The Sojourn Journey of Thyroid Nodules and Thyroid Cancer
The Sojourn Journey of Thyroid Nodules and Thyroid Cancer
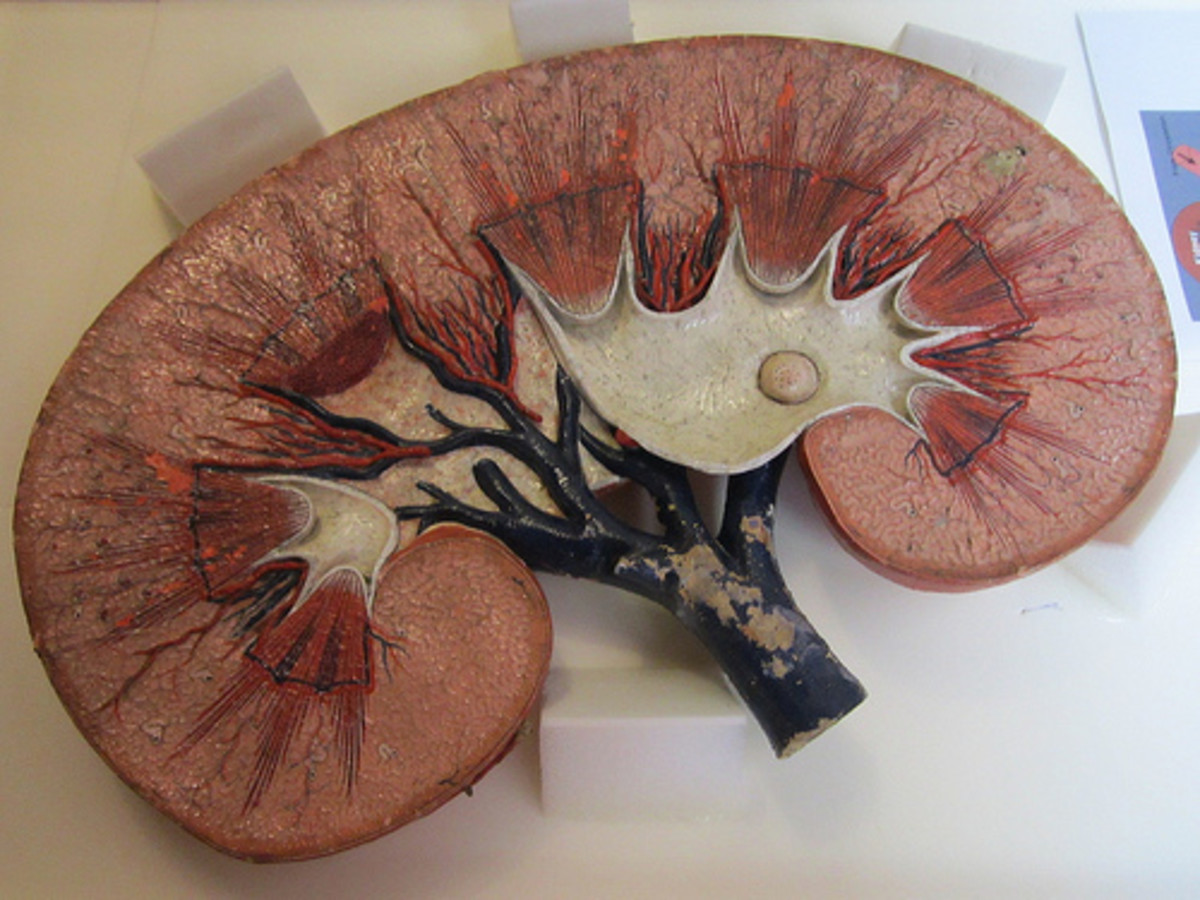
Thyroid nodules are very common. If you were to ultrasound anyone, up to half of 6-year-old would have a thyroid nodule. Thyroid is situated in front of the neck. Risk factors for thyroid nodules are increasing by age, females having a radiation exposure, or being in an iodine deficient part of the country. Thyroid nodules are also more common in women, and we need to differentiate whether the nodules identified on physical exam, or by an ultrasound. About 6% of women and 1.5% of men would have a palpable nodule, but if you were to ultrasound everybody, about 75% of women, and about 45% of men would have a thyroid nodule seen on ultrasound. Thyroid nodules are more common as patients get older. If you ultrasound everybody, by the time their age is 80 or 90 most patients would have a small thyroid nodule seen on the ultrasound, but most of these will not be palpable, meaning one cannot actually feel it in the neck.
It is extremely important to note most of the thyroid nodules are NOT cancer. So, the first time when a patient is told that he or she has thyroid nodule they immediately think this is cancerous. The good news is that it is unlikely to be cancer. The overall malignancy rate is only about 5%, but it is a higher malignancy if you are a child, or if you are older.
As already told most thyroid nodules are benign. We need to separate the benign nodules from the suspicious nodules that require further workup and potentially treatments. So physicians always start with a history by talking to the patient, and this focus is first on could this nodule be producing excess thyroid hormone. Usually, those patients will have weight loss, trouble sleeping, anxiety, heart palpitations things like that. It is also important to note whether there is a family history of thyroid cancer, or any endocrine disorders in the patient, or in the family that might suggest predisposition. The next important point is radiation exposure. That does not include CAT scan, dental exams, or x-rays, if in case one has lived next to a nuclear power plant or if he or she had radiation treatments for something like lymphoma as a child.
Most of the thyroid cancers are painless, and most of the thyroid nodules are also painless. So, pain is usually not a symptom of thyroid nodules. Sometimes if a nodule is very large it can cause compression. In case that nodule is usually about 4 cm in size then the patient may have trouble swallowing.
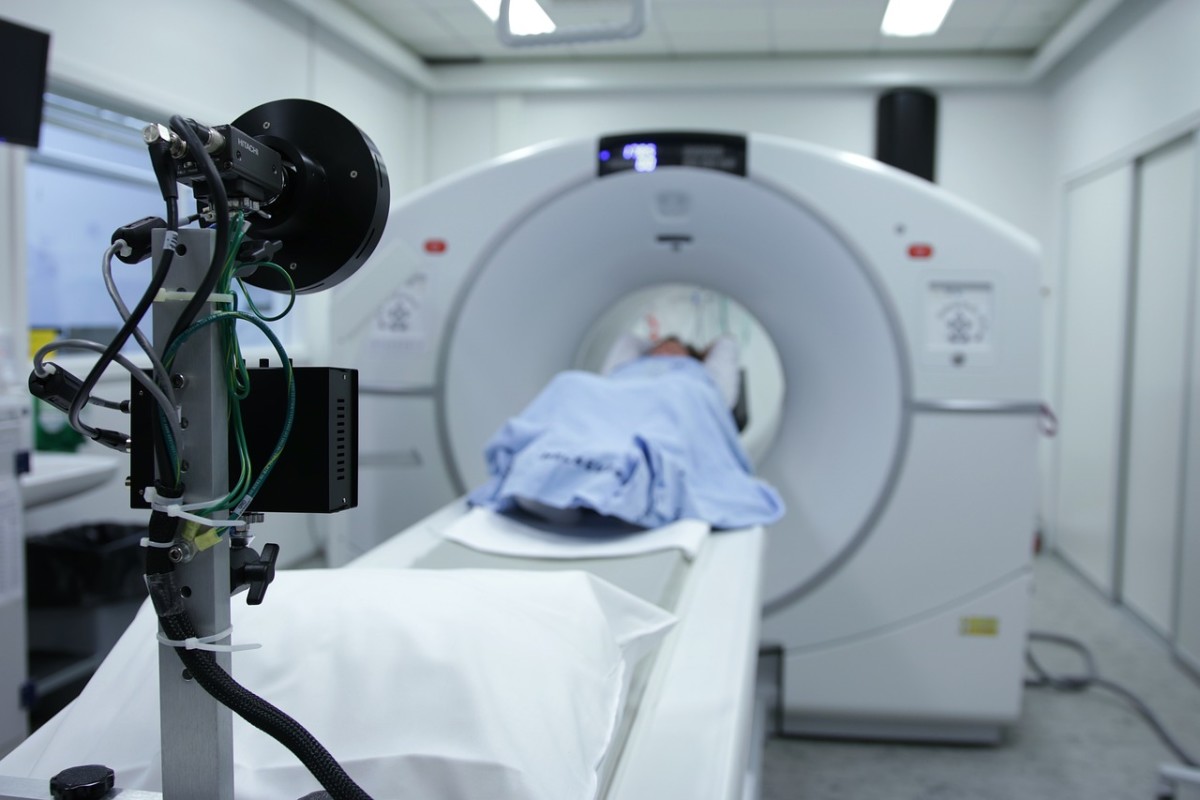
The next step would be a physical exam. The doctor will feel the neck, will feel what the nodule feels like if we can feel it and also feel for any lymph nodes, and then will also check the labs, specifically what the thyroid function tests are. However, the history and the physical exam alone are not very accurate in differentiating between a benign and a cancerous thyroid nodule. What is really a key are the thyroid ultrasound and the biopsy. The ultrasound is highly accurate for thyroid nodules. It is non-invasive, there is no radiation exposure. Most of the patients do not require any other imaging. Most patients do not need a CT scan, or a PET scan, or anything like that. You can see exactly what the nodule looks like, other nodules, and the lymph nodes. The doctor also looks back to see if there are any previous ultrasounds to see if the nodule has grown, and what the lymph nodes look like.
There are as mentioned new guidelines that came out from the American Thyroid Association, and they help us with suggesting how to work up and treat thyroid nodules, and well differentiate thyroid cancer. Ultimately, the treatment decision is up to the patient and the physician working together. Do all thyroid nodules need a biopsy? The answer is no. It depends on how big the nodule is and how suspicious it may look on the ultrasound. They recommend no biopsy for most nodules smaller than 1 cm in size. There are rare exceptions, for example if the nodule looks very very suspicious on the ultrasound, if there is a strong family history, or known genetic condition things like that, but for most patients if you have a nodule less than a cm they recommend not biopsying it and just continuing to watch it with serial ultrasounds. Nodules that are purely cystic, it is completely black inside, as it is filled with fluid, those nodules are almost always benign and usually do not require a biopsy.
They do recommend a biopsy if a nodule is greater than 1 cm in size and looks very suspicious on the ultrasound. However, if a nodule does not look suspicious they recommend waiting until it is over 1.5 cm in size to biopsy, and the whole rationale behind this is to avoid over treatment. The biopsy is performed under ultrasound guidance. Before the doctor is able to biopsy the patients if they had a thyroid nodule the only way we could tell if it is cancerous or not was to remove it. Now with biopsying we can screen out a lot of patients having benign nodules and not operate on them. So it has decreased the number of patients having surgery by half.
These are the main categories of what the biopsy results may be. The first category is non-diagnostic. We would rather not see this. It means that they just did not get enough cells during the biopsy. So usually those patients require a re-biopsy.
The next category would be benign. If it is benign, then there is a very high chance that over 90% that it truly is benign. So those patients usually do not need any surgery and can just be observed.
The next category is indeterminate category. This means that there are some suspicious cells, but you cannot tell that it is cancerous and this can be a little bit frustrating.
The next two categories are basically that it is cancerous or most likely cancerous and the doctors usually treat that with surgery. What do we do with an indeterminate biopsy? This means that the risk of cancer is between about 5 to 30% depending upon the wording of the biopsy. Traditionally, most of those patients would have a repeat biopsy, and then have a surgical excision, because there is no other way that they could tell whether it was cancerous or not, and one might ask why cannot we tell on this biopsy if it is cancerous or not. Sometimes what you need to determine that it is cancer is to see those cells coming outside of the capsule of the nodule. You cannot tell that with just a biopsy a lot of times. So this is where the role of molecular testing has come in. It has really improved the care in these patients. Our whole goal is to avoid unnecessary surgery for indeterminate thyroid nodules, meaning if your nodule is benign and not causing any compressive symptoms we would like to leave it alone and not to operate on it. So if you look at a nodule that it has an indeterminate biopsy result the risk of cancer is about 20%. So if one has surgery, and it ends up being cancerous, then that was good, that was the right thing to do, and you may need further surgery to remove the rest of the thyroid depending on the results. However, most patients here will not have a malignancy in their thyroid, and in that case you have done the surgery, they may require some thyroid hormone. They unlikely, but may have had a surgical complication or a difficult recovery. So we would like to minimize this basically.
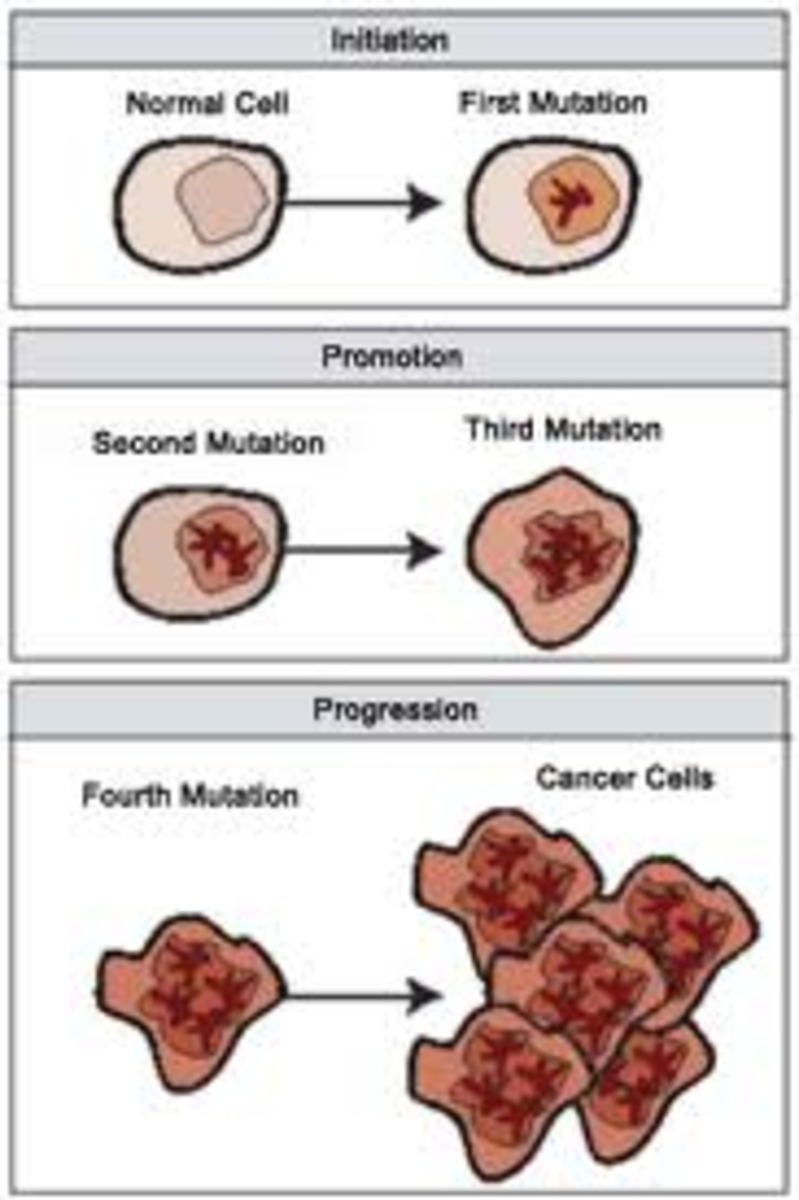
There are some molecular markers that have been developed in the past several years, and they rely on the fact that cancer cells have a different gene expression profile compared to benign cells.
Initial treatment of well differentiated thyroid cancer
A very important point to mention here is that most patients do not die from thyroid cancer, because most of the thyroid cancers are not as aggressive as some other cancers. The mortality is only about 1 out of 200,000 patients, and this has been stable for a long time.
Types of thyroid cancers
- Papillary thyroid cancer.
- Follicular thyroid cancer.
- Medullary thyroid cancer. This occurs in about 5% of patients.
Some unfortunate patients do have what is called anaplastic thyroid cancer, which is a very very aggressive kind. It often presents with a rapidly growing mass, very hard, often already metastatic at presentation. Those patients do have a survival of 6 months. This condition is extremely rare.
Usually the thyroid comes out in halves, so it is either half of the thyroid removed, which is a lobectomy, or the whole thyroid root, which is a total thyroidectomy. This also comes with new guidelines. The new guidelines suggest that the lobectomy alone is sufficient for many patients who have a tumor less than a cm get this well differentiated where the tumor is not growing beyond the thyroid into the muscle, or the trachea. There is no clinical spread to lymph nodes. So there actually could be a couple of lymph nodes that have little microscopic tumors cells in there as long as they are not large and then no high risk features in the family or the patient like radiation exposure. The guidelines do recommend doing a total thyroidectomy if the tumor is over 4 cm in size extending into nearby structures.
The risk of recurrence is really based on the initial extended disease. The overall long-term survival is excellent, but that does not mean that patients cannot have morbidity associated with thyroid cancer. It can really affect their life, cause problems in the quality of life, and some of that comes from a local recurrence, potential need for re-operation that has higher risks associated with that. So, the overall recurrence rate is about 15% and the real high risk features are if you had a really invasive tumor initially that was growing into surrounding structures, if you had incomplete tumor resection the first time and certainly if you have distant metastatic disease.
The doctor usually recommends drinking a lot of water; it can help with the radioactivity washing out sooner so that the patient is safe to be around children quicker, basically anything to keep with the salivary flow. Usually after getting a dose of radioactive iodine typically the patients are isolated for a few days. About 90% of the thyroid cancers are papillary in their variety.
If you have differentiated thyroid cancer most people, nearly 90% will be adequately treated with a single operation. Some people about 9% require two operations. Often times a second operation will be to address a lymph node, or a set of lymph nodes that may not have been fully addressed at the first time, as possible that it was a true recurrence that it grew back later, and just at the very tip of the pyramid are a small number of people with more aggressive thyroid cancer, thankfully that is the minority, and they may need more than two operations. For thyroid carcinoma, based on the size, these people with smaller tumors have excellent survival. In other cancers, for example colon cancer, pancreas cancer, we talk about five-year survival, or ten-year survival, because those diseases are very aggressive. In thyroid cancer people we talk about overall survival, 10-year or 20-year survival. We have the luxury of thinking about this because in general it is a very slow growing tumor. Even if one has a very large tumor, about 8 cm, in terms of survival at 10 years is 80%. So, thyroid cancer patients do really well. Having said that, the larger the tumor is the more likely it is to recur, or come back sometime in the next 10 years. The recurrence rate of thyroid cancer will range from 5% to 35% based on a number of factors. When do these recurrences happen, or who is more likely to have a thyroid cancer recurrence. If one gets a thyroid cancer you may as well be 35-year-old woman, because those people have the best prognosis, they have a very low rate of recurrence, and a very low rate of cancer related death. The people to get recurrent disease are often thyroid cancer growing back in the lymph node, or in lungs, more commonly in the lymph node, are either going to be very young teenagers, or people over 50.
The biggest risk factor for developing thyroid cancer is radiation exposure, especially childhood radiation, a childhood cancer that required head and neck radiation, family history. If persons have iodine deficiency in childhood it can predispose to thyroid cancer in later life.
This content is accurate and true to the best of the author’s knowledge and is not meant to substitute for formal and individualized advice from a qualified professional.
© 2020 Putcha Venu Madhav