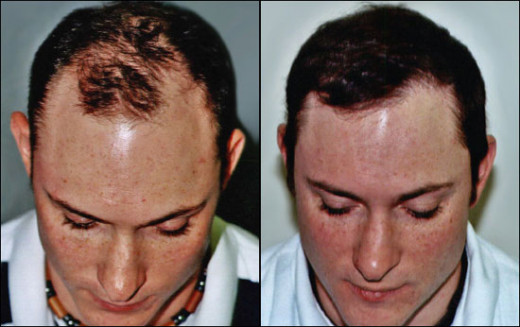
Surgical treatments for hair loss with live hair follicles

What It Is
Three treatment philosophies: There are three treatment philosophies for using surgery for treating hair loss. This hub describes treatments that involve surgical redistribution of one's own live hair follicles for a look of having more hair. Artificial hair implants, and using surgery for hairpiece attachment are described in my other hubs.
Live follicle movement: The most popular surgical philosophy for hair loss treatment is to move live hair follicles that are genetically programmed to continue growing hairs over a lifetime, to new locations where the hairs they grow will have greater visual impact. The new hairs continue to grow just like other hairs on the head, and require no special care or maintenance - just periodic haircuts!
Donor dominance: Hair follicles on the back and sides of the head are the ones selected as donor follicles. They may be moved as grafts, or by repositioning the scalp that contains these follicles. At the new location, these follicles will continue to grow new hairs over a person's lifetime because their genetic program is dominant over environmental characteristics, such as reduced circulation or excessive scalp oil, that may be present at the new location.
No new hair: Despite the amount of hair a particular person may have at the time of surgery, hair restoration surgeons choose to select donor hair follicles only from certain "permanent hair" areas of the scalp, as other follicles are likely to be genetically programmed to stop producing new hairs 10, 20, or 30 years later. No new hair is added. As a result, there are always a limited quantity of donor hair follicles to work with, typically representing about 25% of the hair on a person's scalp, before the hair started thinning.
Illusion of more hair: Hair restoration surgeons must redistribute the limited donor hair follicles in such a way that the hairs they produce give the illusion of having a full head of hair. With a combination of surgical skill and artistic talent, hair restoration surgeons accomplish this goal. Surgical hair restoration procedures that move live hair follicles include hair transplants, bald scalp reductions, and extensive surgical procedures such as scalp lifts and transpositional flaps. Often a treatment program will include two or more different procedures.
Benefits
Permanent: The main benefit of surgical procedures that move live hair follicles is that the "new" hair is the person's own living and growing hair. The results are permanent. Once the surgical procedure (or procedures) are accomplished, the patient can go on with their life and generally not think about hair loss any more.
Natural look: Modern hair restoration surgery techniques allow for dramatically better results today than in the recent past. The results achievable today are even more natural looking, and can be accomplished with less donor material than was the case just a decade ago. Furthermore, the hair looks and feels natural because it is natural, and there are no adhesives, lotions, or sprays to apply.
Confidence: With surgical hair restoration procedures there is nothing to put on and nothing to fall off. Hair restoration surgery patients have confidence. Rather than feeling embarrassment, many become quite proud of how their own relocated hair follicles grow their "new" hair.
Economical: A surprising benefit of hair restoration surgery is that it is often quite economical over a lifetime. After a high initial investment, there is no continuing cost for materials or special maintenance. When the initial cost of surgery is spread out over the patient's remaining life span, surgery can be considered quite economical.

Risks
Expensive: Hair restoration surgical procedures are expensive initially, typically costing several hundred to several thousand dollars or more per procedure. Typically, several procedures are required for convincing results. Unless an accident requires surgical restoration, this type of elective surgery is not covered by insurance. And although almost all hair restoration surgeons accept credit cards and offer financing options, surgery requires a considerable initial investment .
Fear of surgery: There is a general fear of surgeries, including hair restoration procedures. Before surgery, tranquilizers may be given by mouth to ease a patient's anxiety. Most surgical hair restoration surgery is accomplished with local anesthetic medication, meaning that only a portion of the body is numbed, and the patient is awake during the procedure. Medication that induces temporary amnesia may also be administered, to diminish memories about the surgery itself.
Pain: There is the disadvantage of actual discomfort and pain after surgery (analgesic medications are used to eliminate pain during surgery). Hair restoration surgical procedures involve varying degrees of tissue cutting, which creates tissue swelling and discomfort after surgery. Medications are prescribed for use after surgery to minimize swelling and pain, however even with medication, some people will still experience discomfort during the healing period.
Unnatural appearance: Hair restoration surgical procedures typically result in an unnatural appearance immediately following surgery, although sometimes the change is almost unnoticeable. Bandages, crusts from dried blood, and sometimes visible wounds with sutures can affect the patient's appearance for a few days to two weeks or more after the procedure. Typically bandages are used to cover any surgical incisions until the wounds have substantially healed, although with some procedures bandages are not even necessary. To reduce the unnatural look immediately after surgery, existing hair can be combed to camouflage the incisions, or a hat or hairpiece can be worn temporarily. Some patients simply choose to take a few days off of work, until their scalp has adequately healed.
Poor cosmetic results: Poor cosmetic results are a risk of all surgical treatments for hair loss. The results may not be what the patient expected, or the surgeon may not have accomplished what was desired. Sometimes, after several procedures, the relocation of hair follicles leaves the donor areas noticably thinner. Each of the various surgical treatments make a change in the patient's appearance, and there is a risk that the change will look unnatural. Hair restoration surgical procedures require both adequate surgical skill and a fine sense of aesthetics to achieve convincing results, and especially to achieve a natural look at the hairline and temples. In addition, the plan for the final appearance must be designed to look natural 30, 40, and even 50 years after the surgery.
Additional procedures: Most surgical treatments can safely accomplish only a limited amount of restoration in a single session. Usually a series of procedures are planned, spaced at 3-4 month intervals, to adequately improve the patient's appearance. Also, if hair loss progresses beyond what was anticipated, or if a procedure had a bad design or result, additional procedures may be recommended to correct or improve the patient's appearance.
Limited results: Only limited results are possible with hair restoration surgical procedures, because no new hair is added. Bald areas can be covered, and new hairlines can be constructed, however this is all accomplished by skillfully redistributing the patient's own hair follicles. The goal of surgical treatments that move hair follicles is only to create the illusion of having more hair.
Complications: There are risks of unintended complications relating to any surgery. Hair restoration surgical procedures involve varying degrees of tissue cutting. With some procedures there are risks of blood loss. There is a risk of temporary numbness, and sometimes but rarely, permanent partial loss of sensation on the scalp following surgery.
Permanent hair loss: Hair restoration procedures also include a risk of permanent loss of hair follicles. Some hair follicles will not survive being relocated. Sometimes, the yield will be lower than anticipated. On very rare occasions infections can occur, which if not properly treated can result in the permanent loss of large quantities of hair follicles. Once hair follicles are lost, they are gone forever.
Scars: Hair restoration procedures include a risk of visible scars and other cosmetic complications, such as skin pigment changes or bumps where incisions are made.
Hair loss continues: Hair restoration surgical procedures have no effect on one's genetic program for losing hair. After surgery, hair loss due to inherited genetics will continue, and continued loss of hair may cause previously dense hair to become thin. Depending upon the design of the hair restoration procedure and the pattern of loss, further hair loss may eventually result in unnatural appearing "islands" of surgically arranged dense hair surrounded by new thin areas.
Variations
Transplants: Are the surgical movement of live hair follicles contained in small pieces of scalp called grafts. The grafts can be full size, or smaller mini and micro grafts.
Full size grafts (plugs): Full size grafts (or plugs, as they are commonly referred to), have between 10-20 hairs each, and were used in almost all hair transplants in the 1970s and 1980s.
Mini and micro grafts: Mini and micro grafts have between 1-5 hairs per graft, and are presently the most popular surgical hair restoration treatment. Variations of mini and micro grafting procedures include mega-sessions, laser transplants, dense packing, and front forelock transplants.
Mega-sessions: Mega-sessions are micro grafting procedures where over 1,000 specially prepared micro grafts are placed in a single session.
Laser transplants: Laser transplants use a cosmetic surgery laser to vaporize scalp tissue to make recipient holes or slits for placing micro and mini grafts.
Dense packing: Dense packing is a transplant procedure where specially prepared micro grafts are placed close together on a small area of the scalp.
Front forelock: A Front forelock procedure places micro and mini grafts into a patch of the scalp only at the front of the top of the head.
Special Location Transplants: Transplants to locations other than the scalp: Mustache, Beard, Sideburns, Eyebrows, Eyelashes, Chest, Pubic hair reconstruction
Reductions: Reductions move live hair follicles by surgically removing a patch of bald scalp, and then pulling up the hairy scalp to close the opening. Simple reductions are performed with local anesthetic, where only part of the scalp is numbed. There are two basic types of reductions : median and paramedian reductions.
Median reductions: Median reductions remove an oval-shaped patch of bald scalp from the middle of the bald area, usually in a line running from the front to the back of the head.
Paramedian reductions: Paramedian reductions remove a patch of bald scalp away from the middle of the bald area, usually from the edge.
Extensive reductions: Extensive reductions remove large areas of bald scalp, and move extensive amounts of live follicles as the hairy scalp is pulled up to close the opening. Extensive reductions are performed with general anesthesia, where the patient is "asleep" during the surgery. There are five basic types of extensive reductions: scalp lifts, expanders, extenders, transpositional flaps, and free flaps.
Scalp lifts: Scalp lifts remove a patch of bald scalp from the top of the head and, after extensively undermining the adjacent hairy scalp, pull the hairy scalp up to close the opening.
Expanders: Expander procedures involve two surgical sessions spaced 8-12 weeks apart. Expanders are balloon-like devices which are surgically inserted under the scalp during the first surgery, They are then gradually filled with saline solution over a period of weeks. As they expand, the expanders stretch the hairy scalp adjacent to the bald area. On the day of the second surgery, the expanders are removed, the bald scalp is removed, and the expanded hairy scalp is pulled together to close the opening.
Extenders: Extender procedures involve two surgical sessions spaced about 4 weeks apart. Extenders are elastic straps with small hooks attached at both ends. During the first surgery, an extender is stretched and placed under the scalp with the hooks sticking up into the underside of the scalp. Over a period of weeks the extender pulls together the hairy scalp from the sides and back of the head, and extends them into the area where the bald spot was. On the day of the second surgery, the extender is removed, all or part of the bald spot is removed, and the hairy scalp adjacent to the bald spot is pulled together to close the opening.
Transpositional flaps: Transpositional flaps are an extensive reduction procedure where first all or a portion of the bald scalp is removed. Next, strips of hairy scalp are partially detached from their original locations, and are rotated into the opening where the bald scalp had been. Both the area where the flaps were rotated into, and where they were moved out of are then sutured closed.
Free flaps: Free flaps are an extensive reduction procedure where first all or a portion of the bald scalp is removed. Next a patch of hairy scalp is completely detached and placed into the opening where the bald scalp had been. Using micro vascular surgery, tiny blood vessels supplying nourishment to the flap are connected to vessels in the new location. The area where the flap was removed is also sutured closed.
Artificial hair implants: Artificial hairs are typically made out of synthetic materials that the body does not reject immediately. Although new hairs are added, this treatment has serious disadvantages. To date, artificial hairs are the only medical device banned for use in the US by the FDA. Artificial hair implants are continuing to be developed and are available primarily in Japan, and in some European countries.
Hairpiece attachment: There are three ways that surgery is used to create secure but removable attachment points for hairpieces: tunnel grafts, suture loops, and osseo-integrated pins.
Tunnel grafts: Tunnel grafts are loops of live skin formed on the scalp. Tabs on the underside of a hairpiece fit into the loops of live skin.
Suture Loops: Suture loops are synthetic threads sewn into the scalp leaving exposed loops for tying on a hairpiece.
Osseo-integrated pins: Osseo-integrated pins are titanium pins which are positioned with one end imbedded into the bone under the scalp, and the other end exposed for hairpiece attachment.

Candidates
Persistent Loss: The best candidates for surgical hair restoration procedures are people with persistent hair loss, who also have ample hair along the sides and back of their heads. Some procedures, such as mini and micro grafts can help those just beginning to have thin hair, while others, including mini and micro grafts, are suited for those with clear bald areas.
Trauma Repair: Most surgical hair restoration procedures are also be used to repair the appearance of a person who has suffered a traumatic injury to part of the scalp, for example from an automobile accident or a fire.
Adequate health: Adequate health for surgery and is required, with no conditions restricting elective surgery such as pregnancy or severe cardiovascular problems. It is important that the surgeon be informed of any known allergies to medications. It is also important for the patient's health for the surgeon to be informed of any and all medications or nutritional supplements currently being taken, including prescription, over-the-counter, and herbal products, as well as any illegal drugs. Extensive surgical procedures are more demanding on one's health, and have greater health restrictions than simple procedures. Most procedures require no greater health than that needed for a visit to the dentist.
Realistic expectations: Candidates must have realistic expectations for the results achievable with each of the hair transplantation surgical treatment methods. Surgery for hair restoration is designed to give the appearance of having more hair, not resolve emotional and behavioral problems.
Follow through: Hair restoration surgery patients must be motivated to follow through with the entire set of procedures recommended, if more than one procedure is indicated, and to carefully follow the surgeon's instructions for care after each surgery.
Dense, curly hair: Those with dense hair along the sides and back will achieve a greater visual impact than those with less dense donor hair. Curly hair will generally appear denser than straight hair.
Not scar readily: Those with skin that does not scar readily, or form bumps, will have better cosmetic results than those who do. Generally, those whose ancestry is Native American, African, or Asian are more prone to scarring and bumps from surgery than people of European descent.
Tips
Long hair helps: It is helpful to allow your hair to grow long prior to surgery, so that it can be used to camouflage grafts or incisions that may otherwise be visible immediately after surgery.
Plastic shower cap: During the healing period most surgeons advise their patients to apply antibiotic ointment to their scalp to keep their wounds moist, discourage infections, and generally promote healing. At night this can make a mess on bed sheets and pillow cases. One solution is to wear a large plastic shower cap at night to keep the ointment off one's bedding.
Future
Techniques: Surgical techniques are constantly improving in incremental steps, and occasionally in large leaps. Chilling grafts immediately after harvesting and during preparation to improve survival is an example of an incrementally improved surgical technique. Improvements in surgical instruments, such as the development of multi-bladed scalpels and finger-sized instruments also help to improve results. The future will bring more of these improvements.
Medications: In the future new medications to accelerate recapilarization of the transplanted grafts will improve the yield of transplant procedures. Other medications may reduce the tendency for transplanted follicles to enter the telogen, or resting phase of hair growth immediately after transplantation.
Robotics: Currently there are a handful of cutting and insertion machines designed to partially automate the hair transplantation process. As they are improved upon, they bring the promise of consistent quality and reduced costs to some methods of hair restoration surgery.
Lasers: The use of surgical lasers to prepare recipient sites for hair transplantation is gaining popularity. Improvements in surgical lasers, and especially scanning lasers, may advance hair restoration surgery in the future.
Genetics: In the future, with great advances in genetics, the possibility of cloning hair follicles which can later be inserted surgically will revolutionize hair transplantation surgery. Cloning will essentially allow for an unlimited quantity of one's own "permanent" hair follicles to be "test tube" grown and later implanted.