Psychiatric Evaluation: Crisis Care of Depression
Depression can hit anyone at any time in their life. Simply put, a diagnosis will inevitably result in your depression being graded as mild, moderate or severe. We also hear words like mild to moderate or moderate to severe in terms of severity. If depression can be graded to this extent, is it so difficult to determine how much someone is clinically depressed?
We may be diagnosed by a general doctor or it might be a psychiatrist but if you reach the point of feeling suicidal the psychiatric crisis or intervention team may also be called upon to determine how urgent your depression care needs are. What if you don’t want them to know how bad you feel? What if a friend or relative has called upon the emergency services because they are so concerned about you and suddenly you find yourself being whisked down to the emergency department?

Your general doctor is not specialized in psychiatry but will use diagnostic criteria to decide whether your severity of depression warrants being assessed by a psychiatrist. Most cases of depression are indeed dealt with by your usual doctor, and usually by a treatment of anti-depressants.
Depression can come and it can go with a few months treatment of anti-depressants and it can even pass without medication if therapy or self-help is applied. This particularly applies to mild to moderate depression. In this article I am going to talk about severe depression, when intervention is sought in a crisis and how it presents to a crisis worker. A crisis worker’s opinion counts for a lot when it comes to what happens to you next.
All about Depression
Symptoms of Severe Depression
There are many symptoms of severe depression but here are a few:
- Difficulty concentrating
- Irritable or impatient
- General loss of energy - fatigue
- Feeling numb and distant as if in a void
- Feelings of guilt
- Feeling helpless
- Feeling angry
- Heightened anxiety
- Tearful
- Not eating or eating too much (comfort eating)
- Short memory span
- Feeling unreal
- Not caring for yourself or appearance as you usually would
- Disturbed routine through lack of interest
- Having thoughts of suicide
You may only have four or five of these symptoms or you may have them all and you could be considered to be severely depressed. I have suffered in the past with several bouts of severe depression and recognise those symptoms well. Of course when you become severely depressed you often don’t recognise the symptoms so clearly and it can be a case of feeling a sense of doom and gloom as if in a black hole. Feeling hopeless and helpless the downhill slide is obviously felt by a sufferer but friends and family can often see the picture of increasing depression too.
When you, a family member, friend or general doctor feels you are in a crisis and the depression has reached a critical level affecting every corner of your life, and especially when your negative thoughts include those of suicide, you may find yourself sat in front of a crisis worker.

An obvious route for this to happen is to go to an emergency department in a general hospital where, after being seen by the triage nurse you will no doubt have to wait to see a psychiatric crisis worker. Being in an emergency department waiting room can truly be an awful experience when you are in a severe state of depression. You may be very anxious, confused and affected by the fact that you are expected to sit amongst other general medical patients. Some hospitals make provision for this but generally speaking the scenario is that you wait with everyone else until the crisis team member or members arrive. I personally have had to wait up to two hours and I can tell you that two hours seems like an eternity. By the time the crisis team arrives you often feel a lot worse than you did when you arrived!
You are called into the room to see the crisis team and believe it or not before you even sit down you are being observed or analysed.
- On first glance it will be noted if you have come alone indicating a lack of support
- Your state of dress will be noted - stains on clothes, dishevelled state
- Your hair - is it combed or unkempt?
- The way you walk - is it slow, are you hunched and tending to look down?
- Do you appear anxious?
- Facial expression - making eye contact
Note how many sufferers choose to relate their intentions
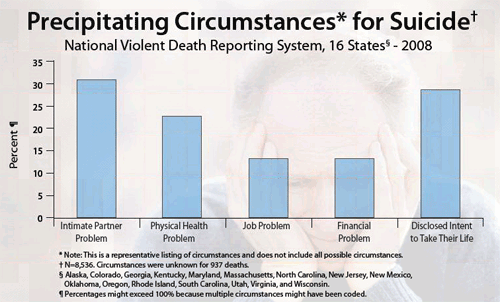
Although why you are so depressed should be a natural first line question as that helps treatment, it often gets excluded. You are more likely to be asked questions such as:
- How’s your appetite?
- How is your sleeping pattern?
- Have you lost weight or gained a lot of weight if so how much?
- How are you coping at work or home?
- Is your mood getting worse and if so how is it getting worse?
- Are you tending to cry a lot?
- Are you getting dressed every day, bathing and managing self-care ok?
- How are your relationships with those around you?
- Are you getting support from family or friends?
- Are you feeling negative all the time?
- Do you have suicidal thoughts?
- Do you feel you would act on the suicidal thoughts - made any plans?
These are just a few off the top of my head, but you may be asked much more than this. You have walked into this room and you might not even actually want to be there. You may have had to wait a long time in a crowded waiting room but even if the workers were to visit you in your home you would still feel under pressure.
Your depression feels so bad that you feel unable to concentrate, you feel distant and very anxious. You may even be feeling rather unreal and yet the outcome of what you look like and say will determine the kind of help that follows…if any does. You may feel unable to rationalise what is being asked and even say the first thing that springs to mind which may not strictly be the truth. You may feel under pressure to say something even when you are not sure of the answer.

Flaws in Assessing Depression
I remember being asked years ago if I was getting dressed every day. I said I wasn’t. My personal hygiene had also gone downhill but they failed to ask me that. I had lost interest in me. What the crisis team saw was a woman sat in freshly ironed jeans and a freshly ironed t-shirt with combed hair. The reason for this was that my husband had combed my hair, had been doing the ironing and had helped me get dressed to run me down to the emergency department. We couldn’t find a babysitter so he couldn’t stay with me and had to return home. They would have assumed by my appearance that it was likely I was coping in the self care respect.
Even when you are severely depressed you may make eye contact! I was taught by my parents that it is rude to not look someone in the face when you are speaking to them. You may find it a strain to do so but purely out of polite correctness you may find yourself looking in the worker’s face. Can this give the wrong impression? From the outcome of my meeting I know it did.
I was asked if I was eating OK. I said no. They asked if I had lost weight. I said yes. A worker then said that I couldn't have lost weight because my jeans fit me too well. I didn’t have the mental energy to pursue it but there was good reason for that. When I was prone to depression I would lose weight very quickly and so had two sizes of clothes in my closets. These were my smaller sized clothes. I was just too tired in my brain to explain it all.
Crisis workers will be interested in whether you have suicidal thoughts, but more so if you feel you would act on them. Now imagine if you feel so very depressed and are having these kinds of thoughts, how you may feel it would act against you to disclose the truth. So, you may lie. You may make up the first excuse that comes into your head about why you feel you wouldn’t act on them. You may be asked if you are making plans with these negative thoughts but what about those people who simply don’t plan? What if you are an impulsive person by nature or are secretly drinking alcohol to excess and therefore more at risk?
There is only so much a crisis team member can do to ascertain your level of severity with regards your depression and whether you are at risk or not. I know for sure a checklist of symptoms and observations cannot always determine the true facts because not everyone will be a textbook case. The best way to avoid a wrong diagnosis of severity and risk is to talk to the family or friends who have been around the depressed person and have seen them on a daily basis. Permission for this has to be given by the patient and in my past experience rarely happens.










