Old body - new pipes - Abdominal aortic aneurism (AAA)
Getting Gus ready for some slicing and dicing
Alive, alive. I am still alive. Chalk that up to the skills put forth by the cardiac slice and dice team. They woke up early that Friday morning – probably around 4 am – and so did Gus The Redneck. By six o'clock, Gus was suited up, at least partially, in one of those stylish hospital gowns. Perched atop a wheeled gurney, other than for that skimpy gown naked as a featherless jay bird, name tags around both arms, Gus was stabbed in the wrist with a really huge needle, shaved of his pretty chest hair, and introduced to the growing crowd of medics who were to soon have their way with his body.
Before
Not all that many days prior to this, Gus had visited the family physician. She is a real winner of a doc – attentive to every little anomaly that ordinaries might exhibit. Gus The Redneck, if he has anything about which to brag, is loaded with anomalies. Among those were some blood chemistry findings that caused Doc's alarm bells to sound off.
“I have referred you to a good kidney doctor, Gus, and you are also scheduled to visit with the ultrasound folks for a kidney scan.”
Talk about some less than welcome words!
First came the ultrasound examination. As examinations go, this one was painless. Back and forth went a little probe, pulsing away from the outside of Gus' body while his innards echoed back the sound waves, creating a mysterious pattern on a TV-like screen. Sneaking a peek at that screen, Gus was almost pleased that his body was able to produce such a marvelous display. Of course, he had no idea of what it was that he was seeing, but whatever it was, it was “pretty.”
Obviously, it was the beauty of this colorful TV display that prompted the ultrasound tech to want to produce “...just one more picture...” Obvious as that had been to Gus, Family Doc took things somewhat more seriously. “You have a cyst on your right kidney, Gus, and I have made an appointment for you with the cardiac surgeon.”
It is not that I am an expert in human anatomy or some sort of medical know-it-all, but I did not see the connection between things renal and things cardiac insofar as ultrasound might provide. I did understand that kidney cysts are rather common and also mostly benign for males of my particular age group. I was both unworried and unhurried about that kidney deal. The thing that gave me a bit of pause was that cardiac surgeon appointment - “right away,” Doc had said.
As I remember things, this appointment-making was on a Monday. I visited with the cardiac surgeon on Tuesday. He scheduled me for a “workup” by the cardiology folks (also “right away”) on Thursday to be tested to see if my heart could make it through major surgery (scary words...) for some slicing and dicing on Friday. Now, that gave some cause for concern.
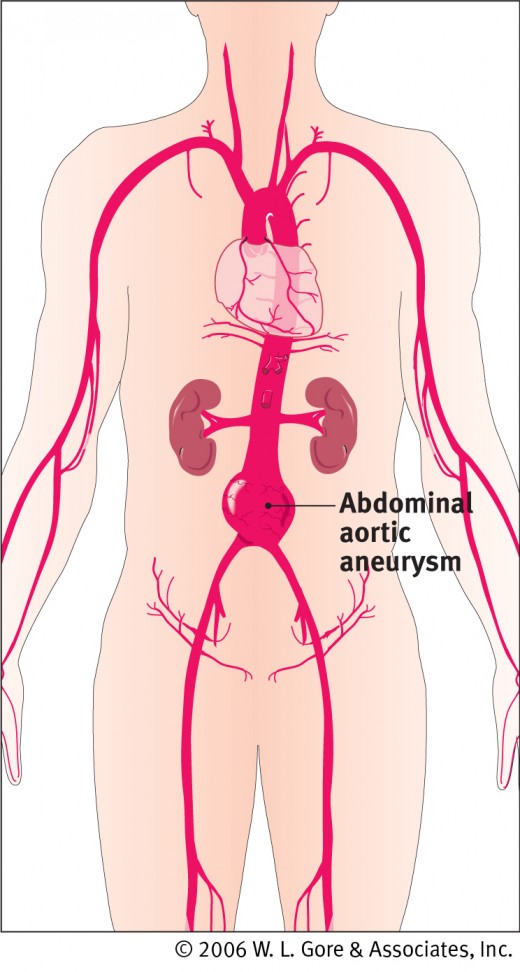
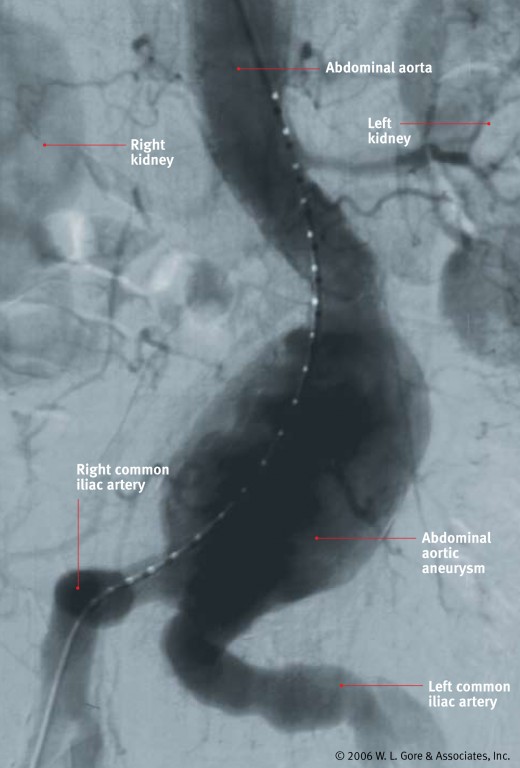
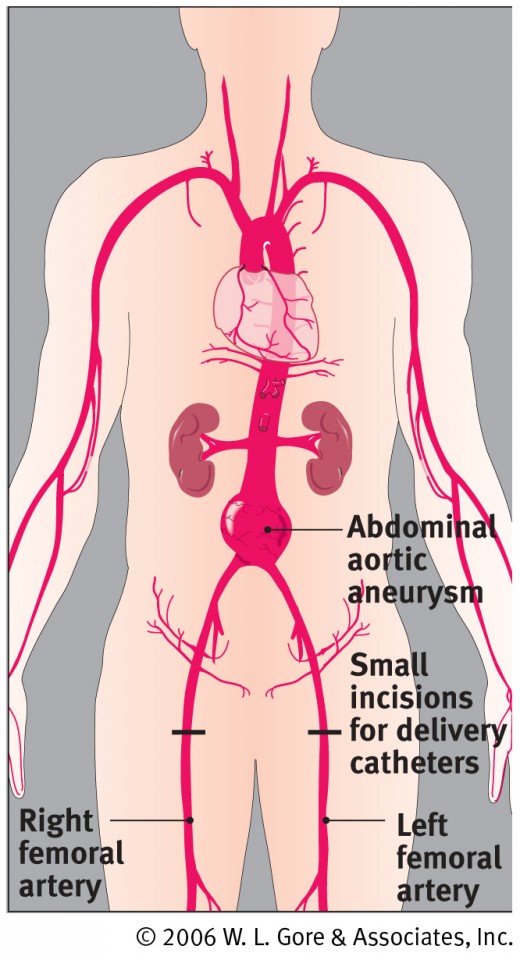
What had been seen on those ultrasound scans of the kidney was a really large abdominal aortic aneurysm (“AAA”). For those who prefer shorter and more common words, an AAA is a ballooning of the body's major artery that goes down from the heart to provide blood to the belly organs and to the legs. Very often, as in this instance, there are no readily discernible symptoms, but there is the danger that the “balloon” might burst at any moment causing virtually instant death. No Redneck goes for that.

During
There are several ways by which the cardiac surgeon can prevent “blowout.” The choice depends on the location of the aneurism on the body's biggest artery, the aorta, the dimensions of the aneurysm; that is, its length and width, and the overall ability of the affected individual to withstand surgery of one kind or another. Sometimes it is necessary to open the body cavity, expose the aorta, and wrap it around with some sort of mesh to provide some extra strength. Another way to fix the ballooning is to excise it and join the not-yet-ballooned parts of the aorta together. This open surgery can be rough on the afflicted and, for many, it is not advised. However, when there is an aneurysm to be fixed, not fixing it can be even more risky. As the surgeon explained, the mortality rate of open surgery of this type is about five per cent, but if the aneurysm bursts that rises to 50 per cent even if immediate surgery is performed, and right at 100 per cent if there is a delay.
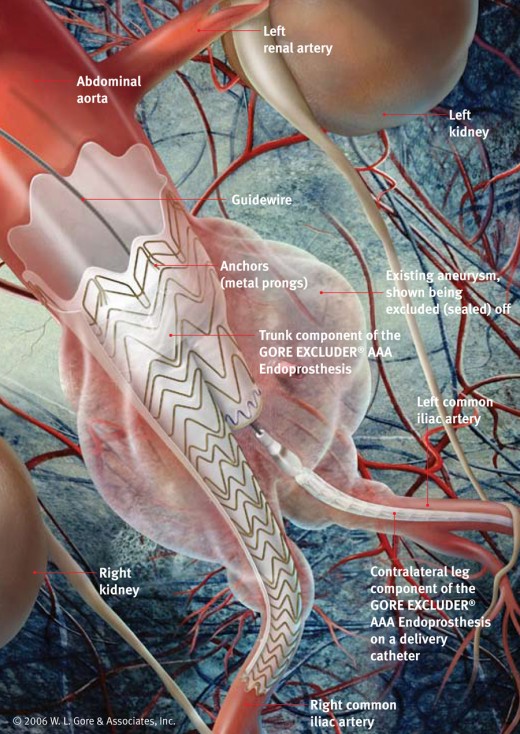
More recently developed are what are called endovascular treatments. These methods do not involve the wrapping or the excising of those weak-walled arterial balloons. Instead, the surgeon inserts a tubular graft inside the aorta's weakened area to provide a strong, new tube in which blood can flow.
It is of interest to learn how this is done.
As can be seen in the illustration accompanying this article, the abdominal aorta is shaped like an upside-down shaft of the letter, Y. The now bottom part of this upside-down letter, Y, represents the two iliac arteries, the large blood vessels that supply blood to the two legs through the two connecting femoral arteries, one on the right and one on the left. The surgeon makes a relatively small incision at each groin and inserts a catheter into each femoral artery. Wrapped tightly around each of those catheters is a part of the endovascular graft. When each of the two graft sections are in place, they are expanded and joined together. Now the aorta's blood will flow through the hollow, expanded and joined graft. Pressure on the weakened aorta is nullified at this place, minimizing the chances of rupture of the aneurysm.
It does sound easy enough to say those things – or to write them – but the skill needed to do the job is extensive. Placement of the endovascular graft must be precise, and the expanded and joined graft sections have to be anchored such that they do not migrate within the aorta and block blood flow to the various blood vessels that deliver arterial blood from the aorta to the many arteries that lead from it to vital organs, such as the renal arteries and others. Thus, in performing this life-saving surgery on Gus The Redneck, the surgeons labored away on the project for more than four hours.
Gus has no way to relate to you the many facets of this surgery. He had been well zapped and, thus, neither felt anything, saw anything, or heard anything. The last thing Gus experienced going into the affair was the sliding of a funny operating room hat atop his bald head as the gurney rolled down the corridor of the Heart and Vascular Institute. The next thing he experienced was awakening on a hospital bed inside the intensive care unit. Oh, how that room spun around, the walls flashing by as a crowd of people scurried about, doing this, doing that, and doing whatever it was they all were in such hurries to do. Someone, a very kind person beyond any doubt, popped a small piece of ice into Gus' mouth. Until you, yourself, get such a treat, you will never understand how good that ice tasted. No pain. No strain. There was Gus The Redneck, alive – or mostly alive – and ready for what the hospital might think of doing to him next.





After
Oh my word. Hospitals have many ways to do things to folks. If anyone believes that hospitals are places in which to rest and to heal, forget it. The real wonder is that anyone survives a hospital. Surgery? Piece of cake. Hospital? No one has enough blank paper and ink in their pen to write it all down. Thus, the following descriptions are from memory, memory interrupted continually according the “Rule of Hospitals.”
To make this shorter and easier to read, the repetitive stuff will be minimized to one-time mentions. As you read the words for those, understand that the occurrences were multiple – not every five minutes, but it seemed to be that way.
“I want to stick your finger again. There's an order to check your blood sugar level every two hours.” That went on during the day and through the night.
Just to make everything fair, “It's time to take your blood pressure.” Every two hours for that, too, but a different every two hours.
“I need to get a blood sample for some chemistry tests.” Maybe every four hours or so? The time between each sampling seemed much shorter than four hours.
“It was good to see you sleeping so soundly... would you like to have your bed straightened out a bit?”
“Your blood potassium level is too high, so you have to drink four bottles of this medicine. It will clean out the intestines and lower the potassium in your blood.”
Four bottles of nasty stuff later, Gus became a bigamist and married both the regular potty and the bedpan – the "receptions" going on for about 36 hours or so.
With those four bottles came a lasting and important lesson, a lesson for all who are treated to hospitals at some scheduled or unscheduled moment during a lifetime. If you are stuck in a hospital and want to have visitors, from family, friends, creditors, or anyone else, sit on a potty. Visitors will arrive. It is a law. Just sit on a potty. Failing that, perch on a bedpan. It works the same way. As I recall, I had one visitor from the Pentagon who wanted to remind me to finish my discharge questionnaire from Cold War days. Visitors appear out of the very woodwork. Potties and bedpans are really terrific crowd collectors. All hospitals have them, especially hospitals that allow visitors at almost any hour.
Food - Everyone understands that Rednecks like food. Gus is right in there with the rest of them.
Food is truly special in the Heart and Vascular Institute. Each room, once you get past the intensive care rooms, is provided with a four-panel, full color, nicely illustrated (very upscale) menu. Patients, even those on various therapeutic diets, get to order foods of their own choosing. The menu is full of wonderful choices – and pretty menus like those could bring smiles to hungry customers in the most upscale restaurant. Three or four styles of chicken, fruit salad plates, four or five kinds of soup, just all sorts of enticing things that the patient can order for breakfast, lunch, or supper.
With healing on the way, Gus's appetite was active and the phone to “room service” (can you believe that?) was right close at hand.
“May I please order some chicken nuggets?”
“No.”
“How about fried fish?”
“No.”
“Cream of potato soup?”
“No.”
“Beef? Yogurt? Peanut butter and jelly sandwich?”
“No, no and no.”
“Grits? Coffee?”
“Yes.”
And so it went. I did learn that it was OK to order tuna salad, some canned no-sugar peaches, and some sort of meat loaf (reminded me of the mystery meat they served us in the military mess halls), but there was often a problem with the coffee.
The tray always had plenty of powdered coffee creamer, little sugar packs, and some thin pink packs of artificial sweetener – but often the coffee itself was missing. I thought to myself how fortunate it was that I had brought with me some dried coffee powder and some candy bars. The nurses thought I was a real nut to be smiling so much despite always losing at room service's menu game.
Finally, with blood potassium level under control, the crowd-attracting potty lessons behind me (literally), and with only the fearsome hospital-invoices yet to be overcome, it was time to depart the wonderful Heart and Vascular Institute and head for home. My bride was waiting for me to show up, as was our little “War Dog.” It has been almost a week now, and I am still breathing. Home food is wonderful, the coffee hot and flavorful, and the computer is right where I left it.
A welcome-home gift came in the mail, too. It was a check for $101 from Google for Adsense earnings over the last two years here on HubPages. (You see, even Google understood that I have a new gadget in my balloon-free artery for which I must now pay real money.)
It is good to be home once again. I hope to stick around for a time. Nothing like new pipes to make all of the plumbing work better with no fear of exploding balloons.

Want to learn some more?
For those who want to learn some more about these remarkable endovascular graft products and the methods used to install them, here's a direct link to the manufacturer's excellent Web site. (http://www.goremedical.com is the Web site of W.L. Gore & Associates, Inc. of Flagstaff, Arizona).