The Health Implications Of Cerebral Malaria And Other Forms Of Malaria
A Cerebral Malaria Patient
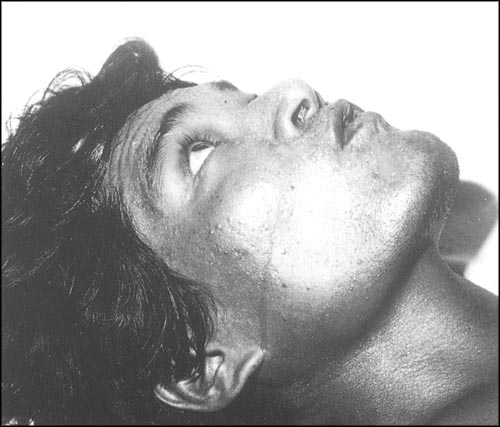
Cerebral Malaria
This is caused by occlusion of the microcirculation of the brain, cerebral edema caused by sludging of the parasitized erythrocytes and arterial damage. Infected erythrocytes develop projections on the membrane called “Knobs”. The knobs of P. falciparum seem to help attachment of parasite erythrocytes to vascular endothelium. Endothelium attachment helps in the maturation of the Schizont and the resultant vascular damage.
Minute areas of infarction, perivascular hemorrhage and edema are seen. Symptoms include hyperpyrexia, headache, convulsions, coma, various forms of paralysis, meningism or neuropsychiatric disturbances. This picture may resemble any other form of acute inflammatory disorder of the brain. The CSF is under high tension, but unlike in meningitis, pleocytosis is not prominent, though mild lymphocytic pleocytosis (less than 300/mm) has been reported. The CSF protein level is not grossly elevated. Cerebral malaria is fatal if left untreated, but if treated with specific antimalarial drugs early in the disease, recovery is dramatic. Even antimalarials may not give prompt relief if the condition is advanced and structural changes have occurred.
A Patient With Malarial Hyperpyrexia
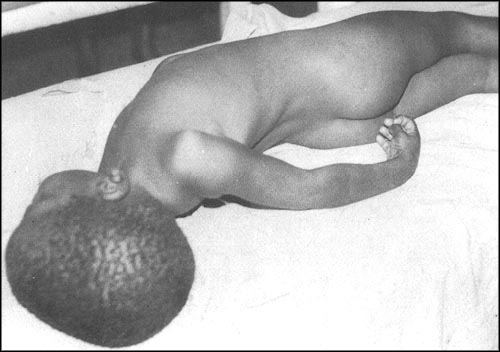
Malarial Hyperpyrexia
Hyperpyrexia (temperature of 410 to 430C) may develop and this may be mistaken for heat stroke.
Gastrointestinal form: This manifests with severe nausea, vomiting, epigastric tenderness, hematemesis and diarrhea. In some cases, the stools are watery as in cholera, in others it is blood stained as in dysentery. Some patients develop severe jaundice, hepatomegaly and a picture clinically resembling fulminant hepatic failure. This used to be known as bilious remittent fever. Death may occur due to dehydration, shock, acute renal failure or hepatic failure.
Algid Malaria
This occurs in patients with predominantly gastrointestinal manifestations. They become extremely dehydrated and shocked without any warning signal. The surface temperature may drop, but the rectal temperature remains elevated. Unless managed as an emergency, mortality rate is high.
A Patient With Black Water Fever
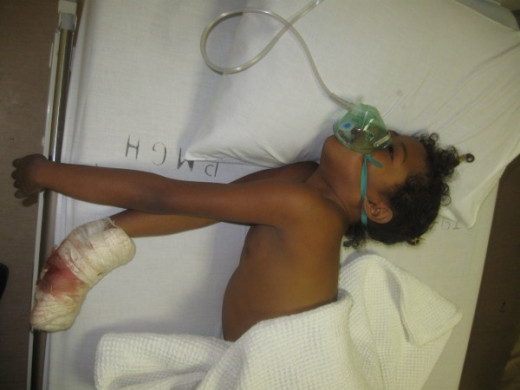
Black Water Fever (BWF)
This complication was frequent a few decades ago, but not it is rare. It occurs in patients suffering from chronic falciparum malaria who are treated intermittently and inadequately with drugs. Immune mechanisms operate to give rise to sensitization of the erythrocytes and severe hemolysis results from a fresh infection or the use of drugs. Both parasitized and non-parasitized erythrocytes are destroyed. Sudden intravascular hemolysis occurs giving rise to fever, rigor, anemia and hemoglobinuria if severe shock, jaundice, anemia and acidosis supervene. Since the parasitized erythrocytes are lysed, blood may not show the parasites. Hemoglobin and methamalbumin are present along with granular casts, hemoglobin casts and epithelial cells. The altered hemoglobin gives the dark colour to the urine. In severe cases, oliguric renal failure develops. Death results from shock, cardiac failure, renal failure or severe anemia. Prompt treatment on modern lines is able to save the vast majority of cases.
Treating A Patient With Quartan Malaria

Malariae Malaria (Quartan Malaria)
The incubation period shows wide variation from one month to several months. Fever occurs with quartan periodicity (every 72 hours). It may take some time to develop the periodicity.
Rigor may be absent at the onset. The paroxysms are shorter and more clearly defined when fully established. Hepatosplenomegaly is common. The parasite stimulates the production of antibodies which form antigen-antibody complexes leading to the development of nephrotic syndrome. Institution of specific treatment early in the disease resolves the renal lesion, if treatment is delayed, the renal lesion may not resolve. Peripheral blood shows all stages of the parasite.
© 2014 Funom Theophilus Makama




