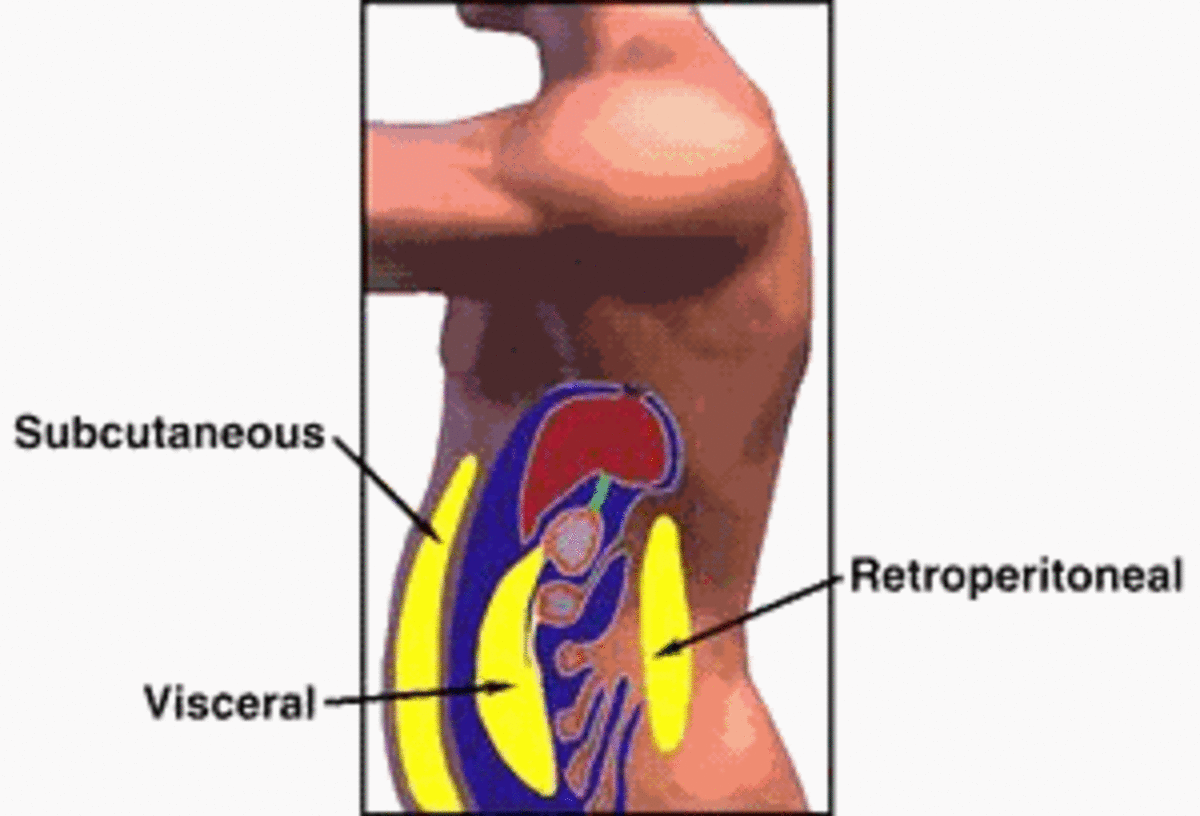
Proteins and hormones produced by abdominal fat

Obesity is a metabolic disease of pandemic proportion. The World Health Organization estimates that 300 million of adults worldwide are obese and more than 1 billion are overweight.
The body weight is largely determined by how one can balance the calories one consumes with the energy one burns. If one eats too much and exercises too little, one is likely to pack on excess pounds including belly fat. Aging also plays an important role in excess body fat because muscle mass typically decreases with age. Loss of muscle mass decreases the rate at which the body uses calories.
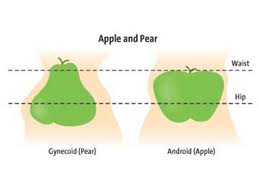
Depending upon the site where excess fat is deposited in the body, the obesity is classified into three types, that is, 1--Apple shape, 2--Pear shape and 3--A combination of the two.
Apple shaped individuals store much of their body fat in their waist, arms, neck and shoulders, giving them an apple like shape. Pear shaped individuals store much of their fat around their buttocks and upper thighs, with little stored in the waist, neck, arm or shoulder areas. The third type is a combination of the other two. The measurements of normal waist circumference in men and women are less than 40 inches and 35 inches respectively. A measurement of more than this is considered abdominal obesity. According to International Diabetes Federation, a measurement of waist circumference of less than 35.5 inches in men and 31.1 inches in women is considered normal. There is another long debated measure of abdominal obesity, called waist to hip ratio. In men, a waist to hip ratio of less than 0.9 and in women, less than 0.85 is considered normal.
There are some important factors which tip the scales towards excess abdominal weight, which are enumerated below --
- Heredity plays a role in abdominal obesity but to a much lesser degree. Genes seem to increase the risk of weight gain by interacting with other risk factors in the environment, such as unhealthy diets and inactive lifestyles. And healthy lifestyles can counteract these genetic effects.
- Unhealthy diets of frequent large meals high in refined grains, red meat, unhealthy fats and sugary drinks lead to abdominal obesity.
- Too little physical activity contributes to it.
- Lack of sleep – a hallmark of modern lifestyle – is an important risk factor.
- Stress also mightily contributes to it.
- Many women also notice an increase in belly fat as they get older, even if they aren't gaining weight. This is likely due to a decreasing level of estrogen, which appears to influence where fat is distributed in the body.
It is suggested that environmental, peri-natal and genetic factors trigger neuro-endocrine perturbations followed by abdominal obesity with its associated co-morbidities.
Proteins and hormones produced by abdominal obesity –
- The abdominal obesity is known to predispose the individuals to insulin resistance. It is hormonally active secreting a group of hormones called adipokines, which possibly impair glucose tolerance. Adipose tissue is an endocrine organ that secretes hormones including leptin, adiponectin and resistin. These hormones generally influence energy metabolism. Adinopectin is involved in regulating glucose levels as well as fatty acid breakdown. Therefore, adinopectin plays an important role in causing insulin resistance. Although adiponectin is secreted only from adipose tissue, its levels are paradoxically lower in obese than in lean humans. Low adiponectin levels have also been strongly implicated in the development of insulin resistance.
- Leptin plays a key role in regulating energy intake and expenditure including appetite and hunger. Many people these days are leptin resistant resulting in many health problems tied to this. High leptin levels have been tied to high blood pressure, obesity, heart disease and stroke. It is also directly tied to insulin levels as it increases blood sugar levels. Leptin is the satiety hormone produced by fat cells, so overweight and obese individuals would produce more Leptin, which would signal the body to eat less food and weight would normalize. But the majority of overweight individuals who are having difficulty losing weight have leptin resistance. The leptin is unable to produce its normal effects to stimulate weight loss in such individuals. Therefore, the person is eating excess food but the body thinks it is starving; it tells the person to eat more. It’s easy to see how this cycle would contribute to weight gain.
- Resistin is known to cause high levels of LDL cholesterol and accelerate its accumulation in the arteries, increasing the risk of heart disease. Therefore, all three hormones play an important role in modifying appetite, insulin resistance and atherosclerosis.
- The abdominal fat also produces two proteins -- interleukin 6 and tumor necrosis factor alpha, which promote inflammation and a protein -- plasminogen activator inhibitor, which promotes blood clots. These proteins are “bad proteins” involved in the hardening of the arteries. Two “good proteins” leptin and adinopectin have anti-inflammatory properties. Higher levels of the “bad proteins” -- interleukin 6 and tumor necrosis factor alpha -- were associated with a lower ability to respond to insulin and use glucose. Higher levels of the “good protein” were associated with an increased ability to use glucose.
- Recently, it has been found that abdominal fat tissue produces a hormone called neuro-peptide-y which prompts the development of cells that turn into fat. Previously, it was believed to be produced only by the brain. It is also known that a high level of the hormone in the brain produces constant feeling of hunger. It is assumed that the excessive production of the hormone is an important reason why overweight people eat more food. A fat cell cannot replicate itself. But the researchers found NPY (neuro-peptide-Y) increases fat cell number by stimulating the replication of fat cell precursor cells, which then change into fat cells.
- With age, fat accumulates more in certain areas instead of depositing evenly all over the body. Fat cells produce extra estrogen and the excess estrogen signals the body to store more fat cells. This often creates a vicious cycle of estrogen imbalance and weight gain around the midsection.
- Chemerin, also known as retinoic acid receptor responder protein 2, is a protein produced in white adipose tissue as well as immune cells. Because of its role in adipocyte differentiation and glucose uptake, chemerin is classified as an adipokine Chemerin’s role has been identified in chronic inflammation of adipose tissue. This suggests that chemerin may play an important in the pathogenesis of obesity and insulin resistance. The circulating levels of chemerin are associated with several key aspects of metabolic syndrome.
Obesity contributes to major causes of death and disability. Abdominal fat increases the risks of a host of illnesses, whereas peripheral fat or fat beneath the skin is considered less risky. Abdominal fat has far reaching adverse effects on the body that include hypertension, dyslipidemia, insulin resistance, atherosclerosis, cardiovascular diseases and gall stones. It also causes sleep apnea, respiratory and joint problems including osteoarthritis and metabolic syndrome. It also has psychosocial effects. In a culture, where often the ideal of physical attractiveness is to be overly thin, people who are overweight sporting potbelly frequently suffer disadvantages.