The General Clinical Significance Of Amoebiasis Infection: Parasitology, Transmission And Pathology
How To Prevent And Cure Amoebiasis

Amoebiasis
The term amoebiasis includes all lesions caused by infection by the protozoan parasite Entamoeba histolytica. Amoeba cause ulcerative lesions in the large intestine causing dysentery and from there, they spread to several organs to produce necrotic lesions. There is a great tendency for the intestinal infection to become chronic and persistent for long periods. However, E. histolytica can also remain in the bowel for many years without causing major symptoms.
Amoebiasis is worldwide in distribution, but it is very prevalent in tropical climates. In many parts of India, the infection rate may be as high as 40 to 50%. Chronic carrier state, poverty, insanitary disposal of excreta, unhygienic food handling and proliferation of flies are responsible for this high prevalence. Though all age groups are susceptible, adults suffer more often.
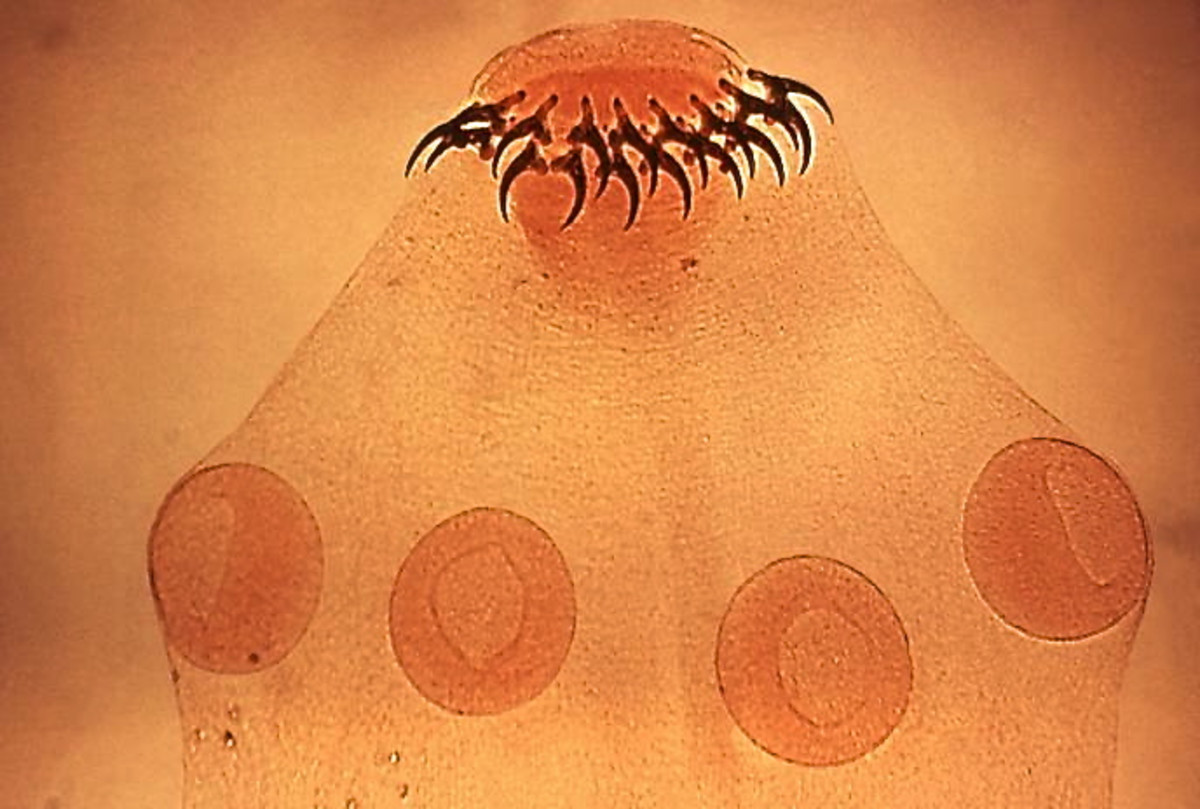
Parasitology: Amoebae are widely distributed in nature. The common pathogen is E. histolytica. It exists in two forms- the cyst and the trophozoite. The cysts are round or oval in shape and measure 10 to 15u in diameter. In iodine-stained preparations, the cysts show one, two or four nuclei depending on their maturity. Cysts resist adverse environment. In addition to the nucleus, one or more rod-like structures called chromosomal bars, and a glycogen mass are also seen. Cysts are formed in the bowel when the environment becomes unfavourable for the trophozoite or they are formed outside when passed out in feces. Cysts are responsible for transmission of the disease from person to person. The vegetative form (trophozoite) is actively motile by the aid of pseudopodia. It measures 20 to 50u in diameter. Invasive trophozoites are identified by the presence of ingested erythrocytes within them. Amoebae multiply by binary fission. The trophozoite is the invasive form and is responsible for all lesions. A large number of trophozoites is seen in the feces of dysenteric patients. Outside the body, they survive only for an hour or so. Normal gastric juice destroys them in the stomach.
How Intestinal Amoebiasis Is Transmitted

Infectious Diseases
Transmission And Pathology
Transmission
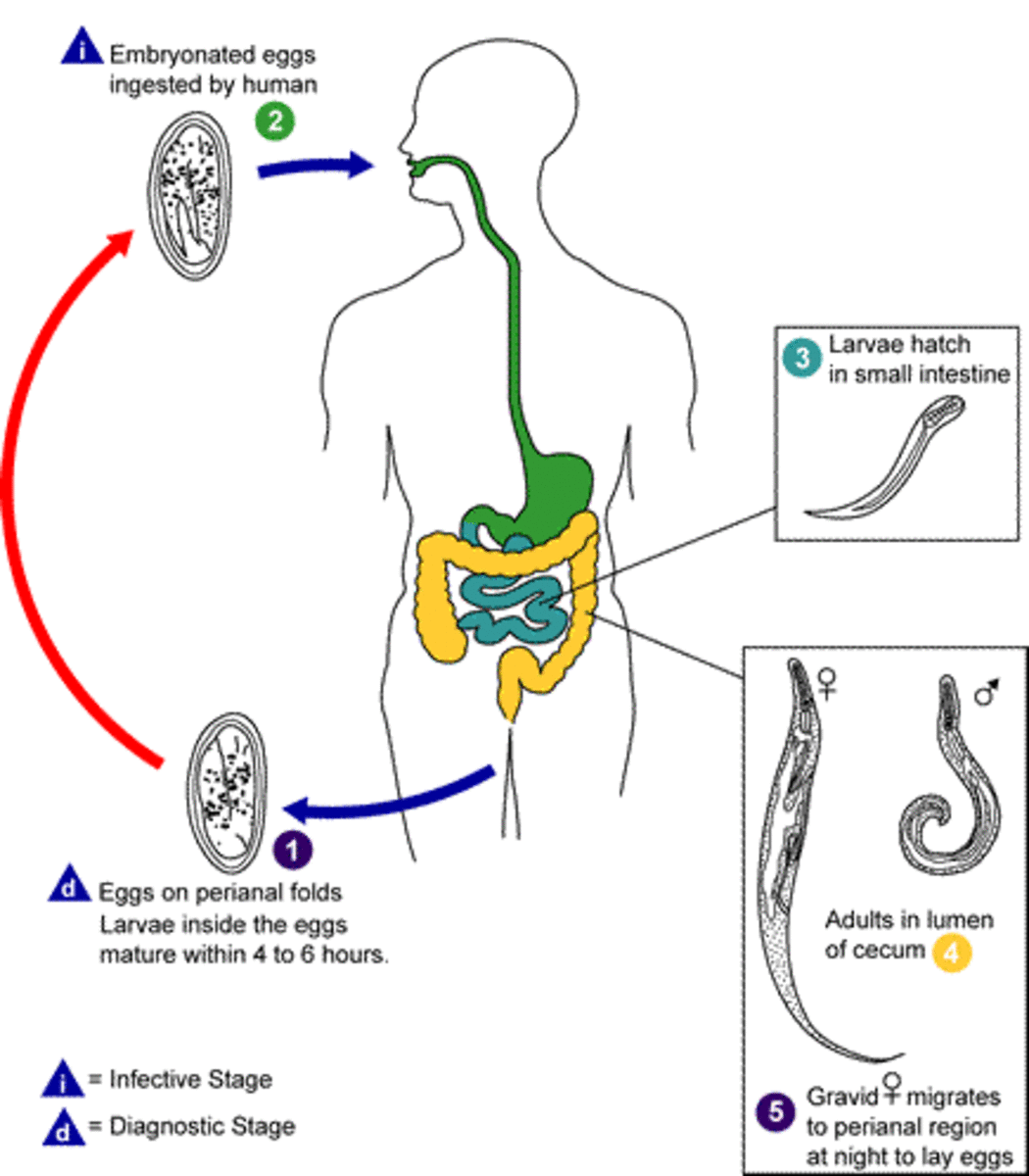
Cysts are passed in the feces of cases and carriers. These are ingested along with food or water. Cysts resist acid digestion in the stomach. Excystation occurs in the intestines. Trophozoites develop from cysts and they establish themselves in the colon, feeding on the bacteria and desquamated epithelial cells. They multiply by binary fission. These non-invasive forms may persist for long periods without producing any symptoms.
Pathology
Intestinal amoebiasis: The invasive trophozoites ulcerate the mucous membrane and penetrate deep into the submucosal layers of the colon. The amoebase burrow laterally to produce flask-shaped ulcers. The basic pathological process is a lytic necrosis of tissue. The cellular response consists of mononuclears and a few polymorphs. Amoebae are seen in the invading margins of the lesions. Cecum, ascending and descending colon and rectum are the sites of predilection. The appendix may be involved. The terminal ileum may be affected rarely. The ulcers have undermined edges and are covered by dense yellow or brown slough. The mucous membrane between ulcers is healthy. Ulceration may extend to blood vessels causing severe hemorrhage at times. Perforation of the bowel may occur, but it is rare. Sometimes, amoeboma or amoebic granuloma develop due to repeated infection by amoeba and bacterial pathogens. The acute inflammatory process has a tendency to subside spontaneously. In many patients, chronic infection persists with microscopic lesions which harbour E. histolytica for many years. The lesions may heal in a few cases. Persistence of the chronic lesions accounts for the carrier state.
© 2014 Funom Theophilus Makama