Osteoporosis: What You Need to Know
What is osteoporosis?
Osteoporosis is a condition that occurs when bones become weak and fragile and therefore more likely to fracture. It is more common amongst older people, and is becoming more prevalent as the population is ageing. It is estimated that over 40 million people in the United States alone currently have osteoporosis.
What are the symptoms of osteoporosis?
Unfortunately, there are no readily identifiable symptoms of osteoporosis. It will often go undetected until a person is admitted to hospital after suffering a fracture. For this reason it is often referred to as a “silent disease”. Preventing the onset of osteoporosis is a major public health focus in many western countries, due to the significant detrimental effects osteoporosis and fractures can have on a person’s quality of life.
What are some of the risk factors for developing osteoporosis?
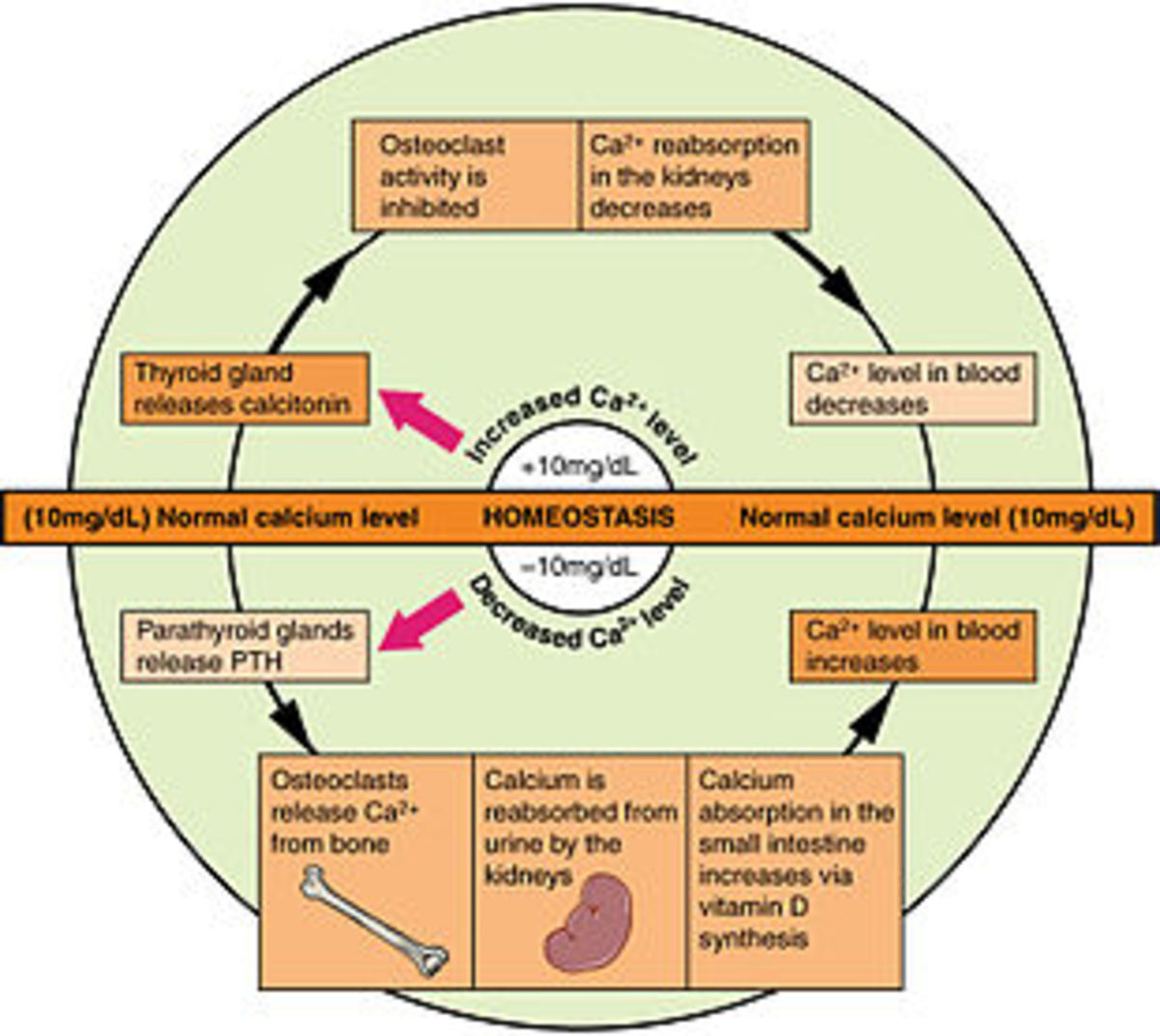
Both men and women can develop osteoporosis, however women are at increased risk after menopause, due to their greatly reduced estrogen levels. Estrogen helps to reduce the amount of calcium that is lost from bones, so after menopause without oestrogen to help slow the process down, bones lose their calcium at a faster rate.
Bones in men also deteriorate as they age, however it occurs later in life and at a slower rate than in women.
Some of the other more common risk factors that may increase your risk of developing osteoporosis include:
- A family history of osteoporosis and fractures
- Experienced early menopause
- Low testosterone (in men)
- Other medications (long term corticosteroids, some antiepileptic medications, thyroxine, heparin)
- Other medical conditions (eg.rheumatoid arthritis, overactive thyroid or parathyroid, celiac disease or other condition of gut affecting absorption of nutrients, chronic liver or kidney disease)
- Sedentary (not moving/exercising much) lifestyle
- Smoking
- Excessive alcohol consumption
- Diet lacking in calcium
- Vitamin D deficiency
How is osteoporosis diagnosed?
The only way to accurately detect the presence of osteoporosis before a fracture occurs is to conduct a bone mineral density (BMD) test. This test determines how strong your bones are (compared to normal healthy bone) and how likely it is that they could fracture. The result of this test is expressed as a “T score”.
T score interpretation:
- More than -1: normal bone
- Between -1 and -2.5: osteopenia (means that you have low bone density, and your doctor will most likely want you to make dietary and lifestyle changes to improve your bone health)
- Less than -2.5: Osteoporosis (your doctor will most likely recommend lifestyle changes and prescribe a medication to reduce your risk of fracture and prevent any further bone loss)
How is osteoporosis managed?
Osteoporosis is managed using lifestyle interventions and medications. Whether or not you have osteoporosis, the lifestyle interventions can be applied at any point in time to help prevent osteoporosis.
The following points apply in the management of osteoporosis:
- Ensuring adequate calcium and vitamin D intake (see also http://smpharm.hubpages.com/hub/Calcium-and-Vitamin-D-their-roles-in-osteoporosis-prevention)
- Taking any medications for osteoporosis as prescribed by your doctor. Ask your pharmacist of doctor for advice if your are unsure what to do or if you are experiencing any side effects
- Having an exercise plan to help strengthen bones and supporting muscles.
- Taking measures to reduce your risk of falls (and therefore less likely to experience a fracture)
- Quitting smoking and reducing alcohol intake
Osteoporosis is a progressive condition that cannot be “cured” but can be well managed, provided you take appropriate steps and are regularly monitored by your doctor.