areas of inflammation. These exudate could be of immuno-protective cells (white blood cells) and mucus due to swelling of the mucous membrane as a response to infection. This classification is called Cattarhal Oesophagitis.
It could also result to a bacterial infection-related acute purulent inflammation, leading to the spread of diffuse inflammatory processes with the formation of purulent/suppurative pus or exudate (a typically yellow-brown or white yellow thick fluid formed at the site of an inflammation during infection). This classification is calledPhlegmonous Oesophagitis. Hence Oesophagitis could be Catarrhal or Phlegmonous.
Complications
If Oesophagitis is left untreated or symptoms persist for a very long time; such complications can occur:
- Barrett;s Oesophagus: A situation in which a metaplastic process occur, changing the cells of the membrane lining of the Oesophagus from white flat cells (stratified Squamous) to pink, Square ones (Columnar cells).
- Oesophageal stricture: This is the narrowing of the Oesophageal lumen (opening).
- Oesophageal rings: Abnormal tissues can form rings around the lining of the Oesophagus.
What is Oesophagitis?
Oesophagitis is an inflammatory process which affects the Oesophagus due to either infection or irritation. Such infection could be fungal, bacteria, viral or immunosuppressing conditions.
Causes
- Viral infections such as cytomegalovirus, Herpes Simplex (Herpes Oesophagitis).
- Fungal infections such as Candida (Oesophageal candidiasis).
- Irritation of the Oesophageal mucosa due to Surgery, Hernias, intake of large medical pills (doxycycline, tetracycline, Vitamin C, alendionate, ibandionate, risedronate) with not enough water immediately before bedtime, toxic substance intake such as acidic or alkaline solutions, vomiting, radiation injury during radiation therapy for cancer treatment and GERD (Gastroesophageal reflux disease).
Pathophysiology
The sequence of disease occurrence is what we call patho-physiology. The sequence of Oesophagitis occurrence depends on its etiology.
- In reflux Oesophagitis, gastric acidic contents from the stomach regurgitate back into the Oesophagus. The persistence of this situation results to damage of the Oesophageal mucosa lining. Contents such as pepsin, gastric acid and bile irritate the squamous epithelium, leading to inflammation, erosion and ulceration of the mucosa membrane of the Oesophagus.
- In infectious Oesophagitis, the affected individual usually is an immuno-compromised patient. In such a situation, opportunistic infections break the protective barrier of his body mechanism. Pathologies which can lead to an immuno-compromised state are: alteration in humoral immunity, impaired chemotaxis, impaired T-cell lymphocyte function and phagocytosis.
- All these and patients with systemic diseases (alcoholism, Diabetes mellitus, adrenal dysfunction) can lead to an immuno-compromised state, hence infection, and finally, infectious Oesophagitis which can as well cause inflammation, erosion and ulceration. Which in Gujarati's case can be classified in this category with his history of Diabetes Mellitus.
Note that: Radiation over 30 Gy through the mediastinum can cause restrosternal pain, Odynophagia etc.
- 40 Gy can cause redness and edema of mucous
- 50 Gy can cause more severe Oesophageal damage
- 60-70 Gy can cause Oesophagitis with strictures, perforations and fistulas.
From the three points above, we can deduce the fact that, despite the different pathways of the disease, they all end up at the same point: inflammation, erosion and ulceration. Therefore, regardless of the etiology (as there are others such as medication induced Oesophagitis, Eosinophilic Oesophagitis or radiation and chemoradiation Oesophagitis), inflammation, erosion and ulceration are the end point/results and based on the Los Angeles classification of Oesophagitis, these erosions/ulcerations/lesion are used to Grade its severity.
Severity Grading Of Oesophagitis
Grade
| Characteristics
| Staging
|
|---|---|---|
Grade A
| 1 or more lesions in the mucosa, < 5mm in maximal length
| 1
|
Grade B
| 1 or more lesions in the mucosa, >5 mm, which is not continuous along the mucosa folds.
| 2
|
Grade C
| Mucosa ulcerations which are continuous between >2 mucosal folds but with involvement of <75% Oesophageal circumference.
| 3
|
Grade D
| Mucosa ulcerations involving more than 75% of Oesophageal circumference
| 4
|
The Los Angeles Classification of Oesophagitis
Immuno-compromised Oesophagitis
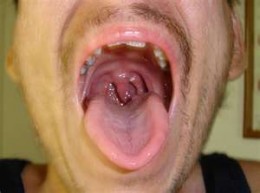
What can we observe in Oesophagitis?
- Dysphagia: Difficulty in swallowing
- Odynophagia: Painful swallowing
- Retrosternal pain: Chest pain behind the breastbone which usually do occur with eating.
- Food impaction: stucked swallowed food in the Oesophagus.
- Decreased appetitie
- Cough
- Abdominal pain
- Heartburn
- Difficulty in feeding
- Sometimes, mouth sores
- Failure to thrive (grasping for themselves or reflexive grasp).
Risk factors: There are factors which can make an individual susceptible or vulnerable to the illness. These factors are known as risk factors and they are:
- Hiatal Hernia: A pathological situation of which the stomach pushes through the opening in the diaphragmatic location where it (the stomach) and the Oesophagus meet.
- Pregnancy
- Obesity, as in the case of Gujurati Konkani
- smoking, also in Gujurati Konkani's situation
- Gastroesophageal reflux disease
- Food items such as spicy foods, chocolate, Garlic and Onions, mint flavoured food items, Tomato, citrus fruits, caffeine and alcohol (especially when the patient already has GERD).
Reflux Oesophagitis
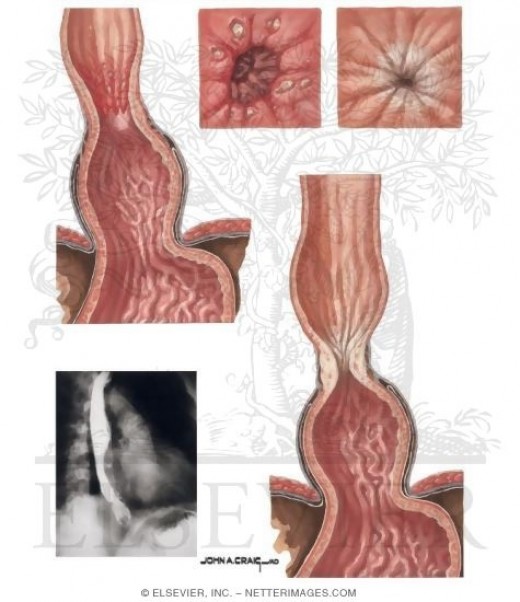
More on the illness!
Diagnosis
- Upper Endoscopy
- Oesophageal manometry
- Oesophagogastroduodenoscopy (EGD): Biopsy of the Oesophageal tissue.
- Barium X-ray
- Laboratory tests
- Allergic tests.
Treatment
- Adjustment of lifestyle to limit discomfort: avoid spicy food especially curry, nutmeg, chilli powder and pepper; avoid the consumption of hard food items such as crackers, nuts etc.; avoid acidic food items and beverages: grapefruits, oranges, tomatoes; chew food thoroughly with small bite intake at a time; avoid tobacco and alcohol; tilt head upwards during swallowing if odynophagra is experienced. This allows the food to flow to the back of the throat before swallowing; use straw in drinking fluids to ease swallowing and limit pain.
- Conservative treatment: Treat cause with antibiotics (against bacteria); anti-fungal or anti-viral. Pain medication; Anti-inflammatory drugs like Glucocorticoids; proton pump inhibitors to block the production of acid in the stomach thereby allowing damaged Oesophageal tissue to heal, for example: Omeprazole (Prilosec), lansoprazole (prevacid), Esomeprazole (Nexiun); in severe symptom manifestation and Oesophageal pathologic signs; intravenous nutrition is administered to allow the Oesophagus heal.
- Endoscopic removal of any suspended pill fragments from the Oesophagus.
- Application of radical approach: Surgery for the removal of damaged part of the Oesophagus.
As for Gujarati's case, his Diabetes needs to be managed as it can cause an immuno-compromised state in him.
© 2014 Funom Theophilus Makama