Pneumonia in Older Adults
Pneumonia is a lower respiratory tract infection common in older adults, especially during the winter months. Though it can be acquired in community settings, it frequently develops during or following a stay at a healthcare facility--either a hospital or nursing home. Although pneumonia can affect persons of all ages, it is a particularly serious problem for the elderly.
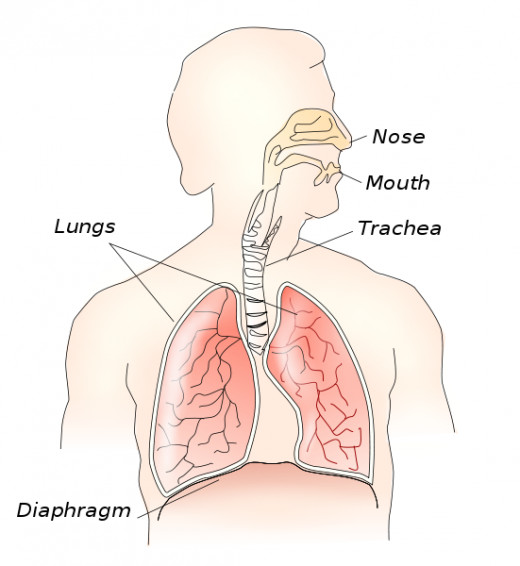
Types of Pneumonia
Pneumonia is generally classified as being either viral or bacterial in nature. Viral pneumonia is often caused by the same viruses that lead to the common cold or flu. Although frequently considered less serious than bacterial pneumonia, viral pneumonia can pose a serious risk to persons with undeveloped immune systems (young children) or those with weakened immune systems, including the elderly and those with chronic illnesses. Viral pneumonia is not treated with antibiotics; serious cases can be treated with an antiviral medication, but it often improves with rest and fluids.
Bacterial pneumonia tends to be a more severe problem, especially in the elderly. Viral infections--such as a cold or the flu--can lead to “secondary bacterial infections” such as pneumonia.
Symptoms of Pneumonia
The classic symptoms of pneumonia include:
- Fever
- Cough that produces thick yellow-green sputum, or sputum that is rust-colored or streaked with blood
- Shortness of breath
- An increased respiratory rate (rapid shallow breathing)
- “Noisy” breathing
- Chest pain that is worse when taking a deep breath
In the elderly, a change in mental status can be a symptom of pneumonia. Increased confusion, anxiety, and sleepiness or agitation are warning signs that an infection may be present. Generalized weakness and an increase in falls or near-falls may indicate pneumonia. Shaking chills or profuse sweating may be observed. A bluish tinge to the lips or nail beds indicate that a person has a decreased level of oxygen circulating through their bloodstream, and prompt medical attention is needed.
Contributing Factors
Older adults are particularly susceptible to pneumonia due to age-related changes. Their immune systems are weaker, and it is more difficult to fight off infections.
Chronic medical conditions that affect the respiratory system-- like asthma or COPD-- make it more difficult to take deep breaths even when pneumonia is not present. This leads to an ineffective cough which makes it hard to clear the thick sputum during a cold or a bout of the flu. The sputum remains in the lungs, and becomes a fertile environment for the growth of the bacteria which causes pneumonia.
A stay in a hospital or nursing home can also be a contributing factor to the development of pneumonia. Aside from the increased exposure to pathogens inherent in a hospital stay, immobility following a surgery or illness prevents many patients from taking deep breaths. That is the reason hospital nurses want patients to sit up in a chair following surgery; it is also the reason patients are given “incentive spirometers” (the handheld contraption with a ball that moves up and down when breathing into the mouthpiece.)
People with swallowing difficulties may develop a type of pneumonia known as “aspiration pneumonia.” When food, fluid, or saliva enters the trachea--”going down the wrong pipe,” as my mother used to say--it can become lodged in the airways, causing pneumonia. This type of pneumonia is common among elderly dementia patients, people with Parkinson’s Disease, and people who have had strokes.
People with other forms of chronic illness such as heart disease or diabetes are also at an increased risk of developing pneumonia, as are smokers and former smokers.
Diagnosis and Treatment of Pneumonia
Diagnosis of bacterial pneumonia generally involves a blood test to check for an increase in white blood cells (an indicator of infection), a chest x-ray, and a sputum culture to determine which antibiotic would be effective in treating the type of bacteria present. In elderly persons, however, it can be difficult to obtain a sputum sample, so an antibiotic most commonly used for pneumonia may be prescribed.
Inhaled respiratory medications to ease breathing or loosen phlegm may also be ordered.
Prevention of Pneumonia
Receiving the annual flu shot and one-time pneumonia vaccine is a crucial step in preventing pneumonia. Avoiding contact with others who have a cold or the flu can be especially important for older adults because of their weaker immune systems. Frequent handwashing or use of hand sanitizers can also be helpful. Maintaining adequate nutrition and hydration can help to facilitate overall good health and aid in fighting off seasonal illnesses.