Symptoms and Classification of Uterine Adenomyosis
Symptoms and Classification of Uterine Adenomyosis
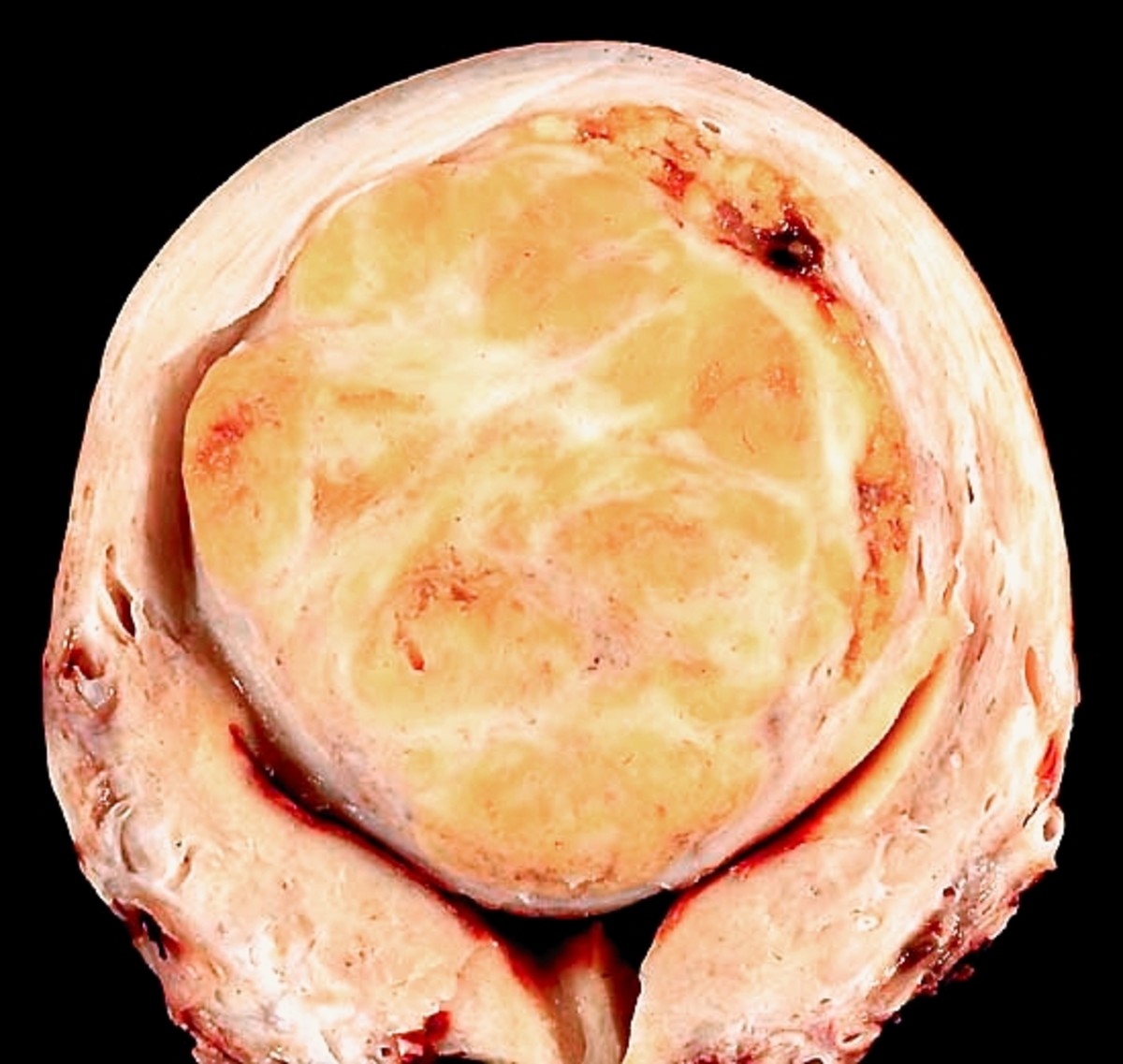
Adenomyosis is a condition that involves the encroachment, or movement, of the endometrial tissue that lines the uterus into the muscles of the uterus. This makes the uterine walls grow thicker. It may lead to heavy or longer-than-usual menstrual bleeding, as well as pain during your menstrual cycle or intercourse. The exact cause of this condition is unknown. However, it is associated with increased levels of estrogen. Adenomyosis usually disappears after menopause (12 months after a woman’s final menstrual period). This is when estrogen levels decline.
The one thing that is needed to be kept in mind with adenomyosis is the major differential is going to be fibroids, leiomyoma.
A Case Study in Brief
A 42-year-old woman presents to the clinic complaining of heavy menstrual flow over the past 9 months. Normally, she goes through about two pads per day, but lately she has needed about four to five pads per day. She also woke up with bleeding on her pajamas. Her menstrual periods are predictable 28-day cycles. She is a G6, P3-0-3-3, with a history of three D&C’s for spontaneous abortion lost between 12 and 14 weeks. All of her three deliveries were via C-section. She does have some mild pelvic pain, but most of the time it is relieved with Midol. She is monogamous with her husband of 23 years, and has no history of sexually transmitted diseases. She is otherwise in good health and is on no medications. She does not smoke and she drinks alcohol only socially. There are no other complaints at this time. Her physical exam is significant for a tender, boggy uterus. There are no masses.
We start to look at this patient with heavy menstrual flow, not an uncommon thing for a woman to present with, especially as they get closer to menopause, not necessarily heavy menstrual flow so much as irregular menstruation. They will not have their periods as frequently, but heavy menstrual flow is always concerning in any woman because of the possibility of developing anemia. So we always want to look into this. Now, the number of pads a woman uses is going to vary from woman to woman, and it also is going to vary on the type of pads she uses, because some are more absorbent than others, but what you want to look at not so much how many pads she is using. Obviously she is going through 10 to 12 pads a day, which is not normal. It is not so much the number of pads she is using so much as has it changed. Some women will go through three pads a day. She has always gone through that many; she uses the same brand that is going to be constant and normal. Now, other women will have a heavy flow or have developed heavy flow, will find that they have been using the same number of pads for 10 years, and now suddenly they are needing more. That would be suggestive of a process going on that is causing them to bleed more. So it can be difficult with distinguishing how many pads is normal, how many is abnormal. Some women bleed more than others, so it is not necessarily very helpful, but please look for changes when you are looking at heavy flow. Her menstrual periods are normal, so this is just menorrhagia, (menstrual periods with prolonged bleeding) not menometrorrhagia, (prolonged excessive uterine bleeding occurs irregularly and frequently than normal). She does have a history of miscarriages, not necessarily associated with this. She also has a history of surgery to the uterus we consider D&C to be a surgery because we are manipulating the uterus internally. She has had three deliveries, obvious C-section, so again more uterine surgery and then she has also got this pelvic pain, but that is mild that is really not the reason she is coming in. She is coming in because of heavier menstrual flow. So, briefly, we have a woman with heavy menstrual flow, a little bit of pain, one of the things that we need to always consider in a woman, especially a woman in her 30s, or 40s who is presenting with heavy menstrual flow is going to be adenomyosis, and there are other things that it could be, but this is one of the things that is going to be in our differential. Now, when we do the physical exam there are other things that are going to point to adenomyosis and that is going to be an enlarged uterus. So typically the uterus is going to be tender. If you were to further probe her and ask her about sex, she may tell you that occasionally she has some pain during sex that is also consistent with adenomyosis. There are no masses. This is very important, because one of the things that we wanted to distinguish this from is leiomyoma fibroids. Fibroids will bleed, they do bleed; however, fibroids typically are not painful so much. This could easily be fibroids because there is not as much pain going on, it is mostly bleeding, and one of the tests that is going to be done is a transvaginal sonography, and that will really help us distinguish this from fibroids.
The following factors need to be considered for the case:
- Pathophysiology.
- Epidemiology and risk factors.
- Presentation.
- Workup.
- Management.
Adenomyosis is characterized by uterine enlargement caused by ectopic rests of endometrial tissue within the myometrium. This is different from endometriosis. There are some similarities. In endometriosis one has endometrial tissue where it should not be, and with adenomyosis you have endometrial tissue where it should not be. It should not be in the myometrium, it should be outside the myometrium along the lining of the uterine cavity. So we do have endometrial tissue where it should not be, but with endometriosis the endometrial tissue will be outside the uterus. It will be on the uterosacral ligament, it will be elsewhere. With adenomyosis it is solely in the myometrium. It can be diffused, or focal, so you could have little bits and pieces of foci of endometrial tissue all over the myometrium that would be considered diffuse adenomyosis or it might just be in one spot, and so you just have an enlargement in one part of the uterus. You can imagine that is the one that is very difficult to distinguish from fibroids, because you just have a little area or maybe a few little areas of uterine enlargement that can feel like a fibroid, but most of the time it is going to be diffuse enlargement. So, adenomyosis differs from endometriosis, but there are some features that it shares in common, so they are both as mentioned characterized by ectopic endometrial tissue. They also both cause pelvic pain, pretty similar pelvic pain. Both are also hormonally sensitive. So increased estrogen is going to cause enlargement, proliferation of the endometrial tissue, and so that is going to worsen the symptoms. So a lot of times the pain will come around the time of menstruation, so both endometriosis, and adenomyosis will experience dysmenorrhea pain during menstruation, specifically secondary dysmenorrhea. As mentioned, both cause pain, and they are both also related to prostaglandin level. There is something unique about the uterus, and that is in between the endometrium and myometrium there is really nothing. It just goes from endometrium to myometrium.
- The pathogenesis is not fully known. As mentioned, it most likely is due to a direct invasion of the endometrium into the myometrial layer, which results in those foci of the endometrium within the myometrium.
- Both increased vascularisation of endometrium near the adenomyotic foci, as well as ectopic estrogen production very similar to pathophysiology. We see with the excess estrogen production in endometriosis. That is going to stimulate that tissue, and so both of these are going to cause increased bleeding, they are going to contribute to the increased bleeding. The reason that one gets pain is probably due to increased prostaglandin production in these foci very similar to endometriosis.
- Risk factors. So most women who present with adenomyosis are going to be in their 40s and 50s. That is very different from endometriosis. A lot of women who present with endometriosis they could be teenagers, they could be in their 20s. Most women with endometriosis will present as young women. With adenomyosis they tend to present as older, but not menopausal women. So they are usually in their 40s, even in 50s, but they are not menopausal, because once they have hit menopause this should get better. There is also an association with multiparity (the production of two or more at a birth). So, 90% of adenomyosis cases happen in women who have had children. The reason for this is probably due to the trauma to the uterus that normally occurs during delivery; yet one gets trauma and that stretching occurs, you have trauma to that endometrial myometrial boundary, and so it is easier for endometrial foci to invade the myometrium.
We also see increased incidence of adenomyosis in women who have had prior uterine surgery, probably the same reason you get that trauma. Other possible risk factors include things like smoking, antidepressants, and tamoxifen. The antidepressants are probably because it alters the dynamics of prolactin, and that is going to affect the chemistry of the uterus. Tamoxifen is actually estrogen for the uterus. So remember tamoxifen is one of those selective estrogen receptor modulators where it sort of inhibits the action of estrogen in one area and then acts as an agonist in another area. These are possible risk factors. These other one though are known risk factors, such as age, parity, and prior uterine surgery.
Epidemiology
Till date no one really has any idea how many cases happen, because many of these cases are under-diagnosed and a lot of these are diagnosed after hysterectomy. The frequency at hysterectomy for any reason has been reported between 20 and 60 percent, a huge variation depending on studies. A lot of these women though will not have symptoms. There is no data on racial differences that is unlike endometriosis where it is believed it happens more in Asians and whites than in blacks and Hispanics, and then unlike endometriosis, adenomyosis as we talked about tends to present in older women, but still premenopausal, so women in their 30s and 40s as opposed to teenagers and twenties. Only about one-third of women with histologic adenomyosis will have symptoms, and a lot of times those symptoms are so mild that it does not get actually diagnosed. So it might just be a woman with heavy flow, but she does not really think twice about it, never gets diagnosed with it. So, adenomyosis is very common, very under-diagnosed, and a lot of women who have it they do not have symptoms or their symptoms are bad enough to where they seek any kind of treatment. So it is usually the severe cases that are the ones that seek treatment. Many women with adenomyosis will also have fibroids and a lot of them are also at mildly increased risk for endometrial carcinoma. Why is that? Because these women likely genetically have higher estrogen levels, they have higher expression of aromatase, so they have higher estrogen levels, and estrogen contributes to all of these leiomyoma, adenomyosis, and endometrial cancer, not 100% certain, but they are still studying that, research is still going on, but we do know that there is a very high correlation between adenomyosis and uterine fibroids.
Presentation
The most common present symptom of adenomyosis is abnormal uterine bleeding namely menorrhagia, as well as secondary dysmenorrhea. So it should be on the differential in any woman who has increased menstrual flow and any woman who is presenting with secondary dysmenorrhea. The severity of symptoms will correlate with a number of foci and the extent of invasion and that makes sense, because the pathophysiology here is that you have these foci and then the endometrium becomes more vascularised over those foci over the myometrium. The more vasculature one has the more she is going to bleed when she has her period. Ten percent of women with adenomyosis will complain of dyspareunia. There is pain during intercourse. Fertility issues usually are not a problem with adenomyosis, but they do have an increased risk. The reason is it is not so much a problem; it is because women typically do not develop problems from adenomyosis until they are older and typically they are not trying to get pregnant at that point. They do not complain of problems with fertility; however, we do know that with adenomyosis there is an increased risk for ectopic pregnancy, so what can happen is that the fertilized egg and embryo will get in a little bit deeper into the endometrium, and if it finds endometrium in the myometrial layer it can implant there and that would be an ectopic pregnancy.
So typically saying, we have seen the above-mentioned patient, she has a few miscarriages, but that is not necessarily due to the adenomyosis.
Adenomyosis management
- Treatment objectives are to relieve pain and control bleeding.
- Combined oral contraceptives or progestin are typically the first line of therapy.
- NSAIDs may be used for additional pain management or as the primary therapy for women wishing to become pregnant.
- Hysterectomy is the most definitive management.
Other surgical techniques commonly used include endometrial ablation and uterine artery embolization.
This content is accurate and true to the best of the author’s knowledge and is not meant to substitute for formal and individualized advice from a qualified professional.
© 2019 Putcha Venu Madhav