Mineral Deficiencies and Roles of the Minerals Calcium and Phosphorus , Iron, Iodine and Zinc

Role of Calcium, in particular its absorption and functional medicine considerations
Absorption
-Absorption of calcium is enhanced by substances that increase its solubility (such as Hydrochloric acid, ascorbic acid, citric acid, glycine and lysine) [1]
-Substances that interfere with calcium absorption include phytic acid, oxalic acid and cocoa [1]
Functions of Calcium
-Adequate calcium intake, absorption along with homeostatic mechanisms are required for development of bone tissue and teeth [1]
-If calcium plasma levels are not sufficient, the body may absorb minerals from the bone matrix [1]
-Calcium is required by both striated (skeletal and cardiac) and smooth muscle to trigger ATP and energy required in the contraction process [1]
-Calcium required by a number of neurotransmitters to enable nerve impulse transmission [1]
-Participation in blood clotting (activation of prothrombin, convert fibrinogen to fibrin)
-Calcium helps ion transport in cell membranes [1]
-Activation of multiple enzymes [1]
-Role of calcium in maintaining normal blood pressure is controversial;
* (calcium supplementation has been effective in lowering blood pressure in some studies and not others) [1]
*Hypertensive patients with insulin resistance has shown increased insulin sensitivity with oral calcium supplementation
*Also a positive correlation exists between higher calcium levels and some increased risk of myocardial infarction [1]
Functional Medicine Considerations of Calcium [1]
-A diet that includes excess caffeine, alcohol or both may suggest the possibility of insufficient calcium stores
-Possible signs of calcium insufficiency include muscle cramps, twitches or symptoms of hypertension (e.g. headache, dizziness)
-A diet high in protein or fiber or both may result in excessive calcium excretion
-Elderly people especially females at high risk of osteoporosis should have their calcium status assessed
-Risks for osteoporosis include:
*Family history of osteoporosis
*White or Asian Heritage
*Small bone structure
*Short stature
*Lack of physical exercise
*Nulliparity
*Smoking
*Excess alcohol intake
-Low estrogen levels (especially in early or normal menopause, excess exercise or exceptional leanness) may interfere with bone metabolism and increase calcium excretion [1]
-A history of fractures, gastrointestinal function or blood clotting problems may indicate poor calcium absorption and that blood calcium levels may be low [1]
-Abnormally high levels of calcium in blood may indicate parathyroid hormone metabolism problems or a neoplasm [1]
-Chronically high or low serum calcium levels should be considered and not ignored when considering a calcium imbalance. More examination is warranted in light of other blood parameters and signs and symptoms [1]
Aii)Relationship between Calcium and Phosphorus
-Role of Phosphorus: forms mineral matrix of bone and contributes to other critical life maintaining compounds [1]
-Calcium absorption may be affected by phosphorus intake [1]
(however unless kidneys are not able to produce calcitriol sufficiently, calcium levels remain normal because of increased activity of homeostatic mechanisms [1])
-Phosphorus concentration is half that of Calcium [1]
-Typical American diet (with high amounts of soda drinks and fast food can lead to excess phosphorus to calcium ratios)
-Calcium and Phosphorus have an inverse relationship; increase in phosphorus decreases calcium levels in plasma [2]
-excess phosphorus tend to suppress the transformation of vitamin D into calcitriol, one of the routes by which the body maintains calcium levels. This is one reason why the normal regulatory actions set in effect by parathyroid hormone to combat lowered calcium concentration involve upping the urinary loss of phosphorus [2]
-Calcium and phosphorus cycle between different parts of the body as needed -a transformation from bone to fluid and tissue and back again that is regulated by hormones [2].
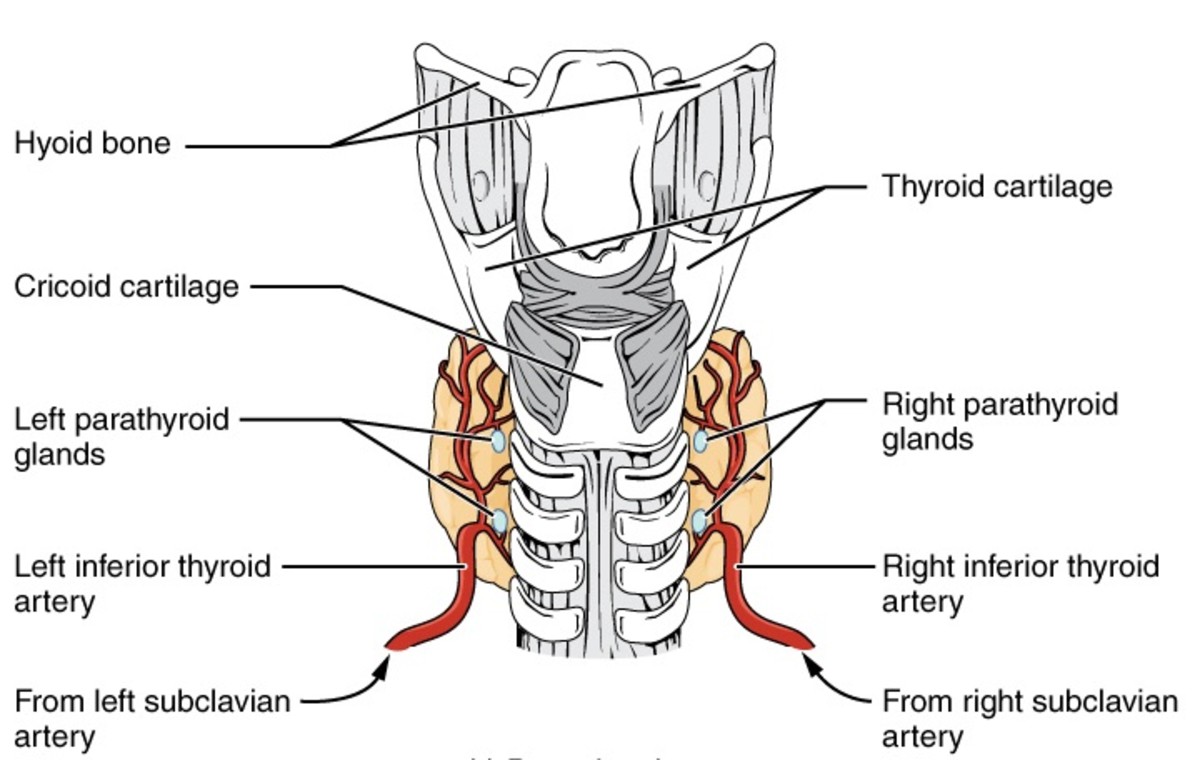
-A decrease in blood-calcium concentrations (registered by the parathyroid glands) provokes a release of parathyroid hormone, which then changes vitamin D in the kidneys into calcitriol [2]. This enhances calcium absorption in the small intestine, whereby dietary calcium and phosphorus are taken in by the body; collaborating with parathyroid hormone, this stimulates special cells called osteoclasts that transfer calcium and phosphorus from the skeletal reservoir into the body. Parathyroid hormone also suppresses the release of calcium and increases the release of phosphorus in the urine [2]
b)The centre of cellular fluid is dependent on the role of sodium, potassium and chloride ions .Discuss fully the role of Sodium, Potassium and Chloride ions as vital minerals as set out in the text. Particular emphasis should be placed on deficiency and toxicity disorders. How is the concept of functional medicine approached through these minerals?
- To better understand the role of these 3 minerals (electrolytes), it is useful to describe the fluid compartments in the body;
-The extracellular compartment in which cells are bathed makes up approximately 1/3 of the body’s extracellular fluid (ECF) [1]
-The other 2/3 resides inside cells (intracellular fluids or ICF) [1]
- Major solutes in extracellular fluid are Sodium and Chloride [1]
- Potassium is the major component of the ICF [1]
→Percentage of fluid constituents may change somewhat in various tissue types due to varying water concentrations
→the differences represent important factors in regulatory and homeostaticmechanisms which includes muscle contractions and nerve impulses [1]
- Upper small intestine = site of greatest absorption for these electrolytes [1]
- Kidneys eliminate the electrolytes and balance is maintained through regulatory mechanisms [1]
- Renal disease may interfere with renal elimination of the electrolytes [1]
- Diarrhoea, excessive vomiting, Addison’s disease (lack of mineral corticoids from adrenal glands) may result in excess loss of electrolytes and hypotension and if severe may cause shock or even death
Hormones that influence balance of sodium, chloride and water include:
-renin-angiotensin-aldosterone axis
-vasopressin etc
- The autonomic nervous system (sympathetic branch) also helps regulate sodium and chloride by altering blood flow through the kidneys [1]
→release rennin from juxtaglomerular apparatus or directly stimulate receptors in the renal tubules
- Renal mechanisms also help control sodium and chloride
Potassium [1]
-primarily exist in ICF
(an increase or decrease in ECF potassium concentration may be due to increase or decrease in potassium intake or potassium excretion from the kidneys)
-passes across cellular membrane quite easily (easier than sodium)
-potassium supplements shown to have blood pressure lowering effect
-participates in nerve transmission, muscle contractions, glycogen and glucose metabolism and maintenance of cellular integrity
-Potassium deficiencies result in:
*Changes in the nervous system
*Muscle weakness
*Bradycardia
*Bone fragility
*Death
[Causes include: Diarrhoea/Vomiting, Renal disease, Aging, Starvation, Burns and some diuretics, dehydration, Magnesium deficiency, Diabetes which causes loss of both potassium and sodium through increased urinary flow]
Sodium [1]
-plays important roles in transport of carbon dioxide, muscle contraction, nerve transmission and amino acid transport
-Deficiency rarely occurs
-Causes of deficiency: Starvation, vomiting, diarrhoea may cause decreased sodium in ECF causing water to pass into cell
→leads to water toxicity (symptoms include appetite loss, muscle twitching and apathy)
[if both sodium and water are lost in these situations, ECF fluids diminish and low blood volume results, muscles can cramp and veins may collapse [1]
Chloride
-Deficiency causes vomiting or diarrhoea
→acid bases disturbances
Functional Medicine Considerations [1]
- Potassium excess or deficiency can result from prolonged ingestion of standard American diet
- A history of renal problems or a recent history of excessive diarrhoea or vomiting should prompt clinicians to investigate electrolyte status (especially if hypotension, muscle weakness or heart disturbances are identified)
- Also consider sodium/potassium ratios in presence of hypertension
- If magnesium deficiency has been determined especially in diabetes cases (due to increased urine flow), potassium status should be determined as it may also be deficient as a result
c)Role of Chromium in control of blood sugar (GTF)
- A major component in glucose tolerance factor (GTF) along with Vitamin B3 and amino acids (glycine, glutamic acid and cysteine)
- Chromium through GTF has a strong insulin-enhancing activity
- May help bind insulin to its receptors in the cellular membrane
- May have an effect on lipid metabolism too (increase HDL in some studies)
- Improve immune response as it may decrease serum cortisol and increase immunoglobulins
Importance of detailed clinical history in diagnosis of sugar related disorders
- When taking patient history and determining the cause of symptoms typical of decreased insulin sensitivity, we should examine the possibility of chromium insufficiency [1]
- Other components of GTF may also be insufficient thus all components need to be included in therapeutic intervention [1]
di)Iodine Functions:
- Body uses iodine primarily as a component of thyroid hormones (thyroxine3,5,3’,5’ tetraiodothyronine T4 and 3,5,3’ triiodothyronine T3) [1]
- Thyroid hormones are needed to increase cellular reactions including Oxygen consumption and basal metabolic rate to influence growth and differentiation [1]. Hence iodine plays a major role.
- Selenium is required in the deiodinase enzyme to convert T4 to T3 in the liver [1]. Thus selenium deficiency can cause thyroid enlargement
- Thyroperoxidase needs iron for its activity hence without enough iron, thyroid metabolism is impaired [1]
Iodine absorption:
- Organic iodine substances are degraded in the gut to inorganic iodide which is quickly and efficiently absorbed [1]
>Blood absorbs free iodide and the kidneys and thyroid rapidly pick up this free form
- Uptake by the thyroid depends on previous iodine intake; if iodine has been deficient, as much as 80% of the available amount will be taken up by the thyroid [1]
- Use of available iodine in synthesis of thyroid hormones is governed by negative feedback loop involving pituitary gland and its product, TSH (thyroid stimulating hormone) and the hypothalamus and its product, thyroid-releasing hormone TRH [1]
Iodine Safety and Toxicity
- High levels of dietary iodine intake have resulted in acne-like skin lesions in some reports [1]
- May inhibit thyroid hormone secretions [1]
Iodine deficiency symptoms [1]:
- Goiters may result (due to enlargement of thyroid through hypertrophy and/or hyperplasia); goiters have also been caused by excessive consumption of cabbage, rutabagas, cauliflower and soybeans all of which have substances that may interfere with the iodine used by the thyroid [1]
- Hypothyroidism
- Severe iodine deficiency in an infant can result in cretinism, growth retardation and even mortality [1]
- May result in decreased immune function of neutrophils (because iodine works with neutrophil peroxidases in bactericidal activity) [1]
Iodine requirements [1; page 154]:
- Infants (1-12 month old): 110-130mcg/d (Adequate intake or AI); Upper Limit N/A
- Children (1-18 years old): 90mcg/day (RDA); Upper Limit: 200-300mcg/d
- Children (9-13 years old): 120mcg/d (RDA); Upper Limit: 620mcg/d
- Adolescents (14-18 year old): 150mcg/d; Upper Limit 900mcg/d
- Adults (>19 years old): 150mcg/d; Upper Limit 1100mcg/d
- Pregnancy (less than or equals to 18 year old): 220mcg/d; Upper Limit: 900mcg/d
- Pregnancy (>18 year old):220mcg/d; Upper Limit: 1100mcg/d
- Lactation (less than or equals to 18 year old): 290mcg/d; Upper Limit: 900mcg/d
- Lactation (>18 year old): 290mcg/d; Upper Limit: 1100mcg/d
Symptoms of low thyroid function:
- Fatigue
- Constipation
- Depression
- Dry Skin
- Weight gain
- Cold intolerance
*While iodine deficiency may not necessarily be the cause of hypothyroidism, it should be explored especially in light of dietary considerations [1]
*a history of recurrent bacterial infections may be the presenting symptom and poor iodine status should be ruled out if other symptoms lead to suspicion of iodine deficiency [1]
Iron functions
- Iron containing compounds may be either directly functional or useful in transport and storage [1]
- The functional compounds have metabolic or enzymatic function in the body (2/3 of total body iron is used in this category; large percentage of this amount is in the form of haemoglobin as iron is required for the structure of the heme portion of hemoglobin) [1]
- Primarily used as part of haemoglobin and myoglobin which carry and release Oxygen in tissue [1]
- Cellular activities
- Enzymes in Kreb’s Cycle require iron
- Helps maintain normal immune function and collagen synthesis [1]
- While bacteria may sequester iron from human iron stores, oral iron supplementation does not increase risk of infection [1]
Iron Absorption
- Absorption occurs primarily in the duodenum by an active process that moves it into blood [1]
- Transferrin (one of the transport/storage compounds) carries iron to cells and the bone marrow [1]
- Absorption is increased when needed and decreased when erythropoiesis is increased
- Excess iron is stored (not excreted) as ferritin and hemosiderin as main storage compounds [1]
- Iron absorption may be inhibited by phytic acid, polyphenolic compounds, calcium and partially digested proteins [1]
- Iron absorption is increased with Ascorbic acid, Cysteine and eating meat during the meal [1]
Iron-Safety and Toxicity [1]
- Iron is not easily excreted and excess iron can build up
- Excess intake (diet or from supplements) can lead to hemosiderosis (condition where transferrin is saturated and iron is deposited in soft tissue)
- A more severe condition of iron deposition in soft tissue is hemochromatosis; alcoholism may put one at risk for his condition [1]
- Excess iron may be linked with increased free radical production and increased risk of cancer and heart disease. Increase in free radicals may also worsen joint inflammation and cause degradation in rheumatoid arthritis [1]
Iron deficiency
- Decreased anatomical development of immune tissue
- Reduction in antibody and interleukin synthesis
- Decreased protein synthesis
- Reduce Granulocyte phagocytosis
- Severe anaemia
- Decreased energy levels
- Decreased immune function
- Learning disabilities
- Deficiency symptoms include: fatigue, lack of energy, shortness of breath or chronic infection
- Causes must be explored for the above symptoms and patient history must be checked for frank or occult bleeding, vegetarian diet, malabsorption or hypochlorhydia [1]
Iron requirements (all are in RDA unless otherwise mentioned)
- Infants (0-6 months old): 0.27mg/d (Adequate intake or AI); Upper Limit 40mg/d
- Infants (7-12 months) : 11mg/d; Upper Limit: 40mg/d
- Children (1-3 years old): 7mg/day; Upper Limit: 40mg/d
- Children (4-8 years old): 10mg/d ; Upper Limit: 40mg/d
- Children (9-13 year old) : 8mg/d; Upper Limit: 40mg/d
- Males (14-18 year old): 11mg/d; Upper Limit 45mg/d
- Males (>19 years old): 8mg/d; Upper Limit 45mg/d
- Females (14-18 year old): 15mg/d; Upper Limit 45mg/d
- Females (19-50 years old): 18mg/d; Upper Limit 45mg/d
- Females (>50 years old): 8mg/d (Adequate Intake or AI); Upper Limit 45mg/d
- Pregnancy: 27mg/d; Upper Limit: 45mg/d
- Lactation (less than or equals to 18 year old): 10mg/d; Upper Limit: 45mg/d
- Lactation (>18 year old): 9mg/d; Upper Limit: 45mg/d
dii)Two deficiency disorders for both Iron and Iodine and Design and Explain nutrient modifications appropriate for client/patient
[Note for the following, doses are provided for Adults]
Deficiency Disorders for Iron include Anaemia and Decreased Immune function
(1) Anaemia
- Caused by a reduction in either the number of red blood cells or the amount of haemoglobin in the blood [3]
- Is sometimes the first detectable of arthritis, infection or certain major illnesses including cancer [3]
- Drug use, hormonal disorders, chronic inflammation in the body, surgery, infections, peptic ulcers, haemorrhoids, diverticular disease, heavy menstrual bleeding, repeated pregnancies, liver damage, thyroid disorders, rheumatoid arthritis, bone marrow disease and dietary deficiencies (especially in iron, folic acid, Vitamins B6 and B12) can all lead to anaemia [3]
- Postmenopausal Women should not be anaemic unless they are vegetarian; this can be a sign that warrants further investigation [3]
- Anaemia’s symptoms can easily go unrecognized. The first signs of anaemia include loss of appetite, constipation, headaches, irritability or difficulty in concentrating [3]
- Established anaemia can produce these symptoms: weakness, fatigue, coldness of the extremities, depression, dizziness, overall pallor which is most noticeable in pale and brittle nails, pale lips and eyelids, soreness in the mouth and in women; cessation of menstruation [3]
- Anaemia has also been linked with loss of libido [3]
- Nutrient Modifications and Recommendations for Deficiency in Iron [3; pages 201-203]:
- Iron supplementation is essential (Ferrous gluconate in doses as prescribed by physician with 100mgVitamin C to enhance absorption)/Floradix Iron plus herbs/Raw liver extract 500mg twice daily
- Very important nutrients:
- Blackstrap molasses 1tbsp twice daily for adults; 1 tsp added to milk for children and infants
- Folic acid 800mcg twice daily plus biotin 300mcg twice daily
- Vitamin B12 injections 2cc once weekly or Vitamin B12 2000mcg three times daily
- Helpful nutrients: Vitamin B complex 50mg of each major B vitamin three times daily plus extra panthothenic acid (50mg three times daily) and Vitamin B6 (100mg daily) and Vitamin C plus bioflavonoids (3000-10,000mg/day)
Deficiency disorders of Iodine include Hypothyroidism and Goitre
(1) Hypothyroidism
- Caused by underproduction of thyroid hormone
- Symptoms include chronic fatigue, appetite loss, cold intolerance, low body temperature and slow heart rate, easy weight gain, elevated cholesterol, painful premenstrual periods, heavy periods, a milky discharge from the breasts, fertility problems, muscle weakness, muscle cramps, dry and scaly skin, a yellow-orange discolouration of the skin (especially on the palms of the hands), yellow bumps on the eyelids, hair loss(including the eyebrows)
- A miniscule drop in thyroid function registers as a distinctly elevated TSH
- Nutrient Modifications and Supplementations for Hypothyroidism and Goitre
- Avoid or minimise goitrogenic foods such as cruciferous vegetables and soy , Babassu (a palm-tree coconut fruit found in Brazil and Africa), African cassava [4]
- Essential nutrients:
- Kelp : 2000-3000mg/day
- L-tyrosine: 500mg twice daily on an empty stomach. Take with water or juice (not milk); Take with 50mg Vitamin B6 and 100mg Vitamin C for better absorption
- Very important nutrients:
- Multi-glandular from American Biologics as prescribed
- Raw thyroid glandular as prescribed
- Important nutrients:
(2) Vitamin B complex : 100mg of each major B vitamin three times daily with food plus extra Vitamin B2 50mg twice daily and Vitamin B12 1000-2000mcg three times daily on an empty stomach
e)Zinc deficiency symptoms
- Skin changes
- Hair loss
- Recurrent infections
- Diarrhoea
- Sleep disturbances
- Slow wound healing
- Dandruff
- Rheumatoid arthritis
- Reduced appetite
- Inflammatory bowel disease
- Minor skin disorders (e.g. acne or psoriasis)
Factors that affect Zinc Absorption
While Zinc may be high in whole grains, legumes and nuts, it is not absorbable from these sources due to the binding with phytic acid [1].
- Zinc is primarily absorbed in the upper small intestine and so it plays a key role in controlling the amount of Zinc absorbed based on previous absorption [1]
- Inorganic Iron in diet and Calcium supplements may decrease Zinc absorption
- Alcohol, infection, surgery and other physiologic factors may alter absorption of zinc too.
- Cytokines (especially interleukins 1 and 6) increases Zinc uptake by liver and thus affects zinc metabolism [1]
- Fecal Zinc excretion helps maintain homeostatic levels [1]
REFERENCES
1) DeAnnLiska, Sheila Quinn, Dan Lukaczer et al.Clinical Nutrition-A Functional Approach, 2004, The Institute of Functional Medicine, a Nonprofit educational organization
2) Schowalter-Hay E. , Relationship between calcium and phosphorus, Sep 2011; http://www.livestrong.com/article/529574-relationship-between-calcium-phosphorus/#ixzz2WeqV2mFO; Accessed 20th June 2013
3) Phyllis A. Balch, Prescription for Nutritional Healing 2010, Avery New York
4) Mary Shomon, All about Goitrogens, June 2012; http://thyroid.about.com/od/symptomsrisks/a/All-About-Goitrogens-thyroid.htm; Accessed 21st June 2013