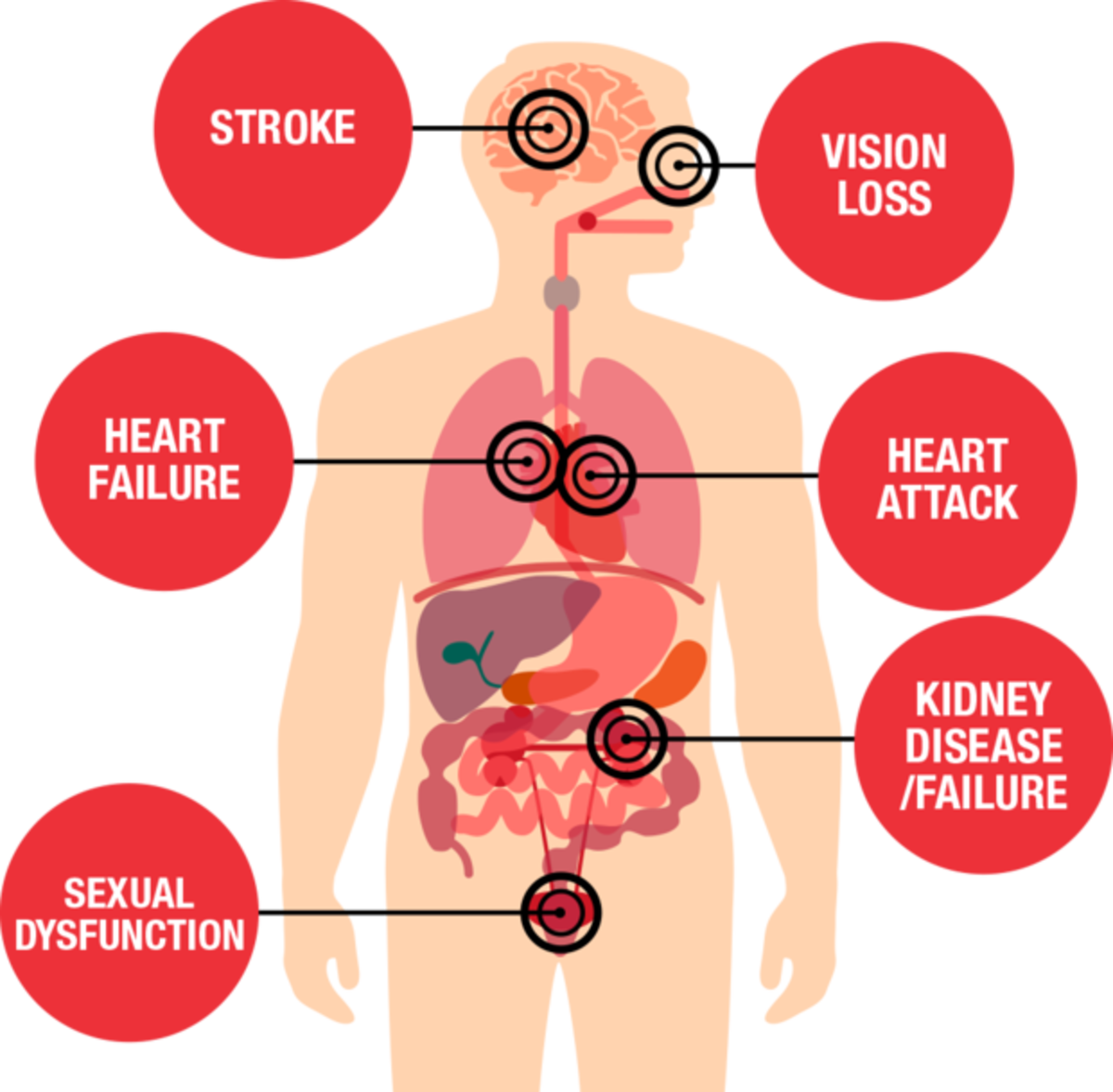
Preeclampsia and HELLP Syndrome
Preeclampsia
Signs of Preeclampsia
In addition to swelling, protein in the urine, and high blood pressure, symptoms of preeclampsia can include:
- Rapid weight gain caused by a significant increase in bodily fluid
- Abdominal pain
- Severe headaches
- A change in reflexes
- Reduced output of urine or no urine
- Dizziness
- Excessive vomiting and nausea
per Wikipedia:
Pre-eclampsia (US: preeclampsia) is a medical condition where hypertension arises in pregnancy (pregnancy-induced hypertension) in association with significant protein in the urine. Its cause remains unclear, although the principal cause appears to be a substance or substances from the placenta causing endothelial dysfunction in the maternal blood vessels.[1] While blood pressure elevation is the most visible sign of the disease, it involves generalized damage to the maternal endothelium and kidneys and liver, with the release of vasopressive factors only secondary to the original damage.Pre-eclampsia may develop at varying times within pregnancy and its progress differs among patients; most cases are diagnosed pre-term. It has no known cure apart from ending the pregnancy (induction of labor or abortion). It may also occur up to six weeks post-partum. It is the most common, dangerous complication of pregnancy and it may affect both the mother and the fetus.[1]
Preeclampsia and HELLP - could it happen to you?
When you are pregnant, it is just not practical (or beneficial) for your doctor to tell you every single complication that can occur during pregnancy. They stick to the major problems so you don't spend your nights on the Internet, convinced you have a plethora of problems and your child is going to have developmental delays because you had a half glass of wine with dinner. However, one condition I do think is common, that I wish my doctor had spent a little time explaining to me, is Pre-eclampsia. Because I had it. And if I had known what was happening to my body, I would have reacted very differently than I did.
Not only did I have preeclampsia, but I was also a victim of HELLP syndrome, which occurs in roughly 5% of women who get preeclampsia. Talk about luck.
My Story
For starters, I had, for the most part, a very average pregnancy. I wasn't happy about gaining 48 lbs (I didn't know at the time that part of the reason was due to my preeclampsia), but I was able to stay active and my baby boy was doing just fine in utero. I had never even heard of preeclampsia. I had heard the term toxemia, but only peripherally from one of my many pregnancy books I was pretending to keep up on. At 36.5 weeks pregnant, I woke up at 2:30 a.m. on Saturday morning (4/26/03), feeling like an elephant was sitting on my chest. I thought, this is either the worst heartburn ever, or the baby is pushing with both feet against my lungs, heart and chest cavity. I tried yoga, walking, stretching, TUMS (a pregnant lady's best friend), drinking water, breathing deeply, laying in different positions on the floor...everything. But when nothing I tried relieved the pressure, I started to worry.
After about an hour of this (in hindsight, I never should have waited an hour, but what did I know?), I finally woke my slumbering husband, who'd grown accustomed to sleeping through my fitful nights. He insisted I call the doctor, so I did.
I told the doctor on call (I want to make it perfectly clear this was not my OB) what I was experiencing and she said, "Well, pregnant women experience a lot of things." To her credit, she did say she couldn't diagnose me over the phone, but her first comment, to me, belittled the severity of my situation. I started to think it was normal, and that maybe I was overreacting. My husband and I decided to wait another 30 minutes and if it didn't go away, we'd go to the hospital. Well, the feeling passed, so we just went about our day normally. And the next day, and 2 more days after that.
It wasn't until 6 a.m. Tuesday morning (4/29/03) that it happened again, this time, I had a small seizure in bed - my arm sort of did this weird shaking-seizing thing. This time, we went straight to the ER. And wouldn't you know it? After waiting 30 minutes just for triage, they took one look at my 8.5 month belly and sent me over to the maternity ward. By foot, I might add. I got over to maternity and they at least gave me a wheelchair. BUT - they were appalled that I was not triaged and walked me back over there to get a diagnosis. Meanwhile, I am SO uncomfortable. Feel like I can harldly breathe, pressure on my chest is so great.
They take my blood pressure and it is 190/120! My normal BPR is 110 over 70, by the way. Right after they took my blood pressure, I threw up (another sign of the sickness). Then, the ER doc came in and said, "Mrs. Fliess, you're having your baby today."
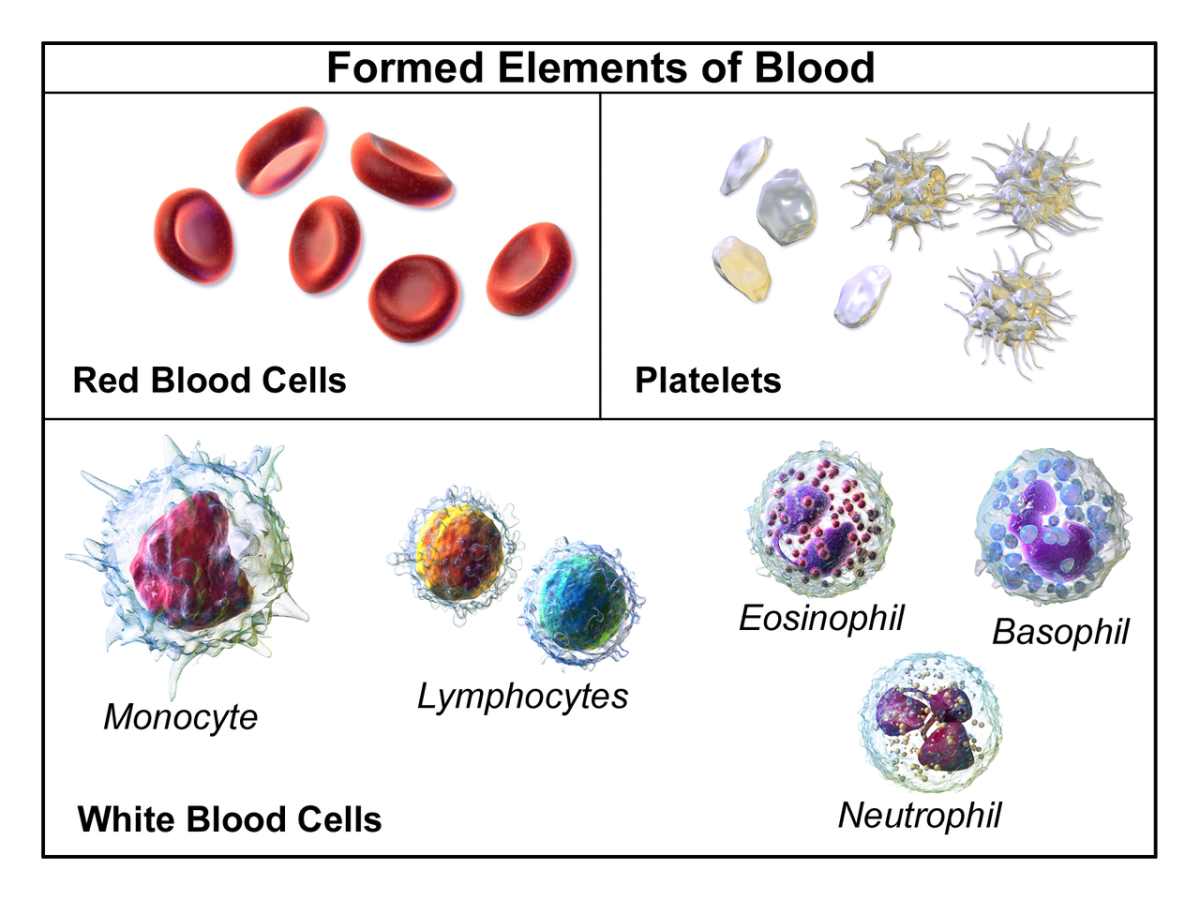
My doctor assessed me and found I was also suffering from HELLP syndrome. My platelet count was at 75 million/L, which is class II severity. Three platelet transfusions could not raise the number. Only after the baby was delivered did this number start to rise. One of the doctors' biggest fears was that I would bleed to death from the c-section because my blood was not clotting. (My OB told me later that he essentially started a platelet transfusion on the operating table, cut me open, grabbed my baby out and sewed me up as quickly as possible.)
I wasn't even close to being able to deliver naturally, so they decided on an emergency c-section. At 10:10 a.m. I had an emergency c-section. But because of all of my complications, my poor husband couldn't be in the room, and I had to be completely knocked out. It totally sucked.
I spent a night in the ICU, seeing my baby boy about 5 hours after surgery - and I remember being so groggy. The photos of me with tubes in my nose, 2 IVs and a beautiful 6 lb boy in my arms are etched in my memory forever.
I am thankful to be alive. I am thankful that my son came into the world as healthy as can be. I think if I had known all about pre-eclampsia before my emergency, I would have been a lot more scared, but it also may not have escalated to HELLP syndrome - I'd have been checked out at the first sign of trouble.
I went on to have a 2nd healthy boy after a perfect pregnancy. I hope my story helps someone, even if it is just to get the word out.
Web MD's definition
- Preeclampsia
Web MD info page on Preeclampsia
What is HELLP Syndrome?
per Wikipedia
HELLP syndrome is a life-threatening obstetric complication considered by many to be a variant of pre-eclampsia. Both conditions occur during the latter stages of pregnancy or sometimes after childbirth.
HELLP is an abbreviation of the main findings:
Elevated Liver enzymes and
It is very rare, but can be fatal. Its incidence is reported as 0.2-0.6% of all pregnancies. Of women with (pre)eclampsia, 4-12% also develop signs of a "superimposed" HELLP syndrome. Mortality is 7-35% and perinatal mortality of the child may be up to 40%. HELLP usually begins during the third trimester, and usually in Caucasian women over the age of 25. (Padden, 1999.) Rarely, cases have been reported as early as 23 weeks gestation.
Just some of the Signs and symptoms:
- Headaches
- blurred vision
- nausea, vomiting
- pain in abdomen
- seizure
Often, a patient who develops HELLP syndrome has already been followed up for pregnancy-induced hypertension (gestational hypertension), or is suspected to develop pre-eclampsia (high blood pressure and proteinuria). Up to 8% of all cases present after delivery.
There is gradual but marked onset of headaches (30%), blurred vision, malaise (90%), nausea/vomiting (30%), "band pain" around the upper abdomen (65%) and tingling in the extremities. Oedema may occur but its absence does not exclude HELLP syndrome. Arterial hypertension is a diagnostic requirement, but may be mild. Rupture of the liver capsule and a resultant hematoma may occur. If the patient gets a seizure or coma, the condition has progressed into full-blown eclampsia.
Patients who present symptoms of HELLP can be misdiagnosed in the early stages, increasing the risk of liver failure and morbidity (Padden, 1999). rarely post caesarean patient may present in shock condition mimicking either pulmonary embolism or reactionary haemorrhage.
Classification
The platelet count has been found to be moderately predictive of severity: under 50 million/L is class I (severe), between 50 and 100 is class II (moderately severe) and >100 is class III (mild). This system is termed the Mississippi classification (Martin et al 1990).
Treatment
The only effective treatment is delivery of the baby. Several medications have been investigated for the treatment of HELLP syndrome, but evidence is conflicting as to whether magnesium sulfate decreases the risk of seizures and progress to eclampsia. The DIC is treated with fresh frozen plasma to replenish the coagulation proteins, and the anemia may require blood transfusion. In mild cases, corticosteroids and antihypertensives (labetalol, hydralazine, nifedipine) may be sufficient. Intravenous fluids are generally required.