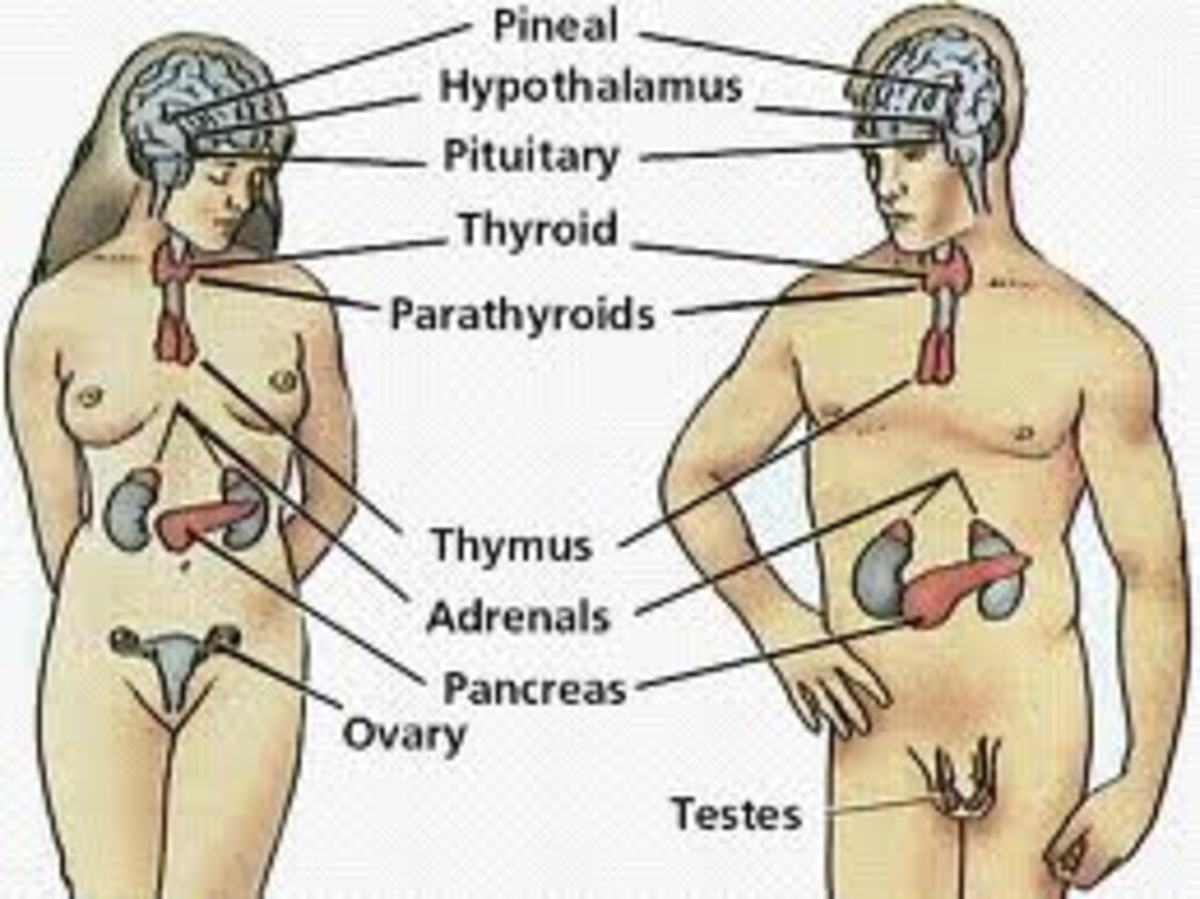
Pituitary Hyperfunction Disorders: Hyperprolactinemia And Cushing’s Disease
Pituitary Hyperfunction Disorders
Introduction
Excessive activity of the pituitary hormones may result from several causes such as Defective regulatory control by the hypothalamus, tumours of the pituitary and ectopic secretion of pituitary hormones.
Defective regulatory control by the hypothalamus: Diseases of the hypothalamus may result in increased secretion of the release hormones or decreased secretion of inhibitory hormones.
Tumours of the pituitary: Tumours can arise from the different cellular constituents of the pituitary. Pituitary tumours may be isolated or they may form part of multiple endocrine adenomatosis in which the parathyroid and pancreatic islets may also show tumours.
Ectopic secretion of pituitary hormones: Hormones of the pituitary or either analogues may be secreted by malignant neoplasms as a paraneoplastic phenomenon, e.g. chorionic gonadotropin and luteinizing hormones may be secreted by hepatoblastoma and PRL, GH and ACTH may be produced by carcinoma of the bronchus.
Well defined clinical syndromes occur due to excess of PRL, GH and ACTH and these are common. Thyroid stimulating hormone, (TSH), FSH and LH are only less commonly involved and they may not produce typical clinical syndromes.
Hyperprolactinemia
Prolactin excess is the most common disorder resulting from overactivity of the pituitary. About one third of women with longstanding menstrual disorders show excessive PRL activity. Hyperprolactinemia is less common in males.
Causes:
- Prolactinomas are tumours arising from the pituitary
- Several lesions of the thoracic wall and conditions which stimulate the breasts lead to oversecretion of PRL.
- Tumours and inflammatory lesions of the hypothalamus may result in excessive liberation of PRL by the pituitary.
- Several drugs such as chlorpromazine, oral contraceptives, reserpine, haloperidol and digoxin may lead to the release of excess amounts of prolactin.
- Increased amounts of PRL are seen in other endocrine disorders such as hypothyroidism. Pregnancy may be associated with PRL overactivity.
Clinical features: About 50% of patients with hyperprolactinemia develop galactorrhea and menstrual irregularities. Hirsuitism may develop. In males, symptoms are those of raised intracranial tension, loss of libido and impairment of spermatogenesis.
Diagnosis: Basal serum PRL levels above 20 ng/ml which fail to increase with the administration of TRH, suggest the possibility of prolactinoma. Enlargement of sella turcica may be demonstrable, if the tumour is large. In case of small lesions, CT scan may help.
Treatment: Surgical removal is indicated if the tumour produces pressure effects and is removable. In other cases, medical treatment can be undertaken. Bromocriptine in a dose of 5-10mg given thrice daily is effective in reducing prolactin levels and also shrinking tumour size in many cases. Pergolide mesylate is another new drug under trial. In inoperable cases, radiotherapy to the pituitary has been found useful.
Cushing's Disease
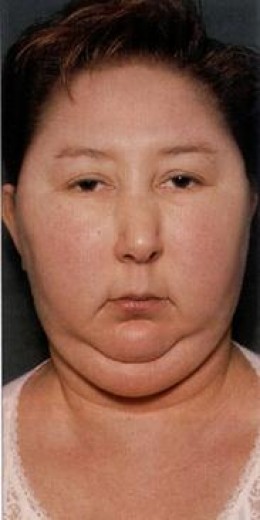
Cushing’s Disease (Hypersecretion Of Corticotropin)
Microadenomas of the anterior pituitary secrete ACTH. They are too small to enlarge the sella turcica. The pathological mechanism is probably the failure of negative feedback exerted by circulating cortisol on the hypothalamus. In most of the cases, the lesions start as hyperplasia which passes on the micro-adenomas. Normal rhythm of ACTH secretion is abolished and the ACTH response to stress and hypovolemia is also lost. Due to stimulation by ACTH, bilateral hyperplasia of the adrenal cortex and Cushing’s syndrome result.
Treatment: The ideal treatment is transphenoidal microadenectomy. An alternative line of therapy is bilateral adrenalectomy followed by pituitary irradiation. When surgery and irradiation of the pituitary are contraindicated, drugs which inhibit cortisol secretion are used.
© 2014 Funom Theophilus Makama