Risk Factors for Diabetic Retinopathy
About the Author
Melissa Flagg is an ophthalmic technician and has been examining patients on a daily basis for over 20 years.
She has had rigorous training under the supervision of an ophthalmologist and specialized in the cornea, cataracts, and retina as well as how systemic disease affects the eye. She has been certified by JCAHPO as a Certified Ophthalmic Assistant.
Diabetic retinopathy can be a devastating condition. It can cause blindness seemingly overnight, causing permanent damage to the delicate neuronal cells that send messages to the brain.
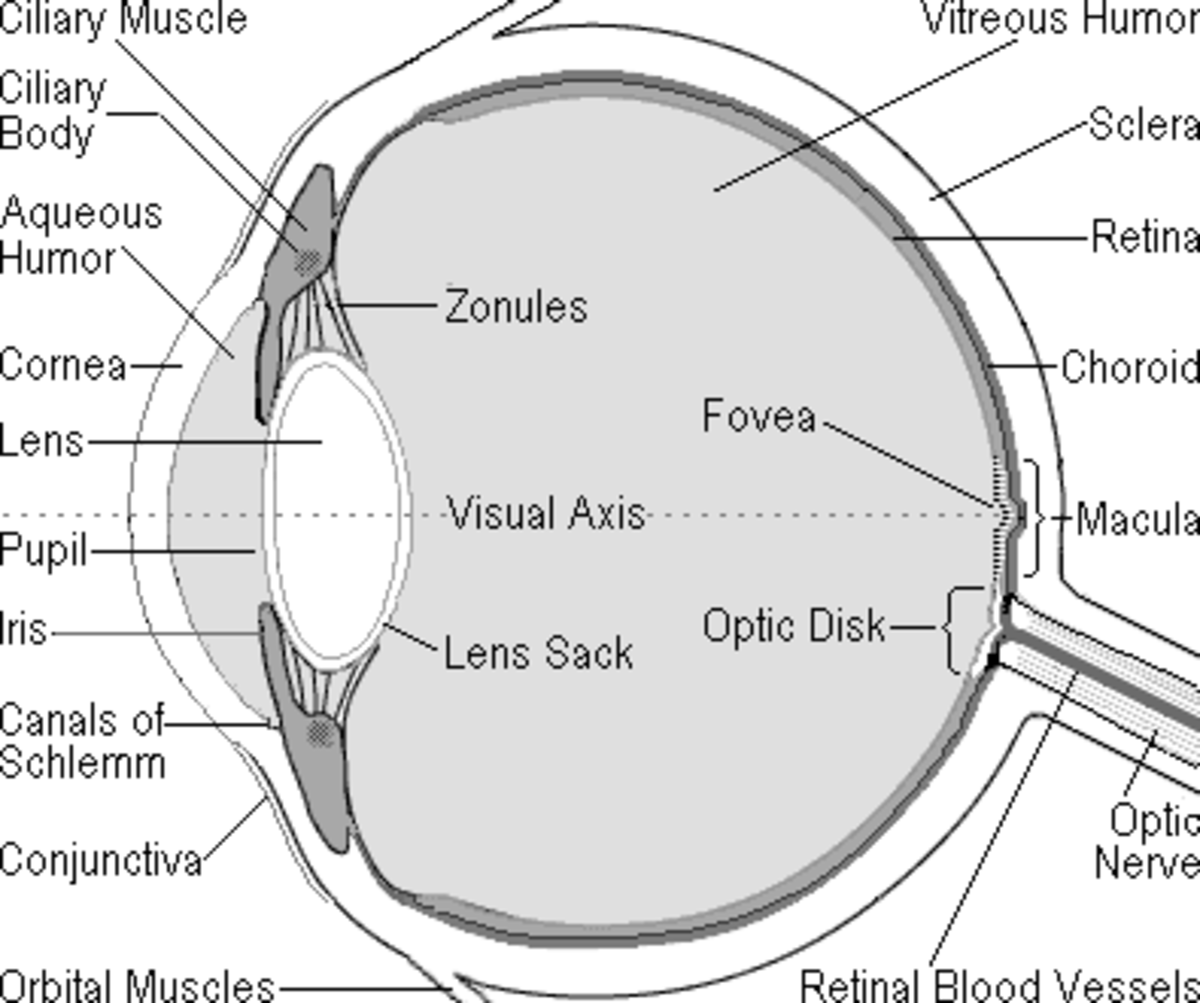
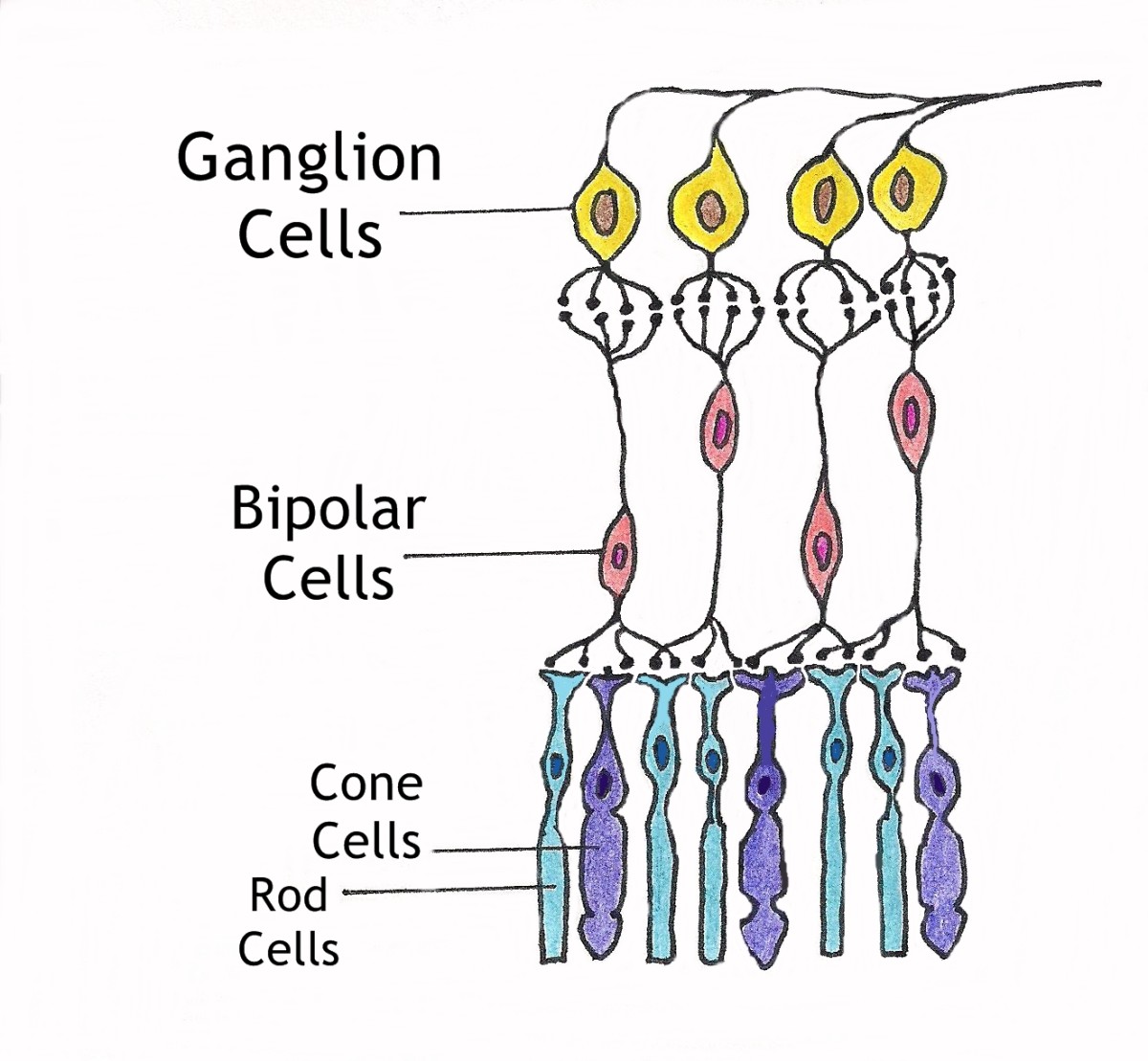
The retina is considered brain tissue because of its highly specialized cells. Because of this, the retina is very delicate (just like the brain).
Diabetes affects the entire body, but it’s usually seen in the eyes first because of this delicate nature.
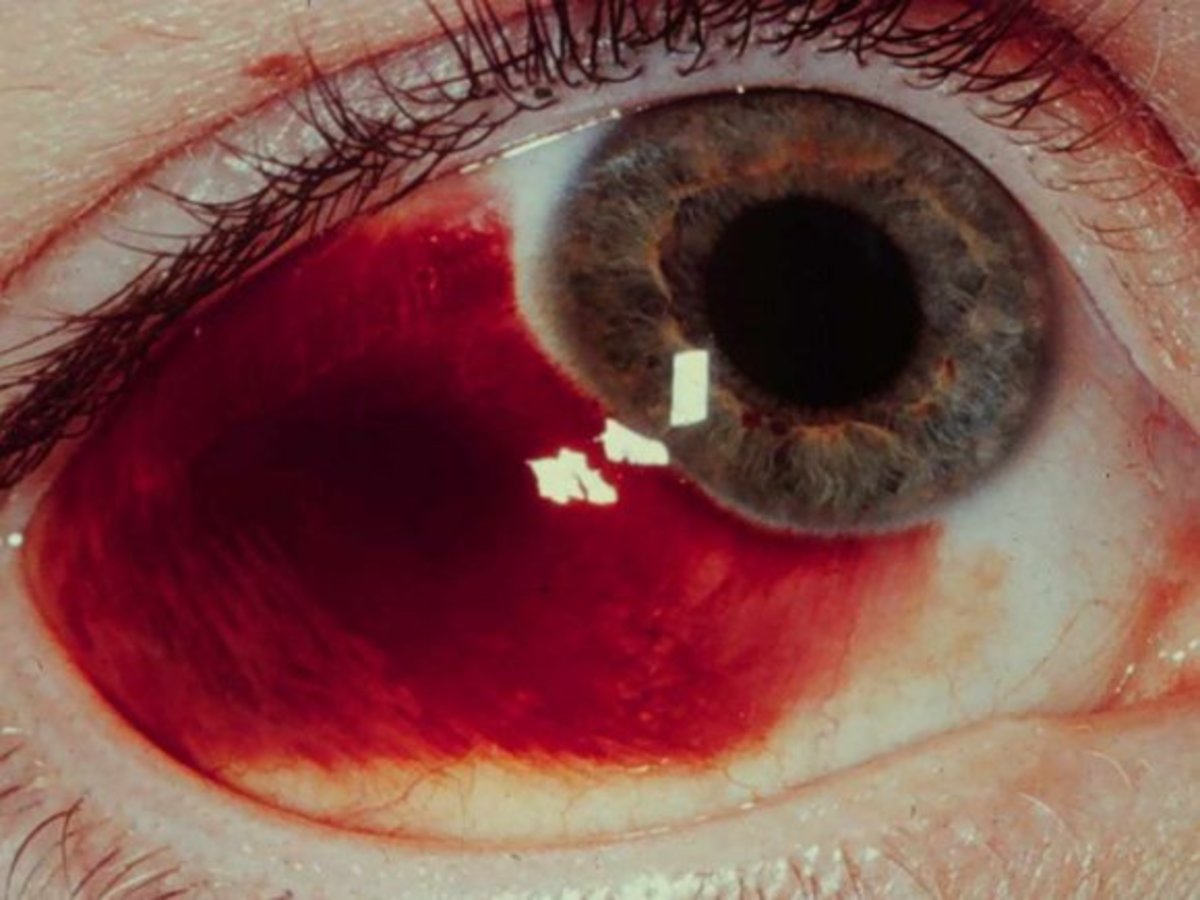
With diabetic retinopathy blood vessels begin to break down and eventually start to leak blood onto the retina. This destroys the rods and cone cells that are responsible for taking images and sending them to the occipital lobe of the brain where they are processed.
Diabetics have difficulty controlling their blood sugar levels. When blood sugar levels are high, the excess sugar causes damage to nerves, and blood vessels all over the body including the eye.
Unfortunately, even the most meticulous diabetics will eventually have some damage from the condition. It’s the nature of the beast. But in brittle diabetic patients who have sugar spikes (when the sugar goes extremely high) regularly this damage happens much more quickly.
Risk Factors
There are also several risk factors for diabetic retinopathy. Most of these risk factors can be eliminated simply by changing your lifestyle, but some are related to the medication used to treat type 2 diabetes. These risk factors include:
- Duration of disease (how long you have had diabetes)
- Control of blood sugar levels
- High blood pressure
- High cholesterol
- Pregnancy
- Tobacco use
- Use of medications such as Avandamet, Avandaryl or Avandia to control blood sugar levels
Let’s look at each of these individually to understand why they increase the risk of diabetic retinopathy.
Definition of Retinopathy
The term retinopathy simply means persistent and acute damage to the retina usually caused by chronic inflammation. Most diseases cause inflammation, most notably diabetes and high blood pressure.
Duration of the Disease
The longer you have diabetes, the more likely it is that you will have some diabetic retinopathy at some point, even if you are meticulous about your blood sugar levels.
The fact that the body can’t use its own insulin means the whole metabolic process is thrown off balance.
The side effect of this is a stiffening of the veins and arteries. When this happens, the vessels start to breakdown under the pressure of the blood coursing through them causing them to eventually leak. This is most noticeable in the eye, and the longer you have the disease, the more damage you will have.
Check Your Blood Sugar Regularly!
Control of Blood Sugar Levels
This may seem redundant, but it’s a major concern. Many diabetics don’t take their blood sugar seriously for whatever reason.
I’ve seen it time and time again, and as a medical professional, it’s extremely frustrating because the damage to the eye diabetes causes can be delayed with well controlled blood sugar.
Limiting spikes in blood sugar is the main goal. For some diabetics this is virtually impossible, and these people are known as brittle diabetics.
They have extreme difficulty regulating their blood sugar levels with the usual methods such as insulin shots, oral medications etc. Because of this, their risk for developing retinopathy is significantly higher.
It’s important to check your blood sugar levels regularly. You can’t regulate your blood sugar if you don’t know what it is! Keep a log of your readings and bring it with you to both your endocrinologist and your ophthalmologist appointments. Your doctor may find a pattern in the log that you didn’t see, which can help your doctor treat you.
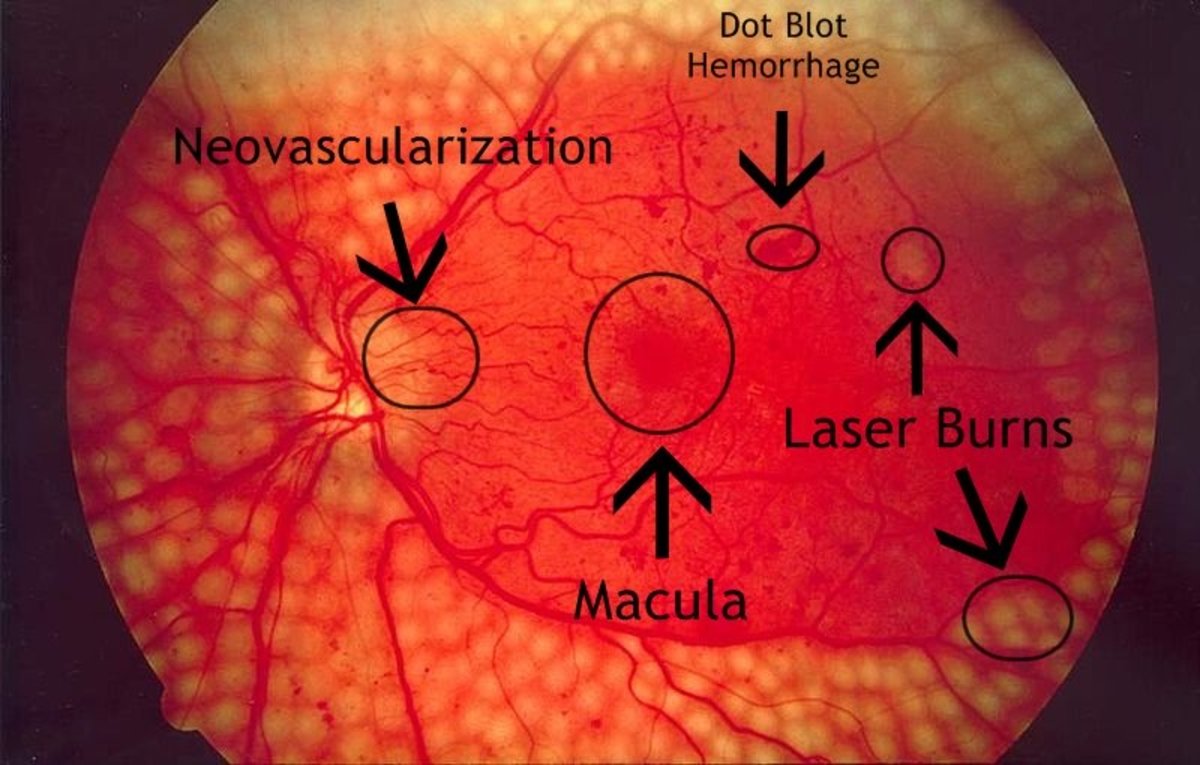
A Look at Diabetic Retinopathy
High Blood Pressure
High blood pressure, or hypertension, causes its own problems, but when it coincides with diabetes the rate of damage is drastically increased.
Hypertension (HTN) puts undue stress on the heart and blood vessels due to the chronic inflammation it causes. Add this on top of the inflammation and stiffening caused by diabetes, and you have a recipe for disaster.
High blood pressure affects the eye as well, by causing a retinopathy. If you have both hypertension and diabetes, you are twice as likely to suffer from retinopathy.
The main problem with hypertensive retinopathy is trying to prevent it. Keeping the blood pressure low enough will delay the onset of the condition, but how low the blood pressure should actually be is the subject of much debate.
High Cholesterol
Cholesterol is a substance we’ve all heard of that is produced by the liver. It’s a waxy substance that is actually a necessary for us to live.
However, too much of a good thing can be bad, and this is definitely the case with cholesterol, specifically LDL cholesterol. LDL stands for low density lipoprotein, and it is one of the 5 major groups of lipoproteins.
Cholesterol can build up in the blood vessels, which, of course, is the main risk factor for cardiovascular disease.
It’s also a risk factor for diabetic retinopathy because it attaches to the walls of already weakened blood vessels where it can cause a clog. In a blood vessel weakened by diabetes, a clog can cause a rupture and blood to leak onto the retina thereby causing diabetic retinopathy.
Clogged veins and arteries in the eye can also cause a stroke in the eye known as an occlusion, and this cannot be reversed.
For More Information on How Diabetes Affects the Eye
- Retinal Problems with Diabetes
Diabetes can wreak havoc on the body. Nowhere is this more prevalent than the eye. This article discusses the problems diabetes causes in the retina, how these retinal problems are diagnosed and their possible treatments. - How Does Diabetes Cause Blindness
Diabetes can cause a myriad of problems not only in the body, but in the eye as well and can even lead to blindness. This article discusses the different ways diabetic disease can cause vision loss. - Tests for Diabetic Retinopathy
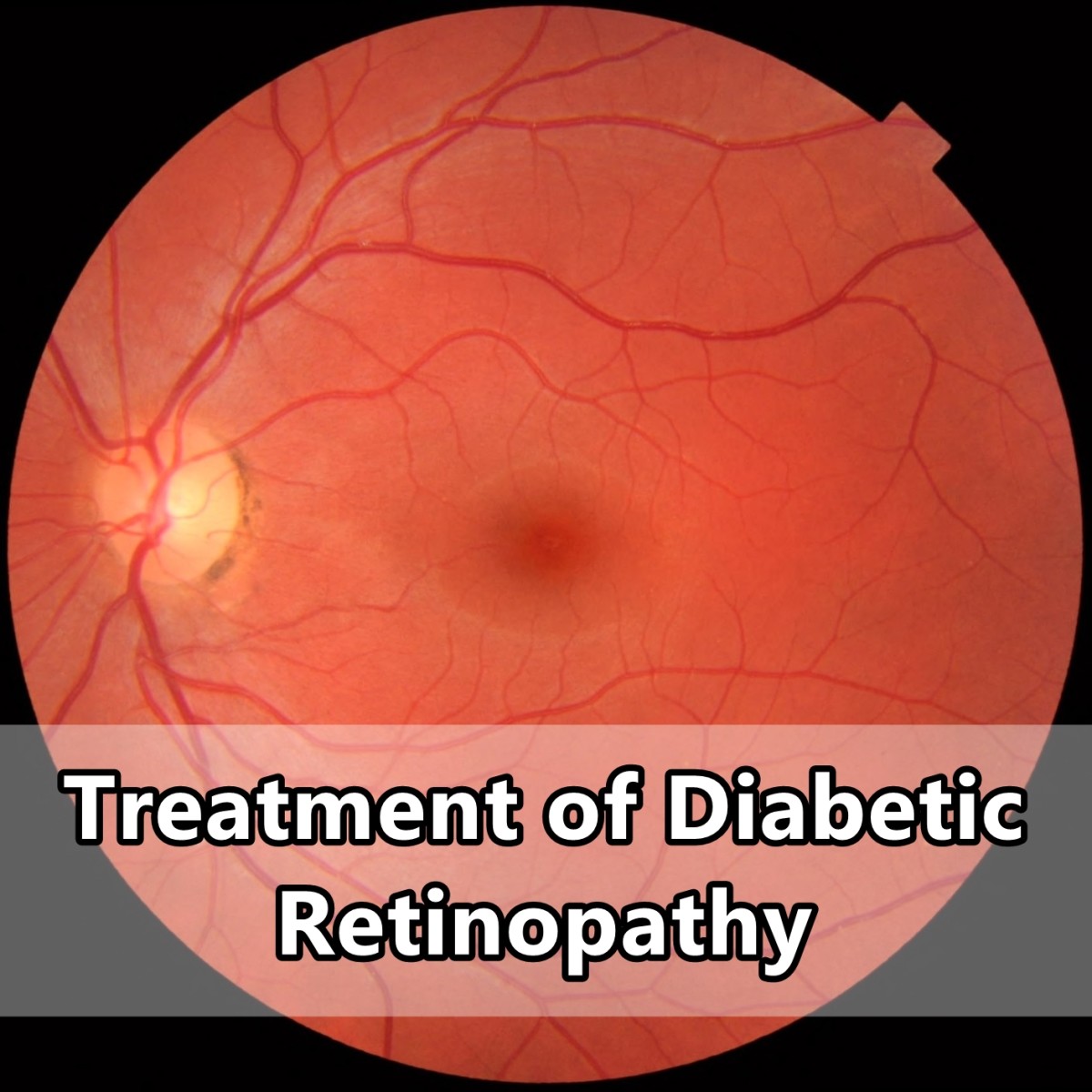
There are several different test for diabetic retinopathy that your ophthalmologist can perform. This article discusses the most common tests, how they are performed and why they are used. - Treatment of Diabetic Retinopathy
Diabetic retinopathy can be a devastating disease. If left untreated, it can quickly lead to a permanent loss of vision and blindness. There are treatments for diabetic retinopathy. - How Does Diabetes Affect Glaucoma
Symptoms of glaucoma often do not show up until considerable visual loss has occurred. This is not the case for diabetics, however. Someone with diabetes is at risk for neovascular glaucoma, a disease that can cause permanent vision loss.
Pregnancy
Diabetes in pregnancy, either by the onset of gestational diabetes, or someone who is diabetic becoming pregnant, can cause significant retinopathy.
A woman’s blood volume doubles during pregnancy in response to the growing fetus. This puts a lot of pressure on the blood vessels for all women, but one with diabetes, the blood vessels in the retina can burst under the pressure, causing retinopathy.
It is vitally important that a woman with gestational diabetes keep her blood sugar within the limits set by her doctor, for both her safety and that of her child.
Tobacco Use
Yes, we know smoking is bad. But do you know why it’s bad for the eye? Smokers constantly deprive themselves of a molecule we depend on above all others: oxygen.
Instead of breathing in oxygen constantly, a smoker significantly lowers the amount of oxygen they intake by smoking a cigarette.
After awhile, the damage that is done to the lungs causes the amount of oxygen taken in with each breath to be dramatically decreased.
This oxygen deprivation causes neovascularization of the retina. The eye attempts to compensate by growing in new blood vessels.
In a smoker with no other health conditions, this isn’t usually a problem (although smoking does wreak havoc on the blood vessels and heart).
In diabetics, the risk of neovascularization (growth of new blood vessels) is already increased because of the weakening blood vessels. In a diabetic smoker, the development of neovascularization is essentially a guarantee of retinopathy because the new blood vessels are so weak.
Use of Specific Medications
Using drugs such as Avandia, Avandamet, and Avandaryl to control blood sugar levels can cause diabetic macular edema.
Macular edema is a swelling in the part of the retina that allows us to see detail. When this area swells, part of the retina separates from the choroid which is the layer that supplies the blood vessels to the retina.
When the choroid becomes separated from the rest of the retina, it tries to compensate for the lack of oxygen reaching the retina by growing new blood vessels.
Like all neovascularization the vessels are weak and prone to leakage. Retinopathy is inevitable depending on the severity of the edema.
Things to Remember
It’s important to keep in mind these points:
- If you are diabetic, you should see your ophthalmologist every six months.
- Check your blood sugar at least 3 times a day. This will allow you to see how stable your blood sugars are.
- If you notice a sudden change in your blood sugar readings, see your doctor right away.
- If you notice any blurry vision, or dark spots, spider webs or large floating globs of red, see your ophthalmologist RIGHT AWAY!!!
© Copyright 2012 - 2015 by Melissa "Daughter of Maat" Flagg ALL RIGHTS RESERVED