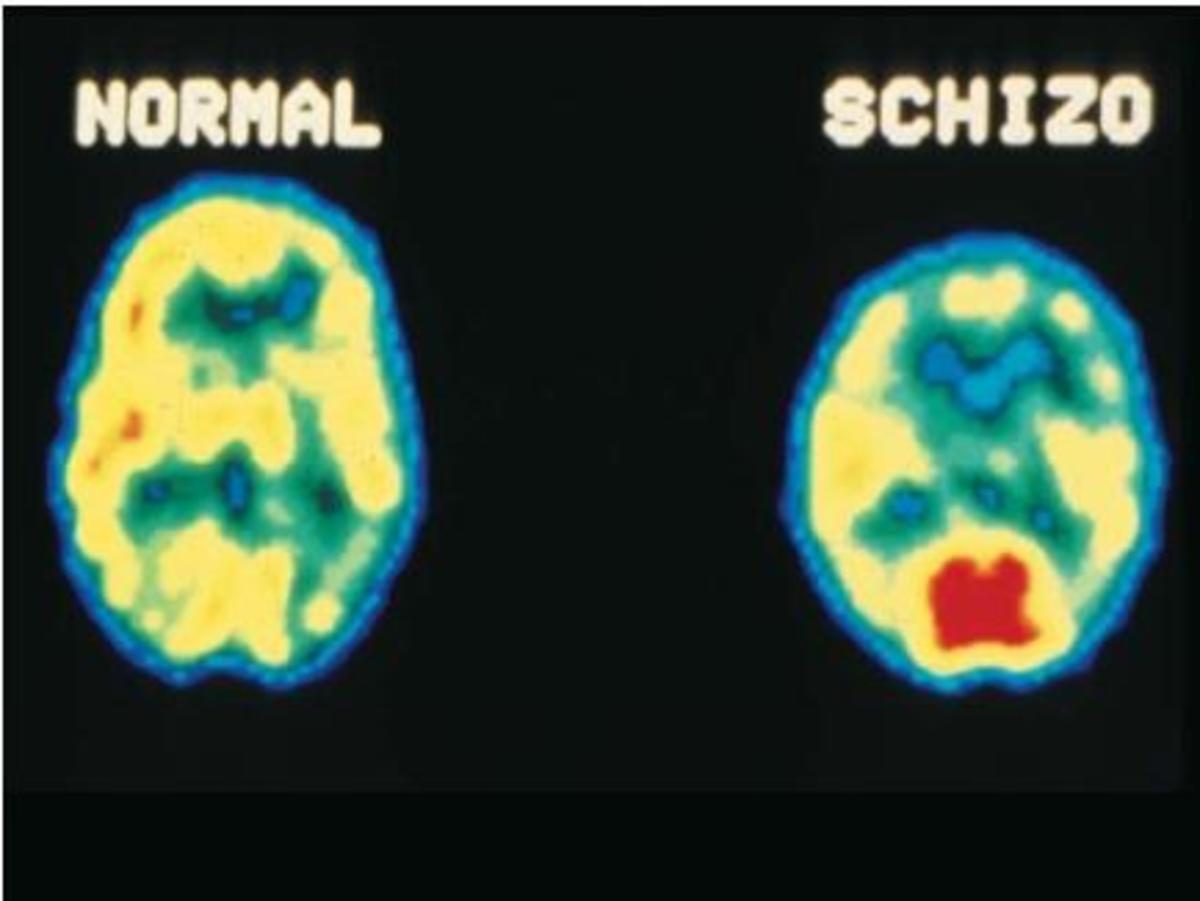
The Symptoms and Causes of Schizophrenia
Schizophrenia (SZ) is often misrepresented in the media or confused with Dissociative Identity Disorder. SZ is characterised by two types of symptoms: positive and negative. There are many different explanations for why some develop schizophrenia, with some claiming the role of the family affects the development of SZ, and others blaming biological factors.

The Symptoms of Schizophrenia
There are many symptoms associated with schizophrenia (SZ) which are placed into two categories: positive and negative symptoms. Positive symptoms add an excess or distortion of typical functions, whereas negative symptoms are a reduction or complete loss of functions. Typically, individuals will experience the negative symptoms before the positive.
Negative symptoms include:
- Speech poverty
- Avolition - a reduction of goal orientated behaviours
- Affective flattening - a reduction of emotional expression
- Anhedonia - a reduction of interest from activities that would normally be pleasurable.
Positive symptoms include:
- Hallucinations - unreal perceptions that can be auditory, visual, olfactory or tactile
- Delusions - bizarre beliefs that are not real
- Disorganised speech
- Grossly disorganised or catatonic behaviour - a lack of motivation to complete tasks
A prevalent issue within diagnosis using this criterion is that many of the symptoms overlap with other disorders. For instance, many of the negative symptoms (like affective flattening and anhedonia) are also symptoms of depression. Psychiatrists would need to know the patient's history to develop a better understanding as to whether they have depression, SZ or even both.
- What is Schizophrenia? DSM-5 Schizophrenia Definition & Symptoms
Learn about the DSM-5 definition of schizophrenia here

Psychological Explanations for Schizophrenia
The double bind theory (1956) claims that when a child receives mixed messages from their parents they are more likely to develop the disorder. For instance, if a mother tells their child they will take care of them but with an aggressive tone, this contradiction means the child is unable to construct a coherent reality.
Expressed emotions is a form of communication within the family in which family members talk in a hostile or critical manner that may also cause individuals to develop schizophrenia. Many families do not deliberately express these emotions and not everyone will develop SZ as a result, implying that some people are more vulnerable to intense emotional communications.
The cognitive approach explains the disorder as a result of dysfunctional thought processing. The way in which an individual interprets the world around them and their own relevance to this world can cause delusions to take place. For instance, when hearing a group of strangers laughing, someone may assume they are laughing at them despite this being unlikely. This individual relates irrelevant events to themselves thus creating delusional beliefs. This is supported by Sarin and Wallin (2014) who found that schizophrenic patients who were delusional were likely to jump to conclusions and not be able to perform reality checks on what appears logical and what does not.
A Biological Explanation for Schizophrenia
Family studies suggest that there is a potentially hereditary factor in developing SZ. Gottesman (1991) found that children with two schizophrenic parents had a concordance rate of 46% compared to the 13% of those with one schizophrenic parent. Twin studies also indicate a genetic explanation, Joseph (2004) found a concordance rate of 40.4% for monozygotic (identical) twins but only 7.4% for dizygotic (unidentical) twins. Both these studies suggest that SZ is can be inherited and is caused by a genetic disposition.
Despite this, if the participants of these studies have parents or siblings with the disorder, it is hard to tell whether their own development of SZ is a result of genetic factors or environmental. Perhaps the behaviours were learned from their family members. This has led to an investigation into adoption. Tienari (2000) compared adoptees with biological parents with SZ to a control group whose biological parents did not have the disorder. 6.7% of adoptees with SZ biological parents went on to be diagnosed with the same disorder compared to 2% of the control group. This further supports the notion of a genetic basis.
The dopamine hypothesis proposes that higher levels of dopamine in certain brain areas are associated with positive symptoms. This idea has led to potentially effective drug therapies. Amphetamines increase the levels of dopamine in the body, when given to a 'normal' individual, they may develop the hallucinations commonly seen in schizophrenia. In contrast, antipsychotic drugs reduce dopamine levels which can then reduce hallucinations and delusions. Antipsychotics are the most popular treatment due to their accessibility; they are quicker and cheaper compared to Cognitive Behavioural Therapy for Psychosis (CBTp).
The biological approach is criticised for focussing too strongly on genes and ignoring cognitive, emotional and environmental factors. Despite this, the explanation has provided valuable insight into the causes and potential treatment for SZ.

To Conclude
SZ has many symptoms that overlap with other mental illness such as depression, but the most defining symptoms are hallucinations and delusions. Research into genetic explanations suggests that there is some degree of inheritance, despite this, environmental factors must also play a role. To overcome this issue, Howes and Murray (2014) conclude that genetic elements make some individuals more vulnerable to developing SZ, then exposure to social stressors can later lead to the development of SZ.
Reference:
Cardwell, M., Flanagan, C. (2016) Psychology A level The Complete Companion Student Book fourth edition. Published by Oxford University Press, United Kingdom.
© 2019 Angel Harper