Somatoform Disorders
Soma literally means the "body." Somatoform disorders are psychological problems that manifest themselves in physical form. They are bodily symptoms (including physical illness or injury) that do not have any physical or medical cause.
People with somatoform disorder are preoccupied with their health and often experience extreme distress and worry over their symptoms. They have recurrent somatic complaints that continue for years and are often debilitating enough to impair normal, every day functioning.
The individual suffering from somatoform disorders has no voluntary control over them. Thus, somatoform disorders are not intentionally or consciously produced by the person.
Medical test results or physical examinations do not explain the symptoms of somatoform disorders. People suffering from this disorder spend a lot of money, time and expenditure trying to find a medical treatment for their problems and frequently change doctors in the process. Often, it leads to exasperation and confusion when any of the doctors fail to give a medical reason for their symptoms.
There is very little systematic research into the causes of somatoform disorders. Psychodynamic theories emphasise the role of unconscious motivations while Cognitive behavioural models stress the different cognitive beliefs that lead to negative responses to bodily sensations.

Types Of Somatoform Disorders:
Following are some of the different types of somatoform disorders:
- Pain Disorder
- Body Dysmorphic Disorder
- Somatization Disorder
- Hypochondriasis
- Conversion Disorder
Related disorders:
- Malingering
- Factitious Disorder

Pain Disorder:
According to DSM-IV-TR (Diagnostic and Statistical Manual of Mental Disorders), the criteria for pain disorder is enough pain to warrant clinical attention. In pain disorder, the psychological factors are very important to the onset, maintenance and severity of physical pain.
Individuals with pain disorder experience the pain as a physical symptom without consciously or intentionally producing or faking it. The pain causes significant distress to impair normal functioning. It may begin to intensify after stress or conflict.
There is no other psychological condition to explain the pain experienced in pain disorder. Nor is it easy to measure it, unlike localised pain caused by a specific physical problem. For this reason, traditional medication rarely helps to cure pain disorder.

Body Dysmorphic Disorder:
DSM IV-TR criteria for Body Dysmorphic disorder is preoccupation with an imagined defect or excessive concern over a slight defect in one's appearance.
There is no other psychological disorder that explains this preoccupation.
Individuals with body dysmorphic disorder may appear attractive to others, but they see themselves as ugly or even hideous. They may spend hours examining their 'flaws' in the mirror or completely avoid looking at themselves.
Some patients with the disorder stop going out or socialising, while others go to long lengths to hide themselves or their imagined defects.

The distress experienced by people suffering from this disorder is significant enough to drive them to cosmetic surgery or even suicide. The results of surgery are often disappointing and do little to alleviate the distress.
Most individuals with body dysmorphic disorder meet the diagnosis criteria for another disorder, the most common of them being Major depressive disorder, Social Phobia or substance abuse.
Research shows that Body Dysmorphic Disorder is slightly more common among women than men (Otto et al., 2001). Moreover, social and cultural factors play a major role in how people view their appearances.
Somatization Disorder:
Somatization Disorder was previously known as Briquet's syndrome. According to DSM-IV-TR, the criteria for somatization disorder is a history of seeking treatment for many physical complaints beginning before the age of 30 and lasting for several years.
For a diagnosis of somatization disorder, the individual must have several different kinds of recurrent physical symptoms which cause impairment and distress. Symptoms are usually pain symptoms, with at least one sexual symptom, one pseudo-neurological symptom and two gastrointestinal symptoms.
- Somatization disorder is rare.
- It is more common among women than men.
- Occurs in 2% of women & 0.2% of men
Usually the symptoms are spread out over the course of the disorder, though they may occur simultaneously.
People with somatization disorder seek frequent treatment even though there is no apparent physical explanation for their symptoms. Hospitalization and surgery is common.
Somatization disorder is chronic and unless treated properly, may never go away. This also puts immense pressure on the close family and caregivers of the individual suffering from the disorder.
Hypochondrias:
Hypochondrias or hypochondria is also known as Health anxiety or Health Phobia.The criteria for a diagnosis of hypochondrias according to DSM IV-TR is a preoccupation with fears about having a serious disease, with symptoms lasting at least 6 months.
Signs Of Hypochondria:
- Fear or anxiety about undiagnosed disease
- Every sensation or symptom causes worry
- Frequent doctor visits
- Repeated self-examinations - checking vital signs
- Switching doctors
- Obsessive health research: books, medical journals, online
- Mental and emotional distress over one's health
There is no actual medical reason for this excessive worry but individuals with hypochondria become completely preoccupied with their bodies, self-examinations and self-diagnosis.
The slightest physical symptoms gives them cause for alarm or extreme distress. Individuals constantly obsess over every lump, sore, bruise or minor ailments and believe them to be the cause of some deadly disease.
Hypochondriacs often seek repeated assurances from doctors, family or friends. They usually view their physicians as incompetent and frequently switch doctors. They are dissatisfied with their diagnosis and often unconvinced or shocked when informed about the absence of a medical condition.
People suffering from hypochondria may also experience rise in blood pressure, stress and anxiety levels at the mention of doctors or within a medical environment.
Some individuals may completely avoid any mention of illness or refuse to speak about their extreme fears. Others constantly visit doctors and their conversations too revolve around their perceived illnesses.
Hypochondria typically begins in early adulthood and has a tendency to be chronic. It is not explained by any other disorder like delusional disorder or body dysmorphic disorder.

Conversion Disorder:
Conversion Disorder has a long history and was originally known as Hysteria.
DSM IV-TR criteria for Conversion Disorder is one or more symptoms affecting motor or sensory functioning and suggesting a medical or neurological condition. However, medical tests indicate that there is no organic cause for them i.e. bodily organs and the nervous system is fine.
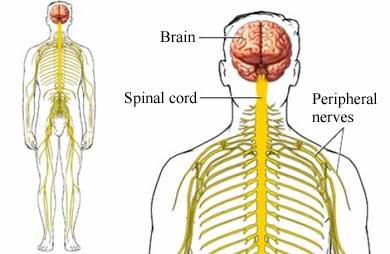
Neurological symptoms include numbness, stroke, partial or complete paralysis of arms and legs, fits, seizures, movement and coordination disturbances. There may be sudden loss of vision, partial or complete blindness or tunnel vision.
Prickling sensations, tingling of the skin or a loss of sensation is also common. There may also be a loss of voice (whispered speech) or loss of sense of smell.
The symptoms of conversion disorder are related to conflict or stress and can cause significant distress. Symptoms are enough to impair normal functioning or warrant medical evaluation.
As with most somatoform disorders, the individual does not intentionally produce or fake the symptoms. Conversion disorder usually develops in adolescence or early adulthood. Stress plays a major role in it's development.

Malingering:
DSM IV-TR classifies Malingering as 'other conditions that may be a focus of clinical attention.' Unlike the other Somatoform disorders, Malingering refers to an intentional faking of physical incapacity in order to avoid responsibility. In this way, it is related to somatoform disorders as the person has symptoms that have no physical or organic basis.
Factitious Disorder:
Factitious disorder is also related to Somatoform disorders, although it is listed in a category of its own in DSM-IV-TR. People with Factitious disorder intentionally produce physical or psychological symptoms in order to assume the role of a patient. Individuals with this disorder fake symptoms, report acute pain and may even inflict injuries on themselves.
Overview Of Somatoform Disorder:
There is little research available on the causes of somatoform disorders, which makes it often difficult to diagnose and treat them.
One of the complications with the treatment of Somatoform disorders is that people suffering from them rarely consult a psychologist or a therapist.
However, Cognitive behavioural therapy has been found to be effective for treating somatoform disorders, particularly Pain disorder and Body Dysmorphic disorder. Anti-depressents have also proved to be helpful, though these only treat the symptoms, not cure them.








