Sciatica - A Natural Approach
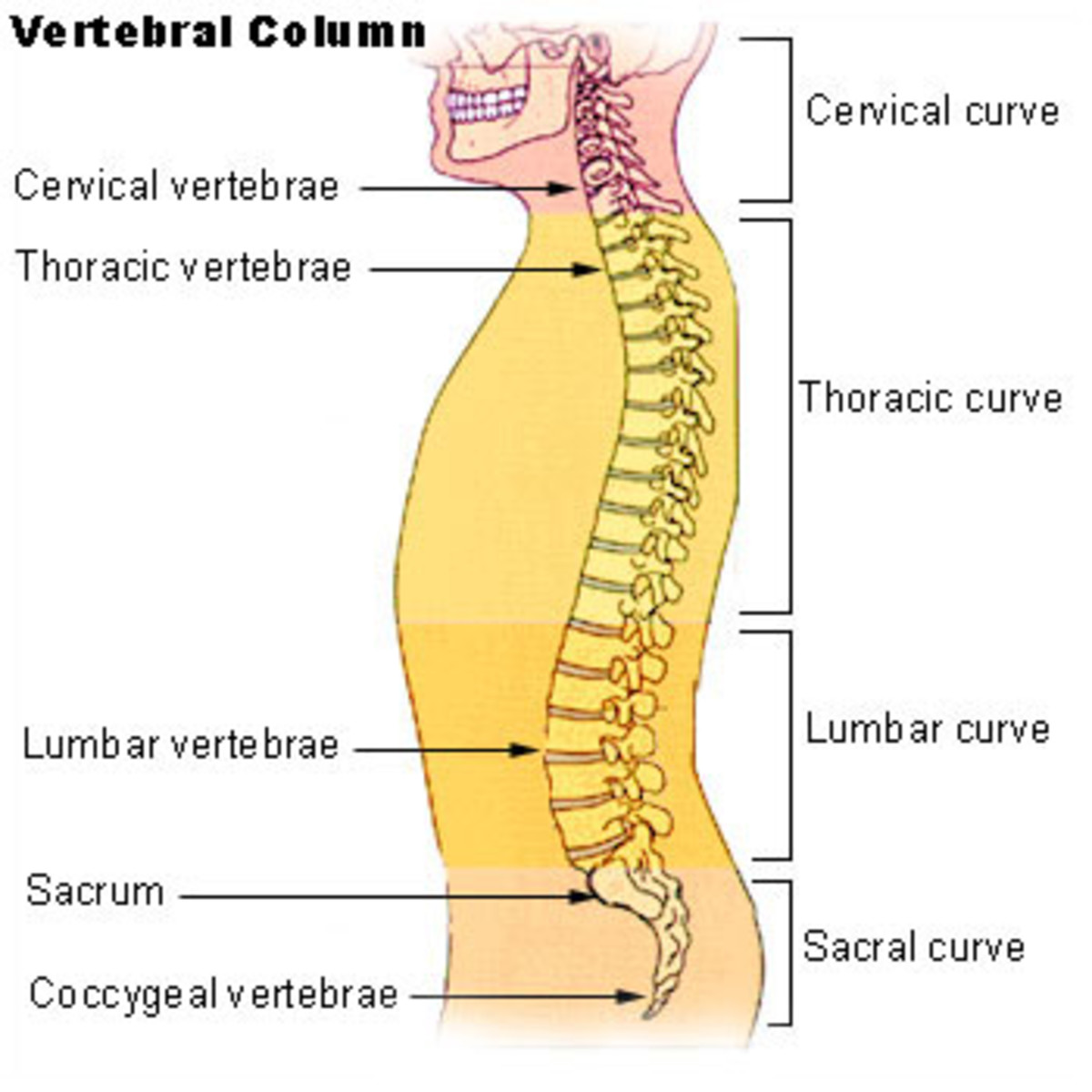
Sciatic Nerve Anatomy
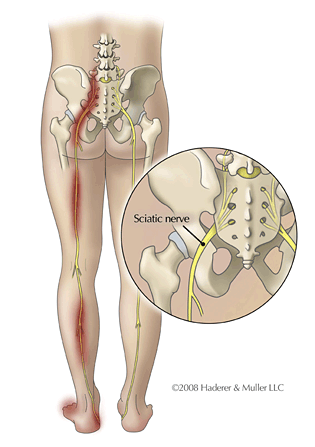
Sciatica - Symptoms and Causes
The symptoms of sciatica are shooting pains in the legs and/or feet, often severe and changed in severity by a change of position; for example, getting up out of a chair. The symptoms of brachial neuralgia are quite similar, except that the problem is in the arms and hands instead of legs and feet. Often, sciatica and brachial neuralgia are associated with loss of muscle strength and mobility in the affected area as well; also muscle spasms can occur.
Both problems are rather close in terms of symptoms to other disorders such as various forms of arthritis. In the case of brachial neuralgia, it might be confused with the symptoms of various forms of heart disease, which often include pain radiating to an arm (usually the left) sometimes without any associated chest pain. Various forms of neuropathy, such as for example the neuropathy associated with diabetes, can have similar symptoms as well.
For this and various other reasons, if you suspect you might have sciatica or brachial neuralgia then you need to see a doctor (at least initially) to rule out these other problems some of which are potentially life-threatening; also so that you know for sure that natural methods (some of which are set out here) that you are about to use are appropriate ones for the problem you actually have.
From here on I will refer to sciatica and assume that brachial neuralgia is included in the discussion; the basic reasons for both and the steps taken to relieve the problem are virtually identical (except for location in some cases) in any event.
Sciatica is caused by irritation and/or pinching of the spinal nerves leading to the affected area. This leads to the rather counter-intuitive conclusion that sciatica, which presents itself as pain in the legs, is not actually a leg problem at all but a problem in the spine - usually in the lumbar region in the case of sciatica itself and the cervical (neck) region in the case of brachial neuralgia.
This rather bizarre state of affairs occurs because the brain interprets signals coming from the appropriate sensory nerves as coming from the area they serve; the brain has no way of knowing, so to speak, that the signals are actually being generated in a completely different place. It’s a little like someone tapping into a phone line and shouting into an attached phone when you are talking to someone else.
The loss of mobility and muscle strength sometimes connected with sciatica has a very similar cause. The pinching of the nerves that leads to the pain can also lead to interruption of the outgoing signals going along the motor nerves leading to the affected area; this means that the muscles are never “told” to move in the first place. The muscle spasms sometimes associated with sciatica occur because a spurious signal is generated by the irritation, and the muscles interpret it as a command from the brain; the muscles have no way of “knowing” that isn’t the case.
The irritation and/or pinching of the spinal nerves are usually caused by a chronic problem of the structure of the spinal column itself. The spine is composed of a number of vertebrae (33 in humans, of which 9 are fused into the sacrum and coccyx at the bottom end of the spine) which are hollow bones varying in size and shape from top to bottom. The lumbar vertebrae in the lower back are the largest, the cervical in the neck the smallest. Each vertebra has a central channel (to allow for the passage of the spinal cord) and various projections that allow for the attachment of various other structures; which other structures depends on which vertebra. The vertebrae are locked in place, with a certain amount of mobility, by a network of strong tendons pulling them together and by the spinal discs pushing them apart.
Several things can go wrong with this arrangement, leading to something (either the discs or the vertebrae themselves) pressing on the spinal cord and causing irritation. The problem, broadly, can be with the supporting tendons; the discs; or the actual vertebrae themselves.
First, the tendons. Back injury can lead to one or more of the tendons supporting the spine being either ruptured or weakened. If a tendon is ruptured, there is really no recourse except surgery - although less drastic and/or natural methods can give some relief. If it’s weakened, then the affected tendon may well heal by itself or, more likely, with some help.
Second, the discs. The inter-vertebral discs are, to simplify matters greatly, a fibrous bag (made of the same sort of material that forms joint capsules and tendons) full of jelly. The gelatinous material is made mostly of polymers of glucosamine and other amino sugars, and the disc is under a fair amount of internal pressure - making it semi-rigid in for the same reason that an inflated balloon is somewhat rigid. This rigidity means that the vertebrae can move a little, and this is why you can usually bend your back; however, the movement is limited. Several things can go wrong with this arrangement. One is that if put under extreme stress, such as lifting a weight heavier than you are accustomed to or in an awkward position, the disc can rupture and the jelly inside protrudes. If you are unlucky, the gelatinous mass goes inwards and presses on the spinal cord. This is basically what happens in what is normally called a slipped disc, although the term is inaccurate.
The second thing that can go wrong with this is for the discs to gradually deflate. This happens precisely because the jelly inside is made of glucosamine polymers. Normally, the body can make its own glucosamine, but with advancing age the production of glucosamine (like everything else!) becomes less efficient and at some point may become inadequate for the needs of the body. This leads to loss of internal pressure in the disc, which becomes less rigid as a consequence.
A deflated disc may bulge inwards leading to problems similar to those which occur when one ruptures, or it may make the spine in the area less rigid and allow the vertebrae to contact the spinal cord. This leads me to the third class of problem, one with the vertebrae themselves.
Third, the vertebrae themselves. The vertebrae can slip out of place because the tendons supporting the spine are weak, or because the discs aren’t doing their job properly (as above). It is also possible to have problems with the vertebrae themselves. Two possible problems are “crumbling” vertebrae (usually associated with osteoporosis, which has consequences elsewhere) and spondylosis. Although that term is often used to cover many types of spinal degeneration, the problem I will cover here is one in which the vertebrae themselves have become deformed. This is more specifically called spinal stenosis.
First, the problem caused by crumbling vertebrae. In the case of osteoporosis, which is fairly common in late middle aged and elderly people and more particularly women of that age group, the vertebrae actually start losing their shape. In extreme cases, bits can break off the vertebrae and it is largely a matter of luck where the bits end up. If they end up pressing on the spinal cord, that can cause sciatica and similar problems. More commonly, the vertebrae become compressed and when that happens the vertebrae affected may press on the spinal cord.
Spinal stenosis can appear as a general narrowing of the canal through the middle of one or more vertebrae, leading to pressure on the spinal cord. Probably just about as often, the vertebrae become deformed by the growth of abnormally-placed spurs. This can happen elsewhere, such as in the heel, leading to the problem known as a heel spur. This sort of spur of bone, although it is very poor quality bone without much strength, is easily capable of irritating soft tissue - such as the spinal cord.
Conventional and Natural Treatments for Sciatica
Conventional treatments for sciatica and similar problems vary greatly, and some are much more drastic than others. The first remedy tried is usually anti-inflammatories and painkillers; sciatica pain can be quite severe and thus require heavy-duty painkillers such as opiates - which themselves vary greatly in strength.
Sometimes, particularly for problems with the cervical spine, traction is used. This is essentially the application of a pulling force to the spine - usually using weights attached to some sort of harness. This sometimes works, because the removal of the normal downward pressure on the spine allows the affected vertebrae to click back into place. Other manipulative therapies normally associated with physiotherapy are sometimes used, too.
Last resort treatment for sciatica and similar problems is usually surgery. This is aimed at removing the irritating agent (part of a ruptured disc or bony lumps) or sometimes a procedure is used that fuses two or more vertebrae together to stabilise the spine. This sort of surgery has a rather long recovery period, and can in some cases be quite risky; after all, the area involved is within millimetres of the spinal cord.
Natural treatments can be quite similar to conventional ones; natural anti-inflammatories and manipulative therapy (usually from an osteopath or chiropractor) are sometimes used. Common natural anti-inflammatories include Boswellia serrata and ginger.
However, complementary therapies for sciatica usually attack the whole problem differently. One type of treatment rather straddles the division between conventional and “alternative” treatments; this is the treatment (actually a palliative one aimed at the symptoms) called transcutaneous electrical nerve stimulation. This mouthful is usually abbreviated to TENS.
TENS involves the application of a low-strength pulsed electric current across an affected nerve. For sciatica, this would mean the application of the electrodes to the lower back. Placement of the electrodes is crucial; get the position wrong and the treatment may not work at all. However, this does no harm so a “hit and miss” approach will usually work - eventually.
TENS works because the electric current disrupts the propagation of signals along the pain nerves. No signal, no pain. These days (2012, as I am writing) TENS units are quite small (pack of cards or smaller) and can be quite cheap. They are also cheap to use; electrodes need replacing on occasion and you need some new batteries every now and then, and that’s about it.
Two other complementary therapies for sciatica are glucosamine and boron, the latter usually used with small amounts of calcium and magnesium as supplements. Glucosamine supplementation is aimed at increasing the body’s supply of amino sugars; in turn, this means that the pressure inside the discs may return to near normal and reduce any abnormal movability of the spine - and also reduce any bulging inwards of the discs themselves. This treatment works very well with osteopathy to put the vertebrae back into place.
Boron is a newly discovered nutrient (found to be essential in the late 1990s) which appears to have an influence on the metabolism of steroid hormones, particularly vitamin D and oestrogen. It is often used by natural practitioners for osteoporosis, and can also be used for virtually any disorder that involves abnormal calcium deposits; this includes chronic tendonitis and bursitis, but also any problem involving the formation of bone spurs or other types of abnormal bone growth. These include spinal stenosis and also heel spurs.