The Health Implications Of Other Filarial Infections To Man’s Health
Culicoides: Blood Sucking Insects

Tetrapetalonema Perstans
This parasite is prevalent in central Africa, South America and the Caribbean. Adults are seen in the subserosal layer of viscera. The pleura, pericardium and peritoneum are involved. In many cases, the mesentery is a frequent site. The microfilaria are unsheathed, non-periodic and are demonstrable in blood. The vectors are the blood sucking insects- Culicoides. Though in the majority of cases, infection is asymptomatic, some cases may develop fever, pruritus, skin rashes and abdominal pain. Demonstration of the microfilariae in peripheral blood confirms the diagnosis.
Treatment: Diethyl carbamizine is generally ineffective. Success has been reported with mebendazole given in a dose of 100mg twice daily in combination with levamisole 100 mg daily for several days.
Tetrapetalonema Streptocerca
It is prevalent in parts of Africa. It is transmitted by Culicoides. Adult worms are seen in the dermis and subcutaneous tissues. The microfilaria are nonperiodic and they are seen surrounding the adult worms and are demonstrable in skin snips, taken from the lesions. Clinical features consist of pruritic papular rashes, edema and hypopigmentation. This worm responds to diethyl carbamazine in the usual doses.
Mansonella Ozzardi
This infection has been reported from the tropical regions of South America. Adult worms are found in the visceral adipose tissue. Microfilaria are nonperiodic and are seen in peripheral blood. Vectors include Simulium and Cuhcoides. In the majority of cases, this infection is nonpathogenic, though fever, lymphadenopathy and erythematous skin rashes may occur at times. Treatment with diethyl carbamazine is generally infective.
Serpent Worm Infection In Sudan

Guinea Worm Infection In Ghana
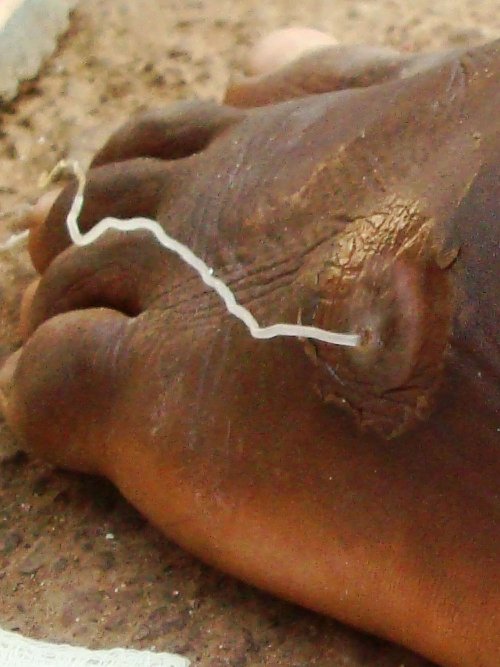
Dragon Worm Infection In Chad
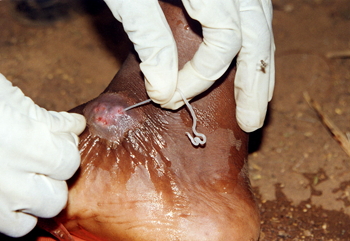
Infectious Diseases
Dracontiasis (Guinea Worm, Serpent Worm, Dragon Worm)
Infection by Dracunculus medinensi is found in several endemic pockets in India, Pakistan, Iran, Middle East, West Indies, South America and East, West and Central Africa.
Morphology and habitat: Adult male is 2.5cm long and is short lived. The female worm is 60 to 100cm long and 1.5 to 1.7 mm in diameter, cylindrical, white and is viviparous. The posterior end is tapering and hook shaped. Opening of the uterus is at the anterior end. Adult females may live up to one year. Larvae are discharged in batches when the anterior end of the worm comes in contact with water.
Lifecycle: The larvae are taken up by fresh water Cyclops, belonging to the family crustacean and these form the intermediate hosts. The larvae become infective to man in 10 days. Man gets infected by ingesting the Cyclops in water. The larvae are liberated in the intestine and these migrate to the retroperitoneal connective tissues to grow into adults in 9 to 18 months. After fertilization, the females come to lie subcutaneously under those parts of the body which come in contact with water. At the anterior end of the worm, a blister develops which breaks down to form an ulcer. When the part comes in contact with water the worm protrudes its anterior end through the ulcer and discharges a milky fluid containing a large number of larvae. Over a period of 3 weeks, the worm is extruded and the ulcer heals. Infection is generally acquired when the drinking water source is infested with Cyclops and people walk into them to fetch water.
Pathogenesis: Initial symptoms include urticaria, eosinophilia, wheezing, nausea, vomiting and diarrhea. Formation of the blister is accompanied by local pain, itching and inflammation. The tissues around the blisters may become red, tender and edematous. Secondary infection of the ulcer Is common. Periarthritis and pyoarthrosis may occur if the worms are in the neighbourhood of joints. The ulcer may even act as a portal of entry for Clostridium tetani. Sometimes, the female worm may be palpable in the subcutaneous tissue. Worms that fail to reach the surface die and get calcified. Aseptic abscesses may develop around the worms.
Treatment: Local dressing and administration of antibiotics serve to minimize local infection. Removal of the worm is achieved mechanically. The worm is induced to discharge its larvae in water for a few days by which process it protrudes more and more. As the anterior end comes out progressively, it is tied with a fine silk thread and rolled up over a matchstick till it is extracted fully over a course of 15 to 20 days. Live worms are easier to extract. If the worm breaks and its anterior end retracts, the track is likely to be infected. Surgical measures are indicated when conservative treatment fails.
Drug therapy: Niridazole given in doses of 26 mg/Kg twice daily for 7 to 10 days effectively kills the adult worm. Thiabendazole given in a dose 25 mg/Kg for 3 days or metronidazole 250mg given 3 times a day for 7 days are also effective.
Rare Helminthic Infestations
Sporadic cases of exotic helminthic infections are reported from time to time. These include multiceps, intestinal capillariasis, anisakiasis, angio-stronglyliasis, gnathostomiasis and sparganosis.
© 2014 Funom Theophilus Makama