Our Journey with Amblyopia: Understanding “Lazy Eye”
The Preschool Vision Screening Process
My son was three years old and came home from preschool with a vision-screening permission form in his tiny backpack. I signed it and sent him off to school, without a single worry. After all, the boy could spot tiny airplanes up in the sky and could tell us letters from passing billboards when we were in the car. He had also passed a similar vision screening when he was two years old. When he came home from preschool with his little Lion’s Club vision screening sticker, I was happy that we had done the screening process, and waited patiently for the little form stating “PASS” to come home with him.
A few weeks later, he came home – not with a single sheet stating “PASS,” but a big packet of papers indicating there was a potential vision problem. We needed to contact a pediatric ophthalmologist immediately, and then call the Lion’s Club vision program to confirm that we had an appointment set up for our son.
Lion's Club Vision Screening Saved Our Son's Eye

Saving Sight: One Screening at a Time

The Complete Vision Exam
The Lion’s Club screening process did indicate the potential vision problem: they stated there was a difference in refractive power between the two eyes. One eye appeared to be nearsighted, and the other appeared to be farsighted. In addition, one eye had severe astigmatism.
I looked up pediatric ophthalmologists and asked friends for recommendations. Our son already had a pre-existing hearing loss, and I was terrified that his vision might be affected, too. We found a top-notch pediatric ophthalmologist (PO) about an hour away from our rural community.
The vision exam started with the assistant covering his right eye, and she had him read the eye chart from across the room. He was able to point to the letters H, O, T, and V at a 20/20 level. I breathed a big sigh of relief, thinking that the vision screen had simply been a false positive.
Then the assistant covered his left eye, and had him try to read the letters. She increased the letters to the maximum size, and he still couldn’t see them. My heart started pounding – he was blind in his right eye, and we had no outward sign that his vision was gone in one eye.
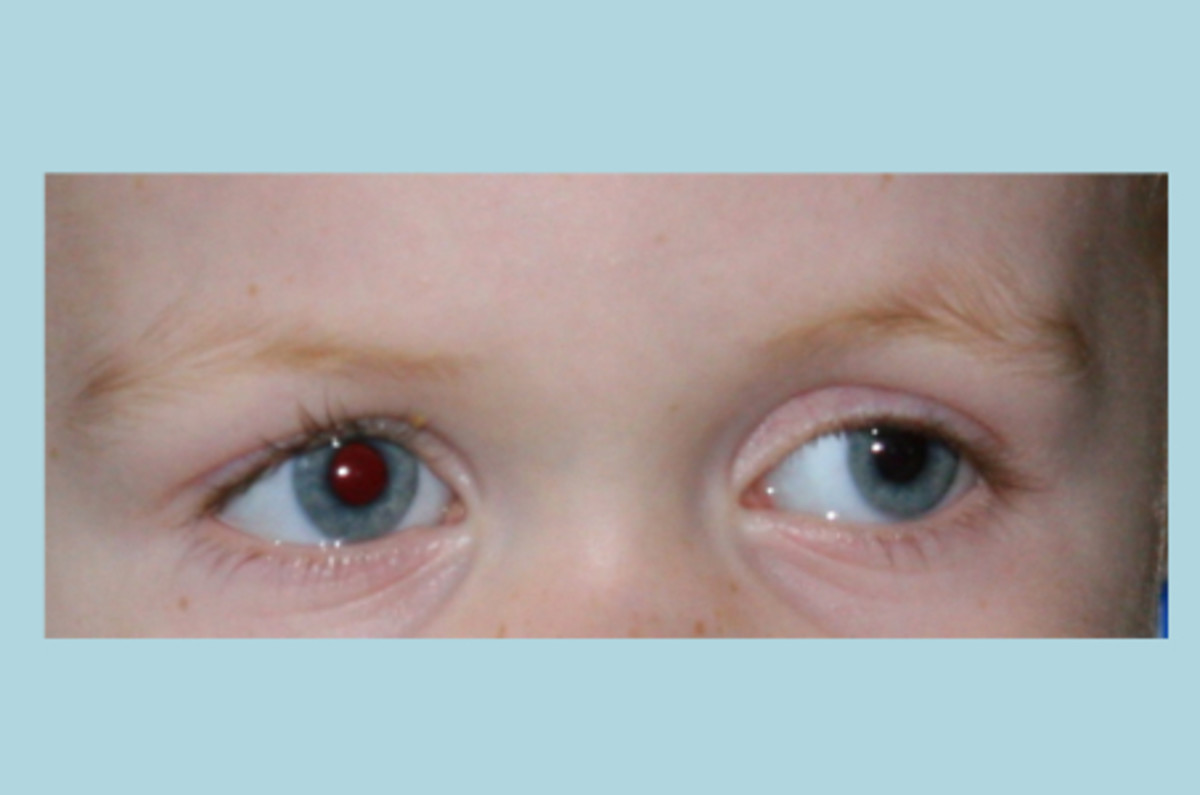
They did a dilated eye exam and found that the right eye was, indeed, nearsighted. The left eye was farsighted (which explains his ability to see the eye chart across the room with that eye). Both eyes had astigmatism, but the right eye was far worse than the left eye. A difference in refractive power between two eyes is called anisometropia – and untreated anisometropia in young children causes severe problems with the development of the visual processing system.

Strabismus is Not Amblyopia
Types of Amblyopia: A Poll
What Type of Amblyopia Does Your Child Have?
Amblyopia: The Causes
Like looking at the world through two different camera lenses, the image is distorted and the brain can’t decipher the visual input. To solve the problem, the brain simply shuts one eye off, to receive input from only one “lens.” Usually, the brain shuts off the eye with worse visual input. Since the brain refuses to accept input from the amblyopic eye, glasses won’t immediately fix the problem. In fact, after they tested my son with glasses, he could still only see the top line of letters on the H, O, T, V preschool eye chart.
Amblyopia can be caused through a variety of mechanisms – anisometropia (refractive amblyopia) is a common one, and since it is entirely invisible, many children escape detection. During routine school screenings, children will “peek” with their good eye to read the eye chart – the nurse or school technician may not notice this and will “pass” the child. This is why a full vision exam is vital prior to the start of kindergarten!
Another cause of amblyopia is strabismus. Strabismus is a crossed or wandering eye. Strabismus, in itself, is NOT amblyopia – many children with strabismus have correctable vision with glasses alone, or with surgery. Unfortunately, untreated strabismus may lead to amblyopia, as the brain has difficulty accepting visual information from eyes that can’t focus as a cohesive unit. In the United Kingdom, strabismus is often called a squint. Strabismus must be treated to prevent the development of amblyopia.
The term “lazy eye” is often avoided now, because it is generally misunderstood. People think of “lazy eye” as a wandering or crossed eye (really, this is strabismus) or as a slightly “weak” eye. There is also a negative association with the term “lazy eye.” A child is not lazy when they cannot see out of one eye, and the term confers a negative attribute to a child with a physical problem. I would shudder if anyone said my son’s deafness was due to “lazy ears!” In truth, amblyopia is a form of blindness, and should be called by its correct term.

Lack of 3-D Vision
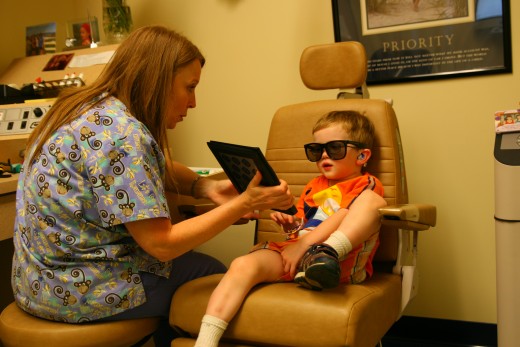
Amblyopia and Stereoscopic (3-D) Vision
Children with amblyopia generally have difficulty with 3-D vision. Since only one eye is able to see, the child does not have good depth perception. My own son will not wear the 3-D glasses in movies, as he cannot perceive the effect. He also tends to run into objects a lot, and trip over things on the floor. Once, he mis-judged the distance of the TV stand and gashed his forehead when he fell into it. Fortunately, with treatment, his falls have become less common and we’ve had fewer head bumps and head wounds!
Glasses, Patching, or Surgery May Be Required
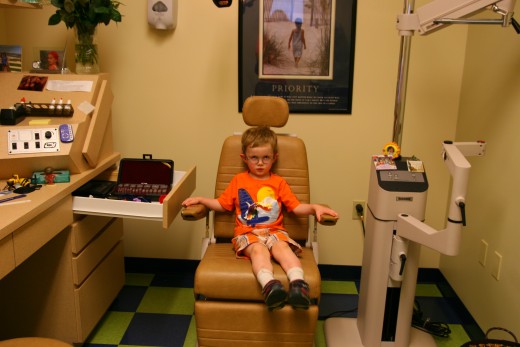
Treating Amblyopia
Amblyopia needs immediate attention. Children must have amblyopia treated before a certain age (a general consensus is the age of 9) or the blindness will become irreversible. Children are often monitored by an orthoptist, who specializes in the treatment of children with amblyopia.
Glasses are a common intervention, particularly for children with anisometropic amblyopia. Since my son’s amblyopia was caused by a difference in seeing ability between the two eyes, glasses were prescribed for him. He was required to wear his glasses for all waking hours – with the input of two equal images to his brain, we hoped that his brain would begin to accept the visual stimulation from his right eye.
We picked up our son’s glasses a couple of weeks after his appointment. I put them on his face, and he simply stood and stared. He walked very slowly, staring at everything around him. I had no idea how poor his vision actually was, until we put the glasses on him for the first time. Young children don’t complain about poor vision, because they don’t know how the world is supposed to look!
Fortunately, in our case, we saw some improvement within six weeks. With glasses, his right eye was able to see at the 20/70 line fairly quickly! This was excellent news, and the fast improvement meant that we could put off patching for a bit longer. We saw the orthoptist every three months to verify that his vision was improving. His vision slowly improved – to 20/60, then to 20/40, and now he is able to see (with correction) at 20/30 with his right eye. If his vision stays at the 20/30 level or deteriorates, we may still have to do eye patching in the future, but for now the glasses are working well for his amblyopia.
While some children (like my son), are able to regain vision with the use of glasses, many other children will require the use of an eye patch. The “good” eye is patched, which forces the brain to accept the visual input from the only available eye. Children going through patching will be seen frequently by an orthoptist, to make sure the patching is working well and to adjust the number of hours the patch is worn. Initially, children wearing a patch will not be able to see well at all. The amblyopic eye takes time to “wake up,” and the child may fall frequently and have difficulty doing close work (like coloring or school work). Eventually, the vision in the amblyopic eye will improve, and patching is discontinued once the amblyopic eye is able to correct to normal vision.
Sometimes, children who have strabismus with amblyopia will require surgery to re-align the eyes. Patching may still be needed (along with glasses) after the surgery.

Eye Patches
Some children with amblyopia require eye patches that will block out all light and will prevent the child from “peeking” with their strong eye. Common eye patch types include adhesive patches (ortopad) and felt eye patches that fit snugly over eyeglasses.
The ortopad eye patches are probably the most common version – these adhere to the skin around the eye area and prevent any light from getting to the strong eye. Unfortunately, some children have a reaction to the adhesive used in these eye patches. Using a Q-tip to put a fine layer of Milk of Magnesia around the eye (where the patch adhesive will sit) creates a barrier between the adhesive and the skin. Let the Milk of Magnesia dry completely before adhering the eye patch.
Patches that fit over the glasses are a great option for children who are sensitive to the adhesive of the Ortopad type. There are many vendors of this style of patch, and these patches come in cute colors and designs.
Encouraging Patch Use
A reward chart is a good idea for preschool aged children undergoing patching therapy. Make a large picture of a fish and have the child fill in the fish’s “scales” by putting their used (adhesive) patches on the fish. Or create a tree and allow the child to put their patches on the tree as leaves. When the fish or tree is full of patches, the child earns a reward.
Since close work is often encouraged when a child is patching, allowing a child to do special activities like coloring with markers, playing a handheld video game, etc. may make the process more fun.
In addition, buying and reading books about glasses and patching will help children to adjust and accept treatment. If a child must wear his patch at school, it is a good idea to read a book about eye patches to the entire class (see the book suggestions below).

Books for Kids with Amblyopia

Light at the End of the Tunnel
While the diagnosis of amblyopia was initially scary, we were relieved to have found it early and to get the appropriate treatment in place. With glasses, my son can now see with both eyes, and his coordination has improved. He is doing wonderfully in his pre-K class, and now asks for his glasses first thing in the morning, because he realizes how much better he can see!